Abstract
We report the case of 63-year-old man, complaining of dyspnea and with abnormal systolic motion of the interventricular septum at echocardiography, referred for coronary angiography and suspect coronary artery disease. In the presence of normal coronary angio, a specific work-up showed chronic thromboembolic pulmonary hypertension requiring pulmonary endarterectomy. The case highlights the need for a global cardiovascular and imaging approach in presence of poorly specific symptoms and signs of coronary artery disease.
Keywords
A 63-year-old man, complaining of effort dyspnea and with abnormal systolic motion of the interventricular septum at echocardiography, even in the absence of any cardiovascular and venous thromboembolic risk factors, was referred for coronary angiography for suspect coronary artery disease. Rest electrocardiogram showed sinus rhythm and diffuse ST-depression (Fig. 1, up, left); admission echocardiography revealed normal left ventricular dimensions, mild hypertrophy and moderate left ventricular dysfunction (LVEF 45%) with abnormal septal motion, dilated right chambers, moderate tricuspid regurgitation with a 102 mmHg gradient (Fig. 1, up, mid-right). Coronary angio was normal; therefore, a CT scan was performed and showed eccentric thrombosis in the right pulmonary artery (Fig. 1, down, left) extending backwards to the bifurcation of the pulmonary trunk. Multiple blood clots were found in superior and inferior branches of the left pulmonary artery. Right heart catheterization confirmed precapillary pulmonary hypertension (CO 3.5 l/m, IC 1.9 l/m × m2, mPAP 53 mmHg, wedge pressure: 5 mmHg, RVP: 1103 dyne/s/cm
5
); coronary angio was normal (Fig. 1, down, mid). A more careful analysis of admission electrocardiogram may reveal an S1Q3T3 aspect with localized ST-depression in V1-2 leads highly suggestive for right ventricular overload rather than myocardial ischemia. Early anticoagulation therapy (warfarin) was started during hospitalization. Pulmonary endarterectomy was therefore performed with significant clinical improvement (WHO class II) (Fig. 1, down, right). The patient was discharged in therapy with warfarin; six-month follow-up was uneventful.
Up, left: admission electrocardiogram showing an S3Q3T3 aspect with localized ST-depression in V1-2 leads; up, mid-right: 2D 4-chamber echocardiography showing left ventricular dysfunction, dilated right chambers, moderate tricuspid regurgitation; down, left: CT scan with pulmonary embolism; down, mid: normal coronary angio; down right: surgery specimen after pulmonary endarterectomy.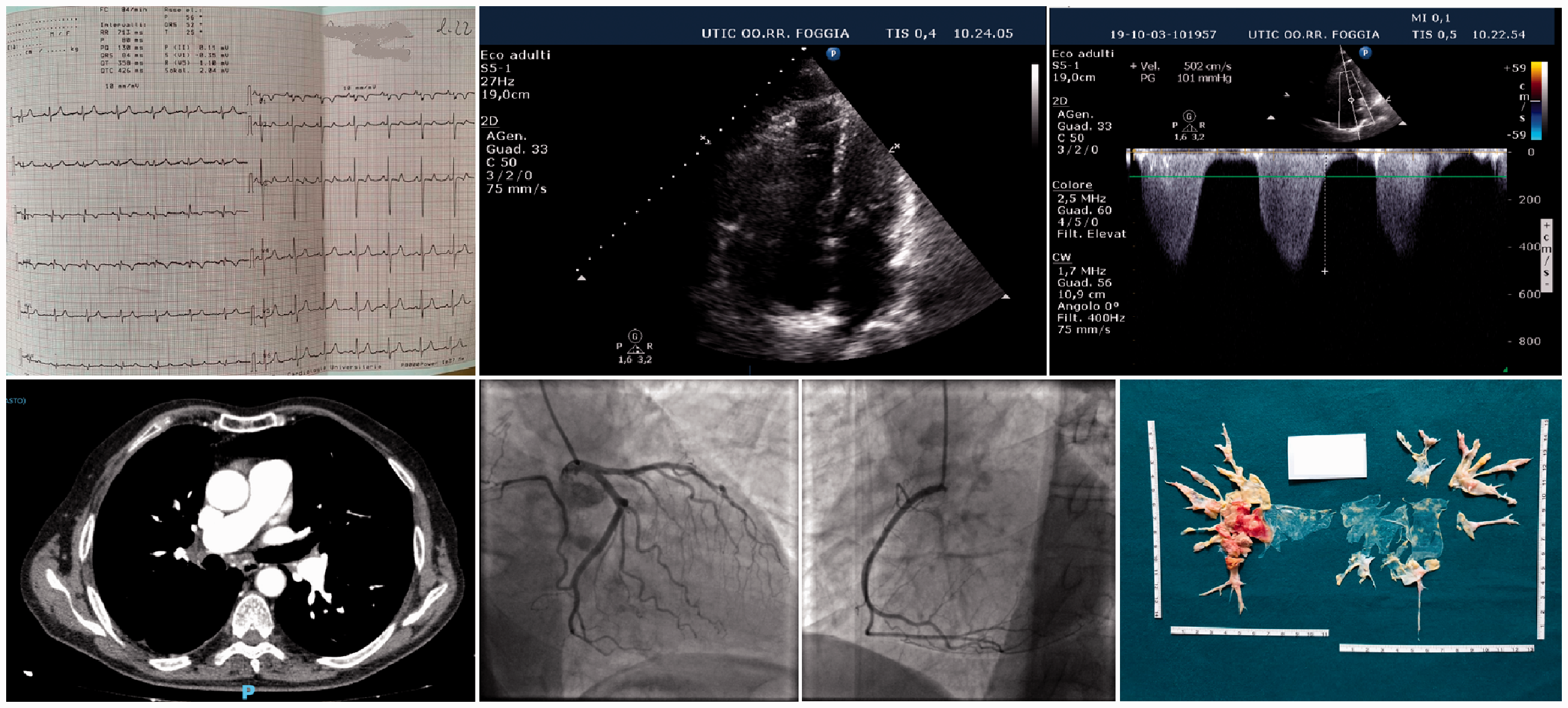
This case highlights the need for a comprehensive cardiovascular approach in case of symptoms poorly specific for coronary artery disease. In case of dyspnea and no evidence of coronary atherosclerosis, even pulmonary hypertension should be considered.
Echocardiography is a fast and easily available tool for the first-line approach to such patients but a systemic approach, not limited to the single cardiovascular disease, is essential. As shown in this report, echocardiography is essential as a screening test for several cardiac conditions including pulmonary hypertension in case of patients complaining of dyspnea; further comprehensive cardiovascular approach and right heart catheterization according to the international guidelines 1 may be required in case of intermediate or high echocardiographic probability of pulmonary hypertension.
In our case the diagnosis was made at late stage of patient pathway, highlighting the need for correct interpretation of echocardiographic findings: “abnormal septal motion” is the result of intraventricular coupling, as the result of right ventricular pressure overload upon the left side.
Echocardiography should be performed by experienced cardiologists and pulmonary hypertension should be carefully considered in case of abnormal systolic motion of the interventricular septum. Even a diagnosis of pulmonary thrombo-embolism exclusively based on echocardiography may be occasionally missed without a careful diagnostic work-up. 2
After a preliminary screening suspect for pulmonary hypertension and/or chronic thrombo-embolic etiology, the patients should be referred to tertiary centers with specific and multi-professional expertise (heart and thoracic imaging).3–6
