Abstract
Background:
Multi-drug resistant Mycobacterium tuberculosis is a growing public health problem in developing countries including Somalia. Although, the prevalence of multi-drug resistant tuberculosis among new and retreated cases is high, data on GeneXpert- Mycobacterium tuberculosis/rifampicin-resistant assay, which is a surrogate marker for multidrug resistance, is not well explored in Mogadishu.
Objectives:
To determine the prevalence of rifampicin-resistant Mycobacterium tuberculosis and its associated factors among presumptive pulmonary tuberculosis patients visiting tuberculosis centers in Mogadishu, Somalia.
Methods:
A multicenter cross-sectional study was conducted in three tuberculosis treatment centers from March 12 to April 30, 2021. Laboratory professionals collected sputum sample consecutively from presumptive pulmonary tuberculosis participants and performed a GeneXpert assay to determine the rifampicin resistance. Socio-demographic and clinical data were collected using structured questionnaire. Logistic regression analyses were performed to assess factors associated with rifampicin resistance using an adjusted odds ratio at a 95% confidence interval. Statistical significance was considered at a p-value of less than 0.05.
Results:
A total of 370 presumptive tuberculosis suspects were included; of whom 58.4% were females and the mean age of the participants was 44.3 ± 14 years. Mycobacterium tuberculosis was detected in 63 (17%) (95% confidence interval = 13.2–20.8) suspects. Of these the prevalence of rifampicin-resistant Mycobacterium tuberculosis was 35% (95% confidence interval = 30.2–39.8). Anti-tuberculosis treatment history (adjusted odds ratio = 4.1; 95% confidence interval = 1.91–6.75), monthly income less than $100 USD (adjusted odds ratio = 2.2; 95% confidence interval = 1.77–5.98) and being diagnosed with Asthma (adjusted odds ratio = 2.63; 95% confidence interval = 1.3–7.3) were significantly associated with rifampicin-resistant tuberculosis.
Conclusion:
A considerable proportion of rifampicin-resistant tuberculosis is reported in these study settings. The strong association between multidrug resistance tuberculosis and patients’ retreatment history of tuberculosis, low income, and co-morbidity with asthma highlights the need for more efforts in tuberculosis treatment and monitoring programs to limit the emergence of multi-drug resistant strain in the study areas.
Introduction
Drug-resistant Mycobacterium is one of the most urgent and difficult challenges facing global tuberculosis (TB) control, with more than half million cases reported worldwide in 2020.1,2 Early case detection of Mycobacterium tuberculosis (MTB) and appropriate case management are key steps to minimize the high risk of human-to-human transmission of the disease and to the success of TB treatment. 3 Since 2010, the World Health Organization began to recommend the utilization of GeneXpert MTB/RIF assay that simultaneously detect TB and rifampicin (RIF) rapidly in people with signs and symptoms of TB. 4 It’s an automated molecular test using real-time polymerase chain reaction (PCR) technology. 5 Resistance to rifampin (RR) in M. tuberculosis is associated with mutations in the rpoB gene coding for the β-subunit of Ribonucleic acid polymerase.6,7 Besides, it is an ideal object for studying the general drug resistance mechanisms of M. tuberculosis 7 and is a surrogate marker for multidrug-resistant tuberculosis (MDR-TB). 8 Now a days, new advances in the molecular detection of TB, including the faster and simpler nucleic acid amplification test (NAAT) and whole-genome sequencing, have resulted in a shorter time for diagnosis.9,10 With respect to drug susceptibility testing, NAATs and next-generation sequencing can provide results substantially faster than traditional phenotypic culture. 11 Matrix-assisted laser ionization-time of flight (MALDI-TOF MS) can be used as an effective alternative for rapid screening of mycobacterial isolates. Furthermore, Sanger sequencing could be used as an additional method to improve identifications in species for which MALDI-TOF MS identification is limited. 12
TB in Somalia is a serious public health problem and one of the leading causes of morbidity and mortality. For instant, the 2021 Global TB report indicated that there was a marginal increase in the estimated TB incidence in Somalia, from 258 per 100 000 people in 2018 to 259 per 100 000 in 2020. 13 An estimated 6.2% annual reported TB cases in Somalia have drug-resistant TB. 14 Furthermore, a nationwide drug resistance survey in 2010–2011, MDR-TB was detected in 5.2% of the newly diagnosed TB cases and 40.8% of TB patients with a previous history of TB treatment. 15
Among the reported contributing factors for the development of MDR-TB are previous history of treatment with anti-tuberculosis drugs, 16 lack of efficient TB control programs, illiteracy, poverty, co-infection with human immunodeficiency viruses (HIV), patients with diabetes mellitus (DM) and a scarcity of research on the causes of MDR-TB. 17 Besides, the absence of adequately funded and properly coordinated TB programs in Somalia had led to incomplete dosing and possible misuse of anti-TB drugs for other ailments providing the basis for the development of MDR-TB in the country. 18
Although a high prevalence rate of drug-resistant TB was indicated from a national survey, 15 there is a paucity of data on the magnitude of RR and associated factors in the study area. In addition, the lack of stable central government for the last three decades, that can lead to the breakdown of the health sector, and intermittent challenges, such as famine, droughts, and communicable diseases including TB are associated factors. Therefore, this study aimed to assess the prevalence of RR-MTB and its associated factors among presumptive pulmonary tuberculosis (PTB) participants visiting TB treatment centers in Mogadishu, Somalia.
Materials and methods
Study area and period
The study was conducted in Mogadishu locally known as Xamar or Hamar, the capital and most populated city of Somalia from March 12 to April 30, 2021. The city has served as an important port connecting traders all-round the Indian Ocean for millennia and currently has a population of 2,425,000 residents. It has a distance of 835 miles (1344 km) over the Indian Ocean. Mogadishu is located in the coastal Banadir region on the Indian Ocean, which, unlike other Somali regions, is considered a municipality rather than a federal state. Although Somalia is recovering from three decades of civil war, the health services of the country are still poor. In general, the country has 264 health posts, 197 health centers, and 47 Hospitals. 19
Study design and population
An institutional-based cross-sectional study was conducted among presumptive PTB adult patients who had visited TB treatment centers in Mogadishu during the study period and who gave written consent to participate.
Patients who were not willing to participate in the study and seriously ill were not part of this study. In addition, patients who were on anti-TB during the study period were excluded from the study.
Sample size determination
Sample size was determined using a single population proportion formula by considering the prevalence of RR-MTB from a previous study conducted in Jigjiga, Ethiopia (18.4%), 20 a confidence interval (CI) of 95% and 4% of margin of error and the final calculated sample size for this study was 378.
Sampling technique and procedures
Mogadishu has two governmental and eight non-governmental TB treatment centers. We purposively selected three TB centers, based on the presence of GeneXpert services. Accordingly, Lansolote TB treatment center, Finsoma TB center from governmental health facilities, and Finsoma TB center and Muslim Aid TB center from non-governmental health facilities were included. The final sample size for this study was allocated proportionally to the selected TB centers based on the number of patients who visited each TB center from March 12 to April 30, 2020. Accordingly, the number of patients who visited Finsoma, Muslim Aid, and Lansolote TB centers was 1740, 953, and 1378, respectively. Therefore, the required sample size from each TB center was (Finsoma = 162), (Muslim Aid = 89), and (Lansolote = 127). Each study participant was selected consecutively until the calculated sample was fulfilled.
Operational definition
Presumptive TB denotes a patient with signs and symptoms of TB such as night sweat, loss of appetite, coughing up blood (Hemoptysis) or mucus, chest pain, short breathing, and productive cough which last for 2–3 weeks
MDR-TB: TB that does not respond to at least isoniazid and RIF, the most important first-line anti-TB drugs.
Rifampicin-resistant TB (RR-TB): It is a genotypic resistance basis to RIF detected using GeneXpert with or without resistance to other first-line anti-TB drugs. 21
Data collection methods
Laboratory professionals collected about 5 mL of a purulent sputum sample in 50 mL Falcon tube from each TB suspect. Socio-demographic and clinical data were collected using a pretested structured questionnaire adapted from previous literature.20,22,23 The questionnaire was prepared first in English and translated to the local language (Af-Somali) and re-translated back to English to check its consistency. The questionnaire contains socio-demographic characteristics, TB-related factors, behavioral-related factors such as tobacco use and cigarette smoking, and finally co-morbidity-related factors such as HIV/TB co-infection, DM, and Asthma were collected. A total of five data collectors (one physician, two Medical laboratory professionals, and two Nurses) who have more than 2 years of experience were used to collect the data and supervised by two qualified Health officers.
Sputum sample processing and laboratory investigation
The sputum specimen was processed in a Class II biosafety cabinet. The sputum sample was mixed with the buffer solution in a 2:1 ratio as instructed by the manufacturer. Then, 2 mL of the mixed sample was transferred to GeneXpert MTB/RIF cartridge and then placed into the machine. The GeneXpert assay is a NAAT that purifies and concentrates M. tuberculosis complex bacilli from sputum samples, isolates genomic material from the captured bacteria, and subsequently detects the genomic Deoxyribonucleic acid by PCR. The GeneXpert automates all of the following steps; sample workup, nucleic acid amplification, detection of the target sequence, and result interpretation. Briefly, the primers in the Xpert MTB/RIF assay amplify a portion of the rpoB gene containing the 81 base pair “core” region. The probes are able to differentiate between the conserved wild-type sequence and mutations in the core region that is associated with resistance to rifampicin. The result of GeneXpert was automatically generated and printed out by the computer attached to the GeneXpert machine.
Examination of co-morbidity
DM status
To examine the DM status of the patients, a random blood glucose test was performed by using a blood glucometer. The finger of the patient was cleaned with 70% of alcohol and cotton. An automatic lancet was used to puncture the finger and a small drop of the blood was placed on the disposable test strip that the glucometer uses for glucose measurement. The glucometer machine uses the electrochemical principle. The test strip contains a capillary that sucks up a reproducible amount of blood. The glucose in the blood reacts with an enzyme electrode containing glucose oxidase or dehydrogenase. Then the glucose undergoes a chemical reaction in the presence of enzymes and electrons are produced during the chemical reaction. Finally, the glucometer machine measures the generated electrons and this is proportional to the concentration of glucose in the sample. 24 The sample was taken at any time that participants visit the health facility without looking at whether they have eaten or not. Patients who have a plasma glucose level which ⩾200 milligrams per deciliter (mg/dl) were considered as diabetic. 25
Blood pressure measurement
Blood pressure was measured using a sphygmomanometer which was regularly inspected and validated. Before measuring blood pressure, it was made sure that the subjects have not consumed any hot beverages, such as tea or coffee, or smoked/chewed tobacco, or undertaken vigorous physical activity within the 30 min preceding the measurement. Three separate measurements were taken on the left arm of the seated participant using a device, and the average BP reading is recorded. The average of the readings of systolic blood pressure (SBP) and diastolic blood pressure (DBP) was taken as the blood pressure of the participant. The three blood pressure measurements are obtained after the patient is rested for at least 5 min in a seated position. The second and third measurement was taken 5–10 min after the first and second measurement respectively. A patient was considered hypertensive if systolic or diastolic blood pressure equals or greater than (SBP ⩾ 140 or DBP ⩾ 90 mmHg) respectively. 25
Assessment of asthma
The assessment of asthmatic patients is mainly depending on the history and physical examination and there is no golden standard test for asthma. 26 Therefore, an experienced physician was allocated to examine patients. Then based on his/her findings the study participants were categorized as asthmatic or non-asthmatic.
Assessment of HIV sero-status
The TB centers in Mogadishu had HIV screening program for all TB presumptive patients. Thus, the HIV status of the study participants was reviewed from their medical records and finally, the participants were categorized as positive, negative, and unknown.
Statistical analysis
EpiData 3.1 version was used for data entry and exported to Statistical Package for Social Sciences version 25 software for analysis. Descriptive statistics like mean and standard deviation were performed. The prevalence of RR-TB was determined as the proportion to those patients with RR-MTB. Bivariate and multivariable analyses were performed to identify factors associated with RR-MTB. Model fitness was checked using Hosmer and Lomshow goodness-of-fit. Variables with a p-value of less than 0.25 in the bivariate analysis were considered as a candidate for the multivariable analysis. The association between RR-MTB and independent variables was measured using an adjusted odds ratio (AOR) at 95% CI. Statistical significance was considered at a p-value of less than 0.05.
Data quality control
Data quality was maintained by pre-testing the questionnaire before actual data collection on 5% of sample size (20) in Bandir and Manhal TB centers which were not selected for data collection. Two-day intensive training was given for data collectors and supervisors on the questionnaires’ interview, appropriate sputum sample collection, the procedure of GeneXpert performance, and satisfactory recording of the patient results. During the data collection, one health officer supervised the data collection site. The principal investigator was also following the laboratory activity on a daily basis and checks the completeness of the filled questionnaire and whether the recorded information makes sense to ensure the quality of data collected.
The GeneXpert diagnostic machine automatically performs its internal quality control for each sample. It has an in-built quality control system within the test cartridge. The cartridge contains a Sample Processing Control (SPC) and probe check control. The SPC ensures adequate processing, while the Probe checks control verifies that all necessary steps of the test take place correctly. When there was an inadequate sample, as well as an error in sample processing, the GeneXpert automatically rejects the specimens. Furthermore, to increase the reliability and accuracy of the test, checking the new batch of cartridges with a confirmed positive specimen was done. Data were cleaned and checked for any missing data by running frequencies and central tendencies before analysis. Two data clerks entered data and consistency was cross-checked by comparing the two separately entered data.
Ethical consideration
This study was performed under the international (Helsinki) and national research regulations. Ethical clearance was obtained from Haramaya University, College of Health and Medical Sciences through the Institutional Health Research Ethics Review Committee (IHRERC) Ref.No. IHRERC/034/2021. A permission letter to conduct this research was obtained from the Mogadishu health bureau. Study subjects were given information about the objectives of the study and informed written consent or thumb print for subjects who were unable to write were obtained. Subjects participated voluntarily and could withdraw from the study at any time without further consequences. Study participants who become resistant to rifampicin were linked to appropriate drug-resistant TB treatment centers.
Results
Socio-demographic characteristics
In this study, a total of 370 individuals have participated with a 97.8% response rate. A higher proportion of the participants were female (58.4%), married (54.9%), and with illiteracy rate of (58.4%). The mean age of the study participants was 44.3 ± 14 years (Table 1).
Socio-demographic characteristics of study participants at Mogadishu TB centers, 2021 (N = 370).

Clinical features
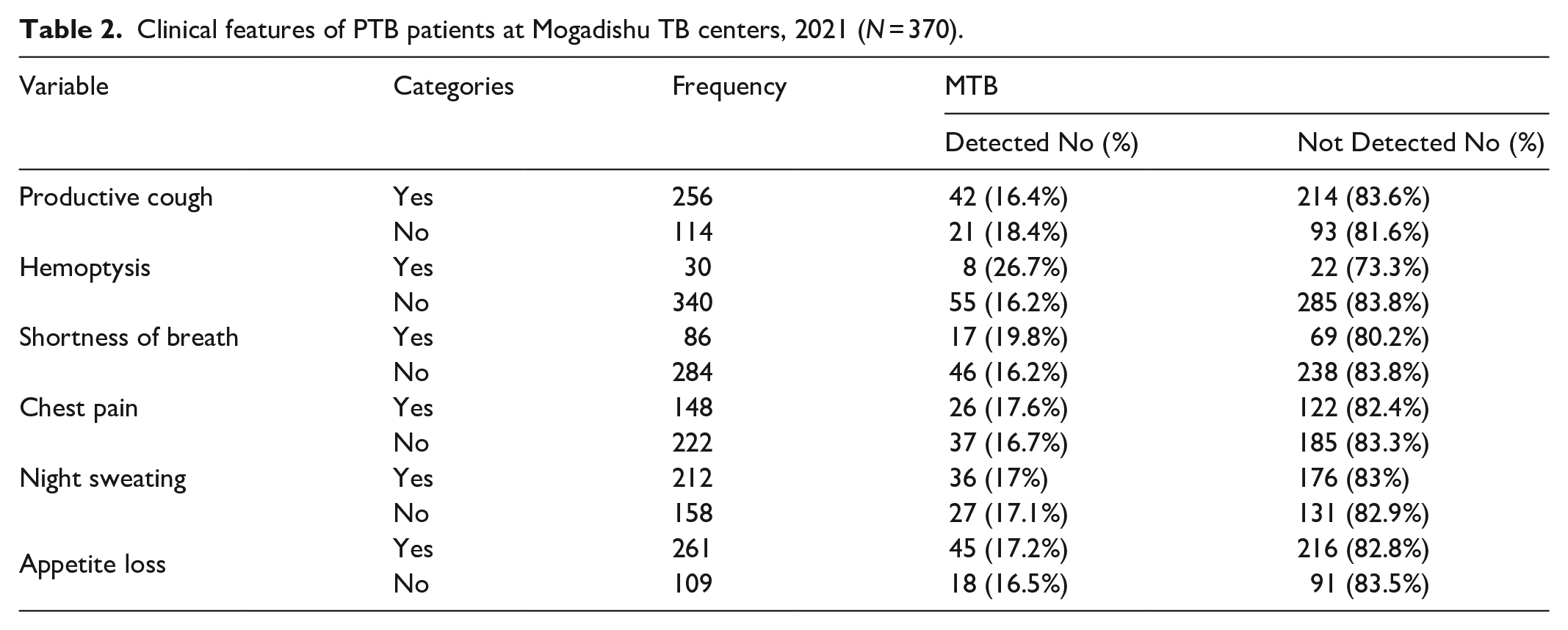
The main symptoms experienced by the participants were loss of appetite (70.5%), followed by productive cough (69.2%), night sweating (57.3%), chest pain (40%), shortness of breath (23.2%) and sputum with blood (8.1%) (Table 2).
Clinical features of PTB patients at Mogadishu TB centers, 2021 (N = 370).
Prevalence of RR-MTB
Out of 370 presumptive PTB patients, 63 (17%) (95% CI = 13.2–20.8) of them were identified as having PTB(Table 3).
Prevalence of M. tuberculosis among presumptive TB study participants in Mogadishu TB centers, 2021 (N = 370).

Among patients diagnosed with PTB, 22 (35%) (95% CI = 30.2–39.8) of them were resistant to rifampicin. The proportion of RR-MTB was 31.6% (12/38) among previously treated TB patients and 3.1% (10/332) among treatment naïve patients. Nine patients had HIV/TB co-infection and only two of them (22.2%) were resistant to rifampicin. Fifty-seven (15.4%) of the study participants were diagnosed with Asthma and eight (14%) of them were resistant to rifampicin (Table 4).
RR-MTB rate among presumptive TB study participants in Mogadishu TB centers, 2021 (N = 370).

Factors associated with RR-MTB
In bivariate analysis variables like place of residence, monthly income, family size, cigarette smoking, chewing of chat and tobacco, history of imprisonment, history of previous TB treatment, contact with known TB case, and asthma status were significantly associated with RR-MTB (Table 5).
Bi-variable and multivariable analysis among presumptive PTB patients at Mogadishu TB centers, 2021.

statistically significant.
However, in the multivariable analysis, only patients with lower monthly income, history of previous TB treatment, chewing of tobacco, and asthma were remaining significantly associated with RR-MTB (p <.05) (Table 5).
Patients who have a previous history of TB treatment were four times more likely (AOR = 4.1; 95% CI = 1.91–7.75) to develop RR-MTB than those who don’t have a previous history of TB treatment. Patients whose monthly income was less than $100 USD were two times more likely (AOR = 2.2; 95% CI = 1.077–5.98) to develop RR-MTB compared to those who have a monthly income greater than $100 USD. Furthermore, patients who were tobacco chewers were about three times more likely (AOR = 2.8; 95% CI = 1.25–5.73) to have RR-MTB compared to their counterparts. The odds of those patients living with Asthma were 2.6 times (AOR = 2.63; 95% CI = 1.3–8.3) higher than non-asthmatic patients (Table 5).
Discussion
RR-MTB is a growing public health problem in the study area. According to this study, more than one-third PTB positive cases were resistant to rifampicin. Previous history of TB treatment, lower monthly income, and co morbidity with asthma were found important factors associated with RR-MTB.
The prevalence of PTB among presumptive PTB patients was 17%. This finding is lower than studies conducted in Ethiopia which ranges from 23.2% to 30.5%.5,27,28 However, it is higher than studies from different parts of Ethiopia which reported 7.9% to 15.1%.29–31 The possible reasons for the variations could be due to differences in the methods of detection of M. tuberculosis, geography, and TB control and prevention programs.
The prevalence of RR-MTB in this study is comparable with other studies conducted in Nairobi, Kenya (30%) 32 and Ghana (31.4%). 33 However, this finding is higher than the national reports and previous studies reported from different parts of neighboring country, Ethiopia which ranges from 4.1% to 15.8%5,27–31 and study reported by Gautam et al. from India (26.1%). 34 A higher proportion of RR-MTB in this study setting could be attributed to weak TB prevention and control measures in Somalia. 15 The variation in rifampicin resistance prevalence could be due to differences geographic location, level of exposure to anti-TB drugs, national health care strategies in TB control among courtiers, population access to health-care facilities, and /or methods of drug resistance gene detection.
In the current study, having a previous history of TB treatment was strongly associated with drug-resistant TB. This strong association could be explained that RR-MTB strains arise after repeated cycles of killing (during treatment) and re-growth after treatment. When patients are medicated repeatedly, the mutant strain becomes dominant. 15 This could support the suggestion that drug resistance results mainly from poor treatment adherence. 35 Furthermore, in the present study, the proportion of RR-MTB was high among previously treated cases (31.6%) when compared to naïve cases (3.1%). This is in line with studies conducted in Debre Markos 5 and Addis Ababa 30 hospitals of Ethiopia. This suggests that previously treated patients were more likely to harbor drug-resistant strains 2 and it also shows the weakness in TB prevention and control measures in the study area. 15 This present finding has significant relevance in the current global efforts to accurately and timely diagnose MDR-TB with the scale up of molecular technology like Gene Xpert MTB/RIF, providing quick results of rifampicin resistance as a proxy to MDR-TB.
The present study also revealed an association between tobacco chewing and RR-MTB development. A study conducted in China indicated that tobacco chewing is a reversible potential factor for the development of drug-resistant M. tuberculosis. 36 Furthermore, tobacco chewing is shown to reduces the successful treatment outcome of anti-TB treatment. 37 Tobacco-addicted patients are less likely to complete anti-TB treatment and this finally participates in the development of drug-resistant TB strain. 38
In this study, a lower monthly income of the family was significantly associated with RR-MTB. This is in line with a study conducted in Brazil which indicated that low socioeconomic status can increase the treatment abandonment rate which consequently participates in the acquisition of drug-resistant TB strain. 37 In addition to this, low socioeconomic status increases the chance of contracting TB resistant strains as such low socioeconomic status communities don’t have access to good medical services.
The present study also revealed an association between being asthmatic and the development of RR-MTB. This could have happened because asthma can cause dysregulation of host defense functions. It damages the lungs and reduces anti-TB treatment efficacy. 39
In the current study, age was not associated with RR-MTB. However, previous studies associated age with RR-MTB. A study conducted in South Africa reported that those patients who have age greater than 40 years were six times more likely to have RR-MTB than those who have age <40 years. 40 The lack of association between age and RR-MTB could be due to differences in the mean age of study participants in different studies.
In this study, gender was not also associated with RR-MTB. This could have been since men and women are exposed equally to factors that lead to rifampicin resistance in Mogadishu. However, the drug-resistance is slightly predominated among males (6.5%) when compared to females (5.6%) and this could be a difference in medical treatment-seeking behavior. This is similar to studies conducted in India 41 and Zambia. 42
Strengths and limitations
Among the strengths of this study is that it provides an overall picture of the prevalence of RR-MTB using the newly endorsed method Gene Xpert MTB/RIF assay and associated factors among presumptive TB patients in Mogadishu TB centers. Nevertheless, the limitation of the study was related to its study design and sampling technique. The cross-sectional study design could not clearly define the cause-and-effect relationship. The convenient sampling technique limits the generalizations of the research findings beyond the population under the study. Therefore, the findings of this study should be interpreted within these limitations.
Recommendations
The Mogadishu regional bureau should emphasize the preventive and controlling strategies of drug-resistant TB by continuous surveillance of drug resistance TB trends and prevent the development of new cases of RR-MTB. The office should also provide broad-scale health education and awareness-building programs to the communities on drug-resistant TB and the health effects of tobacco chewing. Furthermore, the office should give special attention to the poor and vulnerable groups who face barriers to accessing TB services, especially, those in low socioeconomic status.
Conclusions
In this study, the overall magnitude of RR-MTB was 35% and it is very high when compared to most studies conducted in the neighboring countries, Ethiopia and Kenya. Furthermore, this result implies that the country faces a great risk of joining the 20 countries with the highest estimated number of RR-MDR-TB incidents in the world. Having previous anti-TB treatment, a monthly income of less than $100 USD, the habit of tobacco chewing, and being asthmatic are significantly associated with RR-MTB development.
Supplemental Material
sj-docx-1-smo-10.1177_20503121221148603 – Supplemental material for Rifampicin resistant Mycobacterium tuberculosis and associated factors among presumptive pulmonary tuberculosis patients in Mogadishu, Somalia
Supplemental material, sj-docx-1-smo-10.1177_20503121221148603 for Rifampicin resistant Mycobacterium tuberculosis and associated factors among presumptive pulmonary tuberculosis patients in Mogadishu, Somalia by Mohamed Muhumed Ali, Fitsum Weldegebreal, Getachew Kabew and Kedir Urgesa in SAGE Open Medicine
Footnotes
Acknowledgements
We acknowledged Haramaya University Colleges of Health and Medical Sciences Institutional Health Research Ethical Review Committee for giving the ethical clearance. We also thank study participants and all individuals who have in one way or another contributed to the completion of this research.
Author contributions
All authors made significant contributions to the work reported, whether that be in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising, or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics approval
This study was performed under the international (Helsinki) and Ethiopia research regulations. Ethical clearance was obtained from Haramaya University, College of Health and Medical Sciences through the Institutional Health Research Ethics Review Committee (IHRERC) Ref. No. IHRERC/034/2021.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Informed written consent or thumb print consent was obtained from the study participants. Thumbprint mode of informed consent is the form of the sign given by individuals who could not write and read. They put their finger/thumb prints as written signatures. This form of giving consent is equally approved by the ethical committee as written signed consent. Study subjects were given information about the objectives of the study and informed written consent for minor subjects of the age group above 15 years is according to the country’s regulations. Accordingly, Haramaya University, Health, and Medical science college, Institutional Review Board/Ethics Committee waived for the subjects in the age group of 15 to 18. Our study subjects are not aged less than 15 years old and do not require additional consent from their representative.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
