Abstract
Penetrating trauma is one of the most common cause of occult vascular injury, especially in low velocity penetrating injury. This is usually in pretext of an innocuous looking small external wound. It is important for clinician to have high index of suspicion for such types of injuries, as the clinical examination with presenting signs and symptoms may be deceptive. Radiological evaluation is of paramount importance and essential to rule out any occult vascular insult. Conventional open surgical exploration is the gold standard for vascular injuries in neck. Minimal invasive endovascular stenting has selective role based on zone of neck, mechanism of injury, hemodynamic stability, neurological status and resource availability at treating centre. Early diagnosis and referral to an appropriate higher centre, preferably a trauma centre with expertise in handling major vascular injuries, improve the outcome. We present a case report of small innocuous looking external wound harbouring major central vessel injury underneath following low-velocity penetrating injury.
Keywords
Introduction
Penetrating injury to central vessels poses a surgical challenge due to its rarity, complexity of surgical approach and expertise available for its management. Penetrating injury is the most common cause of missed vascular injuries, especially in cases of low-velocity injury. 1 High-velocity penetrating injuries (>1000 ft/s) are associated with extensive surrounding tissue injury due to path of trajectory, energy transferred and cavitation effect. 2 In low-velocity penetrating injuries, especially in region around the major vessels, vascular injuries are often occult/missed in pretext of innocuously looking very small external wounds especially in busy emergency settings. Hence, it is important for clinician to have high index of suspicion in such types of injuries, as the clinical signs may be equivocal. Radiological evaluation is of essence to rule out any occult vascular injury in such cases. Early referral to higher centre, preferably to a nearby trauma centre, improves the outcome. We present a case report of small innocuous looking external wound harbouring major central vessel injury underneath following low-velocity penetrating injuries. All were managed surgically after proper radiological evaluation with a good postoperative outcome.
Case history
A 20-year-old male presented with alleged history of assault having stab injury with a knife over the front of neck. Victim arrived within 1 h of penetrating trauma. On initial assessment as per the Advanced Trauma Life Support (ATLS) principles in Emergency Department, primary survey was unremarkable without any abnormality. However, secondary survey revealed a 1 × 0.5 cm in length penetrating wound situated in zone II of the neck, 1 cm left of midline, anterior to sternocleidomastoid muscle (Figure 1), without any neurovascular deficit. Duplex ultrasound of neck revealed triphasic flow with normal calibre left sided common carotid artery; however, intimal flap visualized in right sided common carotid artery with eccentric partial thrombus (Figure 2). Patient immediately shifted for computed tomography (CT) angiography of neck as per the existing protocol of our institute. CT angiography revealed narrowing of lumen with eccentric thrombus in right common carotid artery about 5 cm proximal to bifurcation (Figure 3). Left sided carotid arteries and brain were unremarkable. Patient planned for surgical exploration of the neck wound under general anaesthesia. There was a through and through tangential rent of 0.5 cm in the right common carotid artery (CCA) with contused segment, situated about 5 cm proximal to carotid bifurcation (Figure 4). Resection of contused segment of about 3 cm done and interposition prosthetic polytetrafluoroethylene (PTFE) graft was placed (Figure 5). Postoperative hospital stay was uneventful and patient was discharged on postoperative day five. Anticoagulants were given for 6 months and then discontinued. Follow-up Duplex ultrasound at 1, 6 and 12 months were normal without any flow abnormality.

External appearance of innocuous looking wound over anterior neck.

Duplex ultrasound image showing eccentric thrombus in the lumen of right common carotid artery.

CT angiography image with narrowing of lumen with eccentric thrombus in right common carotid artery.

Intraoperative findings in right common carotid artery.
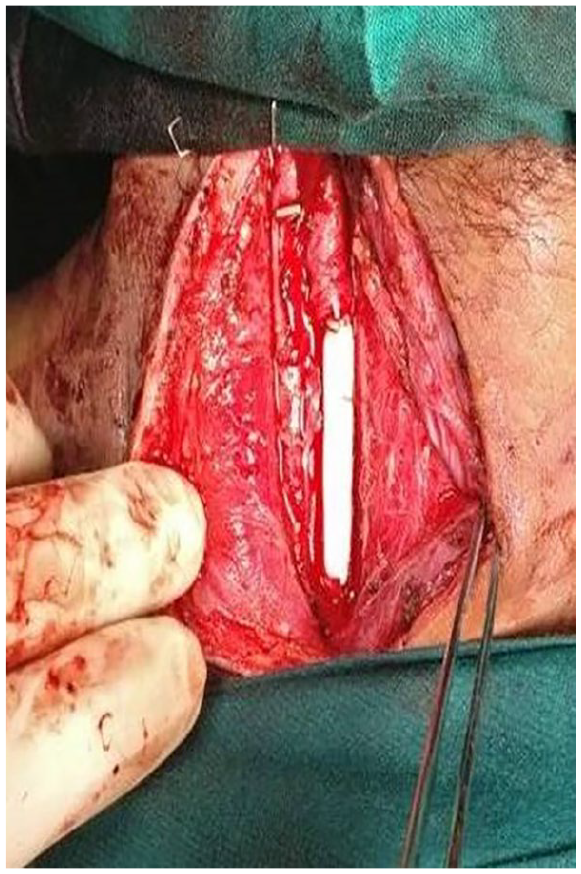
Prosthetic (PTFE) interposition graft placed during surgical exploration.
Discussion
The case discussed above highlights the importance of high level of clinical suspicion for early diagnosis of occult major vascular injury following low-velocity penetrating trauma. These wounds are deceptive like a tip of an iceberg, hiding beneath a major vascular damage. Patients with such small wounds following low velocity penetrating trauma are usually suture repaired especially in the absence of hard signs and discharged without undergoing thorough clinical and radiological evaluation.
Low velocity penetrating trauma has been implicated as a major cause of missed vascular injuries in various studies. Siddique et al reviewed 28 cases of missed vascular injuries. 1 They found that the most important cause of missed vascular injuries was penetrating trauma (64.2%) with low-velocity penetrating trauma being commonest and pseudoaneurysm being the most common complication. Yilmaz et al. reviewed 40 cases with missed vascular insult. They also found penetrating injury as the cause in 38 cases, while blunt trauma in only two cases. 3 Hence, clinician should be vigilant with low threshold for evaluation especially in low-velocity penetrating injury in proximity to a major vessel.
Vascular injuries have been categorized into five types: (a) intimal injuries, (b) pseudoaneurysm, (c) transaction, (d) arterio-venous fistula and (e) vasospasm. 4 Clinical signs for vascular injuries have been divided into two types: hard signs (would mandate intervention, in the form of the open or endovascular procedure) and soft signs (mandates further imaging to rule out vascular insult). 5 Incidence of vascular damage in patients with soft signs ranges from 3% to 25%. 6 Studies have shown the efficacy of clinical examination in the decision to observe penetrating injury with soft signs (proximity to a major vascular structure). However, in places with extensive collateral circulation (e.g. thoracic outlet), reliability of clinical examination is less. Also, in cases of intimal injuries, pseudoaneurysm and arterio-venous fistula, there may be no hard sign at presentation. Such injuries may later manifest as delayed haemorrhage. Missed vascular injury is associated with dreaded complications like pseudoaneurysm rupture, arterio-venous fistula formation leading to congestive heart failure and intimal flaps progressing to thrombosis leading to delayed ischaemia. 7 Pseudoaneurysm may enlarge and may produce compressive symptoms or erode nearby structures. Small flaps, pseudoaneurysm, and A-V fistulas may heal spontaneously without requiring any intervention. 8 However, it still remains a matter of debate as to which injuries can be managed expectantly. Regular follow-up with imaging is essential in such cases to ascertain the progression of injury or symptoms. Thus, it becomes important to identify vascular damages early.
Duplex imaging should be utilized as the first line of investigation for patients with soft signs as it is cost-effective, readily available and non-invasive. However, it is operator dependent, time-consuming and lacks anatomical details. 9 CT angiography is the gold standard investigation and has replaced the conventional catheter angiogram. It is reported to identify 5%–15% of occult vascular injuries in the absence of hard and soft signs. 10 CT angiography is non-invasive and provides a surgical road map for preparing intervention either by surgical exploration or by minimally invasive endovascular techniques.
Although open surgical technique remains to be the gold standard for all zones of penetrating carotid injuries, 11 endovascular stenting does have a selective role in penetrating trauma to proximal common carotid and distal internal carotid artery. 12 Surgical approach to these vessels is difficult with increased morbidity owing to relatively inaccessible location. Moreover, hybrid operating room is a prerequisite for stenting to address the need of immediate surgical exploration in case of unsuccessful endovascular attempt.
Surgical exploration is preferred for the carotid artery injuries situated in zone II of neck pertaining to easy surgical access with good proximal and distal vessel control using single anterior neck incision.12,13 It is prudent to attempt conventional surgical exploration in case of suspicious coexisting aerodigestive tract injuries. The options available on surgical exploration are suture ligation of carotid vessel, end-to-end anastomosis, lateral sutures and interposition (autologous venous or prosthetic) graft, depending on hemodynamic stability, neurological status, extent of damage to the vessel, mechanism of injury, and degree of contamination.
In our case, injury was situated in zone II with about 3 cm long segmental loss of common carotid artery due to oblique trajectory of weapon with minimal contamination of wound as patient arrived within 1 h of injury and surgical exploration done at earliest to reduce chances of potential contamination of wound with elapsing time. Reva et al. 13 reported surgical repair using a reversed long saphenous vein when there was marked (exceeding 2.5–3 cm in length) carotid artery segment defect. In our case, interposition prosthetic (PTFE) graft was placed owing to significant luminal discrepancy between autologous great saphenous vein and common carotid artery.
Conclusion
Small innocuous looking penetrating neck wound may be deceptive during clinical evaluation of a trauma victim. These wound may harbour a life-threatening damage to underlying vascular structure. High index of suspicion is warranted based on external location of wound and mechanism of injury. Radiological evaluation should be performed in cases where clinical evaluation is equivocal. Open surgical exploration remains the gold standard for vascular injuries in neck. However, endovascular stenting has a selective role based on neck zone, hemodynamic stability, neurological status, extent of damage and availability of resources. Prosthetic interposition graft may be safely placed under compelling circumstances of non-availability of suitable autologous venous graft.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics
Permission from Institutional Ethics Committee obtained. Consent from the patient has been obtained for use of pictures and treatment related data for publication/presentation.
Ethics approval
Ethical approval to report this case was obtained from Institute Ethics Committee, All India Institute of Medical Sciences, New Delhi (IEC -788/80).
Institute Ethics Committee, All India Institute of Medical Sciences, New Delhi
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
