Abstract
Pulmonary arterial hypertension is a chronic, progressive, and life-threatening disease in children with diverse causes of pulmonary arterial hypertension. The most severe cases of pulmonary arterial hypertension require aggressive treatments with systemic administration of continuous prostacyclin therapy, including treprostinil and epoprostenol. The successful use of continuous subcutaneous treprostinil therapy eliminates the need for an indwelling central venous catheter and its associated risks. However, pain at the subcutaneous infusion site, an expected side effect of this therapy, is often a deterrent to its widespread use. Effective subcutaneous treprostinil site maintenance and pain management is essential to achieve success with this therapy, but strategies surrounding site maintenance and pain control vary significantly between pediatric pulmonary hypertension treatment centers. In an attempt to standardize practice, a survey on the use of subcutaneous treprostinil and site maintenance and pain management strategies, as well as its perceived effectiveness, was disseminated to 13 pediatric pulmonary hypertension centers of the Pediatric Pulmonary Hypertension Network. Responses to the survey were collected and analyzed and were developed into a set of formalized strategies to facilitate knowledge sharing and standardization of practice.
Introduction
Current pediatric guidelines for treatment of severe pulmonary arterial hypertension recommend the use of continuous prostacyclin therapy in both the inpatient and ambulatory settings. 1 Continuous prostacyclin analogues (epoprostenol and treprostinil) are available for administration intravenously via a central line catheter or subcutaneously via a subcutaneous (SubQ) catheter (treprostinil only). Treprostinil is a synthetic prostacyclin analogue, which when administered subcutaneously, is absorbed rapidly with 100% bioavailability and elimination half-life of 2.9–4.6 h. 2 Effective SubQ administration of treprostinil eliminates the need for a central venous catheter and the associated risks therein. Continuous intravenous administration of prostacyclin can be complicated by bloodstream infection, superficial line infection, impaired line integrity, occlusion, and malposition. Current data suggest that pediatric patients receiving continuous intravenous prostacyclin therapy experience a total complication rate of 1.73 cases per 1000 line days. 3 These complications are burdensome to the patient and family, costly to the health care system, and in some circumstances (such as surgical placement/replacement of CVL) pose additional risk of morbidity and mortality to the patient. Administration of SubQ treprostinil eliminates these risks.
Pediatric patients treated with SubQ treprostinil therapy have demonstrated improvement in functional class, exercise capacity, and hemodynamics. 4 However, pain at the infusion site is the most common and expected side effect, and the successful use of SubQ treprostinil hinges on site maintenance and pain control. It has been reported that 85% of patients describe site pain and up to 23% of patients treated with SubQ treprostinil therapy discontinued long-term use due to site pain that was not well-controlled. 2 Specific strategies are required to alleviate SubQ treprostinil associated site pain, or at minimum, bring down to a level that is acceptable in daily life. However, site and pain management strategies are highly variable between patients and pediatric pulmonary hypertension (PH) treatment centers.
The mechanism of pain with use of SubQ treprostinil is postulated to be its potent local vasodilator effects and the resulting inflammatory response, as well as direct pain stimulation. The pain and inflammatory responses can vary between patients, but usually include site erythema, tenderness, swelling, induration, bleeding, and discharge. As these responses may range from mild to severe depending on the age of the patient and duration of therapy, pain management strategies must be tailored to the individual. Site pain and inflammation are typical in the first week after placing a new SubQ site. 4 Anecdotally, the perception of many providers is that younger patients tend to have less site reaction and pain. An array of anti-inflammatory and analgesic therapies are used both locally at the SubQ infusion site and systemically. The goals of site management strategies are to reduce inflammation, induce vasoconstriction of local blood vessels, blunt the pain response, and maximize the duration that the site is used.
Most PH centers utilize dedicated advanced practice nursing staff to work with the patient and family to minimize pain, maximize therapy effectiveness, and prevent discontinuation of SubQ treprostinil. Current approaches have been limited by lack of consensus from nursing experts in the field. To address this need, a working group of registered nurses and nurse practitioners who specialize in the care of pediatric PH patients was established to create a synthesized document of practice recommendations. This document addresses the PH nursing expert approach in caring for pediatric patients using SubQ treprostinil therapy, specifically regarding SubQ treprostinil site maintenance and pain management.
In an attempt to standardize practice, we categorized providers’ perceptions of the perceived effectiveness and utilization rates of various site pain maintenance and management measures. Creation of a formal set of practice recommendations was done under the guidance of the Pediatric Pulmonary Hypertension Network (PPHNet), a network of centers that include interdisciplinary clinical specialists, researchers, and providers, which brings a collaborative approach to improving care for children with pulmonary vascular disease.
Methods
In March 2019, at the PPHNet annual meeting, the Advanced Practice Provider and Nursing Committee convened and prioritized development of pain management and site management practice recommendations for SubQ treprostinil. A subcommittee was formed with 12 members. Over the spring of 2019, the subcommittee reviewed existing, center-specific SubQ treprostinil guidelines from six PPHNet centers. A draft of recommendations was created by collating common themes which were then reviewed and vetted via teleconference among the subcommittee members.
A formal survey was then constructed by four nurse practitioner committee members based on the consensus practice recommendations developed during the teleconference. The survey was piloted among subcommittee members and was distributed via email to nursing staff at all 13 PPHNet sites. Participants were invited to respond to the survey as a group. One survey per center was submitted. The survey used numeric and Likert scales to rank and categorize perceived effectiveness of common modalities used for routine site maintenance as well as pharmacologic and nonpharmacologic pain relief measures.
The common modalities for routine site maintenance assessed were the type of catheter used and dressing practices to secure the catheter. The type of catheters accepted for routine use for SubQ treprostinil (Cleo 90, Silhouette, Neria, and Quickset) were ranked from most used to least used on a numeric scale by each center. The Likert scale “never, sometimes, often, and always” was used to rank common routine practices for site dressings. The Likert scale “not helpful, somewhat helpful, neutral, helpful, and very helpful” was used to rank perceived effectiveness of pain management therapies. If a center did not have experience using a listed modality or therapy, “do not use” was an option. The percentage of efficacy was calculated using only the centers who reported using the specific modality or therapy. The results were analyzed descriptively with categorical data reported as percentages. The data were collected and analyzed using Research Electronic Data Capture 5 at Vanderbilt University, Nashville, Tennessee and Excel (Microsoft, Redmond, Washington).
Results
At the time of survey dissemination, 11 of the 13 PPHNet sites responded to the survey. Respondents included a mix of registered nurses and advanced practice providers (Table 1). The centers had experience treating pediatric PH patients with continuous SubQ treprostinil infusions and were actively treating >145 SubQ treprostinil patients at the time of survey completion.
Guideline contributors.
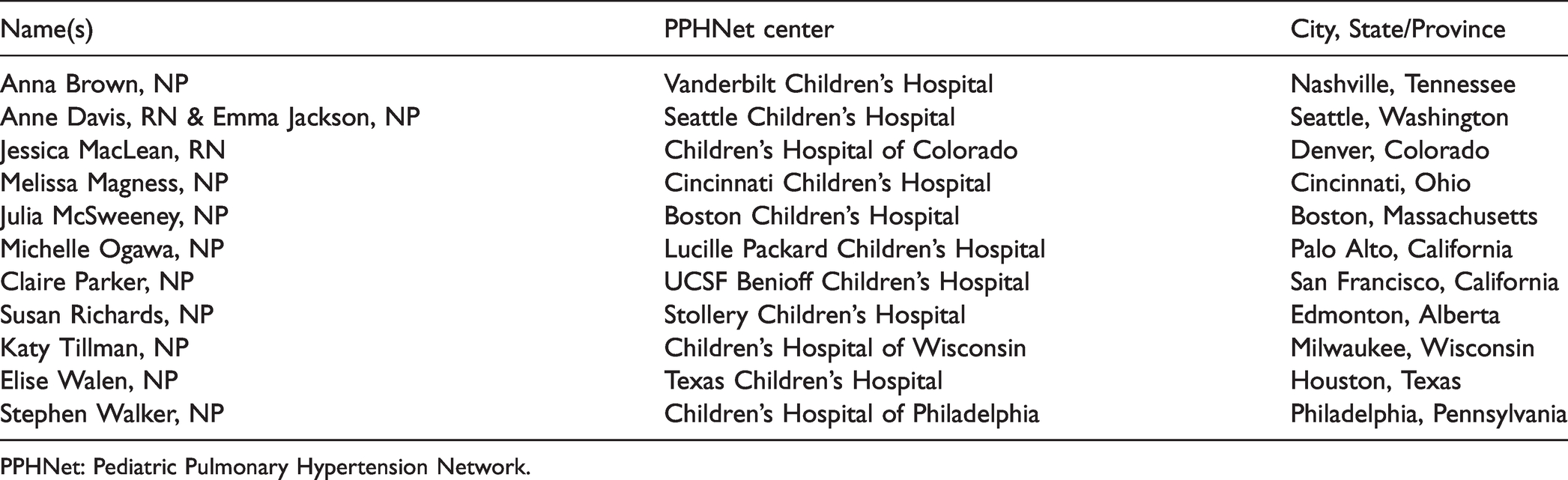
PPHNet: Pediatric Pulmonary Hypertension Network.
Nine of the 11 centers rated the Cleo catheter as the most often used SubQ treprostinil site. Six centers ranked the Silhouette catheter as the second most often used. The Neria and Quickset were also utilized, although the majority of centers did not use either of these types of sites.
Seventy-two percent of centers believed that SubQ site pain is most influenced by the rate of drug infusion (ml/h) as opposed to dose (ng/kg/min) or concentration (mg/ml). The range of maximum rate utilized by PPHNet programs is 0.03 ml/h to 0.05 ml/h (median 0.038 ml/h). Notably, two centers did not have a standard upper limit to the rate of SubQ treprostinil.
Systemic therapies
Results are shown in Fig. 1 for systemic therapies that >50% of centers reported using; 100% of centers that responded utilized non-opioid analgesics, including both acetaminophen and ibuprofen. Long acting second-generation H1 blockers, such as cetirizine, were utilized by all centers as well. Three centers use H1 blockers the first week of a new site, two centers have patients use them continuously, and the other six sites determine usage on an individual patient basis. Six of the centers identified ranitidine as their H2 blocker of choice. Please note this survey was taken prior to FDA removal of all ranitidine products. There was no consistent practice on dosing a neuropathic pain reliever, such as gabapentin; however, most centers reported using them only in an older pediatric patient population with severe pain. Of the centers that reported that they do not use opioids, several were concerned for opioid addiction and would consider switching to a different route of prostacyclin administration if their patient had SC site pain severe enough to warrant opioid use. Of note, the majority of all centers (73%) did not use systemic steroids. Of the remaining centers that used systemic steroids, two found them very helpful, while one center rated them as not helpful.
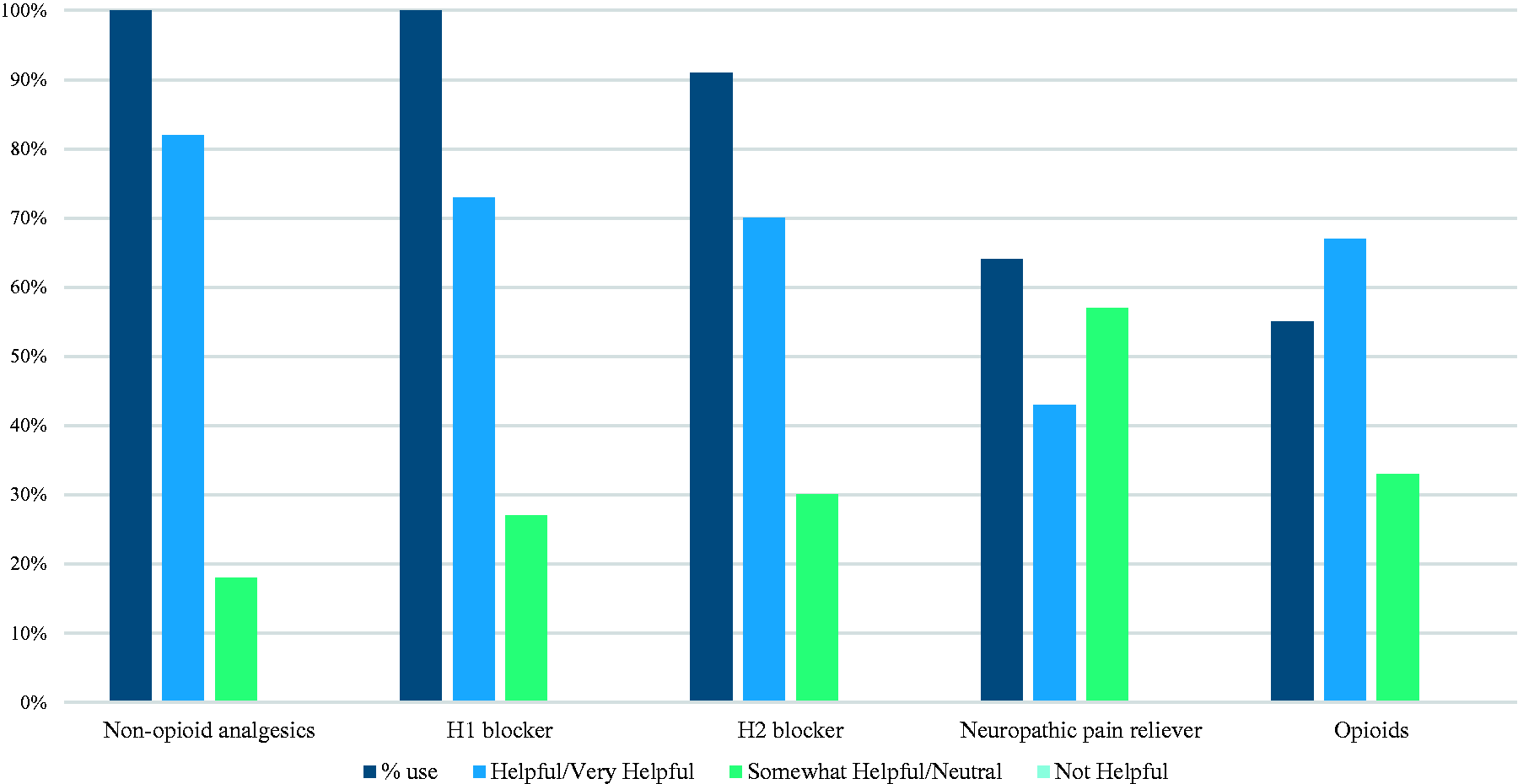
Systemic therapies.
Topical therapies
Results are shown in Fig. 2 for topical therapies that >50% of centers reported using. Topical anesthetic cream, such as lidocaine and prilocaine, is applied to the skin prior to site placement. Anesthetic patches, such as lidocaine, were helpful/very helpful when applied for 12 h on and 12 h off cycles. Steroid spray, such as fluticasone, may be used topically at the location of a new site, prior to placement. The notion behind using a steroid spray is that it is less greasy than a steroid cream and therefore does not interfere with dressing adhesiveness once the site is placed. However, a few centers commented that they have moved away from this practice due to perceived lack of efficacy. Pleuronic lecithin organogel (PLO gel) compounds contain ketoprofen, lidocaine, and gabapentin and may also contain ketamine, amitriptyline, and clonidine. Only 45% of sites reported using phenylephrine cream. Of the sites that use it, 80% of centers report that using phenylephrine cream prior to site placement is helpful/very helpful. Aloe Vera is also reported as low use with only two centers (18%) reporting use. One site found it helpful/very helpful, while the other site reported that it is not helpful. Only 27% of centers are using Cannabidiol (CBD) oil for SC site pain. Two centers (18%) report that it is helpful/very helpful, and one center reported that it is neutral.
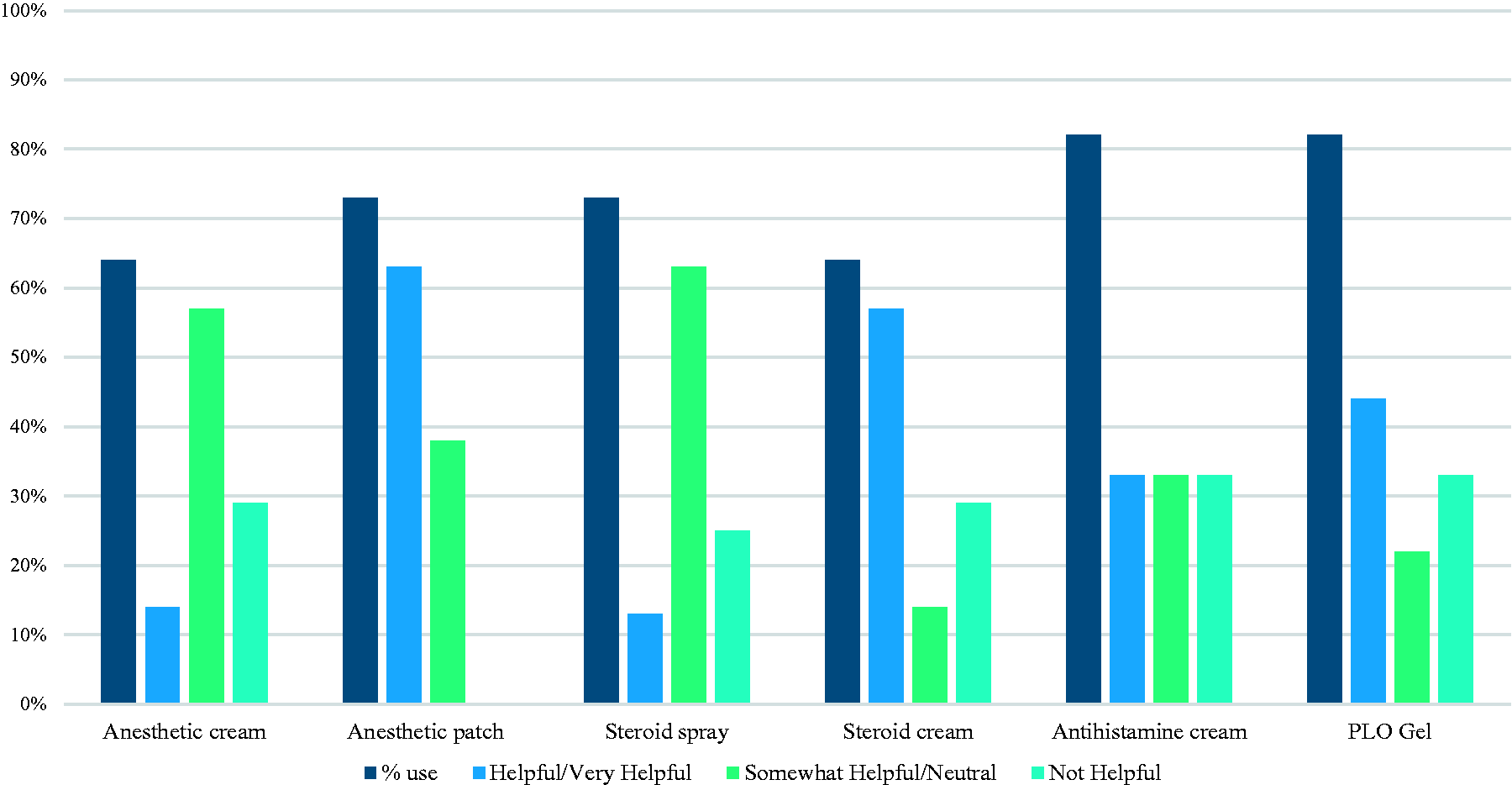
Topical therapies.
Non-pharmacotherapeutic therapies
Results are shown in Fig. 3 for non-pharmacotherapeutic therapies that > 50% of centers reported using.
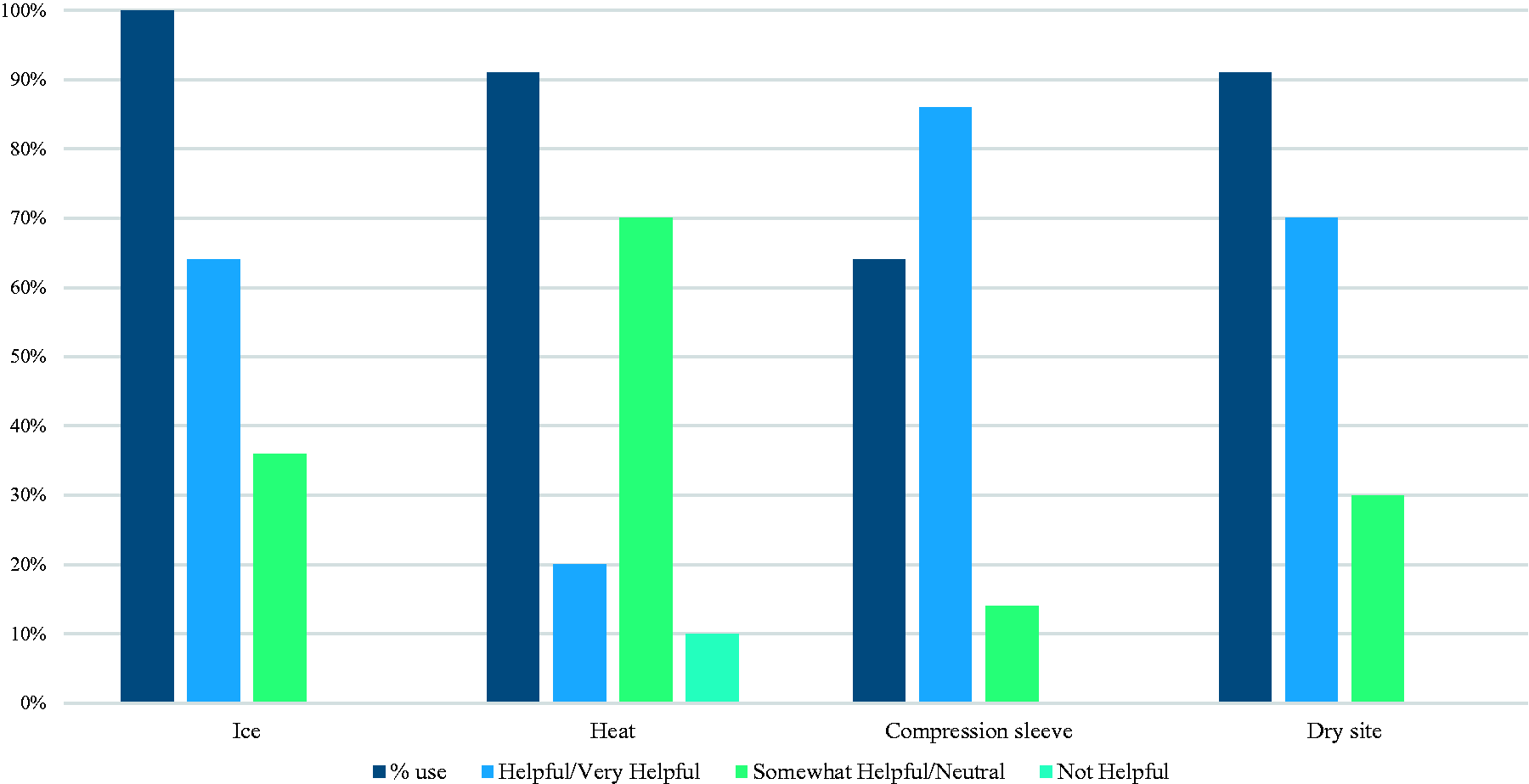
Non-pharmacologic therapies.
Discussion
Results from this survey reflect the general practices and opinions of registered nurses and advanced practice providers from 11 large PH Centers in North America. They have demonstrated extensive experience in managing SubQ treprostinil site pain and site management in children through years in practice and patient numbers. It is clear from survey results that there is variability in management techniques from center to center. However, survey results and evaluation of existing, center-specific SubQ treprostinil guidelines identified many uniform practices, which have been highlighted in Table 2. These practice recommendations may give direction to less experienced PH programs in developing their own SubQ site pain and management strategies.
Summary of recommendations.
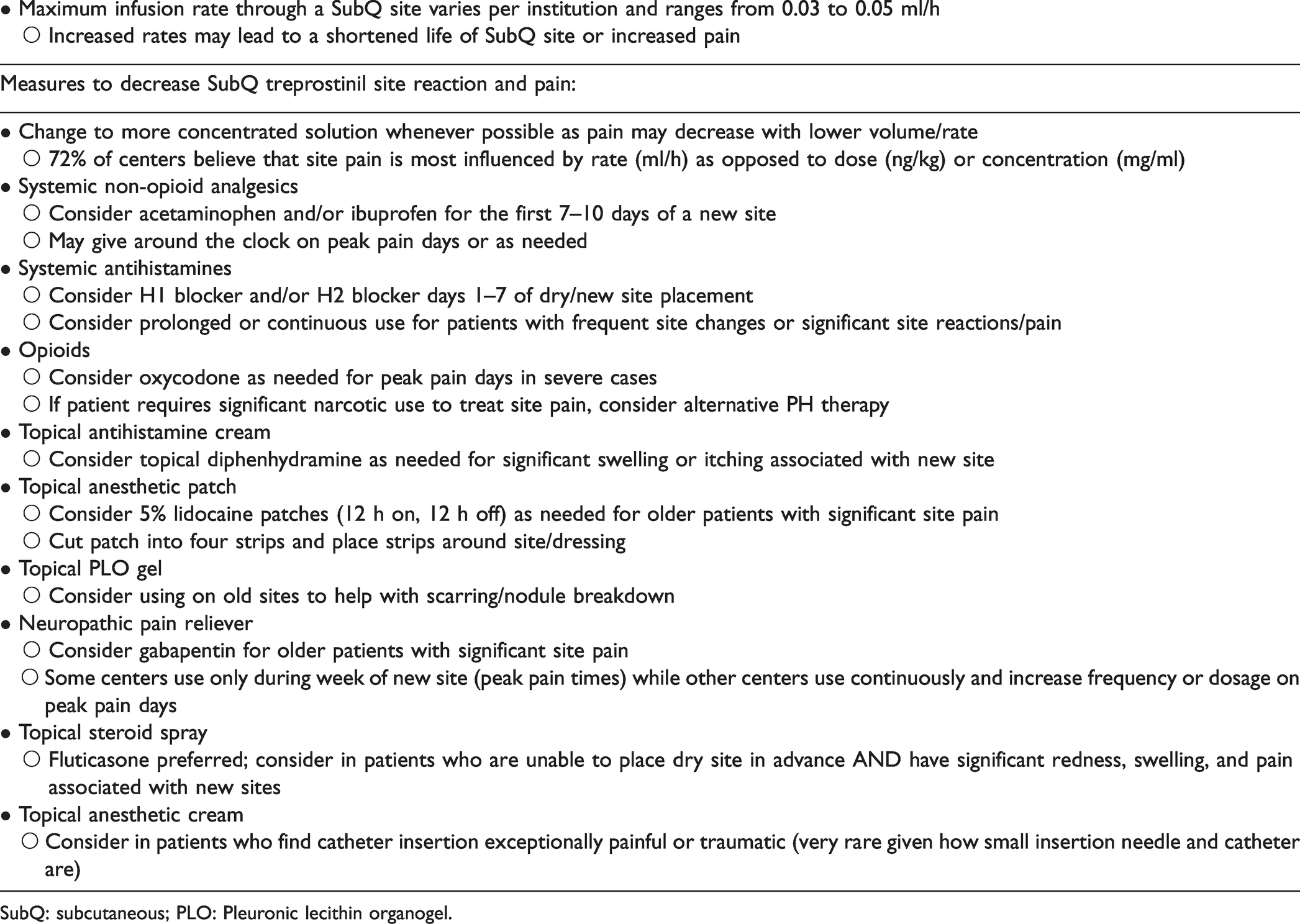
SubQ: subcutaneous; PLO: Pleuronic lecithin organogel.
Results identify strategies such as acetaminophen, ibuprofen, ice packs, and H1 blockers that are used by 100% of centers and are perceived by providers as helpful. These strategies should be considered as first-line interventions. Survey results also found that while CBD oil was only utilized by three centers, it was generally thought to be very helpful/helpful. This may give PH programs incentive to include CBD oil as a part of their pain management strategy. Interventions that had mixed results in perceived helpfulness might be viewed as second- or third-line strategies.
It is important to note that all centers emphasized that SubQ treprostinil site and pain management must be personalized to each patient. Anecdotally, some patients require minimal intervention while others require more aggressive pain management strategies, perhaps due to the variability in mechanism of pain in each patient, which is poorly understood. For this reason, centers often create a menu of site and pain management treatment strategies, which is used by the patient, parent, and provider to individualize a plan of care over time.
Direction for future studies should examine patient demographics as it pertains to pain and site management strategies. The registered nurses and advanced practice providers in the sub-committee agreed on the general statement that younger patients often require fewer pain management strategies in relation to SubQ treprostinil; however, there is no documented evidence. Future studies which examine patient and parent perspectives on SubQ site and pain management may also provide valuable insight to PH providers. Additional areas for future research would include description of pediatric patients that fail to tolerate continuous SubQ treprostinil therapy despite efforts and if a relationship exists between patient age and the preferred pain management and site maintenance strategies.
Conclusions
Our data suggest that the approach to SubQ site maintenance and pain control varies widely between PH centers; however, recurring themes emerged. The Cleo catheter was most frequently employed by participating centers. Site pain was perceived to be most influenced by rate of infusion (mL/h), as opposed to dose (ng/kg/min) or concentration (mg/mL) suggesting the degree of pain is largely related to the volume of medication infusing into the SubQ space. Systemic non-opioid analgesics and systemic antihistamines (H1 and H2 blockade) were used by most centers and perceived to be helpful. Anesthetic patch, steroid cream, PLO gel, and phenylephrine cream were the most frequently used topical therapies felt to be helpful. Placement of a dry site, use of a compression sleeve at the site, and topical ice were perceived to be helpful, nonpharmacologic therapies.
Limitations
The survey assessed the preferred practice at each participating PPHNet center, and the opinions and practices of pediatric PH centers not currently part of the PPHNet were not queried. The joint survey assumed that individual providers at PH centers share the same approach. The survey did not assess individual provider perceptions that may be present within an institution. The survey was a reflection of the provider’s perception of patient experience, not a direct assessment of patient perception. Similarly, the survey did not examine individual patients and the relative efficacy of any pain management or site maintenance strategy. Problematic or ineffective strategies were not assessed.
Conflict of interest
The author(s) declare that there is no conflict of interest.
Footnotes
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
