Abstract
Immunologic risk factors contribute to endothelial dysfunction and development of pulmonary vascular disease. Immune checkpoint inhibitors, used as immunotherapies for malignancies, have a wide range of reported immune-related adverse events. We retrospectively describe the impact of immune checkpoint inhibitors on the development of pulmonary vascular injury and right ventricular dysfunction as compared across both computed tomography and transthoracic echocardiography. Twenty-four of 389 patients treated with immune checkpoint inhibitors at a single academic center between 2015 and 2019 were evaluated. Thirteen (54%) patients were treated with anti-programmed cell death receptor 1 (PD-1), 8 (33%) with anti-programmed death receptor ligand 1 (PD-L1) therapy, and 3 (13%) with combination anti-PD-1 and anti-cytotoxic T-lymphocyte-associated antigen 4 (CTLA-4) therapy. At a median of 85 days of immune checkpoint inhibitor therapy, RVfwLS significantly increased from –20.6% to –16.7% (p = 0.002). After a median of 59 days of immune checkpoint inhibitor therapy, median pulmonary artery to aorta ratio worsened from 0.83 to 0.89 (p = 0.03). There was an correlation of duration of immune checkpoint inhibitor therapy (β = –0.574, p = 0.003) with percent change in RVfwLS. Patients who received anti-PD-1 therapy (β = –0.796, p = 0.001) showed the greatest correlation of duration of immune checkpoint inhibitor therapy with percent change in RVfwLS. Exposure to immune checkpoint inhibitors are associated with RV dysfunction and vascular changes as measured by strain and computed tomography, respectively.
Immune checkpoint inhibitors (ICIs) have emerged as transformative therapies used to treat many thoracic, urologic, and dermatologic malignancies. The primary targets for ICIs include programmed cell death receptor-1 (PD-1), programmed death receptor ligand 1 (PD-L1), and cytotoxic T-lymphocyte-associated antigen 4 (CTLA-4) found on tumor cells and CD4 T-cells, including T regulatory cells (Tregs). The use of these immunotherapies can result in significant immune-related adverse events (irAEs), including cardiopulmonary toxicities like myopericarditis, conduction abnormalities, and left ventricular (LV) systolic dysfunction. 1
T lymphocytes and specifically Tregs play a role in the pathogenesis of pulmonary vascular disease. 2 , 3 Tamosiuniene et al. demonstrated that immune reconstitution with Tregs prior to vascular injury reduced progression of pulmonary hypertension (PH) normally observed in T-cell-deficient rats. This protection afforded by Treg cells was reversed with blockade of PD-L1 with anti-PD-1 ICI therapy. 4 , 5 Fournel et al. previously reported an increased pulmonary artery to aorta ratio (PA/Ao) in humans following exposure to anti-PD-1 therapy. 6 These findings collectively exploring the interactions of T cells, ICI therapy, and pulmonary vascular changes highlights a potential unrecognized relationship between pulmonary vascular toxicity and treatment with ICIs.
Speckle-tracking echocardiography is a Doppler-based method that allows for evaluation of longitudinal myocardial strain, and has been validated for detection of subclinical cardiac dysfunction. 7 , 8 Other methods for evaluating right ventricular (RV) function, such as tricuspid annular plane systolic excursion (TAPSE), rely on surrogate measures of global RV function, while RV strain measures both regional (RVfwLS) and global RV longitudinal contractility; RV longitudinal systolic strain (RVLSS). RVLSS has the highest correlation with cardiac magnetic resonance imaging derived RV volumes, ejection fraction, and, in patients treated with certain chemotherapeutics, can detect preclinical myocardial dysfunction. 8 , 9 Additionally, enlargement of the PA/Ao on computed tomography (CT) scans correlates with worsening PH. 10
To ascertain whether there is a relationship between ICI therapy and pulmonary vascular toxicity, we examined the development of subclinical pulmonary vascular disease as determined by the prespecified outcomes of change in right ventricular free wall longitudinal systolic strain (RVfwLS) and PA/Ao ratio among patients exposed to ICI therapy.
Methods
Population and setting
We reviewed charts of patients from our Hospital who had confirmed malignancy treated with ICIs (Nivolumab, Pembrolizumab, Atezolizumab, Durvalumab, and/or Ipilimumab) between 1 June 2015 and 31 December 2019. The study was approved by the Institutional Review Board.
Data collection and definitions
Demographic and clinical data were collected from the electronic medical records. RV strain and PA/Ao ratio were predetermined primary endpoints in this study. A blinded retrospective RV speckle tracking analysis was performed using a RV-focused apical four-chamber view with R-R gating in TOMTEC (Phillips, USA). 7 A blinded analysis of CT scans was performed by two observers, to measure PA and ascending Ao diameters at the level of the bifurcation. 10
Statistical analysis
The results are reported as medians and interquartile ranges. Categorical variables are reported as counts and percentages. Differences in continuous variables were compared using the paired t-test. Univariate analyses were performed to evaluate whether hypothesized variables correlated with percent change in RVfwLS. We performed analyses with GraphPad Prism v8.0 and STATA v16.1 software.
Results
Demographics, clinical characteristics, and treatment strategies
From 1 June 2015 to 31 December 2019, 392 patients were treated with one or more of the above-mentioned ICIs. Baseline and follow-up treatment echocardiograms performed within one year of starting ICI therapy were available in 24 subjects. All subjects were on ICI therapy at the time of their follow-up echocardiogram. Demographics, clinical characteristics, therapies, and outcomes are summarized in Table 1. Thirteen (54%) patients were treated with anti-PD-1 therapy, 8 (33%) with anti-PD-L1 therapy, and 3 (13%) with combination anti-PD-1 and anti-CTLA-4 therapy.
Demographics, characteristics, echocardiographic findings, computed tomography measurements at baseline and after immune checkpoint inhibitor therapy.
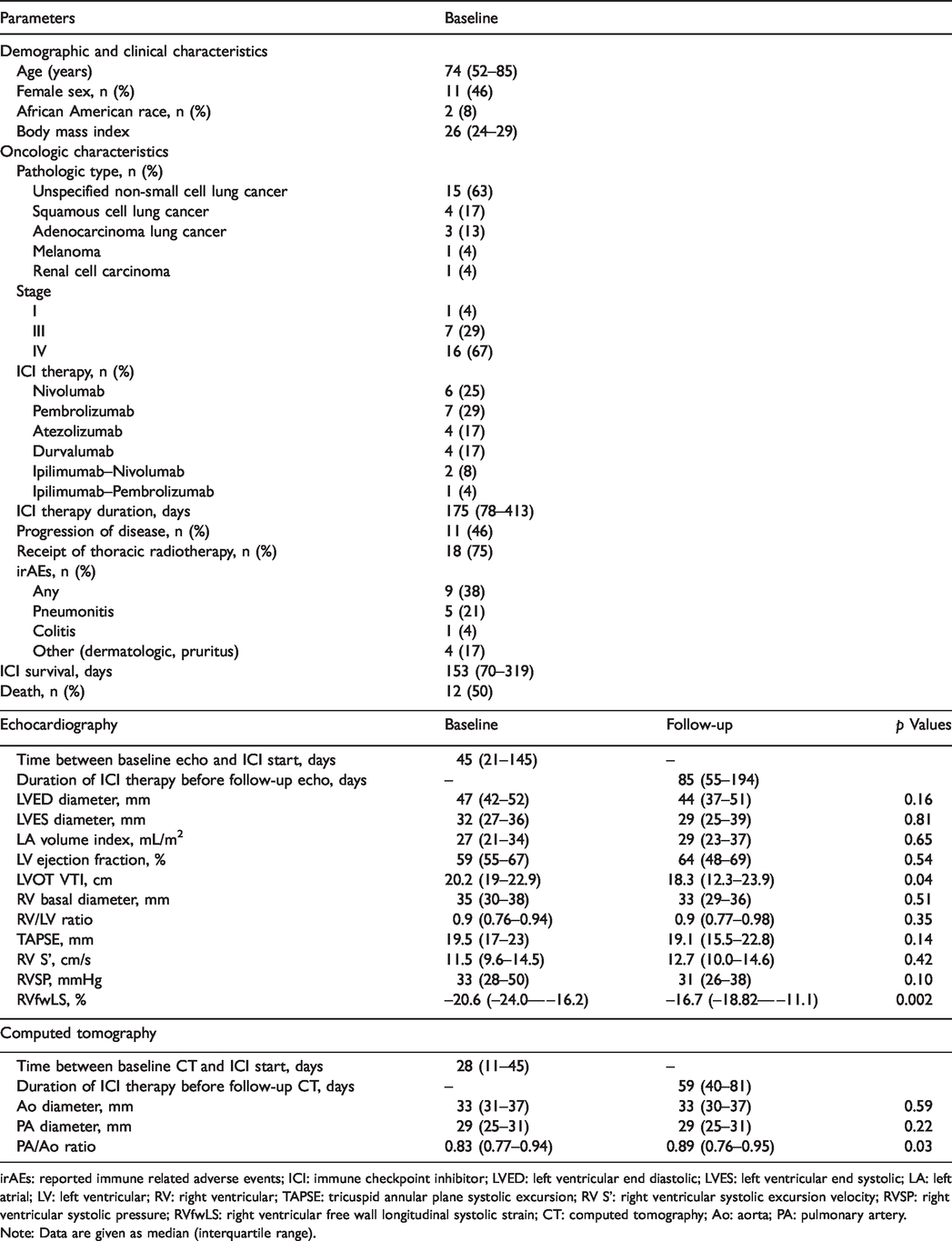
irAEs: reported immune related adverse events; ICI: immune checkpoint inhibitor; LVED: left ventricular end diastolic; LVES: left ventricular end systolic; LA: left atrial; LV: left ventricular; RV: right ventricular; TAPSE: tricuspid annular plane systolic excursion; RV S': right ventricular systolic excursion velocity; RVSP: right ventricular systolic pressure; RVfwLS: right ventricular free wall longitudinal systolic strain; CT: computed tomography; Ao: aorta; PA: pulmonary artery.Note: Data are given as median (interquartile range).
Univariate analysis of percent change in RVfwLS with duration of ICI therapy.

ICI: immune checkpoint inhibitor; XRT: radiotherapy; PD-1: programmed cell death receptor-1; PD-L1: programmed cell death ligand 1; CTLA-4: cytotoxic T-lymphocyte-associated antigen 4.
Patients had normal biventricular size and function at baseline echocardiography. After a median 85 days of ICI therapy, as compared to baseline, left ventricular outflow tract velocity time integral (LVOT VTI) significantly decreased (18.3 vs. 20.2, p = 0.04), and RVfwLS significantly increased (–16.7% vs. –20.6%, p = 0.002). There were no other statistically significant differences in echocardiographic measures of RV or LV function and size.
After a median of 59 days of ICI therapy, as compared to baseline, median PA/Ao ratio increased from 0.83 to 0.89 (p = 0.03). No patients were considered to have aortic disease or significant aortic dilatation. Inter-observer agreement of Ao and PA measurements were excellent, as assessed by interclass correlation coefficient (ICC) (interobserver ICC = 0.95 and 0.98 for Ao and PA, respectively).
On univariate analysis, there was an association of duration of ICI therapy (β = –0.574, p = 0.003) with percent change in RVfwLS. We repeated the univariate analysis stratified by hypothesized confounders including progression of disease, receipt of radiotherapy, and type of immunotherapy. Upon stratification, all confounders showed consistent effect direction. Notably, patients who received anti-PD-1 therapy (β = –0.796, p = 0.001) demonstrated the greatest association of duration of ICI therapy with percent change in RVfwLS (Table 2).
No patients were documented to have been started on therapies specifically targeting PH or left ventricular dysfunction.
Discussion
ICI therapy has been associated with significant cardiotoxic irAEs involving the myocardium, pericardium, and conduction system. 1 Here, we demonstrate that exposure to ICIs are associated with RV dysfunction and vascular changes as measured by strain and CT, respectively. We affirm and expand on the finding of Fournel et al. by showing an association with enlarging PA/Ao ratio in patients treated with anti-PD-L1 and anti-CTLA-4 therapy in addition to anti-PD-1 therapy. We also demonstrate an association with worsening RV function as measured by RVfwLS. Interestingly, duration of exposure to ICIs was most strongly correlated with changes in RV strain, an effect that was mirrored in stratified analyses. The large correlation coefficient associated with anti-PD-1 therapy raises interesting questions about the differential effect of ICI treatment on the pulmonary vasculature.
There are several limitations to our study to consider. The effects of ICI therapy on RV dysfunction should be interpreted with caution, as this was a retrospective study that lacked a control group. Furthermore, echocardiograms were ordered as part of routine clinical care, so timing and availability were not uniform across the cohort introducing selection bias. Additionally, the primary thoracic malignancy represented in this cohort may be an important confounder in the association of RVfwLS and ICI therapy. Finally, although the median age of our cohort exceed the reference values typically reported, referencing the change in strain per individual should help to mitigate this constraint. 11
Our findings coupled with the above-mentioned animal and human basic science data raises interesting questions about ICI therapy and the role T cells potentially play in the pathogenesis of pulmonary vascular injury. Future studies should prospectively examine the correlation of ICI therapy on the development of pulmonary vascular disease and the mechanistic role of T-cell and T regulatory cell function on the pulmonary vasculature.
Footnotes
Conflict of interest
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: R.K. reports grants and personal fees from Boehringer Ingelheim, grants from PneumRx (BTG), grants from Spiration, grants and personal fees from AstraZeneca, personal fees from CVS Caremark, personal fees from Aptus Health, grants and personal fees from GlaxoSmithKline, personal fees from Boston Scientific, personal fees from Boston Consulting Group, outside the submitted work. V.V. reports grants from Takeda, other from Novocure, other from AstraZeneca, outside the submitted work. M.J.C. reports personal fees from Actelion Pharmaceuticals, personal fees from Bayer, personal fees from United Therapeutics, personal fees from Gilead, other from Reatta Pharmaceuticals, outside the submitted work. R.M., R.A., I.G., and C.M. have no conflicts of interest.
Ethical approval
The study was performed according to ethical standards of the 1964 Declaration of Helsinki and was approved by the Northwestern Memorial Hospital institutional review board. The study was approved under institutional IRB STU00210793. Written informed consent was waived.
Contributorship
R.M. provided substantial contribution to the conception, design, data acquisition, analysis, interpretation, drafting and revision of the final manuscript. R.A., I.G., C.M., R.K., V.V., and M.J.C. provided substantial contribution to the conception and design of the work, interpretation of the data, and revision of the final manuscript.
Guarantor
M.J.C.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article: This research was supported, in part, by the National Institutes of Health’s National Center for Advancing Translational Sciences, Grant Number UL1TR001422. The funding source had no role in study design, data collection, analysis, interpretation, writing the report, or decision to submit report for publication. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. R.M. is supported by the T32HL076139-16.
