Abstract
Background:
A growing interest in long-term sequelae of COVID-19 has prompted several systematic literature reviews (SLRs) to evaluate long-COVID-19 effects. However, many of these reviews lack in-depth information on the timing, duration, and severity of these conditions.
Objectives:
Our aim was to synthesize both qualitative and quantitative evidence on prevalence and outcomes of long-term effect of COVID-19 through an umbrella review.
Design:
Umbrella review of relevant SLRs on long-COVID-19 in terms of prolonged symptoms and clinical conditions, and comprehensively synthesized the latest existing evidence.
Data Sources and Methods:
We systematically identified and appraised prior systematic reviews/meta-analyses using MEDLINE, Embase, and Cochrane database of systematic review from 2020 to 2021 following the preferred reporting items for systematic reviews and meta-analyses guidance. We summarized and categorized all relevant clinical symptoms and outcomes in adults with COVID-19 using the Medical Dictionary for Regulatory Activities System Organ Class (MedDRA SOC).
Results:
We identified 967 systematic reviews/meta-analyses; 36 were retained for final data extraction. The most prevalent SOC were social circumstances (40%), blood and lymphatic system disorders (39%), and metabolism and nutrition disorder (38%). The most frequently reported SOC outcomes within each MedDRA category were poor quality of life (59%), wheezing and dyspnea (19−49%), fatigue (30−64%), chest pain (16%), decreased or loss of appetite (14–17%), abdominal discomfort or digestive disorder (12−18%), arthralgia with or without myalgia (16–24%), paresthesia (27%) and hair loss (14–25%), and hearing loss or tinnitus (15%).
Conclusion:
This study confirmed a high prevalence of several long COVID-19 outcomes according to the MedDRA categories and indicated that the majority of evidence was rated as moderate to low.
Registration:
The review was registered at PROSPERO (https://www.crd.york.ac.uk/prospero/) (CRD42022303557).
Introduction
Severe Acute Respiratory Syndrome Coronavirus-2 (SARS-CoV-2), the causative pathogen for the coronavirus 2019 (COVID-19) disease first emerged in 2019 and began to spread quickly resulting in significant mortality and morbidity globally1,2 and the World Health Organization declaring it a worldwide pandemic in 2020. 1
The range of documented COVID-19 clinical symptoms vary from asymptomatic to severe. A recent systematic literature review (SLR) indicated that overall, the majority of patients with COVID-19 disease experience asymptomatic or mild-to-moderate acute symptoms, whereas approximately 15% of patients are estimated to progress to more severe symptoms requiring hospitalization. Around 5% become critically ill and some patients who have recovered continue to have lasting effects of the disease. 3
As of May 2022, over 525 million confirmed cases of COVID-19 disease were reported worldwide 4 of which one in seven remained symptomatic at 12 weeks, suggesting the number of ‘long haulers’ or patients with long-COVID-19 is likely considerable. 5 The data from June 2022 collected by Centers for Disease Control and Prevention indicate, 6 1 in 13 adults in the United States have long-COVID-19 symptoms, defined as new symptoms lasting three or more months after first contracting the virus. A recent global survey of people with suspected and confirmed COVID-19 disease suggested that long-COVID-19 is composed of heterogeneous sequelae that often affect multiple organ systems beyond 4 weeks from the onset of symptoms, with significant impacts on functioning and overall quality of life; however, there is no universally accepted case definition for long-COVID-19 disease.7,8 Many factors contribute to difficulties in fully exploring the long-term impact of COVID-19 including lack of a universal definition of long-COVID-19, evolving clinical features due to different variants, onset of symptoms, and differences in reporting of symptoms.
Due to significant potential health, economic, and societal implications of long-COVID-19, there recently have been several research initiatives 9 to enhance knowledge on long- COVID-19. A growing interest in long-term sequelae of COVID-19 has prompted several SLRs to evaluate long-COVID-19 effects. However, many of these reviews lack in-depth information on the timing, duration, and severity of these conditions.
Therefore, given the critical need to synthesize a growing body of literature and provide clarity on the most important long-COVID-19 health concerns, we conducted an umbrella review of relevant SLRs on long-COVID-19 in terms of prolonged symptoms and clinical conditions, and comprehensively synthesized the latest existing evidence.
Methods
Study protocol
This umbrella literature review was performed in accordance with the guidelines defined in the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA). 10 The study protocol was registered in the International Prospective Register of Systematic Reviews (PROSPERO; CRD42022303557).
Search strategy and data sources
We conducted a protocol-based systematic search using electronic databases through Ovid in MEDLINE, Embase and Cochrane Database of Systematic reviews, and Biosis Previews on 14 January 2022. A list of search terms relating to COVID-19 persistent symptoms and systematic review was employed, with results restricted to English language articles published since 2019. The complete search strategy is in the Supplemental Table 1. We applied hand searching and cross referencing as needed. We did not search gray literature and preprints.
Screening, inclusion criteria, and study selection
Dual-process screening was individually conducted by paired reviewers (JX/DB, FI/MG, HL/RB, FR/BT, JR/MG), with any disagreements in screening resolved during consensus with senior reviewers (YS/HL). Titles and abstracts of the identified articles using the search strategy were individually screened. Studies that included relevant information on the Population, Intervention, Comparator, Outcomes, Timeframe, and Study Design/Setting (PICOTS) according to inclusion criteria (Supplemental Table 2), were carried forward to the full-text review. All studies that were considered out of scope based on the inclusion criteria during the full-text review were excluded with a documented rationale.
Studies included in the final extraction met the following criteria: (1) Population – adults (⩾18 years) who developed long-term complications after being infected with SARS-CoV-2; (2) outcomes – any long-term effects attributable to COVID-19; (3) study design – any systematic review or meta-analysis with the objective of assessing long-term COVID 19. Detailed information about inclusion and exclusion criteria is provided in Supplemental Table 2.
Data extraction
We developed a standardized data extraction spreadsheet form prior to data collection via Microsoft Excel. Paired reviewers (JX/DB, FI/MG, HL/RB, FR/BT, JR/MG) extracted study data independently. Any disagreements in data extraction were resolved during consensus with a third senior reviewer (HL). First, reviewers extracted information on study level: study details (including authors, publication type, year of publication and study design); the definition of long-COVID-19; type of population (general and/or special patient population); principal outcome domain; settings at hospitalization or not; countries included within the studies of the SLR; and the year range of review of primary studies within the SLR. Reviewers extracted information on outcome level: time at assessment of the outcomes; duration of the condition since outcome onset; severity of COVID-19 infection; severity of disease outcome; number of studies included in SLR which reported the outcome; number of total patients included in the SLR; number of patients with a specific outcome; reported or estimated prevalence of an outcome and meta-analysis with effect size (mean difference, relative risk, incidence or prevalence). Outcomes were properly standardized using the Medical Dictionary for Regulatory Activities (MedDRA) version 25 (Supplemental Table 3). There are three major types of 27 MedDRA System Organ Classes (SOCs) in MedDRA 11 : (1) Etiology-based SOCs [such as SOC Congenital, familial and genetic disorders; SOC Infections and infestations; and SOC Neoplasms benign, malignant, and unspecified (incl cysts and polyps)]; (2) Disease manifestation site-based SOCs [such as SOC Gastrointestinal (GI) disorders]; and (3) Supporting SOCs (such as SOC Investigations, SOC Social circumstances, and SOC Surgical and medical procedures).
Data synthesis
For each mapped MedDRA SOC, we summarized the overall prevalence rate according to the reported prevalence of the corresponding outcome. If the measure was not reported, we estimated it by dividing the number of persons having the specific outcome by the total number of persons in the included component study. We also collected the reported prevalence of the outcome during each pre-specified assessment time interval, including 1–2 months, 3–4 months, 5–6 months, >6 months after diagnosis, symptom onset, or hospitalization. If the included reviews did not report the prevalence for a specific time interval, then depending on the reported time of the outcome assessment, we used the value of overall prevalence rate to impute the missing data. To evaluate the trend in the prevalence of each MedDRA SOC over time, a mean of the time-specific prevalence was calculated based on all available non-missing data points (either reported or imputed) for a given time interval. We used line graphs to visually compare patterns of mean prevalence across all MedDRA SOCs for all patients without COVID-19 severity distinctions, hospitalized patients, and non-hospitalized patients, respectively.
For included component studies with reported results from meta-analyses, summary effect size (i.e. pooled prevalence and relative risk) were extracted for each outcome. We created forest plots to illustrate the estimates of effect size for the most common outcomes stratified by MedDRA SOC, including cardiac disorders, eye disorders, ear and labyrinth disorders, psychiatric disorders, and fatigue.
Quality assessment
The quality assessment of included studies was evaluated by the GRADE-CERQual and AMSTAR tools to assess the methodological quality of included SLR.12,13 We used the GRADE-CERQual approach to assess how much confidence to place in findings from individual SLR of qualitative research or qualitative evidence synthesis. This approach evaluates findings on four criteria: (1) methodological limitations of included studies supporting a review finding; (2) the relevance of included studies to the review question; (3) the coherence of the review finding; and (4) the adequacy of the data contributing to a review finding. 13
We used the AMSTAR 2 tool to evaluate methodological quality of the included SLRs and/or meta-analyses. 12 The tool includes 16 items and has an overall ‘rating’ based on weaknesses in critical domains. A high score may disguise critical weaknesses in specific domains, such as a failure to assess Risk of Bias within individual studies that were included in a SLR. Of these 16 domains, seven can particularly affect the validity of the review and its conclusion and are considered ‘critical domains’ (2, 4, 7, 9, 11, 13, and 15), which may greatly weaken the confidence that can be placed in a SLR. Both the GRADE-CERQual and AMSTAR 2 assessments were evaluated independently by two reviewers with all disagreements resolved by a third senior reviewer.
Results
Systematic literature search
Figure 1 displays details of the literature search and study selection. After a comprehensive electronic literature search, 967 SLRs/meta-analysis were identified through the following libraries: MEDLINE (N = 418), Embase (N = 430), Biosis (N = 105) and Cochrane SLRs (N = 14). Duplicated records (N = 430), records marked as ineligible for being animal studies or other irrelevant publication types such as case report, case studies, editorial, comment, historical article, and conference abstract (N = 71), and records in non-English or published prior to 2020 (N = 13) were removed. A total of 453 records were retrieved for title and abstract review, of which 355 were excluded for various reasons. The remaining 96 studies were subjected to a full-text review, among which a total of 36 articles (20 SLRs/16 meta-analyses) were retained in this umbrella review for final data extraction.3,14

Preferred reporting items for systematic reviews and meta-analyses flow diagram.
Study characteristics
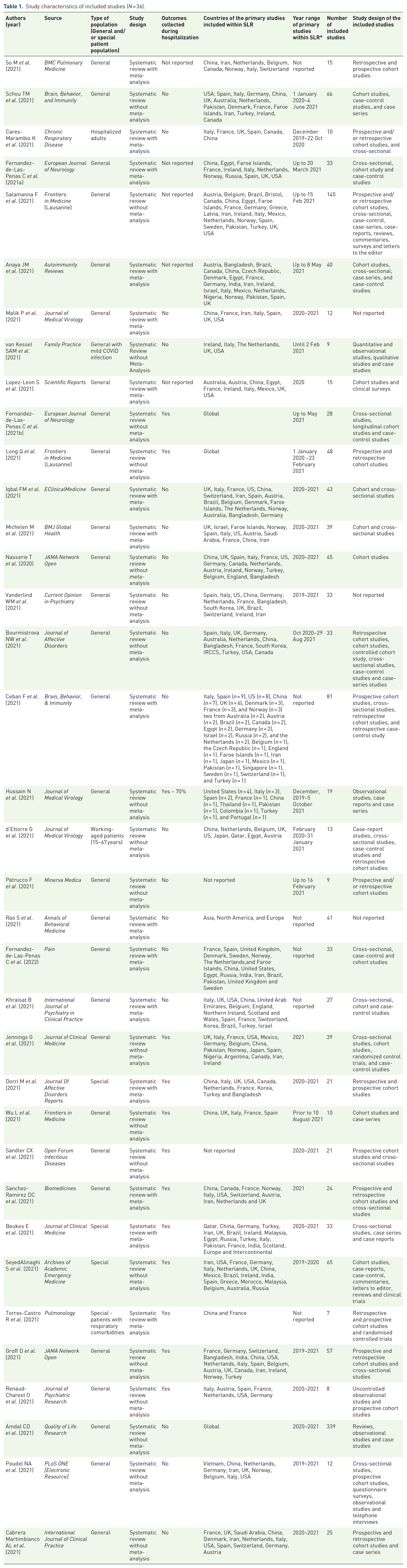
Table 1 describes the characteristics of the 36 included studies. Overall, the population included general patients, and for the majority of the studies, most of the outcomes were not collected during hospitalization. Two studies focused on a special population that included patients with pre-existing health conditions 16 or patients with respiratory comorbidities. 46 The number of included primary studies varied between 7 and 339 where China (N = 29), UK (N = 28), Italy (N = 28), France (N = 27) and USA (N = 20) were the most reported countries. The study design of these primary studies mainly included prospective and/or retrospective cohorts (N = 33), cross-sectional studies (N = 19), case-control (N = 13), case series (N = 8), case-reports (N = 5) and randomized clinical trials (N = 2).
Study characteristics of included studies (N = 36).
Overall prevalence of conditions over time
Figure 2(a) shows the estimated average prevalence of each outcome across all reported studies over the four assessment time intervals based on available data. Of those, the three most prevalent MedDRA SOC reported among the entire patient population were social circumstances (40%), blood and lymphatic system disorders (39%), and metabolism and nutrition disorder (38%) at initial 1–2 months after COVID-19 diagnosis, symptom onset, or hospitalization. An initial decrease in the prevalence of social circumstances was observed between 1 and 2 months and 3 and 4 months post-COVID-19/hospitalization, followed by a slight increase from 35.0% at 3 to 4 months to 38.4% at 5–6 months. As a supporting SOC social circumstances, the reported outcomes following long-COVID we have identified (e.g. poor quality of life, disability, functional impairment) could inform health-care strategies and decision-making for long-term care among ‘long haulers’. In contrast, there was a steep decline in the prevalence of blood and lymphatic system disorders (12% at 3–4 months) and metabolism and nutrition disorder (7.9% at >6 months) after symptom onset or hospitalization.

(a) Prevalence of outcomes by MedDRA SOC by time at assessment: Overall. (b) Prevalence of MedDRA SOC by time at assessment and severity of COVID-19 among hospitalized patients. (c) Prevalence of MedDRA SOC by time at assessment and severity of COVID-19 among non-hospitalized patients.
Among the remaining reported conditions, we found an overall rising trend in the prevalence of general disorders and administrative site conditions, investigations, ear and labyrinths disorders, respiratory, thoracic and mediastinal disorders, and GI disorders over 6 months or more after COVID-19 diagnosis or hospitalization. In particular, investigations SOC prevalence rose substantially from 9.9% at 1 to 2 months to 45.4% at 5–6 months despite a subsequent decline. Similar to the SOC social circumstances, the SOC investigations also support health care management and decisions by administering clinical laboratory tests and other medical procedures, which may help determine a diagnosis and monitor a medical condition over time. In the present study, the reported outcomes in the SOC investigations among ‘long haulers’ identified from the published reviews include pulmonary function test abnormalities, spirometry alterations, chest imaging abnormality, and elevations of inflammation markers (Supplemental Table 4). The prevalence of respiratory, thoracic, and mediastinal disorders increased during the first 4 months and then stabilized thereafter. Conversely, the prevalence of nervous system disorders decreased from 23.9% at 1 to 2 months to 14.5% at >6 months after COVID onset or hospitalization. The prevalence of psychiatric disorders and cardiac disorders remained mostly stable up to more than 6 months following COVID infection or hospital discharge, whereas we observed variations in the prevalence of musculoskeletal and connective tissue disorders and skin and subcutaneous tissue disorders showing an increase and then a decline in rates over time. After 6 months, general disorders and administrative site conditions (36.4%), investigations (29.2%), and psychiatric disorders (25.0%) are the three most common MedDRA SOC.
We further stratified the patient population according to hospitalization status. Figure 2(b) presents estimated prevalence of MedDRA SOC for each assessment time interval among hospitalized patients. There was an increase in the prevalence of GI disorders, whereas the prevalence of skin and subcutaneous tissue disorders and investigations decreased starting 3–4 months after COVID-19 infection, symptom onset, or discharge. The prevalence of general disorders and administration site conditions, respiratory, thoracic and mediastinal disorders, musculoskeletal and connective tissue disorders, and nervous system disorders declined after the preceding increase. Among non-hospitalized patients, the prevalence of psychiatric disorders slightly decreased from 30.1% at 1 to 2 months to 24.1% at >6 months [Figure 2(c)].
Prevalence reported in meta-analysis
Figure 3 and Supplemental Table 3 summarize the meta-analyses prevalence/percentage of patients with an outcome or condition according to MedDRA SOC categories. List of detailed clinical symptoms and conditions associated with MedDRA SOC is included in Supplemental Table 4.

(a) Meta-analysis results of prevalence estimates of conditions within MedDRA SOC: cardiac disorders. (b) Meta-analysis results of prevalence estimates of conditions within MedDRA SOC: psychiatric disorders. (c) Meta-analysis results of prevalence estimates of conditions within MedDRA SOC: fatigue.
We found high levels of heterogeneity across the study results, yielding wide prevalence estimate ranges for most outcomes. The prevalence of dizziness, chest pain, and palpitations within cardiac disorders varied substantially between different meta-analysis results; overall the prevalence was less than 20% each [Figure 3(a)] whereas with respect to the four most common conditions within the psychiatric disorder category, almost a third of patients had at least one of psychiatric/mental health-related outcomes, including anxiety, depression, post-traumatic stress disorder (PTSD), and sleep disorders [Figure 3(b)]. A total of 10 meta-analyses summarized the prevalence of fatigue [Figure 3(c)]. Although the results were inconsistently reported, almost all were above 30%, with the majority reported as fatigue alone (eight meta-analyses; median, 38%; range, 30–64%) followed by fatigue with weakness or muscle weakness (two meta-analyses; median, 47%; and range, 46–47%).
The most frequent general disorders and administration site conditions were impaired mobility (14–36%), pain and/or discomfort (11–30%), walk/gait abnormality (4–26%). The most frequent social outcomes were poor quality of life assessed by EQ visual analouge scale (EQ-VAS) (59%, 95% CI, 42–74%) and decreased functional capacity (36%, 95% CI, 22–49%) (Supplemental Table 3). The frequency of various reported outcomes by MedDRA SOC is described in detail in Supplemental Appendix 1.
Methodological quality assessment
AMSTAR 2
An overview of methodological quality of included SLRs is in Figure 4. The rating of overall confidence (OC) in the results ranged from high to critically low. Among the 36 SLRs, four studies had a high rating of OC,17,20,31,38 three studies had a moderate rating of OC,18,30,32 seven studies22,24,25,27,33,40,46 had a low rating of OC, and 22 studies3,14–16,19,21,23,26,28,29,34–37,39,41–45,47,48 had a critically low rating of OC in the results.
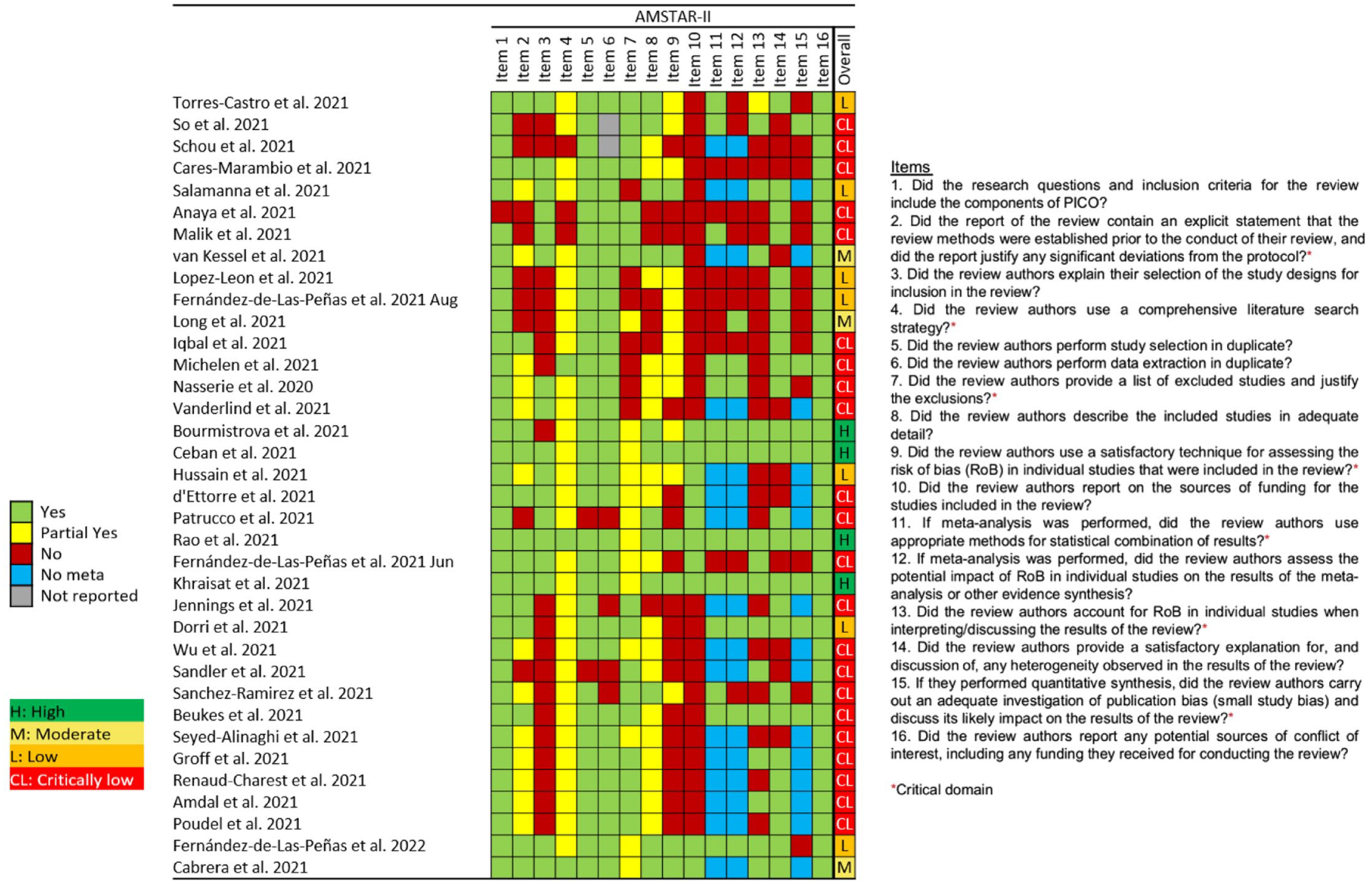
Quality assessment using the AMSTAR 2 tool.
All studies except one included the components of Population, Intervention, Comparison and Outcomes (PICO) (criterion 1). A total of 15 of the reviewed studies included an explicit statement that the review methods were established prior to the conduct of the review, while 13 studies partially fulfilled this criterion (criterion 2). Nearly half of the studies explained their selection of the study designs in the inclusion criteria (criterion 3). Nearly all studies performed study selection and data extraction in duplicate (criterion 5 and 6). A total of 16 studies provided a list of excluded studies and justified exclusion (criterion 7). A total of 6 studies did not describe the included studies in adequate detail (criterion 8) and 10 studies reported on the sources of funding for the included studies (criterion 10). All studies reported potential sources of conflict of interest (criterion 16).
GRADE-CERQual
Of the 36 SLRs, 9 studies had moderate confidence, 11 studies had low confidence and 16 studies had very low confidence as summarized in Table 2. Among the studies with moderate confidence, only two studies18,38 had no or minor concerns methodologically as the primary researchers used appropriate methods that were clearly reported. In four studies18,25,34,40 with moderate confidence, there were no or minor concerns with the patient population studied and long-COVID clinical outcomes were adequately defined. There were no or minor concerns of coherence in the patterns of individual study findings and the richness of the data in only one study. 40 This study included 145 individual studies of diverse study designs (cohort study, cross-sectional, case-report, cases-series, and case-control studies).
Confidence in review findings: GRADE-CERQual assessment.

Headache as an acute and post-COVID-19 symptom in COVID-19 survivors: a meta-analysis of the current literature.
Time course prevalence of post-COVID pain symptoms of musculoskeletal origin in patients who had survived to severe acute respiratory syndrome coronavirus 2 infection: a systematic review and meta-analysis.
Prevalence of post-COVID-19 symptoms in hospitalized and non-hospitalized COVID-19 survivors: a systematic review and meta-analysis.
Discussion
Several systematic reviews of the literature assessing long-COVID-19 have been performed recently but to the best of our knowledge, our study is the first global umbrella review to systematically and comprehensively synthesize evidence on long-term clinical and health outcomes following COVID-19 infection. Our umbrella review sheds more light on the understanding of long COVID-19 and its broader public health implications and brings more depth to the thinking that would eventually sharpen the case definition of long COVID-19.
Several critical findings of our umbrella review study bring important contributions to better understanding and characterization of long COVID-19. First, an important finding is that the three most common MedDRA SOC among the entire patient population were (1) Social circumstances (40%), which included care dependency, consequences for work, decrease in quality of life or usual activities or functional capacity, disability, functional impairment, impaired morbidities or general functioning, poor quality of life, etc.; (2) blood and lymphatic system disorders (39%); and (3) metabolism and nutrition disorders (38%) at initial 1–2 months after COVID-19 diagnosis, symptom onset, or hospitalization. While researchers published timely studies, we found that some key information was missing, such as time at assessment, severity or duration of persistent conditions to determine the healthcare impact due to prolonged COVID-19 symptoms.
Second, our findings also suggest that long COVID-19 negatively affected patients as ‘long haulers’ appeared to face substantial social challenges as they resumed their everyday activities after recovery. Our data confirmed and aligned to current knowledge that long-COVID-19 had a large impact on social measures; 59% of the post–COVID-19 patients had poor quality of life and 36% had decreased functional capacity. Despite different measures, previous studies reported consistently high impact on social outcomes across socially diverse groups.49,50 Notably, social impacts and supportive strategies and systems may vary among social groups, probably due to differences in roles in household or work environments or other capabilities and social resources. Further evidence is urgently needed to identify which groups disproportionately suffer from social impacts and inform public health policy makers.
Although a lack of clarity about the distinct cause of long-COVID-19 in each individual patient remains, there are some leading hypotheses about the theory, one of which is about the presence of persistent circulating plasma microclots that are resistant to fibrinolysis. 51 In addition, increased ferritin levels represent an important host defense mechanism during infection, 52 the idea that lingering viruses might be a cause of long-COVID symptoms. Other studies have also found that the SARS-CoV-2 antigen persistence in infected tissues serves as a basis for postacute COVID-19. 53
The third critical finding is that among conditions that were reported over time, there was no clear decreasing trend with the exception of metabolism and nutrition disorder. General disorders and administrative site conditions and psychiatric disorders were the two most reported MedDRA SOC at >6 months with prevalence estimates >20%. Previously published studies7,54,55 have examined the trend of long-haul COVID-19 symptoms/conditions but none of them have provided a SLR on all organ systems using MedDRA SOC terms. To the best of our knowledge, there have not been published SLR/meta-analyses that reported the trend of long-COVID symptoms at the MedDRA term level since our systematic search for reviews up to December 2021.
In the meta-analysis results of prevalence estimates of conditions within MedDRA SOC, we note several key findings that help us with characterization of long COVID-19. The prevalence of dizziness, chest pain, and palpitations within cardiac disorders varied substantially between different meta-analysis results; overall, the prevalence of each was less than 20%. Importantly, almost a third of patients had at least one of psychiatric/mental health-related outcomes, including anxiety, depression, PTSD, and sleep disorders. For each outcome, results varied significantly between the meta-analyses. Sleep disorders (11–47%), anxiety/depression (25–38%), anxiety (13–22%), depression (4.1–21%), and PTSD (9.1–43%) were very common. We also found a high prevalence of fatigue (above 30%), with the majority reporting fatigue alone followed by fatigue with weakness or muscle weakness. A recently published SLR also reported that the most common system was fatigue or muscle weakness 6–12 months after the COVID-19 infection, which is consistent with our findings. 56
Using AMSTAR 2 and GRADE-CERQual tools to evaluate methodological quality of and the confidence of evidence, we found that only 4 and 9 studies had a high and moderate rating of confidence in the results, respectively. This suggests that more high-quality SLRs are needed to increase the quality of evidence.
This study has several notable strengths. First, this is the first umbrella review to provide reliable and timely evidence on long-term clinical and health outcomes following COVID-19 infection, which includes 36 recently published meta-analyses and/or SLRs. To accomplish this, we conducted a comprehensive literature search with explicit eligibility criteria across several databases with articles subsequently screened for inclusion in this review. Second, selection, data extraction, and the quality assessment of included studies were performed by paired independent reviewers. Third, we used the established guidelines for SLRs (i.e. PRISMA statement), including the use of a pre-specified protocol and search criteria. Umbrella reviews represent one of the highest levels of evidence synthesis currently available and is becoming increasingly powerful in the comprehensive integration of accumulating literature. 57 Importantly to note, umbrella reviews have been developed to synthesize and appraise evidence in previously published SLRs/or meta-analyses and accommodate repetition and heterogeneity across the meta-analyses to allow for their comparison. 57 Fourth, we conducted a thorough evaluation on methodological quality and confidence of clinical evidence from the included SLRs published thus far by applying both the AMSTAR 2 and GRADE-CERQual tools.12,13
However, our study has several limitations. While it is out of the scope of umbrella reviews to review original studies, studies included in each meta-analysis/SLR are often not mutually exclusive. Thus, the findings could be influenced or driven by some studies. Also, it was not possible to adjust for bias confounding, for example, pre-existing conditions, or assess the attribution of these conditions to long-term COVID-19 because such information was not available in the original reviews. Moreover, there was not enough information on COVID-19 vaccine and/or anti-viral treatment among the studies that were identified in the review; thus, no further assessment of the impact of these potential determinants on long-term COVID-19 condition can be done. In addition, we limited the review to English-language publications within the searched bibliographic databases and excluded non-English publications. Lastly, this umbrella review does not necessarily reflect the most up-to-date overview of long-term COVID-19 as our literature search was conducted in 2022 and possible new data has emerged since.
Conclusion
The most frequent SOCs among the entire patient population were social circumstances, blood and lymphatic system disorders and metabolism and nutrition disorders. Despite many published SLRs/meta-analyses of long-COVID-19, only a few studies have reported full aspects of long-COVID-19 in terms of timing, duration, and severity and standardized outcomes. Most of the studies identified and described long-term COVID-19 effects based on symptoms or conditions while few studies adjusted for patients’ underlying conditions or assessed the attribution of these conditions to long-term COVID-19. Future high-quality studies are needed to understand the public impact of prolonged COVID-19 symptoms and medical conditions.
Supplemental Material
sj-docx-1-tai-10.1177_20499361231198335 – Supplemental material for Long-COVID-19 clinical and health outcomes: an umbrella review
Supplemental material, sj-docx-1-tai-10.1177_20499361231198335 for Long-COVID-19 clinical and health outcomes: an umbrella review by Hu Li, Jin Xia, Dimitri Bennett, Fatima Roque, Rujuta A. Bam, Ana Bárbara Tadeu Tavares, Mugdha Gokhale, Fidelia Ida, Jinnie Jiwon Rhee, Montse Soriano Gabarro and Yiqing Song in Therapeutic Advances in Infectious Disease
Footnotes
Acknowledgements
We would like to acknowledge all the authors of the included studies in this review and meta-analysis. We would also like to acknowledge Jinnie Jiwon Rhee for editorial support and assistance with this manuscript.
Declarations
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
