Abstract
Objectives:
Despite most childhood infections being self-limiting, children are among the leading consumers of antibiotics. Little is known about parental expectations of antibiotics for childhood infections. A comprehensive systematic review and meta-analysis was conducted to explore the nature and extent of parental expectations of antibiotic prescriptions for children with respiratory infections.
Design:
Systematic review and meta-analysis.
Methods:
An extensive literature search using six major scientific databases was conducted for all published articles until 7 December 2022. Primary studies reporting parents’ expectations of antibiotics for children with upper respiratory tract infections were included after assessment for quality. Heterogeneity between the studies was assessed using the I2 statistic and publication bias was analyzed using funnel plots and Egger regression tests. The primary outcome was a summary estimate of the percentage of parents who expect antibiotics from their physicians when their child presents with an upper respiratory tract infection.
Results:
From a total of 4510 studies found in the initial searches, a final pool of 19 eligible studies with 15,664 individuals was included in this meta-analysis. Nine of the 19 studies were from the United States or Saudi Arabia. The pooled prevalence of parental expectations of antibiotics in the population reviewed was 55.78% (95% CI = 44.60–66.41). There was significant heterogeneity between the studies, but funnel plot and meta-regression did not detect any publication bias.
Conclusion:
More than half of parents expect antibiotics for their children during consultation for upper respiratory tract infections. Such practices may cause undue side effects among children, contribute to the growing burden of antibiotic resistance, and lead to treatment failure for many common infections in the future. To optimize efforts to tackle antimicrobial resistance, shared decision-making and education emphasizing the proper and judicious use of antibiotics are much needed in pediatric healthcare settings. This can also help to manage parents’ expectations when seeking antibiotics for their children. Despite pressure from parents, pediatric healthcare providers should continue to advocate for antibiotic use only when warranted and help improve knowledge and awareness amongst parents.
Registration:
The protocol has been registered with PROSPERO (CRD42022364198)
Introduction
Antibiotics have revolutionized the management of bacterial diseases. However, indiscriminate and inappropriate use of antibiotics, specifically in the 21st century has led to the growth of antimicrobial resistance (AMR), that has, reduced efficacy of these drugs. 1 Over a million deaths were directly attributed to bacterial AMR in 2019 and another million deaths were linked to AMR. Developing or low-income countries bear the disproportionate burden of AMR.2–4 Primary care providers worldwide have expressed concerns about treatment failures and the inability to treat many infections among patients. With growing AMR at the level of primary care, providers often end up changing the antibiotics and progress toward the prescription of multiple or broad-spectrum antibiotics. All of this has, however, resulted in multidrug resistance leading to a profound impact on healthcare including treatment failure.5,6 The slower discovery of newer antibiotics, the ever-growing burden of infections with a lower threshold for resistance, and the widespread occurrence of emerging and reemerging infections compound the problem of AMR, a problem that lacks a comprehensive global solution as of today.7,8
The general publics’ knowledge, expectations, and beliefs have a major role to play in how and when antibiotics are prescribed or used, and eventually, the occurrence of AMR. Despite their influence, patients are often unable to link the irrational and inappropriate use of antibiotics with AMR.9–11 In this regard, parents of young children are a unique population majorly driving the consumption of antibiotics in the pediatric age group. Parental expectation has often been linked with children being the leading users of antibiotics.12–17 For example, while most childhood infections are self-limiting, due to excessive worries/fear or for quick relief, parents often directly express desires for or directly demand antibiotics from primary care physicians. This impatient approach leads to antibiotic overuse.14–17
Irrational use of and expectations of antibiotics are well explored along with AMR mechanisms among adults.4–9 A few studies worldwide have explored how parents’ decisions and desires for antibiotics may influence the occurrence of AMR among children.10–13 However, there is a lack of a comprehensive summary quantifying parents’ expectations concerning the demand for antibiotics for children’s upper respiratory tract infections (URTIs). Thus, the purpose of this investigation was to carry out a comprehensive estimate of parents’ expectations for antibiotics among children with URTIs by conducting a systematic literature search and meta-analysis.
Methods
This systematic review and meta-analysis was conducted by including observational studies published until 7 December 2022. The protocol was registered with the International Prospective Register of Systematic Reviews (PROSPERO) under the registration number CRD42022364198. The Statement 2020 for Preferred Reporting Standard of Systematic Reviews and Meta-Analyses (PRISMA) was used to report this systematic review incorporating meta-analyses (Supplementary File).
Search strategy and selection criteria
A thorough search was conducted using databases such as PubMed, Scopus, Web of Science, ProQuest, EMBASE, EBSCOHost, and Cochrane. We also checked preprint servers like medRxiv, arXiv, bioRxiv, BioRN, ChiRxiv, ChiRN, and SSRN (Supplementary File). Also, new eligible studies were extracted by carefully searching for relevant references from included articles and other suitable reviews. The primary outcome was a summary estimate of the percentage of parents who expect antibiotics from their healthcare providers when their children presented with a URTI. The search keywords included ‘respiratory tract infections’, ‘children’, ‘parent’, ‘antibiotic’, ‘behaviour’, ‘preference’, ‘expectation’, ‘prescription’, and other similar words for each of these terms. Asterisks were used to identify related articles. (Supplementary File). The articles were saved in Mendeley Desktop V1.19.5 software to manage citations, remove duplicates, and avoid errors.
All original articles published until 7 December 2022 addressing the research question in the form of percentages were considered. Cross-sectional studies, case control, cohort, randomized controlled trials, and all other primary research answering the research question were included. Parents’ expectations or perceptions of antibiotics based on their attitudes were assessed. It is based upon parents’ expectations, and not doctors’ opinions. Studies not published in English, case studies, commentaries, narrative reviews, and letters were excluded from the analysis. Crombie items were used for the assessment of the quality of the studies included for review and meta-analysis (Supplementary File). URTIs include involvement of nose, sinuses, pharynx, larynx, and the larger airways.
Data extraction and management
Two investigators reviewed each paper and if there was a disagreement regarding the choice of an article, two additional co-authors were invited to resolve the disagreement. Subsequently, from the eligible articles, the last three investigators gathered the following information from each source article: the study author’s name, the place where the study was conducted, the year of publication, the study design, the number of participants, and the number of parents expecting antibiotics (Table 1). Articles searched were assimilated using the PRISMA checklist to ensure scientific precision. Finally, 19 studies were included in the meta-analysis for this review.
C/S, cross-sectional; RCT, randomized controlled trial; URTI, upper respiratory tract infection.
Data analysis
The percentage of parents who requested antibiotics from healthcare during the consultation of their children for URTIs was calculated by dividing the number of parents who wanted prescriptions by the total number of study participants. The heterogeneity of the studies evaluated in this meta-analysis was assessed using the I2 test. The heterogeneity was classified as low, moderate, and high, respectively, based on I2 values of less than 25%, 25%–50%, and more than 50%. Cause for heterogeneity was also explored using meta-regression. A random-effects model with 95% confidence intervals was used to evaluate the overall effect and p-values of < 0.05 was considered statistically significant. Subgroup analysis was done based upon geography (continent) using a random intercept logistic regression model. R version 4..2.1 and STATA® software (version 16, STATA Corp.) were used to conduct the meta-analysis.
Results
An extensive search of the databases and preprint servers produced 4510 articles, of which 212 duplicates were detected. We eliminated these duplicate papers during the preliminary screening. Another 4298 articles were screened on their titles and abstracts, and 4244 were removed based on inclusion and exclusion criteria (Figure 1 depicts the PRISMA flowchart for the article selection process). A comprehensive document screening was carried out on 54 articles and 35 of these were excluded as they did not meet the inclusion criteria; a final pool of 19 high-quality studies was used for this meta-analysis.18–36

PRISMA flowchart for included studies in systematic review and meta-analysis of parental expectation for antibiotics for children with upper respiratory tract infections.
None of the studies were reported to be of poor quality. However, one study 35 asked similar questions twice, and received different responses of 59.1% and 91.3%. Thus, we decided to run a sensitivity analysis after excluding this study.
Five of the 19 studies (26%) are from the United States, while four (21%) and two (11%) studies are from Saudi Arabia and Iceland, respectively. The rest of the studies are from Lebanon, Greece, Cyprus, UAE, Israel, Palestine, Hong Kong, and Finland, respectively.
Meta-analysis
A synopsis of the final pool of 19 studies is included in Table 1 (including 18 cross-sectional studies and one randomized controlled trial). A total of 15,664 people participated in these studies where the United States and Saudi Arabia contributed the maximum number of studies (5 and 4, respectively). However, when reviewed individually, a study from Greece had the highest number of study participants (n = 5312). 24 The results of the quality assessment of the studies can be found in the Supplementary File.
A meta-analysis was conducted to determine the percentage of parents who expected antibiotics from physicians during the consultation of their children for URTIs. Among the 15,664 individuals in the populations studied, 8982 had this expectation. The pooled prevalence of parental expectations of antibiotics in the investigated population was 55.78% [95% confidence interval (CI) = 44.60–66.41]. A random effect model was used (I2 = 99.27%; p < 0.001) (Figure 2).

Pooled prevalence forest plot of parental expectation for antibiotics for children with upper respiratory tract infections.
Heterogeneity and publication bias
Significant heterogeneity was observed among the included studies (Figure 3). Since it provides more conservative effect sizes, we used the DerSimonian and Laird random-effects model to determine the total pooled prevalence of parents’ expectations for antibiotics. We performed a univariate meta-regression analysis to identify the most likely causes of the variation and evaluated the publication year and the study sample size as potential factors related to the variation in prevalence. However, there were no statistically significant differences (Supplementary File). To test for publication bias, a funnel plot was utilized which appeared to be slightly asymmetric (Figure 3), which suggested that publication bias existed. We performed meta-regression to explore the cause of heterogeneity. Neither sample size (p = 0.77) not year of publication (p = 0.15) significantly moderated the pooled estimate. This can be visualized in the bubble plots (Figure 4; Supplementary File).

Funnel plot to check heterogenicity of the studies included in meta-analysis.
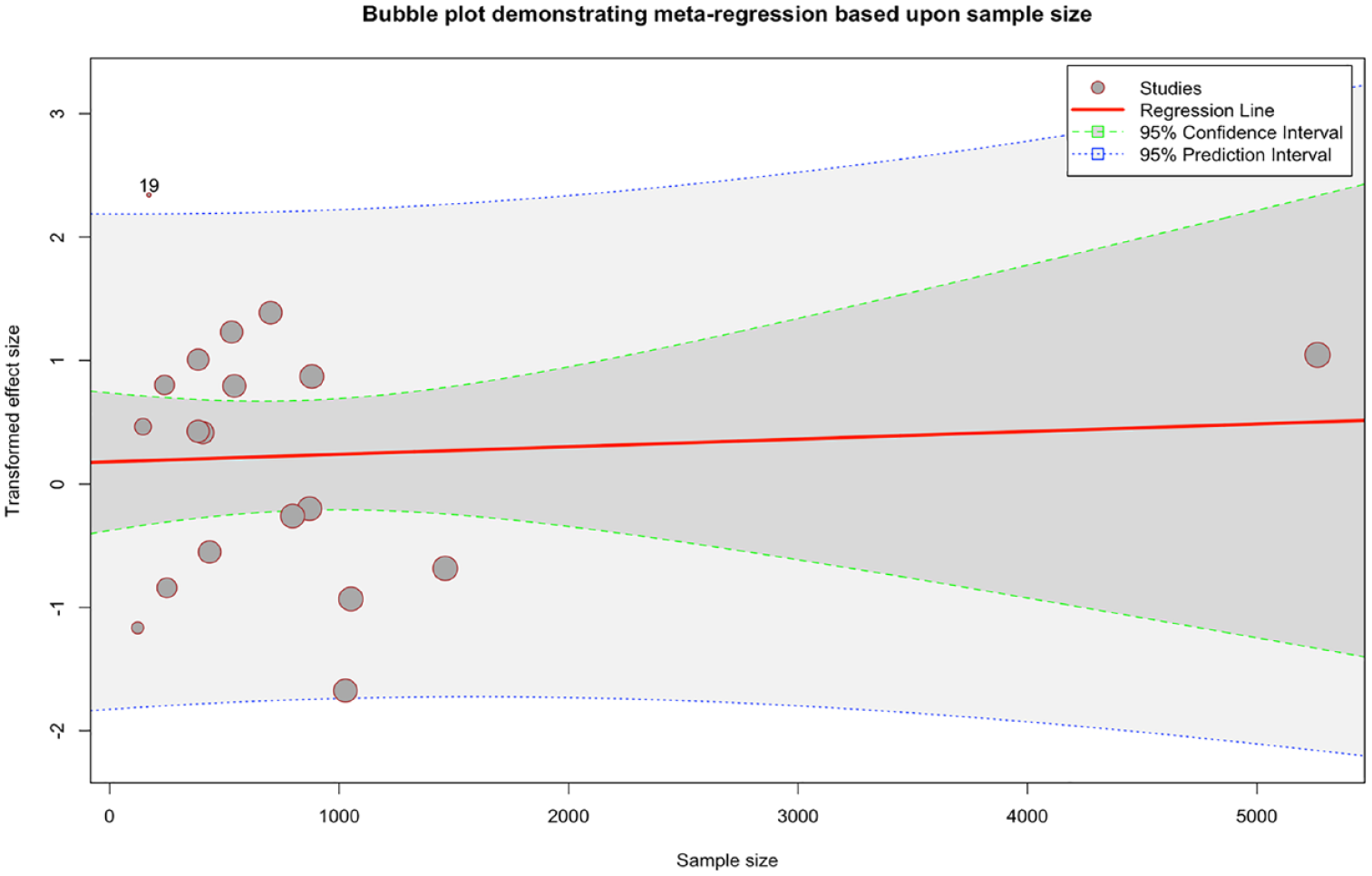
Bubble plot to demonstrate meta-regression based on the sample size in the studies.
Subgroup analysis
We performed a subgroup analysis to explore the causes of heterogeneity. However, there was a lack of homogeneous data reported across the different studies. A subgroup analysis based on geography shows that there is no significant difference between the studies based on continent (Q = 0.11, p = 0.95).
Sensitivity analysis
In the sensitivity analysis run after excluding this study, 35 the pooled prevalence reduced from 55.78% (95% CI = 44.60–66.41) to 53.01% (95% CI = 42.68–63.09) (Supplementary File).
Discussion
In this review, we found that worldwide, the proportion of parents seeking antibiotics for their children with URTIs was nearly 56% out of the total sample of 15,664. This problem is multifactorial and originates at both ends, from the parents’ side and the healthcare providers’ side.32–37 Although antibiotics are mainly designed for bacterial infections, they should not be used injudiciously.38,39
From the parents’ perspective, excessive worries, poor knowledge about URTIs, lack of awareness about antibiotics, and paucity of time and patience may result in unrealistic expectations for antibiotics.19,20,28,30 For example, a randomized control trial with 1051 parents in the United States by Goggin and colleagues found that the degree of parents’ knowledge has a greater influence on their willingness to seek antibiotics. 19 In another study of 239 parents from the UAE, the majority had poor knowledge of antibiotics (54.4%), did not know that antibiotics are used to treat bacterial infections (66.1%), or did not know that the overuse of antibiotics leads to antibiotic resistance (54.5%). However, 63% affirmed that they would ask their child’s healthcare provider to prescribe antibiotics if the provider does not prescribe them. 28 In another study by Zyoud and colleagues with 380 Palestinian parents, the majority did not agree that most URTIs are caused by viruses (59%) and thought that antibiotics are the most suitable treatment for URTIs (73%). 30 Such expectations may also vary by parents’ race, ethnicity, age, and other sociodemographic characteristics. 21 Given that parents could be the major drivers of antibiotic prescriptions for children, certain recommendations and guidelines have been provided by professional organizations and in the scientific literature19,29–31,37,40 These include the usage of effective communication strategies to educate parents about when antibiotics are needed and not needed and the potential harms of antibiotic treatment, providing educational materials in a variety of formats (e.g. multimedia and print) and in a language appropriate for parents, using watchful waiting and delayed prescription, avoidance of unilateral decision-making by providers, adequate discussion of diagnosis with parents, engagement of triage and interdisciplinary teams, promotion of trust with providers among parents/children, giving opportunities to parents and children to communicate their concerns and questions, having contingency plans or prescriptions, provision of symptomatic relief therapies for children, and ensuring timely and adequate access to healthcare providers with expertise on URTIs among children for parents or guardians.19,29–40
Some studies have shed light on the reasons and determinants behind this high expectation. For example, a study in the United States showed that parents who worked full-time were more likely to want antibiotics compared with parents who worked part-time. 18 A cross-sectional study in Israel suggested that parents with more years of education had a lower expectation for antibiotics. Among factors pertaining to medical history, either usage of antibiotics in prior episodes of URTI, or experience of complications in those episodes is associated with a greater expectation for antibiotics. 29
From the healthcare provider’s perspective, pressure from parents, lack of knowledge about URTIs and their appropriate treatment, reduced patient-provider trust, absence of prescription protocol and guidelines, poor diagnostic and antibiotic prescription stewardship, failure to use evidence-based diagnostic and therapeutic criteria, lack of experience in pediatric infectious disease care (e.g. being a trainee) or communication with parents, and providers’ sociodemographic and healthcare facility characteristics could be some of the critical factors related to unwarranted antibiotic prescriptions for URTIs among children19,23–26,37,40,41 For example, in a Greek study of 5312 parents, there were high expectations of antibiotic prescriptions for children with URTIs. However, a trusting relationship with pediatricians made parents follow the instructions of providers without any pressure to prescribe antibiotics. 24 Similarly, a study of parents and pediatricians from Cyprus found that the majority (>50%) of parents considered pediatricians as the main source of information about antibiotics and agreed that the misuse of antibiotics increases antibiotic resistance. In this study, most of the pediatricians believed that URTIs are self-limited and antibiotic misuse increases resistance, and shared that they would not prescribe antibiotics solely to appease parents or for the fear of parents changing providers. 25 Certain recommendations have also been provided for healthcare providers to avoid the injudicious use of antibiotics for children with URTIs19,11–13,37,39–41 These include the encouragement of providers to self-assess antibiotic prescribing practices, participate in continuing medical education and quality improvement activities, engage in communications skills and decision support training, and set expectations with parents and patients, just to name a few. For healthcare facilities, they can assess and share performance on quality measures and establish goals to reduce antibiotic prescriptions when not needed, implement antibiotic prescription tracking systems, require explicit justification in medical records for antibiotic prescriptions, and use phone lines or web communication activities as triage systems to prevent unnecessary visits for URTIs from patients and parents.
Strengths and limitations
The results of our meta-analysis are affected by many of the limitations related to studies included in this review. For example, most of the studies reviewed did not provide enough information to link the high prevalence of antibiotic expectations among parents with parental demographic or socio-economic factors. Furthermore, in all the studies reviewed, children were not characterized by sociodemographic or health-related variables. Many studies did not explore the reasons, or interventions to reduce this. The heterogeneity of studies included for review and their sampling strategy may have influenced our estimates. Finally, the studies included in the review were from a range of countries and the variations in the provision and arrangements of healthcare systems between regions may have influenced the study estimates. The recall, selection, and non-response bias in individual studies could have impacted the findings. However, we attempted to maintain homogeneity as much as possible. We excluded studies that did not answer the research question accurately or were much broader in their scope. Despite these limitations, this is the largest and first systematic review and meta-analysis on this topic to date. The inclusion of studies from populations across the world presents the global picture of the problem under discussion indicating rampant expectations of antibiotics in pediatric healthcare settings. Finally, this systematic review follows the JBI and PRISMA-ScR guidelines authenticating the findings and quality of the review to a great extent.
Conclusion
In this large-scale meta-analysis, we found that the majority (55.3%) of parents worldwide expect a prescription of antibiotics when their children have URTIs. Given that most childhood URTIs are self-limiting and may not need antibiotics, parents’ expectations for unnecessary prescriptions of antibiotics may, in the long run, contribute to the growing burden of AMR. Educational programs for parents and providers and policy interventions may help reduce such tendencies of unwarranted prescriptions and should be implemented across healthcare facilities. Parents should be made to feel a part of the decision-making process and be given accurate information and awareness about the risks and benefits of antibiotics. Parents should also be encouraged to employ alternative symptomatic treatment options for childhood URTIs instead of solely relying on antibiotics.
Supplemental Material
sj-docx-1-tai-10.1177_20499361231169429 – Supplemental material for Parents’ expectation of antibiotic prescriptions for respiratory infections in children: a systematic review and meta-analysis
Supplemental material, sj-docx-1-tai-10.1177_20499361231169429 for Parents’ expectation of antibiotic prescriptions for respiratory infections in children: a systematic review and meta-analysis by Muhammad Aaqib Shamim, Bijaya K. Padhi, Prakasini Satapathy, Abdelmonem Siddiq, Subhanwita Manna, Arun K. Aggarwal, Tareq Al-Ahdal, Jagdish Khubchandani, Andrés F. Henao-Martinez and Ranjit Sah in Therapeutic Advances in Infectious Disease
Footnotes
Acknowledgements
We acknowledge the role of Global Center for Evidence Synthesis, Chandigarh, in supporting us to perform, teach and disseminate systemic reviews and meta-analyses.
Declarations
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.

