Abstract
Background:
Serious infections in persons who use drugs (PWUD) are rising. Dalbavancin, due to its extended half-life, offers an alternative treatment for patients in whom standard of care antibiotics are not feasible or practical, allowing for reduced hospital days and the avoidance of central line placement or the use of complex oral regimens.
Objectives:
We aim to describe the time and effort required for coordination of dalbavancin courses by outpatient registered nurses (RNs) and other outpatient parenteral antimicrobial therapy (OPAT) staff.
Design and methods:
We conducted a retrospective review of adult patients with documented substance use who received at least one dose of dalbavancin and quantified the number of interventions required by our OPAT RNs and other OPAT staff for coordination of dalbavancin courses. Additionally, detailed data on time spent per intervention were prospectively collected for a 1-month period.
Results:
A total of 52 patients with 53 dalbavancin courses were included. Most substance use was intravenous. Infectious diagnoses included bone and joint infections (61%) and endocarditis (7%), in addition to skin and soft tissue infections (19%). Infections were most commonly caused by
Conclusions:
The ease of dalbavancin administration does not eliminate the need for extensive RN coordination for successful administration of doses in the outpatient setting for PWUD. This need should be accounted for in program staffing to help increase successful dalbavancin course completion.
Keywords
Background
The opioid and amphetamine epidemics have a significant impact on healthcare systems in the United States. Nationally, rates of hospital admissions for serious infections among persons who use drugs (PWUD) continue to rise, having more than doubled between 2012 and 2017.
1
People who inject drugs (PWID) are at an increased risk for skin and soft tissue infections (SSTI), sepsis, bone and joint infections, endocarditis,
2
and are more likely to have infections due to methicillin-resistant
Dalbavancin, a long-acting lipoglycopeptide with once-a-week dosing, has potent activity against most gram-positive organisms, including MRSA, and is an enticing alternative to IV antibiotic regimens that require a PICC, daily dosing, and weekly lab monitoring, as well as some of the complex oral regimens mentioned above. The use of dalbavancin has been described as a viable alternative to standard of care daily IV antibiotics, 9 although ongoing clinical trials are needed to provide evidence of non-inferiority to standard of care for more complicated infections. 10 The simplified dosing regimen can result in reduced hospital length of stay and significant cost savings to the healthcare system, but the ambulatory care requirements when used for complex infections are poorly described. 9
We aim to describe the time and effort required for coordination of dalbavancin courses by outpatient parenteral antimicrobial therapy (OPAT) registered nurses (RNs) and other staff.
Methods
This is a multipart study with both retrospective and prospective data collection. First, we conducted a retrospective review of dalbavancin use between 1 April 2015 and 31 December 2019 for any patient with documented history of substance use (active or in any phase of recovery) by either ICD-10 or in chart notes, including alcohol use, defined in this article as PWUD. We identified all patients ⩾ 18 years of age who received ⩾1 confirmed dose of dalbavancin
Results
Of the 52 patients, a total of 53 dalbavancin courses were included with a mean age of 44.8 years (range 23–70 years), and 32% were female. The most common infectious diagnoses were non-vertebral bone and joint infection in 21 (40%) patients, vertebral osteomyelitis in 13 (25%) and endocarditis in 5 (9%) (Table 1). The most common causative organism was
Patient demographics.
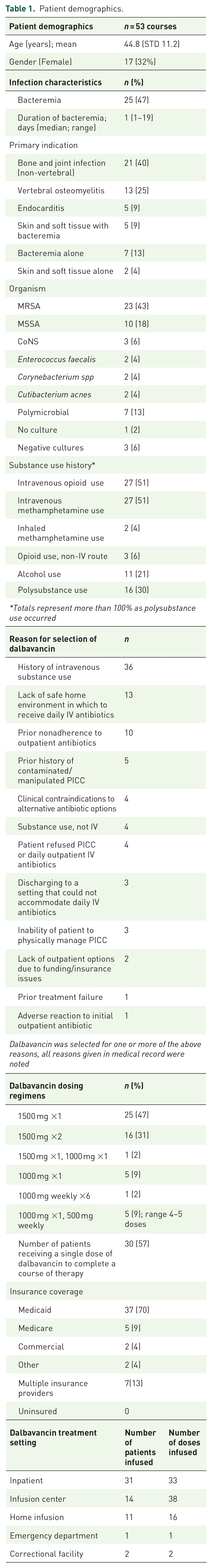
A total of 31 (58%) patients received at least one dalbavancin dose in the hospital, while 14 (26%) patients received their dalbavancin course entirely in the outpatient setting. Of those who received any inpatient dalbavancin, 24 (77%) patients completed their dalbavancin infusions in the hospital, and the remaining 7 (23%) required further outpatient doses. All 53 (100%) courses were ultimately completed.
OPAT RN interventions occurred in 32 (60.3%) of all dalbavancin regimens (Table 2). When comparing interventions by treatment setting, for courses completed inpatient, OPAT RN intervention was required for 6 (25%). For courses including at least one outpatient dose, OPAT RN intervention was required for 17 (77.3%). The most common interventions included reaching a patient by phone for coordination of infusion appointments or labs. There were a total of 171 RN interventions, with a mean of 3.35 interventions (STD 5.11) or median of 1 (range 0–31) per patient. For courses including at least one outpatient dose, there were a total of 143 RN interventions with a mean of 4.93 interventions (STD 5.98) or median 4 (range 0–31) per patient.
Study outcomes.

The 1-month prospective review of dalbavancin coordination time included seven patients. A total of 19 interventions and 179 min were devoted to dalbavancin coordination, with a mean of 8.9 min (STD 5.7) or median 7.50 (range 1–24) in RN intervention per patient dalbavancin course. The interventions requiring the most RN time in dalbavancin coordination included coordination of outpatient dalbavancin infusion appointments and attempting to reach patients for appointment and lab coordination.
As far as treatment outcomes, adverse reactions were documented for one (2%) patient, consisting of nausea, vomiting, and diarrhea following infusion but did not require hospital admission. A 90-day recurrence or relapse of infection occurred for two (4%) patients, both of whom were readmitted to the hospital. A 90-day mortality occurred for one (2%) patient.
Discussion
Dalbavancin is an attractive option for PWUD but to optimize success in this patient population with many barriers, diligent care coordination is required. Potential barriers for OPAT in PWUD include lack of access to a working phone, unstable housing, lack of reliable transportation, inaccessible infusion services for people living in rural areas and financial barriers for uninsured patients or patients for whom dalbavancin may not be covered by insurance. RN-managed OPAT programs have been shown to reduce rates of readmission and therefore result in significant cost savings to health institutions and may help navigate some of the above barriers. 12 In our study, the majority of the recorded interventions were conducted by OPAT RNs compared to the rest of the OPAT team. For regimens requiring at least one dose of dalbavancin outside of the hospital, multiple OPAT RN interventions were required for the majority of patients. These interventions included coordination with antibiotic vendors, lab vendors and patients, as well as vascular access coordination for patients who had difficult venous access. Despite the fact that a majority (74%) of infections were complex (bone and joint infection or endocarditis), all 53 dalbavancin courses were completed successfully. Given the study population and successful completion rate, it is important to note the relatively low number of adverse reactions and 90-day readmissions.
Although dalbavancin use in PWID has been described,13,14 our study is the first to detail the effort required for successful coordination of dalbavancin in the outpatient setting. Our study adds to the literature on dalbavancin use by delineating both the specifics of coordination, the obstacles encountered and provides an estimate of the time involved. Additionally, the need for thoughtful care coordination applies to those with alcohol use disorder, 15 which comprised 21% of our study population. The most common interventions for OPAT RNs were phone calls to the patients to coordinate doses which can be challenging when the electronic medical record has inaccurate contact information, or the patient does not have a phone. Of the 17 patients who had an OPTIONS-DC conference, only 4 (23.5%) had a confirmed working phone during admission, which speaks to PWUD being further removed from their healthcare staff simply due to a lack of communication device. RN coordination with vendors is similar for any coordination of IV antimicrobial therapy but commonly overlooked when assessing the overall cost of administering dalbavancin, likely because it often only requires one outpatient dose. One outpatient consideration for dalbavancin coordination for PWUD is the patient’s vein status which in our study required four interventions to ensure successful dalbavancin administration outside of the hospital.
At our institution, a large portion of RN time is devoted to conducting OPTIONS-DC discharge planning conferences while a patient is still admitted. PWUD admitted with serious infections are often followed by the IMPACT team and often have an OPTIONS-DC conference which is a multidisciplinary discharge planning meeting that uses a structured tool to review risk and protective factors and helps determine safe treatment options for PWUD with serious infections, while emphasizing patient preferences and harm reduction. 11 Patients who leave the hospital on IV antibiotics, including dalbavancin, are then enrolled in the OPAT program. Recommendations from the OPTIONS-DC, implemented in February 2018, resulted in significantly higher use of dalbavancin for treatment or completion of treatment at 27.4% compared to those with substance use disorder (SUD) who did not have an OPTIONS-DC (9%). 16 This highlights that successful coordination of dalbavancin courses begins prior to hospital discharge, and requires comprehensive planning, because patients may be unreachable once they leave.
The nuances of insurance coverage further complicate the coordination of dalbavancin. For example, Medicare Parts A and B will not cover home infusion costs for antibiotics, therefore many patients must travel to an infusion center for their dalbavancin dose if they cannot afford the out-of-pocket home infusion cost. This requires additional resources such as reliable transportation and access to infusion settings in rural areas. Rural infusion pharmacies may struggle to supply this medication based on their formulary limitations. Oregon Medicaid generally covers dalbavancin infusions across many settings; however, in states with less robust coverage, higher rates of uninsured patients, or private insurances that do not cover the medication, this likely presents an additional barrier to coordination.
Another barrier to completing antibiotics in PWUD is the stigma often experienced in healthcare settings. In surveys of PWID, 78–88% of patients reported having experienced stigma in healthcare on at least one occasion.17,18 Additionally, patients identified avoiding stigma in healthcare by delaying presentation, not disclosing drug use, and downplaying pain although patients did report having more positive experiences at community-based organizations like syringe service programs.17,18 Additional barriers to seeking care were identified as difficulty attending appointments due to competing priorities (e.g. finding shelter and obtaining and using drugs to prevent opioid withdrawal). Systemic failures related to difficulty navigating the US healthcare system, unreliable transportation, and long wait times were also commonly identified.17,19 Although these surveys were aimed at primary and preventative care, this stigma persists among ID physicians as well. 5 These experiences discouraging PWUD from seeking preventative care likely also play a role in outpatient follow-up for antibiotic infusions like dalbavancin. In addition to stigma and healthcare systems failures, overarching structural determinants of health pressing down on this population to create unstable housing, food insecurity, lack of agency, and fear of society pose significant barriers to ‘adherence’. In our experience, assessing a patient’s history with medical appointment adherence can help identify a person with multiple of these vulnerabilities, this as well as assessing patient’s current stated desires for infection treatment, are predictors of success in dalbavancin courses requiring follow-up.
Limitations
There are several limitations in this study, including the retrospective chart review that relied on documentation of each intervention. This data are likely an underestimate of the work that happened as we collected only documented interventions performed by the OPAT team but not undocumented interventions or coordination by inpatient RN case managers. Additionally, the time-tracking phase of the study included only a small subset of patients and may under or overestimate the time spent per patient in the entire cohort. This data were also from a single center with an established multidisciplinary care conference supporting antibiotic treatment planning in PWUD, so may underestimate the dalbavancin-related effort required at other centers or in US states with less robust Medicaid coverage than Oregon.
Future directions
Future studies to improve dalbavancin administration success could include coordination with outpatient social workers and community partners to decrease needed phone calls and transportation coordination. Given that PWID report positive experiences at syringe service programs, evaluating dalbavancin infusions in these community settings may also be useful. Evaluating patient perspectives around outpatient antibiotics, improving access to cell phones and other resources, and cost analysis of OPAT RN coordination time would better inform our understanding and improve the success of dalbavancin use in PWUD. Additionally, this RN coordinator model could be applied to care for PWUD outside of long-acting glycopeptides, such as in the treatment of sexually transmitted infections and chronic hepatitis C virus infections.
Conclusion
Successful use of dalbavancin in PWUD requires significant coordination as represented by the number of OPAT RN interventions. Though use of dalbavancin can offer potential cost savings to health systems, the cost of coordination needs to be considered. Institutions frequently recommending dalbavancin in this population should be resourced and staffed to support effective implementation. In this vulnerable population that experiences stigma within the healthcare system, the length of stay for infection treatment and the resulting cost are often scrutinized. Although dalbavancin provides an alternate option for some infections and patients, it does not eliminate the need for patient-centered care and patient autonomy in treatment decisions as well as randomized controlled trials to evaluate non-inferiority to current standards of care.
