Abstract
Background:
Foodborne illnesses pose significant health challenges globally, affecting both developed and developing nations. Despite numerous review addressing pathogenic bacteria in various animal-origin foods in Ethiopia, there is a notable lack of research specifically focused on raw milk and milk products.
Objective:
This study aims to systematically review the prevalence of pathogenic bacteria in raw milk and milk products, identify associated risk factors and assess antimicrobial resistance in Ethiopia from 2014 to 2024.
Methods:
A comprehensive search of PubMed, JANE, Scopus, and Google Scholar yielded 1596 articles, of which 18 full-text studies were included based on eligibility criteria, following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses guidelines. Data were extracted and analyzed to determine pooled prevalence rates, associated risk factors, and antimicrobial resistance across various Ethiopian regions.
Results:
The review identified a pooled prevalence of pathogenic bacteria at 18.7% (95% CI: 17.46%–19.94%) from January 2014 to February 2024. Major pathogens included Escherichia coli O157:H7 (5.2%), Staphylococcus aureus (18.27%), and Listeria monocytogenes (3.86%). The Oromia Region exhibited the highest prevalence (85.9%), while the lowest was recorded in Ambo, Holeta, and Bako towns (2.28%). Bacterial contamination of raw milk and milk product showed a statistically significant association with raw milk sample collectors (p < 0.028), livestock age (p < 0.001), inadequate hygiene (p < 0.0001), and illiteracy (p < 0.000), highlighting urgent educational needs. The overall antimicrobial resistance rate was alarming at 86.2%, with multidrug resistant isolates constituting 50.6%. Significant resistance was noted against commonly used antimicrobials such as nalidixic acid (100%), ampicillin (89.7%), amoxicillin (76.3%), penicillin (75%), oxacillin (73.6%), and streptomycin (61.5%).
Conclusions:
The findings indicate a critical need for enhanced surveillance and intervention strategies to address microbial contamination and antibiotic resistance in Ethiopia’s dairy sector. Targeted educational initiatives and stricter regulations on antibiotic use in animal husbandry are essential to improve dairy safety and public health outcomes.
Keywords
Introduction
Background of study
Milk and dairy products are fundamental components of the human diet, recognized for their essential nutrients that support physical and cognitive development. 1 Globally, cow’s milk serves as the primary ingredient in a variety of dairy products, including cheese, butter, ice cream, yogurt, and powdered milk, making it an integral part of nutrition in many cultures. 2
However, the high nutritional content of raw milk and dairy products creates an ideal environment for bacterial growth. 3 While raw milk from healthy cows typically contains low bacterial levels, it is susceptible to contamination from foodborne pathogens and spoilage bacteria shortly after secretion. Contaminants can originate from various sources, including human hands, milk containers, bedding materials, animal hides, feces, soil, air, feed, water, and infected udders.4,5 This highlights the multifaceted risk of disease transmission, as food consumption, direct contact, and environmental exposure can facilitate the spread of zoonotic diseases from animals to humans. 6
Approximately 60% of human diseases are zoonotic in origin, with 75% of newly identified infectious diseases emerging from vertebrate animals. 7 The consumption of contaminated raw milk is a significant pathway for such diseases, with pathogens such as E. coli O157:H7, Listeria monocytogenes (causing listeriosis), Salmonella spp. (leading to salmonellosis), and Brucella spp. (responsible for brucellosis) known to cause serious health effects.8,9 Common bacterial contaminants in raw milk include S. aureus, E. coli, Salmonella enterica Typhimurium, Shigella spp., L. monocytogenes, and Campylobacter jejuni.10–12
Contamination can occur at multiple stages within the food chain, including production, processing, distribution, preparation, and consumption. 13 Factors such as food handlers’ health, personal hygiene, and knowledge of food safety practices are crucial in mitigating contamination risks. 14
Globally, foodborne illnesses represent a serious public health issue affecting both developed and developing nations, although the burden disproportionately impacts developing regions.15,16 The World Health Organization estimates that up to 2 million people die annually from foodborne illnesses in these nations, while about 30% of individuals in industrialized countries experience such illnesses each year. 15 In Africa, foodborne diseases contribute to 33%–90% of child mortality, underscoring the severity of the issue. 17
Milk is a major source of foodborne illnesses in underdeveloped countries like Ethiopia, where unsanitary production conditions and poor practices exacerbate the risk. 18 Poor hygiene and sanitation contribute to nearly 60% of the disease burden in Ethiopia, as indicated by the National Hygiene and Sanitation Strategy program. 19 A survey in central Ethiopia revealed that 31.8% of farmers utilized raw milk, with contamination rates reported between 45% and 75% in northern regions.20,21
The rise of multidrug resistance (MDR) among foodborne pathogens poses an escalating public health threat. The overuse of antibiotics in both human medicine and animal agriculture has led to an increased prevalence of MDR pathogens, which can cause more severe illnesses than their susceptible counterparts.13,22 This trend complicates treatment options, contributing to higher mortality rates and challenging the management of infectious diseases. 23
Despite existing review on pathogenic bacteria in various animal-origin foods in Ethiopia, there is a significant gap in the literature specifically addressing raw milk and milk products. A comprehensive scientific review is essential to evaluate the current landscape of pathogenic bacteria, and their drug resistance patterns in consumable dairy products. Additionally, establishing baseline data on the risk factors associated with raw milk and milk products contamination is crucial. Therefore, this proposed systematic review and meta-analyses aimed to update the pooled prevalence of pathogenic bacteria in raw milk and milk products, identify associated risk factors, and assess drug resistance patterns in Ethiopia from 2014 to 2024.
Methods and materials
A systematic review and meta-analysis, carried out in Ethiopia to update the pooled prevalence of pathogenic bacteria in raw milk and milk products, identify associated risk factors and assess drug resistance patterns in Ethiopia from 2014 to 2024.
Search strategy
The literature search was performed on the PubMed, JANE, Scopus, and Google Scholar databases for identification of all published articles between January 1, 2014 and February 29, 2024, following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA)-Search guidelines.24,25 The study protocol can found on PROSPERO under the reference Identification number CRD420250649282 and the methodology can also accessed at https://www.crd.york.ac.uk/PROSPERO/view/CRD420250649282
The published articles were searched, as the main sources of literature reviews, and the reference lists of identified articles were searched for additional studies. Subject headings, including Medical Subject Headings terms, were utilized for database searches: “Prevalence” AND (“Pathogenic Bacteria” OR “Spoilage Bacteria” OR “Zoonotic Bacteria” OR “Bacterial Contamination” OR “Bacterial Infections”) AND (“Antimicrobial Resistance (AMR)” OR “Drug Resistance”) AND “Associated Factors” AND (“Raw Cow Milk” OR “Milk Products”) AND “Ethiopia.”
Eligibility criteria
Inclusion criteria
The studies conducted on the prevalence and drug resistance patterns of pathogenic bacteria only in Ethiopia after 2013 and publications in English were used as primary inclusion criteria for this article’s selection. The study participants, study designs, study sample types, studies with sample size and number of positive samples, and studies reporting diagnostic methods were also considered.
Exclusion criteria
This systematic review excluded unpublished manuscripts, studies lacking relevant titles and abstracts, exactly duplicated studies, studies lacking essential primary data, studies with sample size limitations, and studies that didn’t report specific sample types. Studies conducted before 2014, studies conducted outside of Ethiopia, and systematic reviews and meta-analyses were excluded. This review also excluded the reference lists of the research that did not fit the criteria.
Screening procedures
Data extraction for this systematic review and meta-analyses involved thorough screening of each included article to capture essential information. Key variables included the administrative regional state, specific study area (such as zone, district, or town), actual study year, and employed study design. Additionally, data on study participants, sample types, sample size, number of positive samples, laboratory techniques, isolated bacterial pathogens, drug resistances, co-resistances, multidrug resistance, and associated factors were meticulously collected. The name of the first author and the year of publication were also noted. Prior to the commencement of data analysis, independent cross-checks were conducted to verify the accuracy of the extracted information, ensuring the integrity of the final analysis.
Outcome measures
The outcome measures for this systematic review and meta-analyses included the prevalence of pathogenic bacteria in raw milk and milk products, alongside their associated drug resistance patterns. Specifically, metrics such as the rates of multidrug resistance, co-resistance, and the identification of significant risk factors influencing bacterial contamination were evaluated. These measures aimed to provide a comprehensive understanding of the microbiological safety of dairy products in Ethiopia and inform public health interventions.
Data processing and statistical analysis
Data processing and statistical analysis were carried out with precision to ensure the reliability of the results. The data were first cleaned and validated to remove inconsistencies and outliers. Descriptive statistics summarized key variables, including the prevalence of pathogenic bacteria and patterns of drug resistance. Inferential statistical methods, such as Chi-square tests and logistic regression, were employed to examine associations between categorical variables, with significance set at p < 0.05. This rigorous analytical approach facilitated the identification of significant risk factors contributing to bacterial contamination in raw milk and milk products. Such a comprehensive methodology underscored the validity of the findings and their implications for public health.
Heterogeneity assessment
In this systematic review and meta-analyses, examining the prevalence of pathogenic bacteria and drug resistance patterns in raw milk and milk products in Ethiopia from 2014 to 2024, heterogeneity among the included studies was critically assessed. The I² statistic was utilized to quantify the proportion of variation attributable to heterogeneity, with thresholds indicating low (I² < 25%), moderate (25% ⩽ I² < 50%), and high (I² ⩾ 50%) levels of heterogeneity. 26 This statistical approach was complemented by visual assessments through forest plots, allowing for a qualitative understanding of the consistency of findings across studies.
Subgroup analyses were conducted based on factors such as geographical region, sample size, and methodological differences, which provided insights into the sources of variability in the results. When significant heterogeneity was identified, random-effects models were applied to account for the variability in effect sizes. This comprehensive assessment of heterogeneity not only enhanced the robustness of the conclusions drawn but also highlighted the complexities involved in interpreting the prevalence of pathogenic bacteria and their antibiotic resistance in Ethiopian dairy products. 27
Results
Initially, a total of 1596 articles were identified from the PubMed, JANE, Scopus, and Google Scholar databases. Therefore, 1164 articles were identified from other countries, and 172 articles were from Ethiopia. However, 33 articles were assessed for eligibility, and 18 of them with full-text articles were included for the final analysis, following the PRISMA flow diagram, 25 as shown in the figure below (Figure 1).

The PRISMA flow diagram presenting the screening process.
Pooled prevalence of pathogenic bacteria in raw milk and milk products in Ethiopia
This systematic review and meta-analyses identified 18 articles employing cross-sectional study designs, encompassing data from 4 administrative regions in Ethiopia: Tigray, Oromia, Southern Ethiopia, Amhara, and Addis Ababa. A total of 3796 samples were analyzed, yielding 709 positive cases of pathogenic bacteria, which facilitated the calculation of the pooled prevalence over a decade of reporting in Ethiopia.
The review revealed a pooled prevalence of pathogenic bacteria at 18.7% from January 1, 2014 to February 29, 2024. Notably, major pathogens included E. coli (19%, 40/210) and E. coli O157:H7 (5.2%, 11/210), S. aureus (18.27%, 446/2,440), and L. monocytogenes (3.86%, 28/722). The Oromia Region exhibited the highest prevalence, particularly in selected districts of North Shoa and the Special Zone around Fin Fine, where rates reached an alarming 85.9% between January and February 2023. This was followed by the Amhara Region, specifically Debre Berhan town, with a prevalence of 66.7% from February to August 2022.
Conversely, the lowest prevalence was recorded in the Oromia Region, particularly in Ambo, Holeta, and Bako towns, at 2.28% during 2018–2019. Southern Ethiopia, including Dale and Arsi Negele districts and Hawassa city, reported a prevalence of 7.08% from 2019 to 2020.
A 10-year trend analysis indicated a significant decline in prevalence in the Tigray Region (Shire town), decreasing from 32.81% in 2014–2015 to 2.28% in 2018–2019. However, this trend was not uniform; a resistance was observed with a prevalence increase to 25.3% in the Oromia Region (Borena Zone) from March to April 2019. Furthermore, the prevalence in Southern Ethiopia decreased to 7.1% from 2019 to 2020 but surged again to 85.9% in the Oromia Region in early 2023. These findings underscore the variable nature of pathogenic bacteria prevalence across regions and time periods, as illustrated in (Table 1).
Summary of pooled prevalence of pathogenic bacteria in raw milk and milk products in Ethiopia (2014–2024).
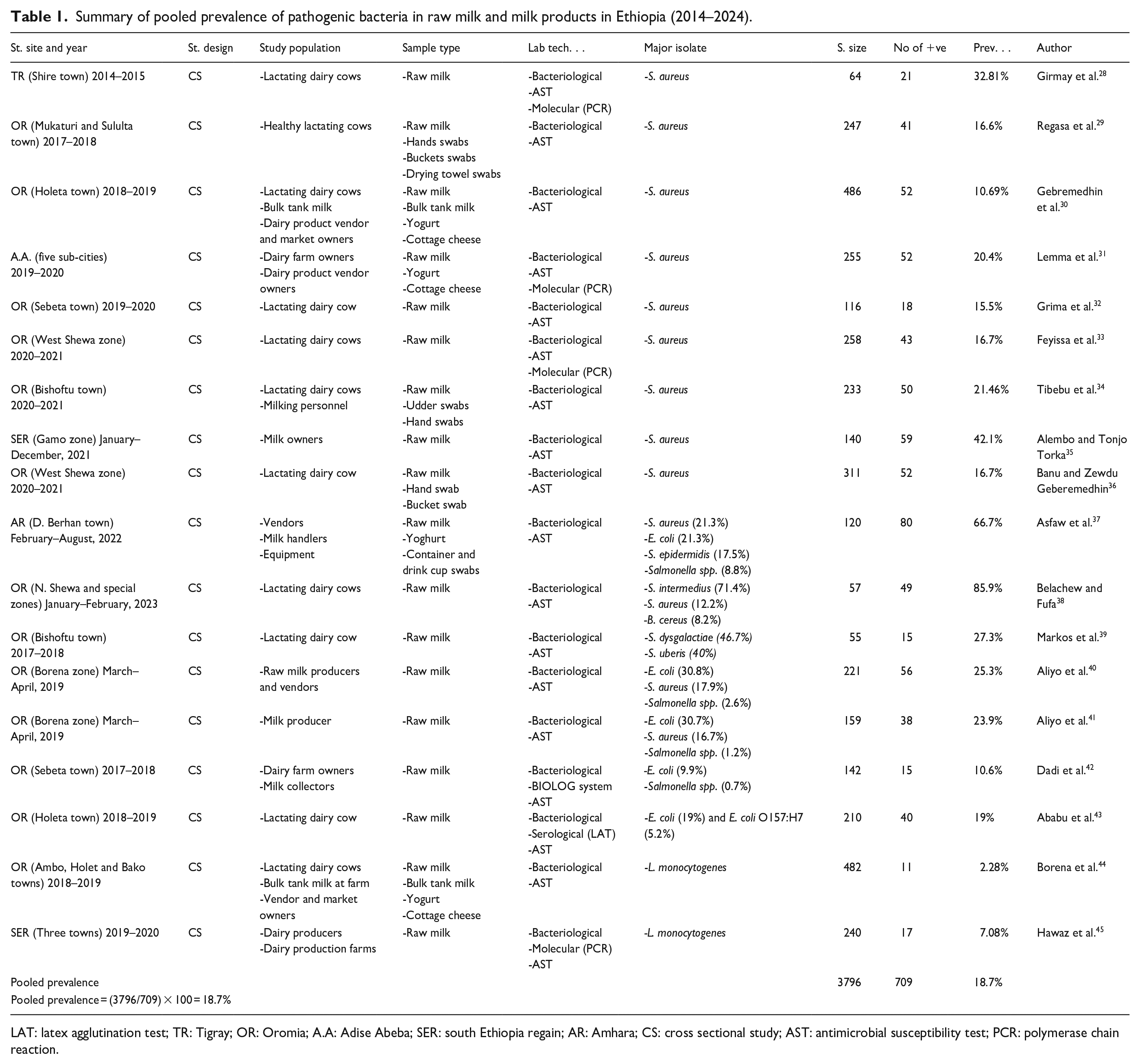
LAT: latex agglutination test; TR: Tigray; OR: Oromia; A.A: Adise Abeba; SER: south Ethiopia regain; AR: Amhara; CS: cross sectional study; AST: antimicrobial susceptibility test; PCR: polymerase chain reaction.
AMR patterns of pathogenic bacteria in raw milk and milk products in Ethiopia
This review provides a comprehensive analysis of the drug resistance patterns exhibited by pathogenic bacteria, revealing a concerning overall resistance rate of 86.2% (514 out of 596 samples). The study identified several critical resistance profiles, with Nalidixic acid (NA) demonstrating a complete resistance rate of 100% (38/38). Other significant resistances included ampicillin (AMP) at 89.7% (339/378), amoxicillin (AMX) at 76.3% (142/186), penicillin (PEN) at 75% (234/312), oxacillin (OXA) at 73.6% (53/72), and streptomycin (STR) at 61.5% (32/52). Furthermore, the analysis highlighted that multidrug resistant (MDR) isolates constituted 50.6% (264/522) of the total isolates examined.
The review particularly noted that the highest levels of drug resistance, reaching 100%, were recorded in specific regions, including Shire town in the Tigray Region (2014–2015), as well as Ambo, Holeta, Bako towns, and the West Shewa Zone in the Oromia Region during 2018–2019 and 2020–2021. Moreover, significant resistance patterns were observed in the Southern Ethiopia Region, specifically in the Bule Hora and Dugda Dawa districts from 2019 to 2020. Conversely, the lowest resistance rate of 14.3% was documented in Sebeta town of the Oromia Region during the 2017 to 2018. These findings underscore the alarming prevalence and variability of AMR across different regions of Ethiopia, highlighting the urgent need for enhanced surveillance and targeted intervention strategies to curb this public health threat, as shown in Table 2.
Summary of drug resistance and multidrug resistance patterns in raw milk and milk products in Ethiopia (2014–2024).

STR: streptomycin; SXT: sulphamethoxazole-trimethoprim; CLO: cloxacillin; AMC: amoxicillin-clabulanic acid; CTX: cefotaxime; OT: oxy tetracycline; GM: gentamycin; EM: erythromycin; PEN: penicillin; NA: nafcillin; AMP: ampicillin; OX: Oxacillin; TET: tetracycline; FOX: cefoperazone; SX: sulfamethoxazole; AMX: amoxicillin.
Associated factors of pathogenic bacteria in raw milk and milk products in Ethiopia
Among the 18 articles reviewed in Ethiopia, 11 identified significant risk factors contributing to increased bacterial contamination in raw milk and milk products. Most of these factors were reported in the Oromia Region, with additional insights from the Southern Ethiopia Region, specifically the Gamo Zone in 2023. Table 3 summarizes a 10-year analysis of the factors influencing the prevalence of pathogenic bacteria in raw milk and milk products from 2014 to 2024. Notably, a study in Sebeta Town highlighted milk sample collectors as a critical contamination risk, revealing a p-value of <0.028. Similarly, in Mukaturi and Sululta Towns, several factors-such as age (old >9 years), high parity (>4 calves), semi-intensive management systems, and poor drainage conditions-were linked to contamination, all with p-values ⩽ 0.001.
Summary of factors associated with pooled prevalence of pathogenic bacteria in raw milk and milk products in Ethiopia (2014–2024).

OR: Oromia; SER: south Ethiopia regain.
Findings from Holeta Town further indicated significant associations with herd size (⩾42), parity (1–3 calves), poor body condition, age (3–6 years), udder lesions, and inadequate udder hygiene practices, with p-values ranging from <0.001 to <0.0001. In the Borena Zone, the studies emphasized the importance of clean water sources and handwashing before milking, with significant p-values (p < 0.01 to <0.001). In the Southern Ethiopia Region, particularly the Gamo Zone, alarming associations were noted between educational attainment, hygiene practices, and cleaning methods, all showing p < 0.001. Recent findings from Northern Shewa and Special Zones identified late lactation stages and extensive farming systems as notable risks. Overall, this analysis underscores the urgent need for targeted interventions to enhance dairy safety and public health in Ethiopia, as detailed in (Table 3).
Discussions
This systematic review and meta-analysis have aimed to examine and quantitatively summarize the pieces of scientific literature in Ethiopia; on the prevalence of microbial contamination in raw milk and milk products from this review was 18.7% (95% CI: 17.46%–19.94%), suggesting that a significant portion of milk samples were microbiologically unfit for consumption due to poor bacteriological quality. This finding is in agreement with studies conducted in various Ethiopian regions, such as Oromia Region, Holeta town (19%) 43 and Addis Ababa (20.4%). 31 These results indicate that while contamination remains a major concern, the prevalence appears to be relatively moderate in these regions. The regional variations observed in contamination levels could likely be attributed to differences in agricultural practices, milk handling techniques, and overall hygiene standards, all of which significantly influence the safety and quality of milk and milk products.
However, this prevalence of 18.7% is lower than contamination rates observed in regions such as Borena Zone (25%), 40 Bishoftu (27%), 39 Shire town (32.81%), 28 Gamo Zone (42.1%), 35 Debre Berhan (66.7%), 37 and North Shoa and Fin Fine (85.9%). 38 These higher rates underscore the persistent challenges in managing milk quality, likely exacerbated by factors such as inadequate sanitation, poor milk handling practices, and livestock management issues. The elevated contamination levels in these regions highlight significant gaps in practices that are essential for maintaining milk quality, aligning with prior concerns about regional disparities in the dairy industry and the resulting public health risks. On the other hand, the prevalence of microbial contamination in this review is higher than the findings from Sebeta town (10.6%), 42 Holeta (10.69%), 30 Southern Ethiopia, the selected two districts (Dale and Arsi Negele) and Hawassa city (7.08%), 45 and the Oromia Region, Ambo, Holeta, and Bako towns (2.28%). 44 These lower contamination rates may reflect better sanitary practices, more effective livestock care, and possibly stricter regulatory measures in these regions, underscoring the importance of localized interventions to improve milk quality.
In addition to contamination, this review revealed a high overall drug resistance rate of 86.2% (95% CI: 83.4%–89.0%) in pathogenic bacteria found in milk. This high rate of resistance to commonly used antibiotics such as NA, AMP, AMX, PEN, OXA, and STR is a serious public health threat in Ethiopia, indicating widespread antibiotic misuse in animal husbandry. These findings are lower than research conducted in Addis Ababa, selected five subcities (94%), 31 Tigray Region, Shire town (100%), 28 Oromia Region, Ambo, Holeta, and Bako towns (100%), 44 Southern Ethiopia, the selected two districts (Dale and Arsi Negele) and Hawassa city (100%), 45 and Amhara Region, Debre Berhan Town (98.8%). 37 The higher resistance rates in these regions suggest that antimicrobial stewardship programs and regulations concerning antibiotic usage in livestock may be insufficient or poorly implemented. However, the resistance rates in this study were higher than those found in the Oromia Region, the selected districts of North Shoa and the Special Zone around Fin Fine (55.6%) 38 and Sebeta Town (14.3%), 42 indicating substantial regional variation in the effectiveness of control measures and the degree of antibiotic misuse in animal farming. The consistently high resistance rates in this review emphasize the urgent need for stricter regulations on antibiotic use in animal husbandry to mitigate the rise of AMR, which poses a serious risk to public health.
The MDR rate in this review was 50.6% (95% CI: 46.4%–54.9%), which aligns with findings from Southern Ethiopia, the Dale and Arsi Negele districts, and Hawassa city (47%). 45 The MDR rates observed in this study were higher than those in regions such as Borena Zone (14.3%), 40 Sebeta (11.11%), 32 and Bishoftu (10.42%), 34 suggesting that MDR pathogens are more prevalent in some areas than in others. This may be due to factors such as overuse of antibiotics, poor hygiene practices, and inadequate veterinary oversight in certain regions. However, the MDR rate in this review was lower than those observed in studies from Addis Ababa (75%), 31 Sebeta (65%), 42 Debre Berhan (65%), 37 Tigray Region, Shire town (100%), 28 Oromia Region, Ambo, Holeta, and Bako towns (81.82%), 44 and Southern Ethiopia Region, Gamo Zone (83%). 35 These discrepancies underscore the complex nature of AMR, suggesting that local factors such as farming practices, sanitary conditions, and veterinary interventions play a crucial role in the emergence and spread of MDR pathogens.
In terms of risk factors for bacterial contamination in raw milk and milk products, the review of 18 articles revealed several critical associations, especially within the Oromia Region and Southern Ethiopia. Notable risk factors include the role of milk sample collectors in Sebeta Town (p < 0.028), 42 the influence of livestock age, high parity, and poor drainage in Mukaturi and Sululta (p < 0.001), 29 and the significant contributions of herd size and inadequate udder hygiene in Holeta (p < 0.0001). 43 Other contributing factors such as the lack of handwashing and poor container cleanliness in Borena (p < 0.001) and the impact of tick infestations in West Shewa (p < 0.000) highlight widespread hygiene issues that exacerbate microbial contamination.33,40,41 Moreover, a strong correlation between illiteracy and poor cleaning practices in the Gamo Zone (p < 0.000) further emphasizes the need for targeted educational initiatives to improve milk safety across these regions.
Limitations
This review, while comprehensive, has several limitations. First, there is insufficient literature available in Ethiopia concerning the risk factors associated with pathogenic bacterial contamination in milk and dairy products. Many studies conducted in the region lacked specific results, which hampers thorough understanding of the issue. Additionally, the absence of systematic reviews or meta-analyses focused solely on milk and dairy products in Ethiopia limits our ability to contrast and compare findings effectively. Lastly, challenges in accessing non-English literature may have further constrained the review’s comprehensiveness. These limitations underscore the necessity for enhanced research efforts in this critical area to support food safety and public health initiatives.
Conclusions and recommendations
This systematic review and meta-analyses highlights critical public health concerns regarding microbial contamination and antibiotic resistance in raw milk and dairy products in Ethiopia. The pooled prevalence of pathogenic bacteria was found to be 18.7%, indicating that a significant proportion of milk samples are microbiologically unfit for consumption. Alarmingly, the overall drug resistance rate of 86.2% underscores the widespread misuse of antibiotics in animal husbandry, exacerbating the public health threat posed by AMR.
Regional disparities in contamination and resistance rates reflect varying agricultural practices, hygiene standards, and regulatory oversight. The findings emphasize the urgent need for targeted interventions, including enhanced surveillance, education on hygiene practices, and stricter regulations on antibiotic use in livestock. Collaborative efforts among stakeholders are essential to improve dairy safety, thereby protecting public health and ensuring the quality of milk and dairy products across Ethiopia.
To address these pressing issues, it is imperative for all stakeholders in the dairy industry including farmers, processors, distributors, and consumers to implement stringent food safety measures. Governments and regulatory bodies should establish comprehensive inspection and monitoring programs to ensure safe production, transportation, and storage of dairy products.
Educational initiatives are essential to improve hygiene practices among dairy operators and consumers. Increasing awareness of the risks associated with contaminated milk can empower stakeholders to implement higher safety standards. Moreover, localized interventions should be prioritized, especially in regions with higher contamination rates, to enhance milk quality.
Routine, population-specific research is crucial for understanding the dynamics of microbial contamination and drug resistance. Identifying risk factors such as inadequate hygiene and livestock management will inform targeted intervention strategies. For instance, improving udder hygiene and promoting effective milk handling practices could significantly reduce contamination rates. Finally, stricter regulations on antibiotic use in animal husbandry are necessary to combat the rise of AMR. Collaborative efforts among farmers, veterinarians, regulatory bodies, and public health officials are essential to enhance the safety and quality of raw milk and dairy products, ultimately benefiting both public health and the economy.
Author summary
This systematic review and meta-analysis assessed the prevalence of pathogenic bacteria, associated factors, and AMR patterns in isolated photogenic bacteria in raw milk and dairy products in Ethiopia. Led by SBB, the research team (SBB, CKL, SAB) conducted a comprehensive literature search using stringent inclusion and exclusion criteria. Initially, 1596 articles were identified from databases including PubMed, JANE, Scopus, and Google Scholar, with 1164 from international sources and 172 specifically from Ethiopia. After rigorous eligibility assessments, 33 articles were reviewed, of which 18 full-text articles met the criteria for final analysis, following the PRISMA flow diagram. This study highlights critical insights into microbial threats in dairy, emphasizing the need for continued surveillance and intervention strategies to ensure food safety and public health in the region.
Footnotes
Acknowledgements
We thank the researchers and institutions whose studies contributed to this review. Their commitment to advancing research has offered invaluable insights into the prevalence of pathogenic bacteria, drug resistance patterns, and associated factors in raw milk and dairy products in Ethiopia. We also appreciate the support from our colleagues and peers, whose contributions were essential in the development and refinement of this manuscript. Your efforts have significantly enriched this work.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
All the data included in this review has been cited and can be accessed online.
