Abstract
Deep granuloma annulare is an uncommon benign granulomatous skin disorder that presents almost exclusively in the paediatric population. It presents as an asymptomatic subcutaneous nodule with normal overlying skin on distal extremities, the scalp, or the forehead. It shows a deep palisading granuloma with areas of central necrobiosis on histologic examination. Due to its self-limited nature, clinical follow-up is recommended over surgical interventions. We present a case of cephalic deep granuloma annulare in a healthy 5-year-old girl who remains free of recurrence after surgical excision at the 6-month follow-up. Our case emphasizes the importance of differentiating the lesion from its clinical and histopathological mimickers, such as the rheumatoid nodule. The awareness of this entity is important to avoid the overinvestigation and overtreatment of a benign and self-limited disease.
Keywords
Introduction
Granuloma annulare (GA) is a common benign inflammatory skin disorder of unknown origin that affects children and adults. Four main clinicopathological variants of GA have been described: localized GA, disseminated GA, perforating GA, and deep GA (DGA). 1 The latter is an uncommon subtype that is seen almost exclusively in children. 1 Although DGA is a well-described entity in the literature, the diagnosis is often missed when it presents as an asymptomatic subcutaneous mass in children. We present a case of DGA in a 5-year-old girl in order to increase the awareness of this disease and to underscore the importance of differentiating DGA from its clinical and histological mimicker: the rheumatoid nodule.
Case presentation
A healthy 5-year-old girl was referred to a plastic surgeon for an evaluation of a subcutaneous nodule on her right superolateral forehead, which appeared spontaneously 7 months ago (Figure 1). There was no history of trauma or insect bites. She complained about intermittent swelling with erythema and mild tenderness on several occasions (Figure 2). On physical examination, a firm, non-mobile, and non-tender subcutaneous nodule with normal overlying skin was noted on her right temporal forehead. The magnetic resonance imaging showed a 5 mm subperiosteal lesion without deep extension. The Doppler ultrasound demonstrated the absence of vascularisation. The complete excision of the lesion was elected due to diagnostic uncertainty. Histologic examination showed a palisaded granuloma with central fibrinous degeneration in the deep dermis and subcutis that is compatible with deep GA (Figure 3). Special stains such as alcian blue/periodic acid–Schiff, Grocott methenamine silver, periodic acid–Schiff–diastase, and Ziehl–Neelsen were negatives (Figure 4). Our patient did not present clinical signs of arthritis and tested negative for rheumatoid factor and anti-cyclic citrullinated peptide. She remains free of recurrence at her 6-month follow-up.
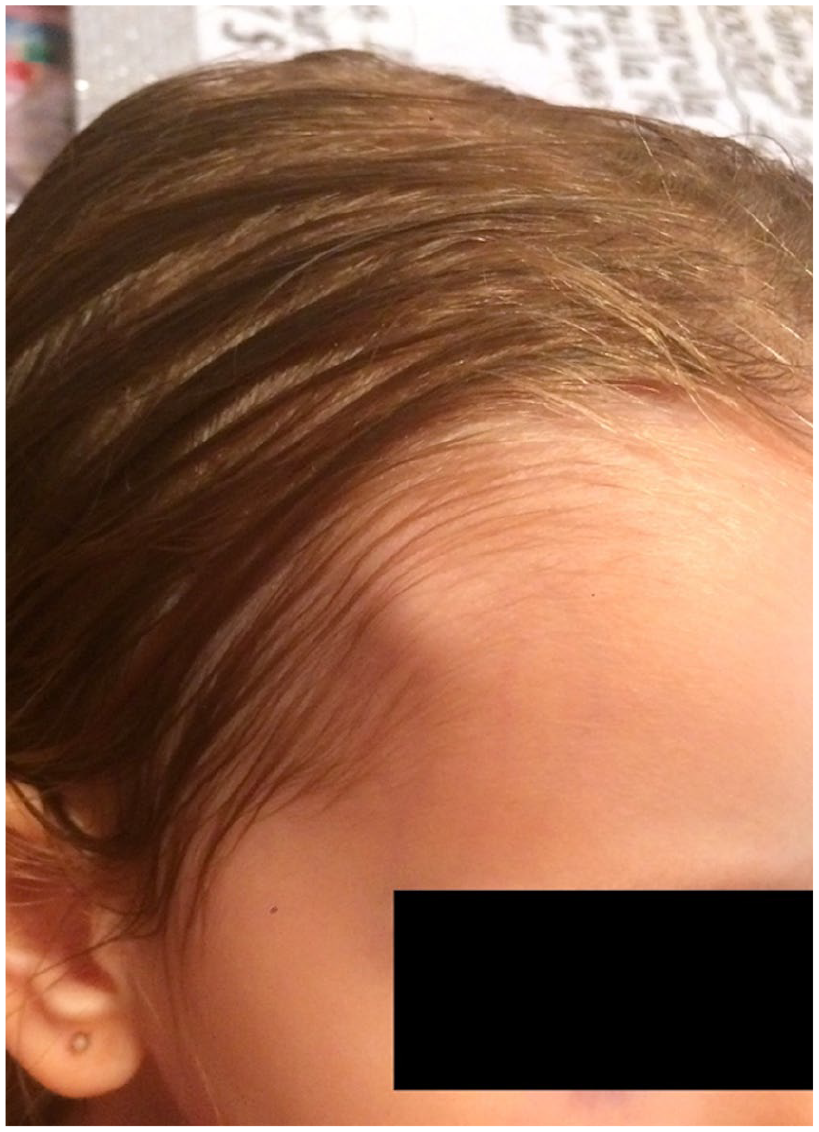
Subcutaneous nodule on the right superolateral forehead.

Subcutaneous nodule with intermittent swelling and erythema.

Palisaded granuloma with central fibrinous degeneration in the deep dermis and subcutis.

Negative by periodic acid–Schiff–diastase staining.
Discussion
DGA, also known as subcutaneous GA, was described for the first time by Ziegler in 1941. 1 It is a self-limited benign inflammatory granulomatous dermatitis of unknown aetiology. It presents almost exclusively in the paediatric population with a typical age of onset between 2 and 6 years old. 2 Upon physical examination, DGA presents as a firm non-tender subcutaneous nodule that grows slowly with normal overlying skin. Rarely, the lesion can become inflamed, erythematous, and tender. 3 Lesions can be solitary or multiple. DGA can also occur in association with a classic localized GA. It is usually located on the distal extremities, the scalp, or the forehead. The pathogenesis of the disease is unknown; however, multiple triggers have been proposed: trauma, insect bites, diabetes mellitus, tuberculosis, varicella, and streptococcal infection. 4
The clinical differential diagnosis is very broad and includes rheumatoid nodule, dermoid cyst, pilomatrixoma, lipoma, hemangioma, lymphangioma, osteoma, epithelioid sarcoma, infectious granuloma, and abscesses. 5 When medical history, physical examination, and imaging cannot discriminate between these diagnoses, an incisional biopsy is recommended.
On histologic examination, DGA shows areas of central necrobiosis in the deep dermis and subcutaneous fat with increased mucin deposition surrounded by palisading histiocytes, and occasional lymphocytes, fibroblasts and eosinophils. The rheumatoid nodule is the main histological mimicker of DGA. For this reason, DGA is also known under the confusing name of pseudorheumatoid nodule. Histologically, the difference between the two entities is very subtle and sometimes impossible to make. Since rheumatoid nodule typically lacks mucin, alcian blue or colloidal iron stains may provide important diagnostic value. However, the absence of mucin deposition does not rule out the diagnosis of DGA. Moreover, DGA can be differentiated clinically from rheumatoid nodules by its age of onset, localization, and lack of systemic involvement. 6 Numerous retrospective studies in the past showed that despite their histological similarities, DGA is not associated with connective tissue diseases. 1 The other main histological differential diagnosis of DGA is infectious granuloma which can be ruled out with special stains and skin cultures.
Spontaneous regression of DGA is expected over months to years. Due to its self-limited nature, clinical follow-up is recommended over surgical interventions. The latter can be pursued if the lesion becomes symptomatic or impairs the patient’s daily functioning. However, the recurrence rate varies from 40% to 80%. 2 Therefore, clinical recurrence does not change the diagnosis unless there are additional clinical clues that would point towards rheumatic diseases.
Our case emphasizes the benign nature of DGA and the importance of differentiating the lesion from its mimickers, such as the rheumatoid nodule. DGA is not associated with connective tissue diseases and resolves spontaneously. It should be included in the differential diagnosis of a subcutaneous nodule on the head and neck region in healthy children. The awareness of this entity is important to avoid the overinvestigation and overtreatment of this benign and self-limited disease.
Footnotes
Acknowledgements
The authors express gratitude to the patient and her parents for the permission to publish this case.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics approval and consent to participate
Our institution does not require ethical approval for reporting individual cases.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
The consent to publication occurred in the context of the photo documentation.
