Abstract
Pulmonary arterial hypertension impairs exercise tolerance and daily physical activity. Aside from the hemodynamic limitations, physical, cognitive, and emotional factors may play a relevant and as yet unexplored role. We investigated whether there is an association between the physical activity level and psychological disorders, health-related quality of life, and daily activities. We also searched for an association of the physical activity level with clinical factors and functional capacity. This was an analytical, cross-sectional, observational study conducted in a Brazilian University Hospital. Twenty stable pulmonary arterial hypertension subjects wore an accelerometer for a week and completed an activity diary. They answered the quality of life questionnaire (SF-36), as well as the Hospital Anxiety and Depression scale, and the Manchester Respiratory Activities of Daily Living questionnaire. Transthoracic echocardiography, the six-minute walk test, the one-minute sit-to-stand test, and spirometry were performed. For statistical analysis, we used Chi-square tests or Fisher’s test as appropriate and the Mann–Whitney test to compare numerical values between two groups. The relationship between the parameters was assessed using the Spearman correlation test. The mean age was 44.3 years, 80% were women, 80% had idiopathic pulmonary arterial hypertension, and 20% had connective tissue disease. The mean daily step count was 4280 ± 2351, and the mean activity time was 41.6 ± 19.3 min. The distance covered (six-minute walk test) was 451.5 m, and the number of movements (one-minute sit-to-stand test) was 23.8. Thirty percent scored positive for anxiety, and 15% for depression (Hospital Anxiety and Depression scale). There was a significant correlation between accelerometer data and walking distance (six-minute walk test), number of movements (one-minute sit-to-stand test), level of daily physical activity (Manchester Respiratory Activities of Daily Living questionnaire), and depression symptoms. Our findings support the hypothesis that other aspects beyond physical and hemodynamic ones might impact the daily physical activity of patients with pulmonary arterial hypertension.
Introduction
Exercise tolerance impairment is a hallmark of pulmonary arterial hypertension (PAH). In addition to its impact on quality of life, it is associated with a worse prognosis. 1 Hemodynamic impairment hinders the increase in cardiac output required for exercise and accounts for much of the effort limitation. Symptoms such as fatigue, lack of energy, dyspnea, chest pain, or discomfort are also frequent in individuals with PAH. 2
Some studies have shown that PAH patients have reduced daily physical activity (PA)3,4 and spend more time being sedentary.4,5 This lower level of PA has been associated with decreased six-minute walk test (6MWT) distance, 3 hemodynamic impairment, 6 and reduced survival 6 in patients with PAH. The association between PA and Health-Related Quality of Life (HRQL) was evaluated in two studies5,7 with different findings: Okumus et al. 7 found a moderate correlation between steps per day and all SF-36 domains; Matura et al., 5 using the CAMPHOR scale, found that only the self-reported energy component was associated with lower activity levels. 5
Guidelines recommend that PAH patients be encouraged to be active. 1 However, this demands more knowledge about all aspects of PA limitations. The mechanisms that reduce PA in these individuals are multifactorial and influenced by environmental factors, exercise tolerance, and psychological factors. Nevertheless, the relationships between PA level, psychosocial distress, and impairment of the activities of daily living (ADL) remain poorly understood. Therefore, this study aims to investigate a potential association between PA levels and psychological distress, HRQL, and ADL impairment in patients with PAH. Additionally, it evaluates whether there is an association of PA level with clinical factors and functional capacity.
Method
This was a cross-sectional, observational study with a convenience sample of patients over 18 years old diagnosed with PAH. All patients had right catheterization and a diagnosis according to PAH guidelines. 1 Patients must have been receiving targeted PAH therapy at a stable dose for at least eight weeks and categorized as functional class (FC) I, II, or III for dyspnea New York Heart Association (NYHA). The following subjects were excluded: those diagnosed with depression, receiving medication for this condition, those with cognitive impairment who might have difficulty completing the questionnaires, and subjects with mobility limitations or any muscular or neurological condition that could compromise walking or PA.
All patients were recruited from the Pulmonary Vascular Disease Service of the Pulmonology Division of the Universitary Hospital. The study was submitted to and approved by the Research Ethics Committee of the School of Medical Sciences (ruling no. 76543617.9.0000.5404/2017). All patients participating in the study signed the informed consent form.
Patients were seen in two visits. On Day 1, medical history was collected and the FC-NYHA was graded. The SF-36 questionnaire 8 and the Hospital Anxiety and Depression scale (HADS) 9 were completed. The 6MWT, 10 the one-minute sit-to-stand test (1-STST),11,12 and spirometry were performed. Subjects were then given an accelerometer (Power Walker, Yamax®) that may be used inside their shirt pocket, pants, or even strapped to their belt. These recommendations are given by the manufacturer to ensure that steps are counted correctly (Fig. 1). Participants were instructed to wear it during all waking hours for seven days. It could be removed for bathing/showering and sleeping. They were required to complete an activity diary and to report any complications with the use of the device. The patient was asked to write down the number of steps when removing the equipment and it was emphasized that the purpose of using the device was to evaluate his activities on ordinary days, that no additional activities to his routine should be done or left to do. On Day 8, the accelerometer and the diary were returned, the Manchester Respiratory Activities of Daily Living questionnaire (MRADL) was applied, 13 and underwent a transthoracic echocardiogram.

Different ways of carrying the accelerometer.
The 6MWT was performed under supervision of the same technician, according to the American Thoracic Society guidelines. 10 The 1-STST involves the performance of as many sit-to-stand actions as possible in one minute without using the upper limbs. Spirometry was performed according to the American Thoracic Society guidelines 14 and reference values for the Brazilian population 15 were used.
The SF-36 is a well-validated, generic questionnaire consisting of 36 items that evaluate eight domains: physical functioning, physical role functioning, bodily pain, general health perceptions, vitality, social role functioning, emotional role functioning, and mental health. 16 The score varies from 0 to 100 (0, worse health). The SF-36 has been validated in the Portuguese language 8 and it is commonly used in PH trials.17,18
The HADS (Portuguese version) 9 was used to assess anxiety and depression. It consists of 14 items divided into depression (HADS-D) and anxiety (HADS-A) subscales, each with seven items. Each subscale scores from 0 to 21 and a cut-off score of 8 or more was used to determine depression or anxiety in patients.
The MRADL questionnaire aims to establish a scale of physical incapacity and impairment of daily living activities in respiratory diseases. It consists of four domains: mobility, kitchen activities, domestic tasks, and leisure activities. The MRADL score ranges from 0 to 21 with a score of 21 indicating no physical disability. We used a Portuguese version validated for Brazil. 13
Data analysis
Continuous variables are displayed as mean ± sd or median (min – max range). We used the chi-square test or Fisher’s exact test as appropriate. The Mann–Whitney test was used to compare numerical values between two groups. The relationship between parameters was assessed with the Spearman correlation test. Numerical variables were ranked due to a lack of normal distribution. Probability values of < .05 were considered to be statistically significant. Analyses were performed with the SAS System for Windows (version 9.4, SAS Institute, 2002–2012; Cary, NC, USA).
Results
Twenty patients with PAH were enrolled and completed all tests. Clinical data are shown in Table 1.
Clinical and demographic data of PAH patients.

aData expressed as mean ± sd.
bDiabetes and systemic arterial hypertension.
IPAH: idiopathic pulmonary arterial hypertension; PAH-CD: pulmonary arterial hypertension associated to collagen disease.
All participants completed the seven-day protocol wearing the accelerometer throughout the waking period, except during the bath and there were no adverse events or complaints of discomfort. Two patients reported having forgotten to write down the data at the end of one of the seven days; in these cases, the average was calculated based on the six-day data. The mean daily step count was 4280 ± 2351 (median 3452 (2069–11,829)), 4497 being the mean for work days and 3608 for weekend days. There were no differences in average daily activity time or number of steps per day between days of the week and days of the weekend. The mean activity time was 41.6 ± 19.3 min (median 37.5 (20.4–94.9)). Fig. 2 shows the daily step count for each patient.
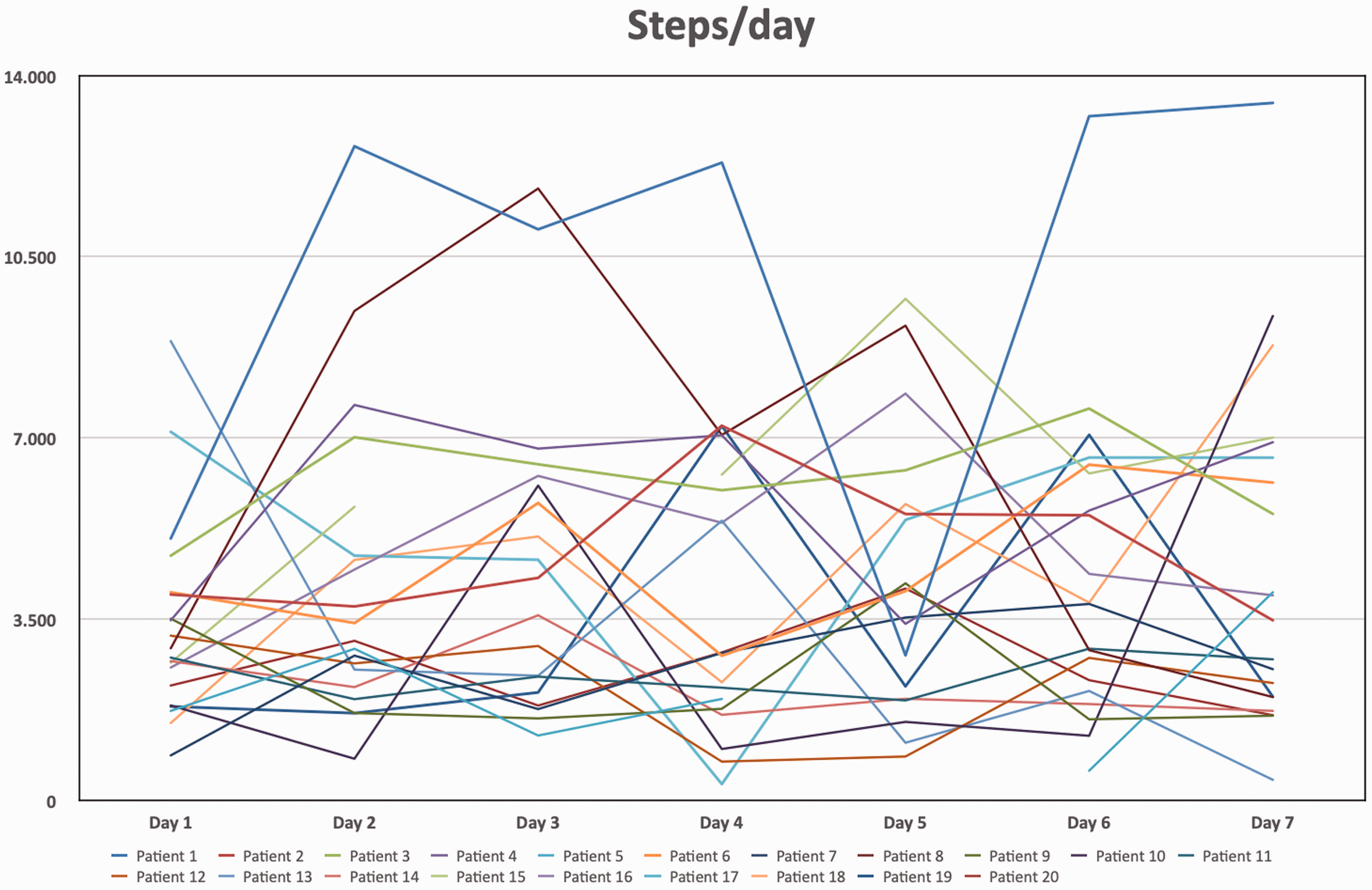
Daily step count for each patient.
The mean distance covered in the 6MWT was 451.5 ± 96 m, and the mean number of repetitions in the 1-STST was 23.8 ± 6.1. Lung function and echocardiographic data are shown in Table 2.
Functional data of PAH patients.
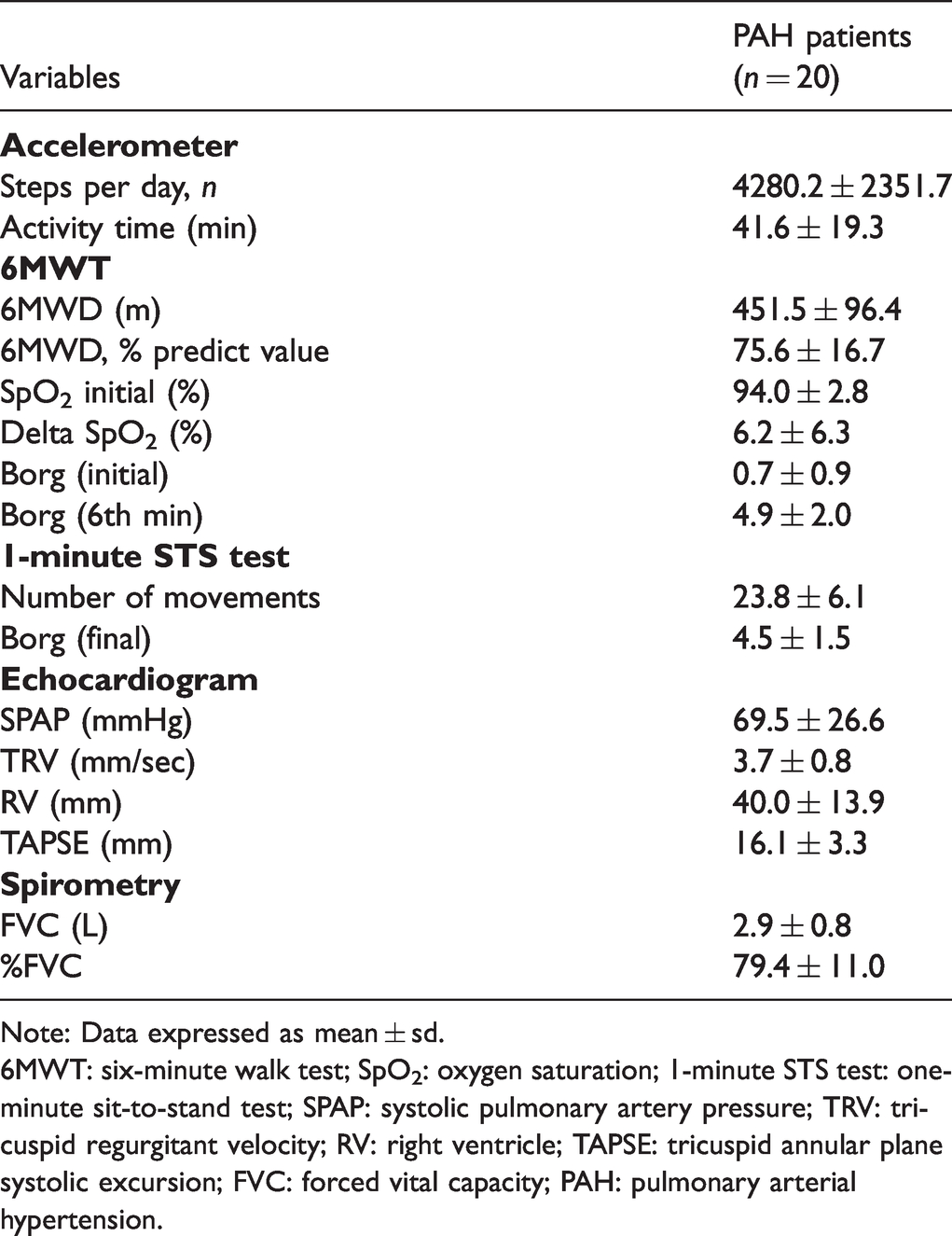
Note: Data expressed as mean ± sd.
6MWT: six-minute walk test; SpO2: oxygen saturation; 1-minute STS test: one-minute sit-to-stand test; SPAP: systolic pulmonary artery pressure; TRV: tricuspid regurgitant velocity; RV: right ventricle; TAPSE: tricuspid annular plane systolic excursion; FVC: forced vital capacity; PAH: pulmonary arterial hypertension.
The main questionnaire results were: (1) in the SF-36, patients scored higher in the physical functioning, general health perceptions, and vitality domains; (2) in the HADS, 30% of patients scored positive for anxiety (HADS-A) and 15% for depression (HADS-D); and (3) in the MRADL questionnaire, the mean score obtained indicated no restriction in daily activities. Complete questionnaire data are shown in Table 3.
Questionnaires data of PAH patients.
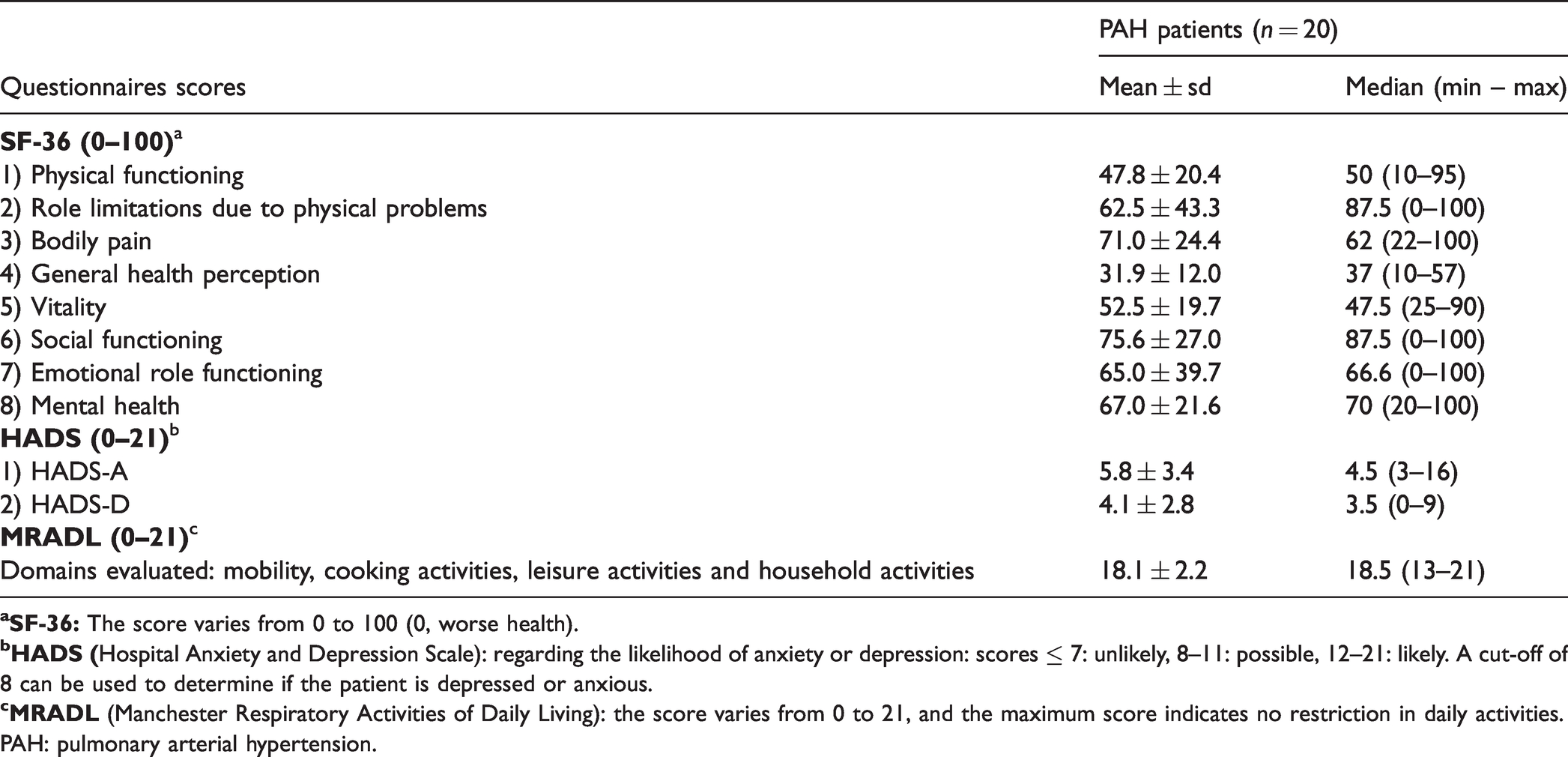
PAH: pulmonary arterial hypertension.
In the correlation analysis, the daily step count and activity time (accelerometer data) showed a correlation with walking distance (6MWT, p < 0.002) and number of repetitions (1-STST, p < 0.005). There was also a significant correlation between accelerometer variables, the MRADL questionnaire (p < 0.01), and depression (HADS-D, p < 0.05). No significant correlations were observed with echocardiography, spirometry, or with the SF-36. Only the 6MWT and the 1-STST presented a significant correlation with echocardiography data. Correlation analysis data are presented in Table 4 and in Fig. 3.
Correlation analysis of physical activity with exercise tests and questionnaires.
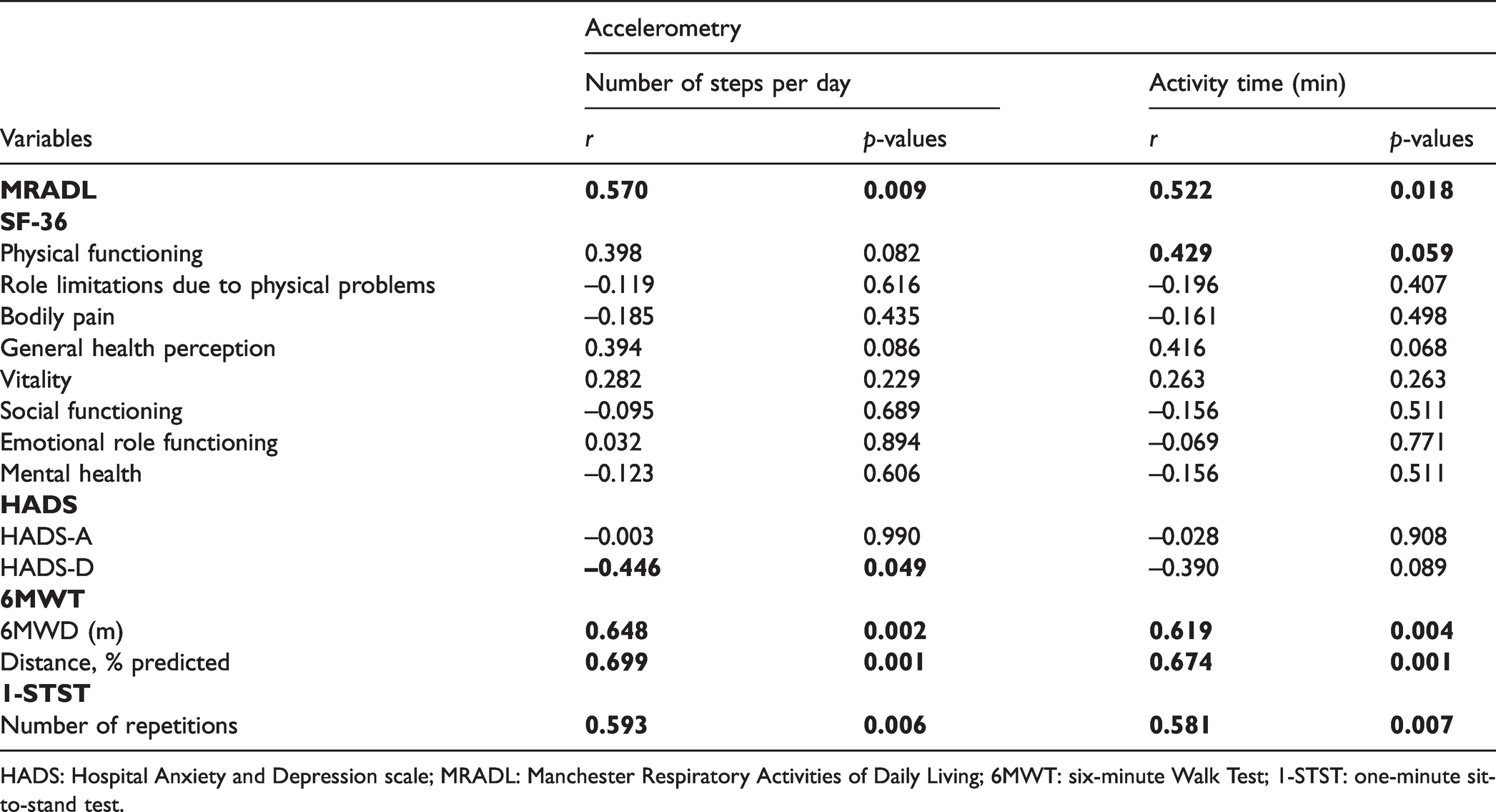
HADS: Hospital Anxiety and Depression scale; MRADL: Manchester Respiratory Activities of Daily Living; 6MWT: six-minute Walk Test; 1-STST: one-minute sit-to-stand test.
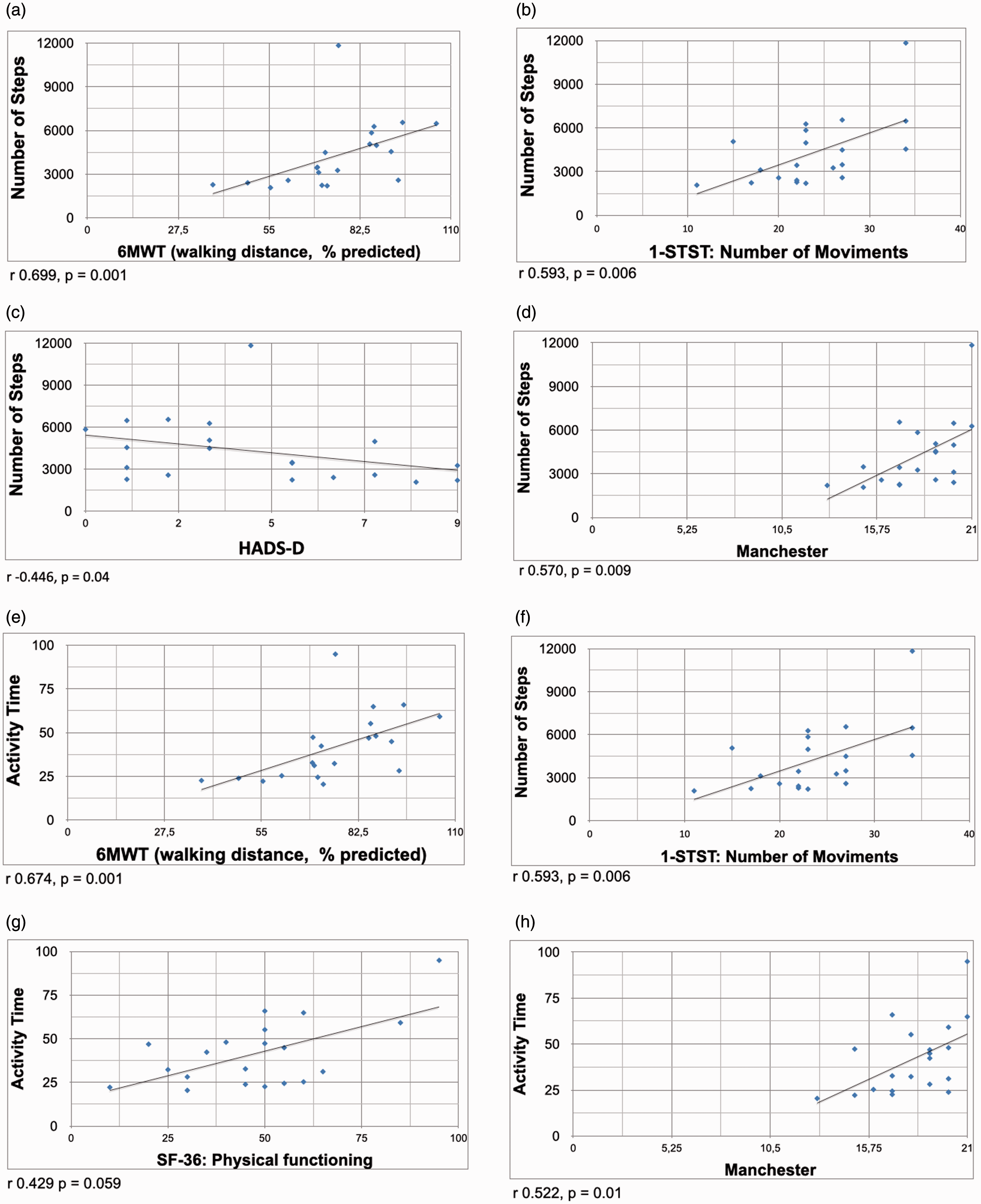
Correlation analysis results of number of steps (accelerometer) versus (a) 6MWT; (b) 1-STST; (c) HADS-D; (D) Manchester questionnaire; and of activity time (accelerometer) versus (e) 6MWT; (f) 1-STST; (g) SF-36 questionnaire; (h) Manchester.
Discussion
The results show that assessing PA with an accelerometer is feasible and is an easy way to evaluate daily activity in patients with PAH more objectively. Mean daily step count was 4280 and mean activity time, which here refers to the time the subject was walking, was 41.6 min. Additionally, the results show that more active PAH patients have fewer symptoms of depression, less ADL impairment, and better physical function.
Daily step count in the present study was lower than in other studies that measured PA using an accelerometer in patients with PAH.3,19 Mainguy et al. evaluated patients with PAH and healthy individuals and found a mean daily step count of 5041 versus 9189 steps per day in the control group, matched by sex, age, and body mass index. 3 Sehgal et al. found a higher mean daily step count of 5847. 19
In a study to detect fluctuations in the PA level in individuals with PAH according to the weather, patients had daily averages ranging from 5567 ± 2434 steps per day in mild weather to 3995 ± 2013 steps per day on days with temperatures higher than or equal to 25°C. 20 These numbers are similar to ours, especially taking into account that Brazil has a predominantly tropical climate and on most days, the temperature is higher than 25°C. It is important to mention that the PA level may vary among countries, not only because of climate, but also due to other socioeconomic and cultural characteristics. For example, Brazilian patients with Chronic Obstructive Pulmonary Disease (COPD) patients are more physically active than Austrian patients. 21 Comparing against Brazilian data, PAH patients in our study seem to be less physically active than COPD patients (6251), despite the fact that COPD patients are usually older and show more comorbidity.
In this study, the mean walking distance in the 6MWT was 451.5 ± 96.4 m, which is slightly higher than that found in a Brazilian registry (398 ± 152 m) 22 and similar to another Brazilian study, which reported 463 ± 78 m. 23 The figures from these Brazilian studies are higher than those reported in other registries, such as the American registry with 374 ± 129 m 24 and the French registry with 329 ± 109 m. 25 We observed a strong correlation between accelerometer data and 6MWT distance, a finding similar to other studies that also used an accelerometer to assess PA in patients with PAH.3,19
The mean number of repetitions in the 1-STST was 23.8 ± 6.1. Literature data show that the mean number of repetitions ranges from 8.1 (stroke patients) to 50.0 (young men). 26 Already tested in patients with COPD, cystic fibrosis, and interstitial diseases, this test showed a good correlation with 6MWT distance 27 and with exercise-induced oxygen desaturation,12,28,29 muscle strength,29,30 and mortality. 31 As far as we could identify, this is the first study to evaluate 1-STST in PAH patients.
We found strong correlations between 1-STST and daily step count (r = 0.59, p = 0.006) and 6MWT distance (r = 0.62, p < 0.001). Similar findings were described in COPD patients in whom daily step count had a moderate correlation with 1-STST (r = 0.51). 32 These results, combined with the fact that the 1-STST is easily performed, require no special infrastructure and seems to be less hemodynamically stressful than the 6MWT, 33 which may indicate that this test could be used as a surrogate in future studies with patients with PAH, especially within the context of pulmonary rehabilitation programs. 26 However, more studies are needed to validate the 1-STST in this context.
The MRADL questionnaire seeks to identify to what extent respiratory problems interfere with the individual’s daily life activities. Patients scored (18.1 ± 2.2), which indicates no restriction in daily activities. Nevertheless, daily step count and activity time had a positive correlation with MRADL (r = 0.57 and r = 0.52, respectively). This result shows that the more the patients feel independent in their daily activities, the greater the activity time and the number of steps per day. Okumus et al. also observed this association in a previous study with PAH patients. 7 It is important to emphasize that, although there was a moderate correlation between MRADL and the daily step count, these instruments evaluate different aspects of PA, as daily step count quantifies PA and the MARDL evaluates the capacity and ability to perform it. 21
Mean HADS score was 5.8 ± 3.4 for anxiety (HADS-A) and 4.1 ± 2.8 for depression (HADS-D), which means a low probability for both. Even so, 30% had symptoms of anxiety and 15% had symptoms of depression. Our figures are similar to those of Somaini et al., 34 who investigated the prevalence of depression and anxiety in 131 patients with PH using the HADS. The authors found prevalence of depression in 21% and anxiety in 24% of patients with PH, rates slightly lower than those of Pfeuffer et al., 35 who reported 30% with depression and 32.9% with anxiety. Using different self-administered questionnaires, the prevalence of mood disorders ranged between 7.5 and 53% for depression and from 19 to 51% for anxiety.34,36–40 Our findings are in consonance with the literature and reinforce the high prevalence of mood disorders in this population. Interestingly, we found a moderate negative correlation between depression score and daily step count (r = –0.45, p = 0.048), but not with the 6MWT or 1-STST. The association between depression and PA was observed in individuals at high risk of cardiovascular disease 41 and in COPD patients. 42 Depression symptoms may impact PA and further studies should focus on diagnosing and managing psychological distress in patients with PAH.
HRQL is often considered the most meaningful measurement of disease from a patient perspective. Previous studies have demonstrated that HRQL is reduced in PH patients compared with healthy subjects. 38 Many studies have shown that although HRQL improves with diagnosis and treatment, it remains low.43,44 Our patients had low scores on the SF-36 questionnaire, mainly in the physical functioning, general health perceptions, and vitality domains; however, there was no correlation between HRQL and steps per day. To the contrary, Okumus et al. 7 found a moderate correlation between number of steps per day and SF-36 domains. This discrepancy may be because our patients had less severe disease, walked more in the 6MWT, and had better HRQL, as evaluated by the SF-36, than patients in the Okumus study. Matura et al. 5 used the CAMPHOR scale and found that only the self-reported energy component was associated with lower activity levels.
There are several limitations to our study. First, it is a single-center study with a small sample size. Patients wore the accelerometer in different places according to the manufacturer’s specifications, and the individual’s preference and clothing. It is difficult to know if this fact could have interfered with the results. As the patients evaluated were relatively young and non-obese, the findings may not be replicated in patients with different demographic and functional profiles, for example older, obese, or less functional patients. Larger studies are needed, mainly to validate the 1-STST. Second, because there is no previous study with the 1-STST in patients with PAH, a comparison against healthy controls is warranted. Third, we could not use specific questionnaires, like the CAMPHOR questionnaire, because there were no validated versions for Brazil at the time of study. Thus we decided to use other tools translated to and validated in Brazilian Portuguese, knowing that they were not specific to PAH.
Exercise capacity impairment is a hallmark of the disease, but symptoms like fatigue, lack of energy, and mood disorders are also frequently observed in individuals with PAH.2,45 A low level of PA associated with these symptoms suggests that physical, cognitive, and emotional components overlap. Our study supported the multifactorial nature of reduced PA.
Although there is increasing evidence of reduced PA in patients with PAH, there is still uncertainty, such as how PA should be measured or how these measurements correlate with well-established outcomes used in clinical trials. Our findings reinforce the importance of assessing PA and the feasibility of doing so with an accelerometer. The correlations between daily PA and emotional aspects, quality of life, and activities of daily living reinforce the potential of the accelerometer to actually reflect the impact of PAH on the individual’s life.
Protection of human and animal subjects
The authors declare that the procedures followed were in accordance with the regulations of the relevant clinical research ethics committee and with those of the Code of Ethics of the World Medical Association (Declaration of Helsinki).
Ethical statement, ethical approval, informed consent
The study was submitted to and approved by the Research Ethics Committee of our University (ruling no. 76543617.9.0000.5404/2017). All patients participating in the study signed the informed consent form.
Confidentiality of data
The authors declare that they have followed the protocols of their work center on the publication of patient data and that all the patients included in the study received sufficient information and gave their written informed consent to participate in the study.
Right to privacy and informed consent
The authors have obtained the written informed consent of the patients or subjects mentioned in the article. The corresponding author is in possession of this document.
Conflict of interest
The author(s) declare that there is no conflict of interest.
