Abstract
Experimental models of sepsis in small and large animals and a variety of in vitro preparations have established several basic mechanisms that drive endothelial injury. This review is focused on what can be learned from the results of clinical studies of plasma biomarkers of endothelial injury and inflammation in patients with sepsis. There is excellent evidence that elevated plasma levels of several biomarkers of endothelial injury, including von Willebrand factor antigen (VWF), angiopoietin-2 (Ang-2), and soluble fms-like tyrosine kinase 1 (sFLT-1), and biomarkers of inflammation, especially interleukin-8 (IL-8) and soluble tumor necrosis factor receptor (sTNFr), identify sepsis patients with a higher mortality. There are also some data that elevated levels of endothelial biomarkers can identify which patients with non-pulmonary sepsis will develop acute respiratory distress syndrome (ARDS). If ARDS patients are divided among those with indirect versus direct lung injury, then there is an association of elevated levels of endothelial biomarkers in indirect injury and markers of inflammation and alveolar epithelial injury in patients with direct lung injury. New research suggests that the combination of biologic and clinical markers may make it possible to segregate patients with ARDS into hypo- versus hyper-inflammatory phenotypes that may have implications for therapeutic responses to fluid therapy. Taken together, the studies reviewed here support a primary role of the microcirculation in the pathogenesis and prognosis of ARDS after sepsis. Biological differences identified by molecular patterns could explain heterogeneity of treatment effects that are not explained by clinical factors alone.
Sepsis and acute respiratory distress syndrome (ARDS) are heterogeneous syndromes associated with high mortality rates and substantial healthcare costs in critically ill patients.1–4 Sepsis is defined as life-threatening organ dysfunction due to a dysregulated host response to infection. 5 The clinical manifestations of severe sepsis syndrome involve organ dysfunction including encephalopathy, acute kidney injury, coagulopathy, and acute lung injury (ALI) or ARDS.
The initial site of injury in ARDS after sepsis or other etiologies of indirect lung injury is the injured lung microcirculation that leads to increased permeability pulmonary edema resulting in bilateral alveolar infiltrates on the chest radiograph and arterial hypoxemia.6,7 Considerable progress has been achieved by studying ARDS using broad clinical and physiologic criteria as illustrated in the Berlin Criteria for ARDS and the approach taken by the NHLBI ARDS network in testing therapies by the broad definition of bilateral pulmonary infiltrates and a Pa02/Fi02 < 300 mmHg. However, the failure of pharmacologic therapies in ARDS highlights the importance of recognizing the heterogeneity of ARDS and finding approaches to classify ARDS patients in categories or phenotypes that might be responsive to specific therapeutic approaches that may not be effective in all ARDS patients. Thus, in keeping with the goal of personalized medicine, there is a high priority for matching the optimal treatment to the appropriate patients by identifying meaningful subtypes within a heterogeneous population of critically ill patients. 8 For targeted therapies, “splitting” study populations into endotypes on the basis of differences in biology—by biomarker concentrations, gene expression profile, or genotype—may enhance our ability to identify effective treatments.
Several clinical disorders can precipitate ARDS, including pulmonary or non-pulmonary sepsis, pneumonia, and aspiration of gastric contents. While there are several important clinical and demographic risk factors for both sepsis 9 and ARDS,10–12 this review will focus on the biological mechanisms involving the microcirculation in the development of ALI after sepsis in ARDS patients. We will discuss recently published biomarker studies to highlight what is known about sepsis-induced endothelial injury in humans and then describe the relationship of endothelial injury in sepsis to ARDS with an emphasis on human studies.
Identifying cases of sepsis for clinical and research purposes is challenging and the approach has changed over time. 13 In this article, we discuss studies that have used various definitions of sepsis contemporary to the date of their publication. Similarly, we will use the terms ALI and ARDS interchangeably and discuss studies that identified this outcome by a variety of evolving criteria. 6
Endothelial injury from human sepsis
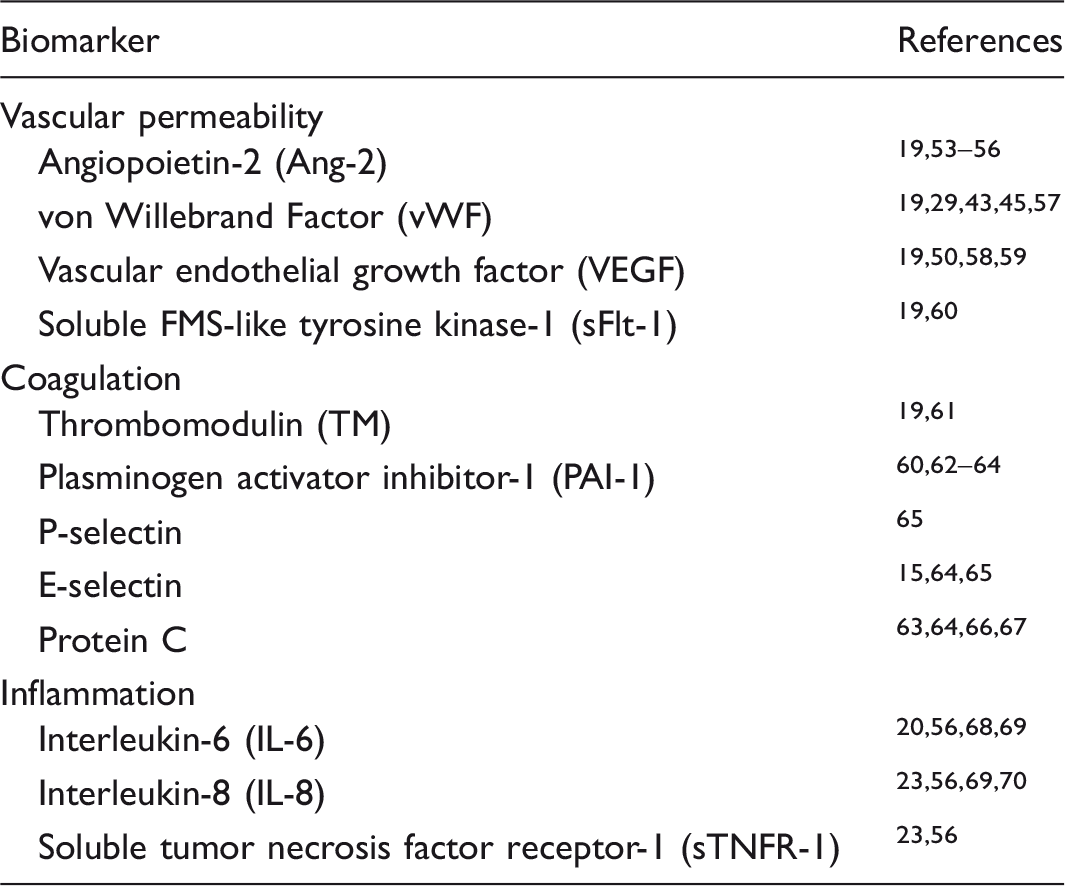
The endothelial lining is in continuous contact with circulating cells and soluble proteins (Fig. 1). The importance of the vascular endothelium in the pathophysiology of sepsis is well established and is regulated by pathways that control vascular permeability, coagulation, and systemic inflammation (Table 1).14–16 Severe sepsis causes an upregulation of several pro-inflammatory adhesion molecules, release of pro-inflammatory mediators including cytokines and lipid products, and is accompanied by procoagulant factors, activated neutrophils, platelets, and monocytes, all of which disrupt the barrier function of the microcirculation and also result in impaired tissue perfusion and oxygenation.16,17 Figure 1 highlights some of these pathways of injury. We describe the findings from three recent publications of prognostic biomarker studies in large cohorts of patients with sepsis to frame what is currently known about the importance of the vascular endothelium in predicting clinical outcomes after sepsis. In the next section, we will discuss the role of endothelial injury in the pathogenesis and prognosis of ARDS after sepsis.
The pathways by which sepsis induces injury to the endothelium. Sepsis upregulates the expression of selectins on the endothelium (P- and E-selectins), to which activated leukocytes (both neutrophils and monocytes) and platelet aggregates can adhere, and induce an increase in endothelial permeability. The potential role of neutrophil extracellular traps (NETS) and histone release is also included as well as olfactomedin 4, lipocalin 2, and CD 24, and bacterial permeability increasing protein, products primarily of neutrophils. Some circulating factors in the plasma are both biomarkers of injury and also enhance the injury, including Ang-2 and VEGF. In addition, the diagram shows circulating factors that enhance inflammation such as IL-8 and IL-6, sTNFr-2. Markers of endothelial injury also include vWF and sFLT-1, the circulating VEGF receptor. Also noted in the diagram are components of the activated protein C complex including protein C, protein S, factor V, and thrombomodulin because sepsis deranges the normal function of activated protein C leading to a pro-coagulant environment. Selected clinical studies of endothelial and inflammatory biomarkers in sepsis.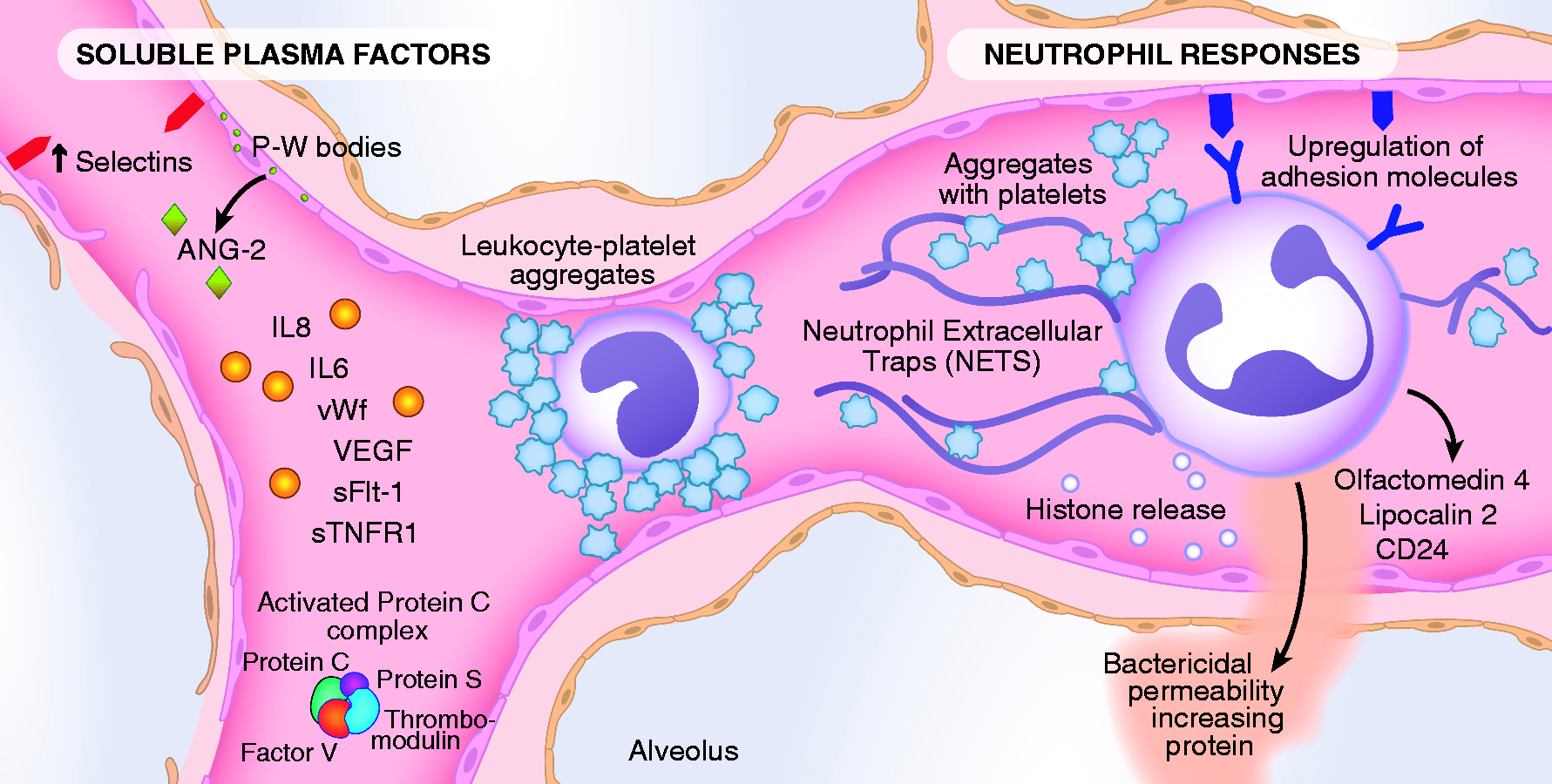
Two recently published studies leveraged clinical data and biospecimens from the Protocolized Care for Early Septic Shock (ProCESS) trial 18 to test the prognostic value of biomarkers representing various domains of sepsis pathophysiology. The ProCESS trial was a multi-center randomized control trial (RCT) that enrolled patients with sepsis early in the course of illness, while they were still in the Emergency Department. The size of the trial and the study design targeting intervention for early sepsis lends strength to the two biology studies described below.
In 2017, Hou et al. reported results from a large biomarker study of 1341 individuals enrolled in the ProCESS trial split into derivation and validation subgroups. 19 The authors measured baseline plasma levels of several proteins associated with endothelial cell permeability and hemostasis and tested the associations with mortality. The baseline values of several markers of endothelial injury were higher in patients who died compared to those who survived, including angiopoietin-2 (Ang-2), soluble fms-like tyrosine kinase 1 (sFLT-1; the soluble vascular endothelial growth factor [VEGF] receptor), thrombomodulin (TM), and von Willebrand factor (vWF). The authors analyzed the prognostic value of a panel of multiple biomarkers to identify patients with septic shock who had an increased risk of death. Lactate is a biomarker indicating impaired oxygen delivery to tissues and is used in clinical practice to identify high-risk patients with sepsis and to guide fluid resuscitation. Sequential Organ Failure Assessment (SOFA) score predicts mortality among patients with suspected infections and is commonly used as a marker of severity of illness in clinical research. 5 Interestingly, sFLT-1 had a point estimate for mortality discrimination (derivation area under the curve [AUC] = 0.74; validation = 0.70), similar to lactate (AUC = 0.74) and SOFA score (AUC = 0.73). Models testing if sFLT-1 added prognostic value to multivariate models incorporating lactate or SOFA score were not reported. The plasma levels of the biomarkers were not affected by the resuscitation strategies tested in the ProCESS trial. The resuscitation treatment protocols may not have altered mortality because they did not have a direct effect on altering the fundamental pathways of endothelial injury, as reflected in part by the levels of the circulating plasma biomarkers. Because several of the markers were associated with higher mortality, the results support the importance of endothelial injury in the pathogenesis of poor clinical outcomes in sepsis and suggest that measuring sFLT-1 in patients with sepsis may help identify those patients at the highest risk for death. However, based on the data in this study, it is not clear if sFLT-1 would add prognostic value beyond lactate and SOFA score.
Findings from a separate biomarker study conducted in 628 of the participants enrolled in the ProCESS trial were reported by Kellum et al. in 2017. 20 In this study, the authors made serial measurements (baseline, 6, 24, and 72 hours after initiation of study treatment) of plasma and urine biomarkers representative of four pathophysiologic domains: inflammation, coagulation, oxidative stress, and tissue hypoxia. For each domain, a primary marker and up to two secondary markers were measured as follows: inflammation: interleukin (IL)-6 (primary), tumor necrosis factor (TNF), and IL-10; coagulation: thrombin-antithrombin complex (TAT) (primary) and D-dimers; oxidative stress: urine isoprostane; and tissue hypoxia: lactate. The authors tested the association of the biomarkers with mortality and also used linear mixed effects models to determine if the trajectory of the biomarker measurement differed by treatment protocol. As in the study by Hou et al., 19 all of the biomarkers were higher at baseline among those who died compared to survivors. Despite these associations, none of the biomarkers alone, or models with combinations of biomarkers, discriminated well for mortality. Although lactate was the best-performing biomarker, when added to a parsimonious regression model using clinical variables, it did improve the area under the receiver operating characteristic (ROC) curve for predicting death among patients with sepsis. Similar to the findings reported by Hou et al., the biomarker profiles over time were not significantly different among the three resuscitation treatment arms of the ProCESS trial. The authors analyzed treatment effect on mortality among quartiles of the baseline biomarker measurements. Contrary to their hypothesis, the authors found an interaction between treatment effect and baseline IL-6 and IL-10 and mortality, suggesting that protocol-based resuscitation benefited patients with less-inflammation. In other words, among individuals with lower baseline inflammatory biomarkers, the group that received more intravenous fluids, had a lower mortality rate than individuals who received less intravenous fluids. A similar interaction was found in a secondary analysis of data from patients with ARDS enrolled in the Fluid and Catheter Treatment Trial (FACCT). 21 Famous et al. found that patients with a subphenotype characterized by lower inflammatory markers had a differential response to fluid therapy. Mortality in this group with less inflammation was 26% with fluid-conservative strategy versus 18% with fluid-liberal strategy. 22 Taken together, these findings from ProCESS and FACCT suggest that defining a biologic profile using markers of inflammation early in the course of critical illness could guide clinical decision-making. While the mechanisms underpinning these observations are not clear, both studies suggest that a more liberal fluid resuscitation strategy may benefit critically ill patients with less inflammation.
Taken together, the findings from these two biomarker studies of patients enrolled in the ProCESS trial indicate that patients with sepsis who develop more severe disturbances in any of the domains studied—inflammation, coagulation, endothelial permeability, oxidative stress, and tissue hypoxia—have a worse prognosis and higher mortality rates. Thus, these two recent clinical studies confirm experimental data that have identified the severity of endothelial injury and inflammation as major mechanisms driving the severity of organ injury. However, these studies find that the levels of plasma biomarkers did not add substantial prognostic value beyond models that incorporate clinical risk factors and plasma lactate.
Mikacenic et al. recently published results from a study with a large derivation and internal and external validation cohorts describing a two-biomarker model that identifies patients at low risk for death and organ dysfunction after sepsis. 23 The authors studied patients admitted to the ICU in academic institutions enrolled in prospective cohort studies of patients with systemic inflammatory response syndrome (SIRS), most of whom had sepsis. The derivation and internal validation cohort enrolled participants between 2006 and 2010 and obtained plasma samples within 24 h of ICU admission. The external validation cohort enrolled participants between 1999 and 2010 and obtained plasma samples within 48 h of ICU admission. The investigators tested the value of a panel of biomarkers of inflammation, microvascular injury, and apoptosis along with a panel of clinical predictors and developed a model to predict mortality. Specifically, the authors measured several plasma biomarkers including interleukin-8 (IL-8) and soluble tumor necrosis factor receptor 1 (sTNFR-1) within 24 h of ICU admission in the derivation and internal validation cohort. The authors analyzed the data using least absolute shrinkage and selection operator (LASSO) regression, a method that identifies a subset of predictors and enhances prediction accuracy. The LASSO analysis method eliminated clinical predictors from the model and the final model included only the two plasma biomarkers: IL-8 and sTNFR-1. Low levels of these biomarkers had a high negative predictive value for 28-day mortality and persistent organ dysfunction. There were similar results when the cohorts were restricted to patients meeting criteria for Sepsis-2 and Sepsis-3. 24 This two-biomarker model did not include clinical variables but performed similarly to APACHE III (a multivariable measure of severity of critical illness) and was superior to the day 0 SOFA score in predicting 28-day mortality. The authors also measured plasma concentrations of Ang-1, Ang-2, IL-6, soluble vascular cell adhesion molecule-1, granulocyte-colony stimulating factor, and soluble Fas. The authors tested models that included all of these biomarkers, as well as clinical variables in the model development and testing process, but ultimately found that a simple model including only IL-8 and sTNFR-1 performed best. The study was limited by a very low mortality rate of 9–13% but does establish the value of potentially using levels of two biomarkers for a negative predictive value of 28-day mortality and persistent organ dysfunction.
The strengths of these three recently published studies include large sample sizes of heterogenous populations of critically ill patients. The studies by Hou et al. 19 and Mikacenic et al. 23 used validation cohorts to test the clinical prediction models they developed. The secondary studies of the ProCESS trial data are strengthened by the enrollment of patients in the Emergency Department, early in the course of sepsis, limiting confounding by treatment interventions and strengthening the value of these biomarkers for the purposes of cohort enrichment and triage decisions. 25 The Emergency Department-based studies stand in contrast to the Mikacenic et al. study which measured plasma biomarkers obtained up to 24 h and 48 h after ICU admission in both the internal and external cohorts. Another limitation of the Mikacenic et al. study is the enrollment of patients from nearly 20 years ago (1999), raising some concerns of confounding of clinical outcomes by temporal trends in sepsis treatment, including changes in clinical practice spurred by the landmark study of Early Goal Directed Therapy by Rivers et al. 26 and the Surviving Sepsis Campaign. Another important difference in the Mikacenic et al. study is the application of the model to identify patients with a low risk of mortality. A model that identifies patients at low risk of death could be useful in clinical triage decisions if the biomarkers are measured very early in the course of illness using a point of care assay with immediately available results. Lactate and sFLT-1 seem to be the most promising early biomarkers that predict mortality after sepsis. Whether measurements of IL-8 and sTNFR-1 discriminate well for mortality after sepsis remains to be further validated. To answer this question, these biomarkers could be tested in a study design that enrolls patients with contemporary standard of care treatment for sepsis with plasma samples obtained earlier in the course of illness. However, the association of lower plasma levels of IL-8 and sTNFR-1 with survival reported by Mikacenic et al. and the interaction between treatment effect and baseline IL-6 an IL-10 on mortality reported by Kellum et al. raise the possibility that treatment effects in sepsis could differ among patients with higher and lower inflammatory profiles. Findings from secondary analyses of large RCTs identified a hyperinflammatory subphenotype of ARDS patients, characterized in part by differences in plasma levels of IL-6, IL-8, and sTNFR-1. In these studies, there was a differential response to treatment with protocols of positive end-expiratory pressure (PEEP) and fluid balance strategies.22,27 Future studies could test differential treatment effects among patients with sepsis who present with different molecular phenotypes providing that point-of-care measurements are available for measurement of key biomarkers.
Endothelial injury from sepsis and the development of ARDS
These three recent studies of mortality in patients with sepsis evaluated the prognostic value of biomarkers from several pathophysiologic domains related to the microvascular circulation: inflammation, vascular permeability, coagulation, oxidative stress, and tissue hypoxia. In particular, markers of inflammation (IL-6, IL-8, IL-10, and sTNFR-1), vascular permeability (sFLT-1), and tissue hypoxia (lactate) showed promise in identifying the risk of death and possibly a differential response to fluid resuscitation therapy. In addition to conferring a high risk of death, sepsis is associated with a variety of organ dysfunctions, including acute kidney injury, cardiovascular failure (shock), coagulation abnormalities including thrombocytopenia, altered mental status, and also lung injury and ARDS. We will now turn our attention to the relationship between the vascular endothelium and ARDS after sepsis.
ARDS is a heterogeneous syndrome characterized by impaired oxygenation and bilateral infiltrates on chest radiograph.
28
A variety of clinical risk factors have been associated with the development of ARDS and fall into two broad categories: direct and indirect lung injury (Fig. 2). Common causes of direct lung injury are pneumonia and aspiration of gastric contents. Sepsis is the most common cause of indirect lung injury. Together, pneumonia, aspiration, and sepsis account for 85% of ARDS cases enrolled in recent clinical trials.
28
Because there appear to be different biological profiles between patients with direct and indirect mechanisms of lung injury, these classifications are useful for research purposes.29,30 However, in clinical practice these entities are not always distinct. A patient with lobar pneumonia, a direct lung injury, may subsequently develop sepsis. In this clinical presentation, pulmonary infection first causes local injury of the lung epithelium and lung endothelium, the injury progresses to generalized systemic illness manifesting as sepsis, followed by more diffuse, bilateral lung endothelial injury resulting in respiratory failure and ARDS, and often other organ injury (Fig. 3). The early, exudative phase of ARDS is characterized by damage to the alveolar epithelium and endothelium leading to the accumulation of protein-rich edema fluid within the pulmonary interstitium and alveoli. When evaluating studies of pathogenesis and prognosis in ARDS, we find it useful to refer to a conceptual framework that distinguishes endothelial from epithelial lung injury and direct from indirect causes of lung injury. In this article, we distinguish what is known about the role of the vascular endothelium in ARDS caused by sepsis, a form of indirect lung injury, from other etiologies of ARDS. In clinical research, the distinction between pulmonary and non-pulmonary sepsis can be a useful extension of the direct and indirect lung injury framework discussed above.
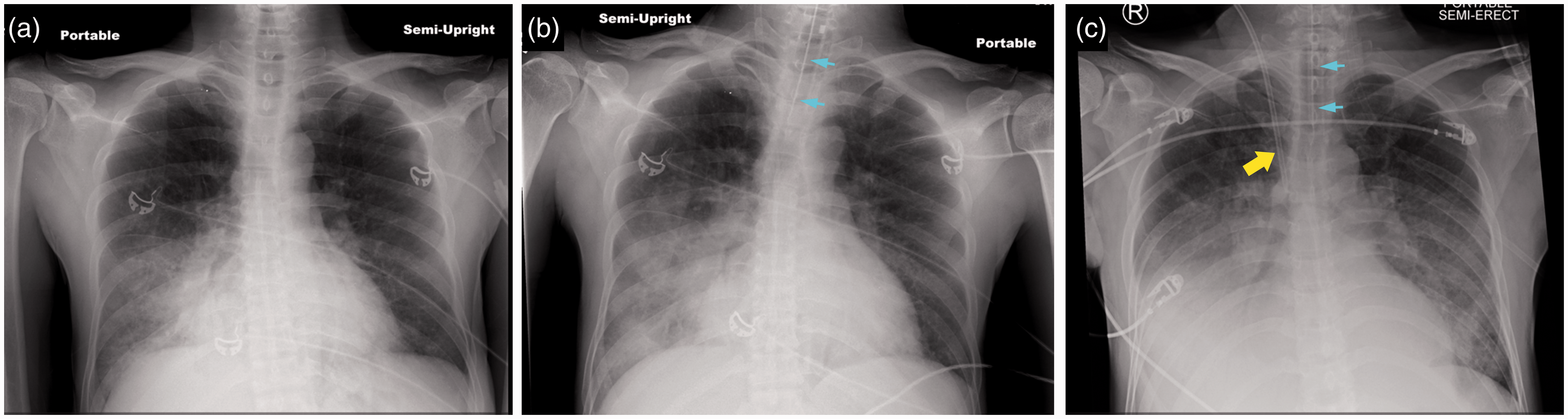
The common and less common causes of ARDS sepsis segregated into direct and indirect causes, including sepsis. Three chest radiographs showing progression of lobar pneumonia to ARDS in a 55-year-old man. (a) The patient presented with lobar pneumonia (blood culture positive for S. pneumoniae) with consolidation of the right lower and middle lobes. (b) Radiograph now shows that the consolidation has progressed to involve more of the air spaces in the right lung and the patient has required endotracheal intubation (see turquoise arrows) because of progressive arterial hypoxemia, tachypnea with a respiratory rate of 40 per minute, and a high work of breathing. (c) Patient’s chest radiograph now shows bilateral pulmonary infiltrates consistent with ARDS. The Pa02/Fi02 is 120 mmHg. A central venous catheter has also been inserted (yellow arrow) through the right internal jugular vein to infuse vasopressor treatment with norepinephrine as the patient has developed shock unresponsive to 3 L intravenous Ringer’s lactate. In addition to ARDS, the patient has acute kidney injury from sepsis with oliguria and a serum creatinine that has risen to 3.1 mg/dL.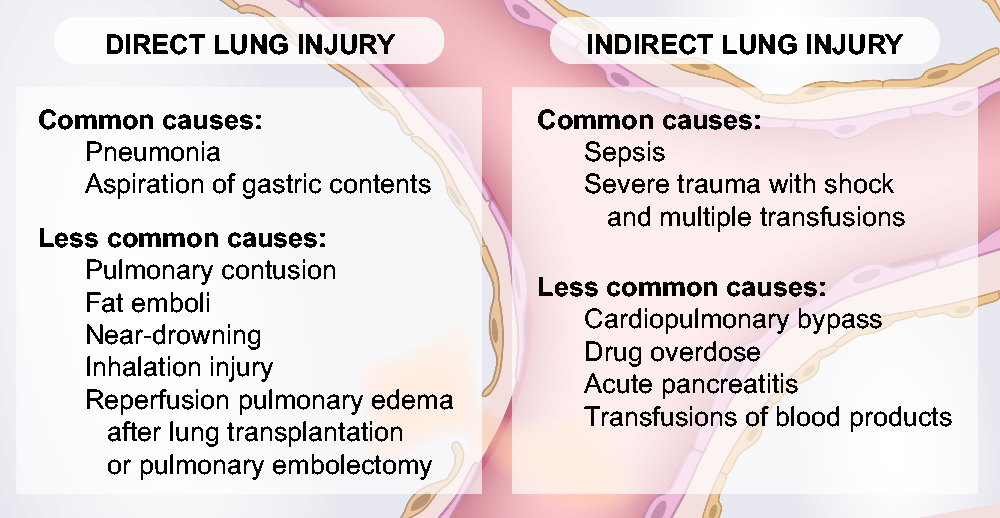
In vitro studies, animal models, and translational research have elucidated important mechanisms involving alterations in the permeability of vascular endothelium and interactions between the endothelium and the innate immune system in the pathogenesis of ARDS after sepsis. Translational studies identified a key role of circulating Ang-2 in pulmonary vascular leak and disruption of the endothelial architecture in sepsis. 31 In animal models, extracellular histones have been implicated in sepsis pathophysiology and organ dysfunction in sepsis. 32 Xu et al. found that mice challenged with a sub-lethal dose of histones showed characteristics of mice with sepsis, including neutrophil accumulation in the alveolar microvessels, vacuolated endothelial cells, and platelet- and fibrin-rich microthrombi in pulmonary circulation. Alterations in vascular permeability in ARDS pathogenesis after sepsis usually require the interaction of neutrophils and platelets with the microvasculature.7,17 Histopathology and in vivo microscopy studies support the key role of the interaction of platelets and neutrophils in mouse models of ALI after LPS administration and cecal ligation and puncture-induced sepsis. These mechanisms include the formation of neutrophil extracellular traps (NETS) and neutrophil platelet aggregation in the pulmonary microcirculation.33,34
Most of the evidence supporting the importance of the innate immune system in sepsis-related ARDS derives from animal models and translational studies using human-based samples in animal and in vitro experiments to assess changes in vascular permeability.35–39 These mechanisms of lung injury are challenging to study in humans because they require more complex measurements to detect cell–cell interactions such as flow cytometry and lung intravital microscopy.40,41 Recent gene-expression studies in human participants suggest that several neutrophil-related pathways may be involved in the early pathogenesis of sepsis-related ARDS. 42 In a case control study, gene expression study of blood samples obtained within 24 h of ICU admission comparing 29 patients with sepsis and ARDS to 28 patients with sepsis alone, there was early differential gene expression of mediators related to the initial neutrophil response to infection: olfactomedin 4, lipocalin 2, CD24, and bactericidal/permeability increasing protein. 42 These gene expression differences were robust to adjustment for several potential confounders, including mechanisms for direct lung injury, pneumonia, and aspiration.
When summarizing the literature describing the pathogenesis of ARDS after sepsis in humans, it is important to bear in mind that many studies do not distinguish subpopulations of patients with ARDS after sepsis from ARDS from other causes of lung injury. Additional heterogeneity arises from study designs that measure biomarkers at different time points in the course of illness. Furthermore, the standard of care treatment for both ARDS and sepsis has changed over time and may alter the pattern of biomarker expression and the risk of developing ARDS after sepsis.
Circulating vWF is predominantly released by vascular endothelial cells and to a lesser extent by megakaryocytes and platelets. vWF can regulate vascular permeability and has been measured in several studies of patients at risk for ARDS, some of whom have sepsis. Results from a prospective cohort study of vWF in non-pulmonary sepsis were published in 1990 by Rubin et al. 43 Plasma vWF was measured in 45 patients with non-pulmonary sepsis without evidence of lung injury. In this cohort, 15 individuals (33%) subsequently developed lung injury. Among those who developed lung injury, plasma vWF was significantly higher than in patients who progressed to develop ARDS. Notably, there was a significantly higher mortality rate in the group that developed lung injury (93% vs. 30%). The authors concluded that in patients with non-pulmonary sepsis at risk for lung injury, elevated plasma vWf is a useful, early biomarker of endothelial injury and it has both predictive and prognostic value. In a later study, published in 1995, Moss et al. measured vWF at 6-h intervals over 48 h in a prospective cohort study of 96 individuals at risk for ARDS and 30 of these participants had sepsis. 44 Plasma for these measurements was obtained within 6 h of developing an ARDS risk factor. Of the 30 patients with sepsis, ten developed ARDS. The study did not consider non-pulmonary sepsis separately from pulmonary sepsis. Among individuals with sepsis, the authors found no difference in vWF levels between those who developed ARDS and those who did not. Reconciling these findings with those reported by Rubin et al. requires consideration of several key differences in study design. The later study included both pulmonary and non-pulmonary sepsis. This is perhaps the most important difference in study design as there has been more recent work showing the pathogenesis and prognosis of ARDS differs between direct and indirect mechanisms of lung injury.12,29 The earlier study excluded patients with any evidence of lung injury at enrollment while the later study only excluded patients who met full diagnostic criteria for ARDS at enrollment. There were also differences between the two studies in the ascertainment of the outcome, ARDS.
In a more recent study published in 2013, Agrawal et al. studied 167 patients at risk for ARDS, including 46 (28%) with sepsis. 45 The authors measured vWF along with several other biomarkers of endothelial permeability and inflammation: Ang2, Ang2: Ang1, IL-8, and receptor for advanced glycation end products (sRAGE). Similar to the finding in the Moss et al. study, in this study, baseline vWF was not different between those who progressed to develop ARDS and those who did not. Similarly, sRAGE did not differ between those who developed ARDS and those who did not. Baseline Ang2, Ang2: Ang1, and IL-8 were higher among those who later developed ARDS (n = 19 [11%]) compared to those who did not. In univariate logistic regression analyses, higher Ang-2 and IL-8 levels were associated with higher risk of ARDS. This association between Ang-2 and ARDS did not differ between those with sepsis and those without sepsis. In other words, the association between baseline Ang-2 levels in this cohort and ARDS was independent of sepsis. In contrast, the association between IL-8 and ARDS was attenuated by adjustment for sepsis, suggesting that in this study, sepsis was a confounder and both contributed to the increased levels of IL-8 as well as the risk of ARDS. When evaluating these findings in the context of what is known about the role of endothelial injury in ARDS after sepsis, there are several important considerations. This study enrolled patients with a variety of risk factors for ARDS. Furthermore, the investigators did not distinguish between patients with pulmonary and non-pulmonary sepsis. The severity of illness of patients enrolled in this study was substantially lower than in the Rubin et al. study. In the Agrawal et al. study there was a 25% mortality rate and 11% incidence of ARDS, compared to 51% mortality rate and 33% incidence of lung injury in the Rubin et al. study. The three aforementioned studies indicate that markers of endothelial injury and inflammation—including vWF, Ang-2, and IL-8—perform differently in the varied cohorts of patients at risk for ARDS. Thus, it seems critical to interpret the associations between the biomarkers and the development of ARDS in the context of the specific risk factor for lung injury.
The biology and prognosis of ARDS differs between direct and indirect mechanisms of lung injury 12 and the disparate findings of the association of vWF and ARDS in the studies discussed above can be attributed to different study bases: (1) patients with non-pulmonary sepsis; (2) patients with a sepsis from both pulmonary and non-pulmonary sources; and (3) patients with a variety of risk factors for ARDS, with 28% of participants having sepsis. In a case control study of 100 patients with severe sepsis comparing individuals with ARDS to those without ARDS, Ware et al. evaluated a panel of 11 biomarkers reflecting different aspects of the pathophysiology of ARDS. 30 The authors described a multivariate model incorporating a panel of five biomarkers—SP-D, RAGE, CC-16, IL-8, and IL-6—with an area under the ROC curve of 0.75 (95% confidence interval [CI] = 0.7–0.84) for diagnosis of ARDS. Of note, in this study, Ang-2 did not differ significantly between those with ARDS and those without ARDS. The authors found that among study participants with severe sepsis, biomarkers of lung epithelial injury and inflammation were the most useful for discriminating patients with ARDS from those without ARDS. This finding is somewhat surprising because sepsis is generally considered a risk factor for indirect lung injury that would be expected to act through biological pathways involving the endothelium. A limitation of this study is that there was no distinction between pulmonary and non-pulmonary sources of severe sepsis. The authors did not report the incidence of pneumonia in the cases and controls, nor does the article indicate if the models were adjusted for the source of infection. It is possible that the association between ARDS and the biomarker profile of epithelial injury reflects a difference in the pathophysiology between pulmonary and non-pulmonary sepsis and ARDS.
A study published by Calfee et al. in 2015 builds on this distinction between direct and indirect lung injury. The authors measured biomarkers of endothelial injury (Ang-2, vWF), alveolar epithelial injury (SPD, sRAGE), and inflammation (IL-6, IL-8) in two populations: one prospective single-center cohort study and one large multicenter RCT. 29 All study participants with indirect lung injury had non-pulmonary sepsis. The authors tested whether each biomarker differed between individuals with direct vs. indirect lung injury. They found that indirect lung injury, caused by non-pulmonary sepsis, was characterized by a molecular phenotype consistent with more severe endothelial injury and less severe alveolar epithelial injury. The opposite pattern was identified in patients with direct lung injury. In keeping with the finding from Rubin et al., 43 in the multicenter study cohort, vWF was higher among participants with non-pulmonary sepsis compared to those with direct lung injury. These associations were robust to adjustments for severity of illness. Compared to individuals with ARDS from pneumonia or aspiration, those with ARDS from non-pulmonary sepsis had higher levels of Ang-2 on study enrollment. While IL-6 and IL-8 were not different between participants with indirect vs. direct lung injury in the single center study of 100 patients, in the multicenter study that included 853 patients IL-6 and IL-8 were higher among those with indirect lung injury. Taken together with the findings from the earlier studies of vWF, Ang-2, and IL-8, the results suggest that endothelial permeability and inflammation play a key role in the pathophysiology of ARDS after non-pulmonary sepsis, a specific etiology of indirect lung injury. However, in more heterogeneous populations of patients at risk for ARDS the associations between these biomarkers and the subsequent development of ARDS are less consistent.
Prognosis of patients with ARDS after sepsis
A study published in 2004 evaluated the prognostic value of vWF in patients with ARDS. 46 vWF was measured in 559 patients with ARDS enrolled in the National Heart, Lung, and Blood Institute ARDS Network RCT of low tidal volume ventilation, the ARMA trial.46,47 All individuals enrolled in this study had established ARDS and 141 participants (25%) had sepsis. Pulmonary sepsis was not distinguished from non-pulmonary sepsis. In this cohort of patients with ARDS, baseline vWF levels were similar in patients with and without sepsis and were significantly higher in non-survivors compared to survivors. vWF levels did not differ by treatment arm. The authors concluded that the degree of endothelial activation and injury was strongly associated with outcomes in ARDS, regardless of the presence or absence of sepsis, and was not modulated by a protective ventilatory strategy.
A similar study was conducted in a cohort of patients enrolled in different ARDS Network RCT testing a two fluid management treatment protocols and the use of pulmonary artery catheters in patients with ARDS. 21 Calfee et al. measured day 0 and day 3 plasma vWF and Ang-2 in patients enrolled in the FACTT trial and tested the association of these biomarkers with mortality. 48 There were 24% of the 917 individuals in this biomarker substudy of FACTT had sepsis. The authors distinguished patients with infection-related lung injury from those with non-infection causes. However, they did not distinguish between pneumonia and sepsis as the cause of ARDS in the infection-related lung injury group. Similar to the findings from the biomarker studies in ARMA trial discussed above, the authors found that vWF was significantly associated with mortality in both participants with and without infection-related lung injury and that vWF levels were not affected by fluid therapy. In other words, in patients with ARDS, vWF predicted mortality, but this association appeared to act independently of infection or sepsis. The authors also measured Ang-2 in this cohort of patients enrolled in the FACTT study. Unlike vWF, the association between Ang-2 and mortality differed between individuals with infection and those without infection. Among participants without infection, baseline Ang-2 levels were associated with higher morality (odds ratio [OR] = 2.43 per 1-log increase in Ang-2, P < 0.001). Among individuals with infection (pneumonia or sepsis), baseline Ang-2 was not different between survivors and those who died. Among those with infection, patients whose plasma Ang-2 levels increased from day 0 to day 3, there was more than double the odds of death compared with patients whose Ang-2 levels declined over the same period of time. This difference was statistically significant. Taken together, these findings show that among patients with ARDS, Ang-2 has differential prognostic value for mortality depending on the presence or absence of infection. The authors also found that Ang-2 was highest among patients with sepsis. Among participants with sepsis, a fluid conservative strategy was associated with a 15% greater decline in Ang-2 levels from day 0 to day 3 compared with fluid-liberal therapy in patients with infection-related ALI. This difference was statistically significant. These findings suggest that fluid conservative therapy preferentially lowers plasma Ang-2 levels over time and thus may be beneficial in part by decreasing endothelial inflammation and are supported by earlier experimental studies showing a pro-inflammatory response of the endothelium to high vascular pressures. 49
In a study of 259 children with ARDS, Zinter et al. measured vWF, Ang-2, and VEGF on study day 1 and day 3 of study enrollment and tested the association of these biomarkers with mortality. 50 There was a 15% mortality rate in this cohort. Sepsis was the ARDS risk factor in 22% of patients and sepsis was the most common of indirect lung injury risk factor (n = 56 individuals with sepsis, 57% of 97 participants with indirect lung injury). Analyses were stratified by prior hematopoietic cellular transplantation (HCT), given the severe ARDS phenotype of this subgroup. The authors did not report findings for models testing the association of the Ang-2, VEGF, or vWF and mortality adjusted for direct or indirect mechanisms of lung injury, or for patients with sepsis after ARDS. Compared to patients with direct lung injury, patients with indirect lung injury had higher plasma Ang-2 on day 1 but not on day 3. In logistic regression models adjusted for age, sex, race, and PaO2:FiO2 ratio, day 1 and day 3 Ang-2 levels were associated with mortality (OR = 3.7, 95% CI = 1.1–11.5, P = 0.027 and OR = 10.2, 95% CI = 2.2–46.5, P = 0.003, for each log10 increase in Ang-2 on day1 and day 3, respectively). These associations were independent of vWF and VEGF levels. Nearly half of the cohort (45%) had a rising Ang-2 levels between days 1 and 3; this was strongly associated with mortality, particularly among children with HCT. Children with indirect lung injury had similar vWF levels compared with direct lung injury patients. In the aforementioned studies, the association of vWF with mortality was compared between adult participants with and without infection. In this study, the authors distinguished indirect and direct causes of lung injury. Importantly, sepsis was the most common cause on indirect lung injury in this cohort and pneumonia was the most common cause of direct lung injury. It is therefore difficult to compare some of the reported findings of Ang-2 and vWF as prognostic biomarkers in sepsis after ARDS, the focus of this review. In contrast to the studies discussed earlier, although children who died had higher vWF on day 1 compared to survivors, the association between vWF and mortality in univariate logistic regression models was not significant. The authors attribute this to three outliers of high vWF measurements among children who survived. VEGF was not measured in the previously discussed ARDS Network prognostic biomarker studies. In this cohort of pediatric patients with ARDS, patients with indirect lung had similar VEGF levels compared to those with direct lung injury. Plasma VEGF was not associated with mortality in pediatric ARDS.
Thombomodulin (TM) is an activator of protein C and a biomarker for endothelial injury. A different substudy of 449 individuals enrolled in the FACTT trial tested the association between soluble thrombomodulin (sTM) and mortality among patients with ARDS. 51 In this cohort, 22% of patients had sepsis. The authors also tested the association between TM gene polymorphisms and levels of sTM at baseline to assess whether genetic heterogeneity contributed to differential TM gene expression in patients with ARDS. Plasma sTM levels were higher among patients with non-pulmonary sepsis compared to those without. Plasma sTM was higher in non-survivors than survivors at baseline and on day 3. In analyses adjusted for non-pulmonary sepsis, among other variables, each log increase in sTM at baseline and at day 3 more than doubled the odds of death, OR = 2.4 (95% CI = 1.5–3.8, P < 0.001) and OR = 2.8 (95% CI = 1.7–4.7, P < 0.001), respectively. The addition of sTM to the APACHEIII scale significantly improved discrimination for mortality from 77% to 80% (P < 0.03). The authors found no differences in sTM levels by single nucleotide polymorphism (SNP) genotype. They concluded that the lack of association between the sTM levels and genetic variants indicated that the increased levels of sTM among those who died reflected the severity of endothelial damage rather than genetic heterogeneity. In patients with ARDS, sTM was associated with death. Although sTM levels were highest among participants with non-pulmonary sepsis, the association between sTM and death was independent of non-pulmonary sepsis.
Conclusions
Summary of endothelial and inflammatory biomarker studies in ARDS after sepsis.
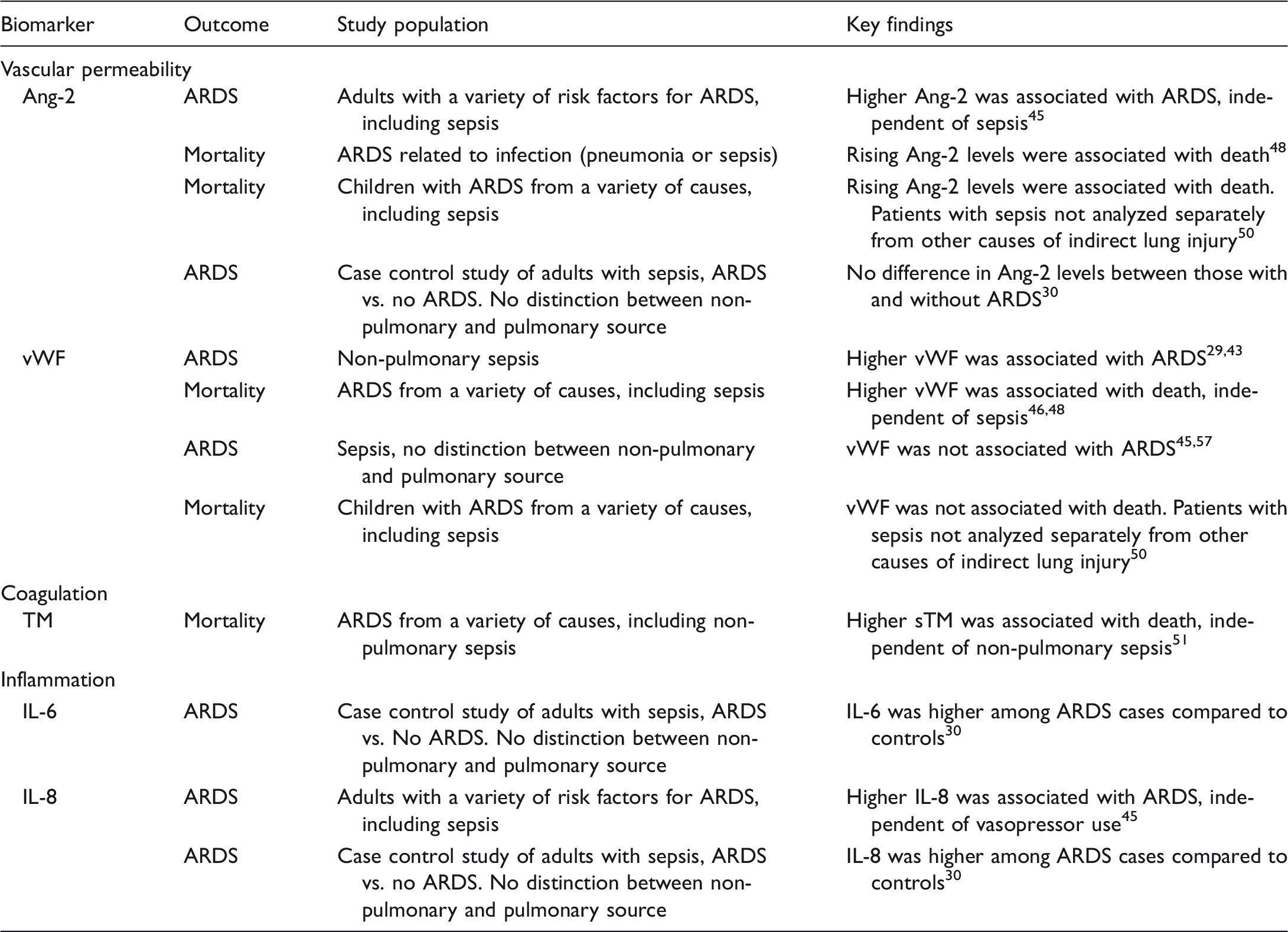
Unless otherwise specified, all clinical studies listed above are cohort studies of adult patients.
Ang-2, Angiopoietin-2; vWF, von Willebrand Factor; TM, thrombomodulin; IL-6, Interleukin-6; IL-8, Interleukin-8; ARDS, acute respiratory distress syndrome.
How can these data inform future study design? The heterogeneity of results in the biomarker studies above seems to be in part driven by heterogeneous patient populations. Taken together, these findings suggest that future biomarker studies should differentiate patients with sepsis as the primary risk factor for ARDS from other causes of lung injury. Further differentiation between pulmonary and non-pulmonary sepsis may allow researchers to better understand specific biologic pathways involved in ARDS after sepsis. This could be accomplished through a study design with a well-defined patient population, or using adjusted or stratified data analyses of more heterogeneous cohorts. These distinctions may provide valuable insights into the biological differences among subgroups of patients. It follows that biological differences identified by distinct molecular patterns could explain heterogeneity of treatment effects that are not explained by clinical factors alone. 52
Footnotes
Acknowledgements
The authors thank Diana Lim for help with designing and formatting the figures in this manuscript.
Conflict of interest
The author(s) declare that there is no conflict of interest.
Funding
CMH was supported by National Heart, Lung, and Blood Institute (NHLBI) Career Development Grant, NHLBI K23HL-133495. MAM was supported by HL51856, HL110969, and HL10871301.
