Abstract
A 79-year-old man visited our hospital with a chief complaint of erythema around the urethral orifice of the glans, and a diagnosis of penile Bowen’s disease was made by penile skin biopsy. Initially, local tumor resection with skin grafting from the femoral skin was performed. However, histopathological examination revealed a positive urethral margin of tumor. Since the degree of urethral lesion of penile Bowen’s disease was unclear, the patient received glansectomy. Histopathological examination revealed a tumor lesion in the distal urethra, 7 mm from the external urethral orifice, and confirmed the complete resection of urethral Bowen’s disease. The patient recovered well, with no definite recurrence of Bowen’s disease up to 13 months after partial penectomy. Human papillomavirus 16 DNA was detected in the paraffin-embedded tumor sample, and in situ hybridization confirmed human papillomavirus 16 DNA locations in the tumor tissue. Immunohistochemistry revealed that p16-INK4a was widely expressed in the tumor tissue.
Introduction
Bowen’s disease (BD) is a squamous cell carcinoma (SCC) in situ that develops in the epithelium and was first described in the United States in 1912. 1 BD is frequently associated with epithelial tumors in the neck and external genitalia in men and women, and tumors on the palms, tongue, and perianal skin are occasionally found. 2 BD can progress to invasive SCC without clinical intervention, which results in severe clinical conditions with distant metastasis and fatal disease. Progression of BD to invasive carcinoma is reported to develop in 3%–5% of extra-genital lesions; this risk increases up to 10% in cases of genital localization. 3 Human papillomavirus (HPV) infection, immunosuppression, ultraviolet radiation exposure, arsenic, chemical carcinogens, X-ray irradiation, trauma, and genetic factors have been suggested as some of the causes of BD.2,3
BD occasionally occurs in the glans penis, whereas penile BD involving the distal urethra is extremely rare, and therapy options for these cases are limited. Here, we report an extremely rare case of penile BD with distal urethra involvement in a patient who was treated with a glansectomy. In addition, this study demonstrates the presence of HPV16 in the tumor tissue and its potential etiological role for the development of tumor. Hence, we reviewed previous studies of this rare clinical finding of penile BD with the involvement of distal urethra.
Case
A 79-year-old man visited our hospital with a chief complaint of erythema around the urethral orifice of the glans, which exacerbated 6 months ago. Visual examination revealed red-brown erosion on the glans penis around the external urethral orifice (Figure 1). Physical examination showed no definite inguinal lymph node swelling. A diagnosis of penile BD was made with a penile skin biopsy. The patient was referred to our department to evaluate the involvement of BD in the distal urethra.
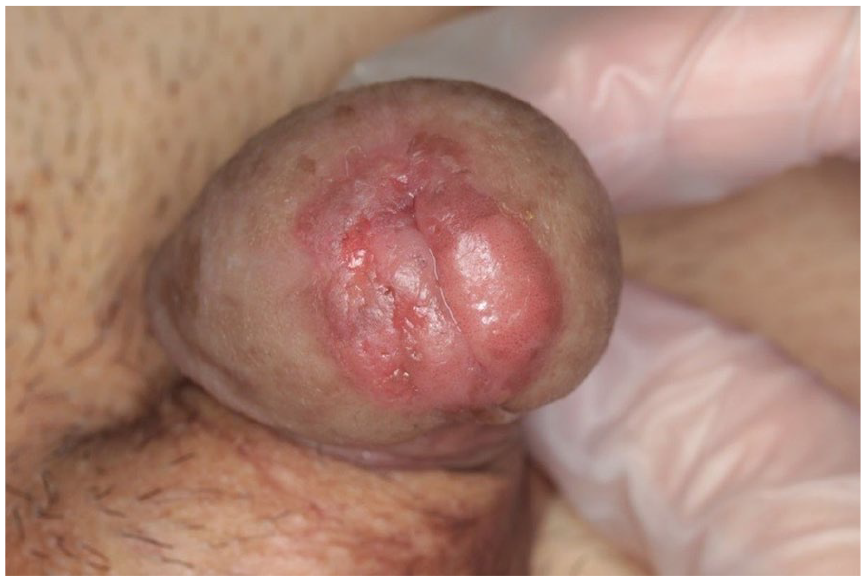
Visual examination revealed a red-brown erosion of the glans penis around the external urethral orifice.
Visual examination and cystoscopy revealed no definite tumorous lesions in the urethra or urinary bladder. Urine cytology was negative. No definite BD lesions in the distal urethra were expected to be found in this case; therefore, local tumor resection with skin grafting from the femoral skin was performed (Figure 2(a)). The superficial region of the glans penis, with a margin of 5 mm from the visual lesions, was resected, together with the external urethral orifice.

(a) Growths of stratified squamous epithelial cells with nuclear atypia in all layers of the glans mucosa are shown, and a diagnosis of penile BD was made (H&E stain, 40× magnification). (b) ISH analysis revealed the widely observed punctate HPV16 DNA signals (brown staining) in the nuclei of cancer cells (100× magnification). (c) Immunohistochemistry revealed that p16-INK4a was widely expressed in the tumor tissue (40× magnification).
Although the peripheral surgical margin of the glans penis was negative, a positive urethral margin of the tumor was revealed upon histopathological examination. Since the degree of urethral involvement of penile BD could not be estimated with any clinical observation, the patient received a glansectomy 2 months after the initial surgery. The decision to completely resect the carcinoma was confirmed by the intraoperative frozen section analysis. Histopathological examination revealed the growth of stratified squamous epithelial cells with nuclear atypia in all layers of the urethral mucosa; hence, the patient was diagnosed with urethral BD. A tumorous lesion in the distal urethra, 7 mm from the external urethral orifice, was found. The patient recovered well, with no definite recurrence of BD up to 13 months after the glansectomy. After the second surgery for limited resection of the penis, the patient could urinate in a normal position.
DNA was extracted from the paraffin-embedded tumor sample using the Pinpoint Slide DNA Isolation System™ (Zymo Research, Orange, CA), and HPV16 DNA was detected using flow-through hybridization (HybriBio™; HybriBio Ltd., Hong Kong). In addition, the locations of HPV16 DNA in the tumor tissue could be observed with in situ hybridization (ISH) (Figure 2(b)). Immunohistochemistry demonstrated that p16-INK4a, which is a surrogate marker of oncogenic HPV-E7 protein, was widely expressed in the tumor tissue (Figure 2(c)). Based on these findings, we diagnosed the patient with HPV16-positive penile BD involving the distal urethra.
Discussion
The patient developed penile BD involving the distal urethra, which was successfully treated with a glansectomy. This disease frequently occurs in the epithelium and occasionally appears in the glans penis; however, involvement of the distal urethra is extremely rare.
Several treatments for genital BD have been proposed, including surgical excision, penectomy, local application of 5-fluorouracil, cryotherapy, irradiation, photodynamic therapy, and laser therapy.2,4 Surgical resection is the most common and highly reliable treatment for BD, in which a surgical excision margin of 5–15 mm from definite tumorous lesions is recommended. 2 Concerning the patients’ quality of life, penectomy should be avoided, if possible. Therefore, local resection of penile lesions was initially performed in this case.
A limited number of case reports have described penile BD with distal urethra involvement, and treatment options for these cases are limited.5–8 Focal therapy, such as irradiation and laser for urethral lesions, may cause urethral stricture.2,4 In addition, it is challenging to detect urethral lesions or their degree of involvement in the urethral mucosa using urethroscopy. Therefore, a partial penectomy was chosen for complete resection in many of the previous cases.5–7 Conversely, a few reports have described that penile preservation surgery was performed for cases of BD involving the urethra, 8 and carbon dioxide laser vaporization was used for a case with visible urethral lesions. 9 In this case, a tumor lesion of BD was present 7 mm from the external orifice, suggesting that a glansectomy would likely be reasonable to preserve urinary function. In accordance with the present and previous findings, the treatment option for penile BD involving the urethra is not limited to only radical penectomy, but a preservative surgery, which maintains urinary and penile functions, is also likely to achieve a complete resection of this disease.
Recently, HPV infection has attracted attention due to its etiological role in the development of penile carcinomas including genital BD.2,6,10–12 In particular, anogenital BD is likely to be involved with HPV infection, and HPV16 is often detected in genital BD tissues. 11 However, limited studies have investigated the etiological role of HPV in the development of genital HPV-positive BD. Similar to the previous studies, HPV16 was detected in the paraffin-embedded tumor sample in this case. In addition, ISH analysis revealed that active HPV16 DNA signaling in the nuclei of cancer cells was observed, and the ISH signals had a punctate pattern, which is indicative of HPV genome integration into the host tumor cells as seen in penile and cervical cancer.12,13 Furthermore, p16-INK4a, a widely accepted surrogate marker of the oncogenic domain (HPV-E7) of HPV in cervical, oropharyngeal, and penile carcinomas, 12 was widely expressed in the tumor sample. These findings are likely to suggest a potential etiological role of HPV16 for the carcinogenesis of penile BD in this case.
Conclusion
We report an extremely rare case of a patient with penile BD involving the distal urethra, who was treated by glansectomy. This study demonstrates the presence of HPV16 in the tumor tissue and its potential etiological role for tumor development.
Footnotes
Data policies
This case is not shared with any prior published cases and data.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
The Kanazawa University Hospital Institutional Review Board approved this study.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient for his anonymized information and images to be published in this article.
