Abstract
Boerhaave syndrome is caused by spontaneous, vertical tears, which are most commonly seen in the distal esophagus. Boerhaave syndrome may develop after vomiting, severe cough, blunt trauma, and difficulty swallowing. In our study, we aimed to present a 66-year-old male who developed mediastinitis secondary to Boerhaave syndrome and was admitted to the emergency department of a secondary-level public hospital. In our case, despite early exploration, esophageal repair, mediastinal debridement, and subsequent esophageal stent application to the perforation, the condition was mortal. In this rare syndrome, surgical repair to the esophagus can be done within the first 24–48 h.
Introduction and purpose
Boerhaave syndrome (BS) is characterized by spontaneous, vertical tears seen in the distal esophagus, which may develop due to etiologies such as vomiting, severe cough, blunt trauma, and difficulty swallowing. 1 The global estimated incidence of BS is approximately 3.1 per 1,000,000 per year, yet this figure is likely underestimated due to underreporting. BS has been documented across all races worldwide, predominantly affecting males with male-to-female ratios ranging from 2:1 to 5:1. 2 When diagnosis and appropriate treatment occur within 12–24 h, patients have a good prognosis with a survival rate approaching 75%. BS, if left untreated, has a mortality rate of over 90%. 3 BS is an uncommon condition, and the diagnosis can easily be missed or delayed, leading to complications like dehydration, mediastinitis, sepsis, acute respiratory distress syndrome, massive pleural effusion, esophageal fistula, empyema, shock, and eventually death. 4 In our study, we aimed to present a case that developed mediastinitis secondary to BS and was admitted to the emergency department of a secondary-level public hospital.
Case report
A 66-year-old male patient was admitted to the emergency department with complaints of high fever, weakness, and dyspnea following severe vomiting approximately 24 h ago. In his history, it was learned that he had been suffering from intermittent vomiting for about a month. The patient has had no previous surgery. In his blood analysis tests, his White Blood Cell count was 12.44 103/mL, Neutrophil count was 9.86 103/mL, and C-reactive protein count was 20.4 mg/L. The other blood results were normal. Thorax computed tomography (Thorax CT) showed widespread consolidated areas in all lobes in the bilateral lung parenchyma, hydropneumothorax on the left side, loculated areas containing air-fluid level in the mediastinum, and bleeding areas and edema around the distal esophagus (Figures 1 and 2). A left tube thoracostomy was performed. After applying tube thoracostomy, the stomach contents came out of the thorax drain. Esophageal perforation was confirmed by checking with methylene blue, and the decision was made for exploration. During exploration, a full-thickness perforation of approximately 3 cm at the lower end of the esophagus + widespread abscess formation in the mediastinum was detected. The perforated esophageal layers were repaired separately and supported with mediastinal fatty tissue. The loculated and necrotic areas in the mediastinum were debrided, and the pleural cavity was lavaged copiously with saline and povidone iodide solution. A simultaneous feeding jejunostomy was performed, and he was transferred to the intensive care unit. The patient, who was extubated on the third postoperative day, was taken to the wards and followed up. The patient, whose culture showed Acinetobacter, Pseudomonas, and Candida growth, was started on meropenem + levofloxacin + vancomycin + fluconazole with an infectious diseases recommendation. On the 27th postoperative day, the patient was transferred to the university hospital. Here, a self-expandable nitinol stent was placed in the leak area after an opening was detected in the repair line at the lower end of the esophagus with esophagoscopy (Figure 3). During the ward follow-ups, the patient developed respiratory failure on the 46th postoperative day and was intubated and taken back to the intensive care unit. However, the patient died due to septic shock on the same day.

Thorax computed tomography (Thorax CT) showed widespread consolidated areas in all lobes in bilateral lung parenchyma (red arrow), hydropneumothorax on the left side (orange arrow), loculated areas containing air-fluid level in the mediastinum (blue arrow), and bleeding areas and edema around the distal esophagus (green arrow).
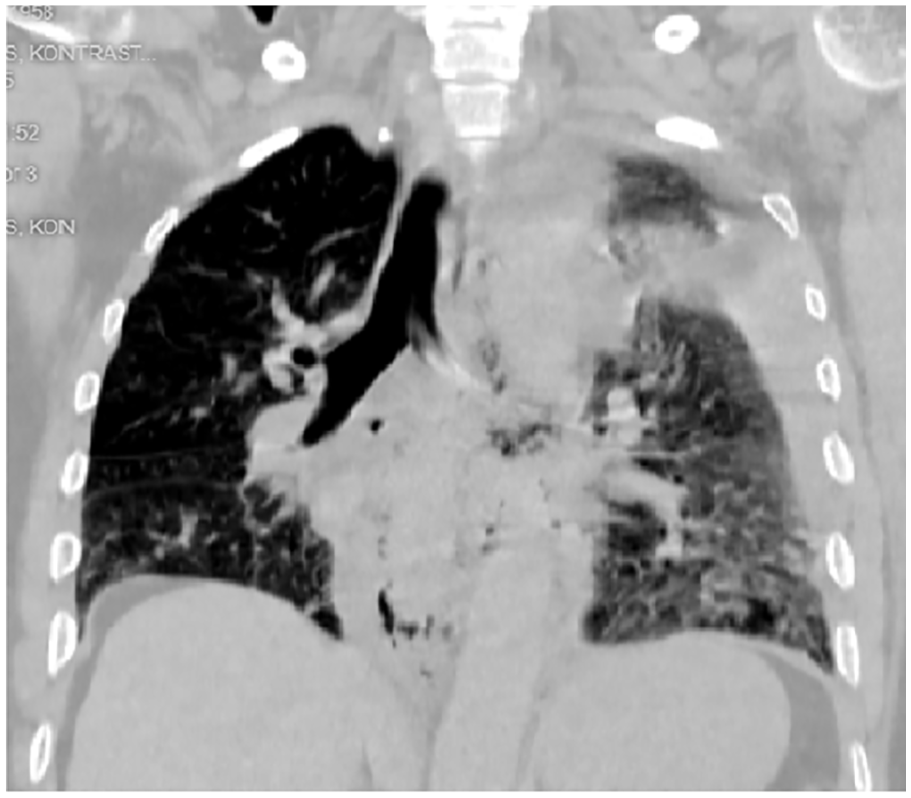
Thorax computed tomography (Thorax CT) showed widespread esophageal perforation in the left thorax (red arrow).

A self-expandable nitinol stent was placed in the leak area after an opening was detected in the repair line at the lower end of the esophagus with esophagoscopy (orange arrow).
Discussion
According to the literature, due to its rarity, nonspecific clinical presentation, and subtle or absent findings on plain radiographs, BS usually represents a diagnostic challenge. The cardinal symptom is sudden lower thoracic pain, sometimes radiating to the back and aggravated by swallowing, associated with vomiting and variable signs of the systemic inflammatory response, respiratory, and hemodynamic compromise.5,6 Although controversy exists about appropriate therapy, surgical management is currently considered the gold standard for ruptures diagnosed within 24 h of onset and allows a 75% chance of recovery. Surgery should include pleural cavity drainage, perforation debridement, and primary repair through an open thoracotomy or video thoracoscopic approach. 7
Conservative management with resuscitation and broad-spectrum antibiotics should be reserved for patients with minimal sepsis and mediastinal abnormalities, and for those too unstable to undergo surgery. In additive polymicrobial infections, two or more nonpathogenic microorganisms together can cause bacteremia and lung abscess. Many of these polymicrobial interactions occur within biofilms that form on natural or artificial surfaces within the human host.7,8 The development of multiple organisms rather than a single organism is thought to be associated with poor outcomes. In our case, Acinetobacter, Pseudomonas, and Candida growth occur.
Despite early exploration, esophageal repair, mediastinal debridement, and esophageal stent application, the chance of survival decreases logarithmically. Survival rates as low as 20% have been reported. Therefore, a high index of clinical suspicion and prompt diagnostic assessment are needed. 8 In this rare syndrome, early intervention and surgical management are considered the gold standard for ruptures diagnosed within the first 24 h from onset.5–8 In our case, the surgery is done within the first 24 h from application to the hospital. It is not known exactly when the esophageal rupture occurs. So, delayed intervention and the mediastinitis contributed to the poor outcome.
Symptoms of BS are generally nonspecific and may be seen with many other conditions, such as aortic dissection, pancreatitis, myocardial infarction, pulmonary embolus, perforated peptic ulcer, spontaneous pneumothorax, pneumonia, pericarditis, or Mallory–Weiss tear. These disorders can be distinguished from BS by history, physical examination, laboratory evaluation, electrocardiogram, and other imaging. 9
Treatment of the esophageal rupture with an esophageal stent is an alternative option for highly selected and inoperable patients. Few studies have compared stenting with surgical intervention. In a meta-analysis looking at 75 studies from 2000 to 2012, Biancari et al. 10 reported a mortality rate of 7.3% for esophageal stenting compared with 9.5% for open repair. Complications may occur due to the placement of self-expandable metallic stents, such as aspiration, stent malposition, and esophageal perforation. Chest pain, bleeding, tracheal compression, and respiratory problems may occur in the early period. In the late period, distal migration of the stent, perforation, and stent occlusion may occur.
The appropriate method for the management of esophageal perforation depends on many factors, such as severity, time since perforation, location, age, and patient status upon presentation. Treatment could be conservative (antibiotics with percutaneous drainage of abscesses or collections) or surgical; there is no consensus. However, most series show good results with surgical repair, and it has been the definitive treatment. There have been few reports describing thoracoscopic management of this entity, and there is a new endoscopic management. The endoscopic management is well established at present and is usually considered for patients with high-risk surgical intervention and those with a minimum leak. Boerhaave’s syndrome is managed on a case-by-case approach. 11
Conclusion
In our case, despite early exploration, esophageal repair, mediastinal debridement, and subsequent esophageal stent application to the perforation, the condition was mortal. In this rare syndrome, surgical repair to the esophagus can be done within the first 24–48 h. In cases detected in the later period, a combination of mediastinal drainage-debridement, tube jejunostomy, and continuation of nutrition is recommended to protect the patient from septicemia. Ongoing research and refinement of these approaches are crucial for improving long-term prognosis and patient outcomes in this life-threatening condition.
Footnotes
Acknowledgements
We would like to thank all the doctors and nurses working at the Lüleburgaz State Hospital and Trakya University Faculty of Medicine for their superhuman effort.
Ethical considerations
Our institution does not require ethical approval for reporting individual cases or case series.
Consent for publication
Written informed consent was obtained from a legally authorized representative(s) for anonymized patient information to be published in this article.
Author contributions
OEE and FY: responsible for inpatient care. OEE, FY, and YAK: synthesized the case report and retrieved the articles for the discussion. OEE: designed figures. OEE and FY: wrote the background and discussion. YY: conceptualization and supervision. All authors contributed to the manuscript revision and approved the submitted version.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
