Abstract
Objectives:
We aimed to establish a new reference interval of blood cell parameters by classifying and counting blood Cells of 16- to 85-year-old healthy volunteers and observing continuous changes with age.
Methods:
We analyzed the blood cell parameters of 42,678 cases (men, 24,406; women, 18,272), and compared the blood cell parameters of men and women in different age groups using an independent samples t-test. Using limits of 2.5%–97.5%, a 90% confidence interval was used to develop new reference intervals.
Results:
Counts of blood cell parameters, including white blood Cells, neutrophils, lymphocytes, monocytes, eosinophils, basophils, red blood Cells, hemoglobin, hematocrit, distribution width of red blood Cells and platelets, were found to differ between men and women in different age groups. These parameters were used to establish a new reference interval of blood Cells.
Conclusion:
The blood cell parameters of both men and women changed with increasing age. The reference interval that we established will provide more accurate basic evidence for clinical diagnosis and treatment of diseases.
Introduction
Blood cell parameters, which play an important role in the clinical diagnosis and treatment of disease, are strongly affected by factors such as geographical region and gender. There are significant differences in blood cell parameters, such as white blood cells (WBCs) and hemoglobin (HGB), at different altitudes, 1 and hypoxic environments affect the volume of red blood cells (RBCs) 2 and amount of HGB. 3 Oxygen levels at the average altitude of Yuxi City, Yunnan Province, China (1700 m) are different from those in China’s low altitude areas. There is no relevant literature describing continuous changes in the levels of various blood cell parameters in the population of this area, and a local clinician asked the clinical laboratory to provide accurate reference intervals for various blood cell parameters. In this study, therefore, we established accurate reference intervals by investigating continuous changes in various blood cell parameters in healthy individuals between 16 and 85 years old in the local region.
Methods
Study population
In 2016, we visited each health consultation center in Yuxi City and recruited 48,821 volunteers from different areas of the city and from different industries to participate in the study. Details of fever, allergies, medical history, medication, height, weight, head circumference, waist circumference and chest circumference were recorded for each participant. Exclusion criteria were in accordance with the Chinese “Clinical Laboratory Test Project Reference Standards” and the standards document of US CLSI C28-A3 4 and included history of marriage with Caucasians or black people for three generations, cardiovascular disorders (thalassemia, acute blood loss, unexplained low HGB, abnormal blood pressure), malignant tumors, severe traumatic burns, tuberculosis, autoimmune diseases, severe dysfunction of the digestive or urinary system, long-term use of antibiotics or hormones, pregnancy, lactation, long-term or recent blood donation, drug use, smoking, abuse of vitamins, obesity, special occupations, alcohol abuse and surgery within the past 2 weeks.
This is a retrospective study. The number of individuals less than 15 years old (including 15-year-olds) and more than 86 years old (including 86-year-olds) who met the inclusion criteria was insufficient for statistical analysis (less than 30 cases). Therefore, only 16- to 85-year-olds (24,406 men, mean age 43 ± 13 years and 15,562 women, mean age 39 ± 14 years) were included in the study. In order to better analyze continuous changes in blood cell parameters, we divided the 16- to 85-year-old participants into 14 age groups, at 5-year intervals, calculated the mean and standard deviation for each group, and then compared differences between men and women in each age group.
Sample collection and handling
Sample testing was carried out in the clinical laboratory of Yuxi People’s Hospital and was strictly in accordance with the standard (ISO15189: 2012, China) for specimen testing. All analysts were certified Chinese laboratory technicians and were qualified for preservice training. Appropriate reagents and quality control products were used. The laboratory test system is calibrated and validated every 6 months. High, medium and low internal quality control (IQC) is carried out daily. The laboratory guarantees that the external quality assessment (EQA) score is >98/100 points and that the quality performance of the laboratory is satisfactory in both external and internal quality assurance. Venous blood samples (2 mL) were collected using a vacuum tube containing dipotassium edetate (EDTA-K2) anticoagulant and, to avoid the influence of food on blood cell parameters,5,6 the samples were collected in the morning after an 8-h overnight fast. Immediately after collection, the blood samples were shaken up and down eight times. WBC, neutrophils (NEUT), lymphocytes (LYMPH), monocytes (MONO), eosinophils (EO), basophils (BASO), RBC, HGB, red blood cell distribution width (RDW), hematocrit (HCT) and platelets (PLT) were then measured using an XN-9000 blood cell analyzer (Sysmex Corporation, Kobe, Japan).
Statistical analysis
SPSS 22.0 software was used for statistical analysis, a box chart was used to eliminate outliers and a P-P chart and frequency histogram distribution were used to test the normality of all data. An independent sample t-test was used to compare blood cell parameters of men and women. The significance of an increasing or decreasing trend was calculated separately for men and women using the Jonckheere–Terpstra test. Using limits of 2.5%–97.5%, a 90% confidence interval was used to develop new reference intervals.
Results
Comparison of men and women aged 16–85 revealed significant differences (p < 0.01) in levels of various blood cell parameters. Different age groups showed statistically significant differences in different parameters (Tables 1 and 2). We divided the 16- to 85-year-olds into 14 groups, with a 5-year age span in each group, and drew a box chart of blood cell parameters for each group (Figure 1). We compared differences in blood cell parameters between men and women in the same age group (Tables 1 and 2) and calculated continuous changes for each blood cell parameter according to the average value for each group. In men, WBC count, NEUT, LYMPH and MONO increased with increasing age and peaked at 46–60 years. Levels of RBC, HGB, HCT and PLT in men decreased with increasing age. In women, WBC count, NEUT and LYMPH decreased with increasing age. Except for MONO, EO and BASO, all other blood cell parameters showed peaks or troughs to different degrees. The levels of red blood cell distribution width-standard deviation (RDW-SD) and red blood cell distribution width-coefficient of variation (RDW-CV) increased with increasing age. Each parameter showed a continuous increase or decrease, and the Jonckheere–Terpstra test results are shown in Table 3. The reference intervals developed in this study are shown in Table 4.
Comparison of blood cell parameters between men and women (aged between 16 and 55 years).
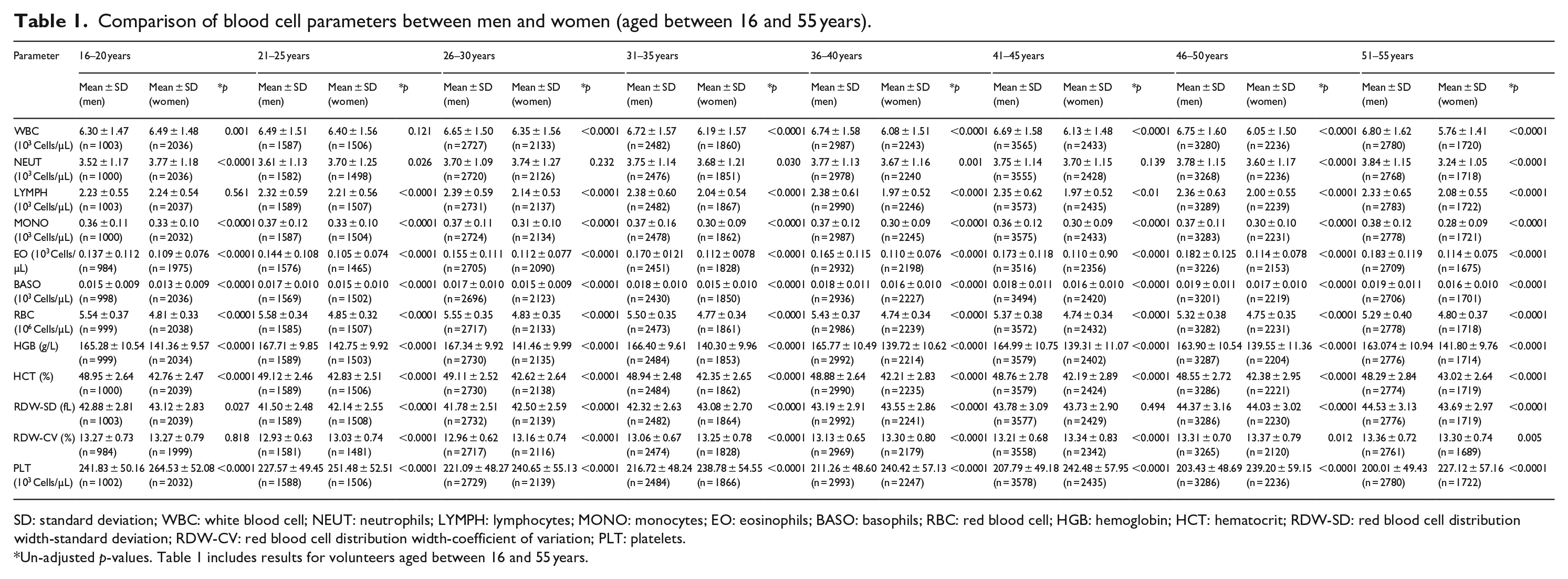
SD: standard deviation; WBC: white blood cell; NEUT: neutrophils; LYMPH: lymphocytes; MONO: monocytes; EO: eosinophils; BASO: basophils; RBC: red blood cell; HGB: hemoglobin; HCT: hematocrit; RDW-SD: red blood cell distribution width-standard deviation; RDW-CV: red blood cell distribution width-coefficient of variation; PLT: platelets.
Un-adjusted p-values. Table 1 includes results for volunteers aged between 16 and 55 years.
Comparison of blood cell parameters between men and women (aged between 56 and 85 years).

SD: standard deviation; WBC: white blood cell; NEUT: neutrophils; LYMPH: lymphocytes; MONO: monocytes; EO: eosinophils; BASO: basophils; RBC: red blood cell; HGB: hemoglobin; HCT: hematocrit; RDW-SD: red blood cell distribution width-standard deviation; RDW-CV: red blood cell distribution width-coefficient of variation; PLT: platelets.
Un-adjusted p-values. Table 2 includes results for volunteers aged between 56 and 85 years.

Changes in blood cell levels with age in men and women.
Jonckheere–Terpstra test results, calculated separately for men and women (14 groups).

WBC: white blood cell; NEUT: neutrophils; LYMPH: lymphocytes; MONO: monocytes; EO: eosinophils; BASO: basophils; RBC: red blood cell; HGB: hemoglobin; HCT: hematocrit; RDW-SD: red blood cell distribution width-standard deviation; RDW-CV: red blood cell distribution width-coefficient of variation; PLT: platelets.
Un-adjusted p-values. All parameters tended to increase or decrease. The increasing or decreasing trend of some parameters was different in men and women.
Reference interval (aged between 16 and 85 years).

CI: confidence interval; WBC: white blood cell; NEUT: neutrophils; LYMPH: lymphocytes; MONO: monocytes; EO: eosinophils; BASO: basophils; RBC: red blood cell; HGB: hemoglobin; HCT: hematocrit; RDW-SD: red blood cell distribution width-standard deviation; RDW-CV: red blood cell distribution width-coefficient of variation; PLT: platelets.
Discussion
In this study, we analyzed continuous changes in blood cell parameters with increasing age in a healthy population, and established reference intervals for blood cells in the local population, which will provide a reliable reference for the diagnosis and treatment of diseases. This study shows that the WBC count of men is higher than that of women, indicating that men can mobilize more WBCs in the peripheral blood than women. A large WBC count contributes to the body’s resistance to inflammation, but in acute inflammation, excessive WBCs may participate in the inflammatory response and cause harm to the body. Compared with results reported in the literature, 7 overall levels of WBC, NEUT, LYMPH, MONO, RBC, HGB, HCT and RDW were higher than in Africans or Caucasians, but the overall number of PLT was lower than in Africans or Caucasians. It is unclear whether these differences are attributable to ethnicity or geographical location. In the present study, we found that, in addition to MONO, EO and BASO, all blood cell parameters in menopausal women (41–50 years old) had different peaks and troughs, whereas in men, WBC, NEUT, LYMPH, MONO and EO had different peaks in 46- to 60-year-olds. These differences may be related to estrogen levels and life cycle regulation. It seems most reasonable that the reference interval should be adjusted continuously, according to the level of blood cell parameters.
RBC, HGB and PLT levels in men and women in the study group were significantly higher than those in individuals living in low altitude areas of China,8–10 which may be attributable to the increase in RBC caused by high altitude hypoxia.11,12 In this study, the continuous changes in RBC and HGB levels in men and women are similar to those in other regions in China. 13 The year-on-year decrease in HGB in men is similar to that seen in Nordic men. Levels of HGB in women, on the other hand, fluctuate within a certain range, whereas levels of HGB in Nordic women increases year-on-year. 14 A report from Canada 15 shows that HCT levels in men and women gradually increase with age, while our study suggests that HCT in men and women gradually decreases with age. This difference may be due to ethnicity and/or geographic location. RDW-SD and RDW-CV, which indirectly reflect the volume of RBC, have not been taken seriously for a long time, but they are very important parameters of RBC. Changing estrogen levels are reported to lead to changes in numbers of RBC in women, 16 and this study also showed that changes in estrogen levels may affect numbers of RBC. RBC strongly influences HGB and, since HGB and RDW 17 are positively correlated over a certain age range, changes in RDW may be related to changes in estrogen levels. RDW is an independent predictor of coronary atherosclerosis, and also has some significance in the diagnosis of anemia18,19 and coronary atherosclerosis.20,21
This study has some limitations. Individuals of 15 years or less and individuals of 86 years or more were not included in the study because of insufficient sample size. In addition, the sample size selected in this study was not calculated, but selected as far as possible, and the study includes only residents of Yuxi City and the results reflect only levels of blood cell parameter in the local population. This may have an impact on the results. In a future study, we will calculate the sample size and increase the number of individuals under 15 years old and over 86 years old, and also include individuals from other provinces and cities to make up for these deficiencies.
Conclusion
RBC parameters are affected by both age and gender. We have established reference standards that can provide better evidence-based guidance for the diagnosis and treatment of diseases. Our results provide the basis for further calibration of reference standards.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Ethical approval for this study was obtained from the Review Board of the People’s Hospital of Yuxi City Yunnan Province, China (approval number/YX-20160428).
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by the Regional Fund Project of the National Natural Science Foundation of China (Serial number: 81460326), the Joint Special Funds from the Yunnan Province Science and Technology Department and Department of Applied Basic Research of Kunming Medical University (Serial number: 2018FE001-081) and the Special Funds for Training High-level Health Technical Talents in Yunnan Province (Serial number: D-201644). The funding did not influence the study design, the collection, analysis, and interpretation of data, the writing of the report, or the decision to submit the article for publication.
Informed consent
Written informed consent was obtained from all subjects before the study. Both adults and minors had the ability to make decisions. We obtained written informed consent from the legally authorized representatives of all minors (in addition to the assent of the minor) prior to initiation of the study.
