Abstract
Mitochondrial dysfunction within the pulmonary vessels has been shown to contribute to the pathology of idiopathic pulmonary arterial hypertension (IPAH). We investigated the hypothesis of whether impaired exercise capacity observed in IPAH patients is in part due to primary mitochondrial oxidative phosphorylation (OXPHOS) dysfunction in skeletal muscle. This could lead to potentially new avenues of treatment beyond targeting the pulmonary vessels. Nine clinically stable participants with IPAH underwent cardiopulmonary exercise testing, in vivo and in vitro assessment of mitochondrial function by 31P-magnetic resonance spectroscopy (31P-MRS) and laboratory muscle biopsy analysis. 31P-MRS showed abnormal skeletal muscle bioenergetics with prolonged recovery times of phosphocreatine and abnormal muscle pH handling. Histochemistry and quadruple immunofluorescence performed on muscle biopsies showed normal function and subunit protein abundance of the complexes within the OXPHOS system. Our findings suggest that there is no primary mitochondrial OXPHOS dysfunction but raises the possibility of impaired oxygen delivery to the mitochondria affecting skeletal muscle bioenergetics during exercise.
Introduction
Idiopathic pulmonary arterial hypertension (IPAH) remains a progressive disease leading to premature death despite the availability of effective targeted therapies. 1 Patients report not only breathlessness, but fatigue as one of the predominant symptoms. 2 Beyond the obstruction observed in the pulmonary vessels, a number of other organs are involved in IPAH. These include the presence of insulin resistance, skeletal muscle dysfunction, bone-marrow derived mononuclear cells, and iron deficiency. 3 In terms of skeletal muscle changes, a shift in muscle fiber types—from type I to type II—with a concomitant change in the metabolic profile from oxidative to glycolytic, imbalance in the muscle protein breakdown, and synthesis pathways have been recorded in these patients. 4 Impaired mitochondrial function has been shown to contribute to the pathology of the disease within the pulmonary vessels but whether there is mitochondrial dysfunction in the skeletal muscle is unclear. 5 In particular, the question arises as to whether impairment of the oxidative phosphorylation (OXPHOS) process, the final pathway to energy generation within the mitochondria, is contributing to exercise intolerance in IPAH. Therefore, we tested the hypothesis that in IPAH, there is skeletal muscle mitochondrial OXPHOS dysfunction affecting exercise capacity. We undertook a pilot study using both in vitro and in vivo methods.
Methods
Nine participants were recruited from the National Pulmonary Hypertension Service (Newcastle) and were deemed clinically stable on targeted IPAH-specific therapy for at least three months. All nine participants underwent symptom-limited cardiopulmonary exercise testing with six patients having simultaneous non-invasive hemodynamic measurements, vastus lateralis muscle biopsy, 6-min walk distance (6MWD), and completion of two questionnaires: EmPHasis-10 and Fatigue Severity Scale (FSS). Six participants underwent 31P magnetic resonance spectroscopy (31P-MRS) scans. Three were unable to undergo 31P-MRS due to prostacyclin pumps proving to be a contraindication. Muscle biopsies underwent mitochondrial OXPHOS assessment by histochemistry and quadruple immunofluorescence, as previously reported.6,7 31P-MRS scan was performed using 3 T Achieva Scanner (Philips, NL) with a 14-cm diameter phosphorous surface coil for transmission /reception for signal and the in-built body coil for anatomical imaging, as previously reported, to obtain PCr and ADP half-times. 8 Approval for the study was obtained from the regional ethics committee.
Results
Baseline and exercise characteristics of individual participants are summarized in the table in Fig. 1. Five IPAH patients reported to be suffering fatigue scores > 4, with three patients reporting severe symptoms (FSS > 5).
Table: Baseline clinical characteristics of the nine IPAH patients including age, gender, treatment, quality of life scores, peak oxygen consumption (VO2), peak cardiac index (CI), maximum peripheral oxygen extraction (arterial-venous O2 difference), and the oxygen consumption – work rate relationship (ΔVO2/ΔWR). (a–d) The mitochondrial respiratory chain profile (levels of complex I, complex IV, and porin) in selected patients: (a) Healthy control (male, 49 years, n = 238). (b)IPAH (Patient 4, n = 317). (c) IPAH (Patient 1, n = 166). (d) Patient with genetically defined mitochondrial DNA disease (positive control; male, 60 years, n = 188). n is the number of fibers analyzed in each muscle section. Each dot represents the measurement from an individual muscle fiber, with color according to the mitochondrial mass (very low: blue, low: light blue, normal: light orange, high: orange, and very high: red). The thin black lines indicate the SD limits for classification of the fibers. Bold dashed lines indicate the mean abundance level of complex I (NDUFB8) and complex IV (COX-I) in normal fibers.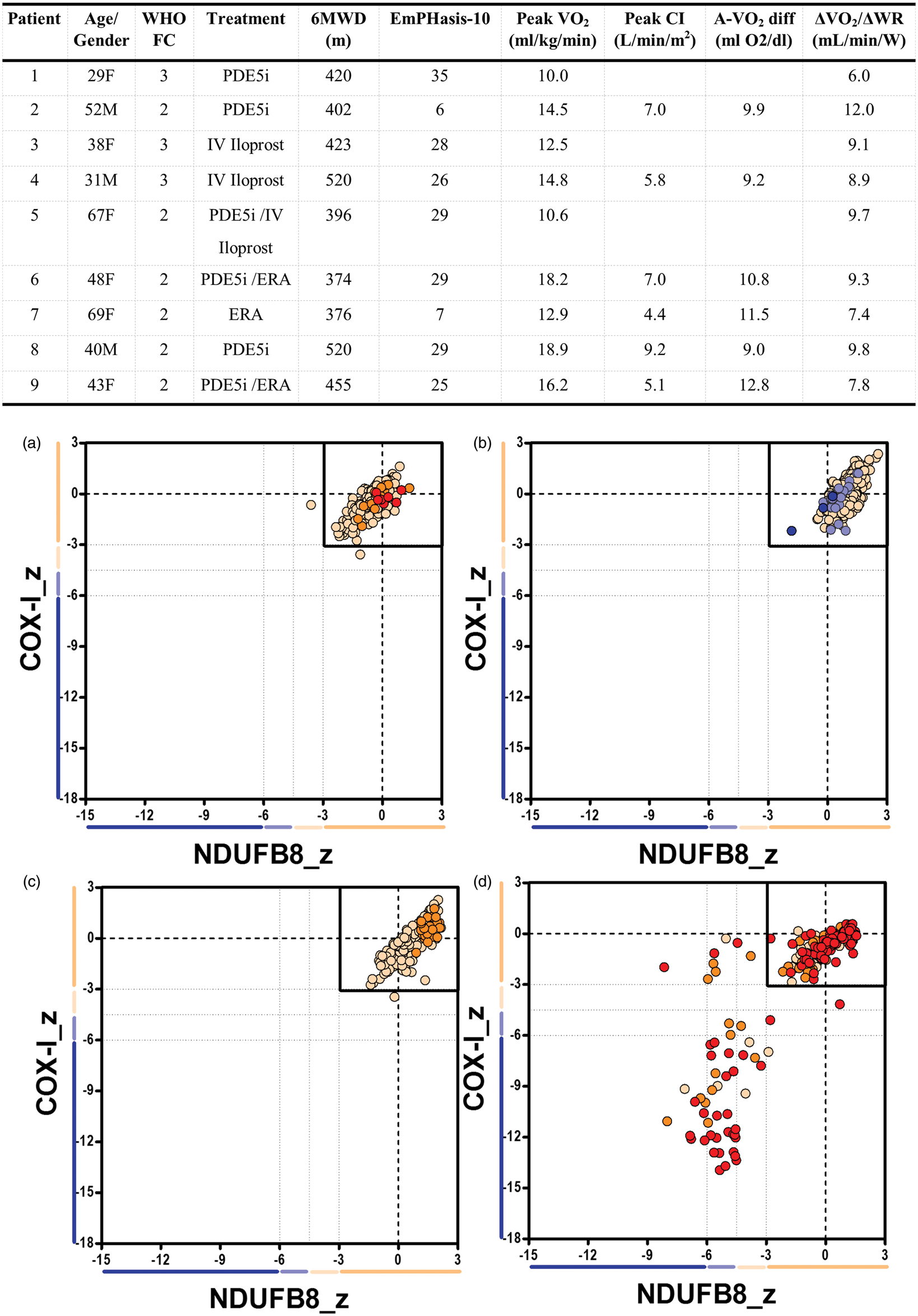
Representative examples of the evolution in phosphocreatine (PCr) concentration and intramuscular pH changes during exercises as assessed by 31P-MRS are shown in Fig. 2a and b. The results of the IPAH patients in comparison to referenced historical control values
8
are shown in Fig. 2c. The six participants who underwent 31P-MRS scans, exhibited higher phosphocreatine recovery time kinetics (PCr t1/2) (40.0 ± 8.8 versus 27.2 ± 7.1 s, P = 0.013) and achieved lower minimum pH values (6.85 ± 0.10 versus 7.00 ± 0.02, P = 0.001), but had normal ADP recovery kinetics (25.5 ± 7.1 versus 20.9 ± 5.1 s, P = 0.228), rest pH (7.03 ± 0.02 versus 7.03 ± 0.04, P = 0.573), and end pH (7.02 ± 0.04 versus 7.02 ± 0.02, P = 0.573). IPAH patients demonstrated evidence of an increase in pH recovery times compared to controls (197 s, range = 130–240 s versus 58 s, range = 0–160 s).
(a, b) Tracing of the intramuscular PCr concentration decay (a) and change in pH (b) during rest, exercise, and recovery are shown. Start of exercise was at 80 s and recovery commenced at 260 s. (c) Table demonstrating the comparisons between healthy control data
8
and IPAH patients. Values are mean ± SD. Non-parametric independent data analyzed by Mann–Whitney U test. P value < 0.05 was considered significant.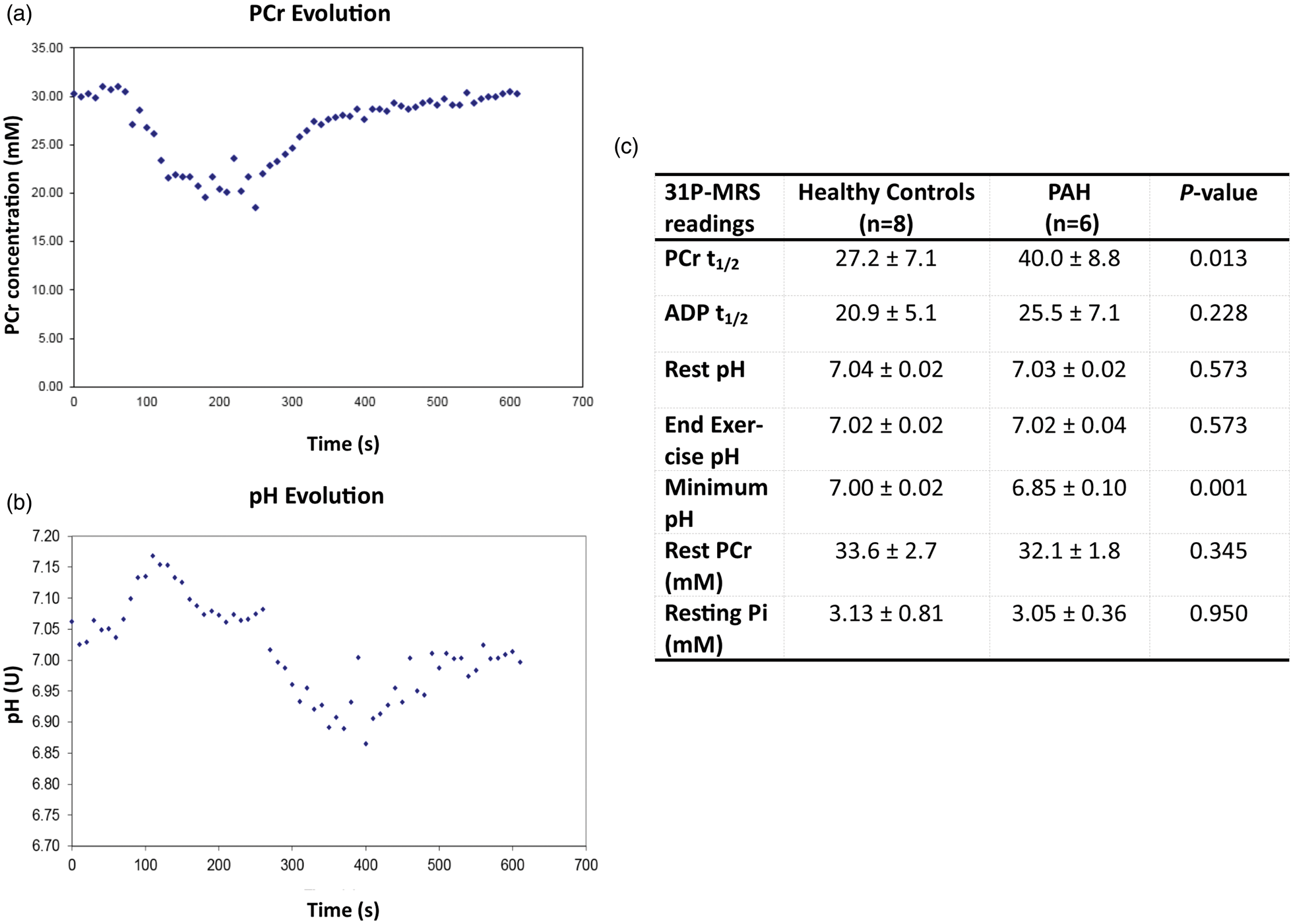
The COX/SDH histochemical assay, which allows detection of enzymatic activity of succinate dehydrogenase (SDH) and cytochrome c oxidase (COX), did not reveal any respiratory-deficient myofibres in patients. This was also supported by modified Gomori trichrome staining that demonstrated absence of any ragged-red fibres, otherwise commonly found in primary mitochondrial myopathies. In order to corroborate our findings, quadruple immunofluorescence to assess abundance of selected protein subunits of complex I and IV of the mitochondrial respiratory chain was subsequently undertaken. We compared the results to skeletal muscle biopsy samples of two healthy normal controls and a patient with genetically-defined mitochondrial DNA disease, as positive control. Representative results are shown in the panels in Figure 1a–d. These demonstrated normal levels (within 3 standard deviations [SD]) of complex I and IV in all nine muscle samples obtained from IPAH patients comparative to normal healthy controls.
Discussion
This pilot study assessed skeletal muscle mitochondrial function using in vivo and in vitro methods in idiopathic pulmonary arterial hypertension. First, we have shown evidence of abnormal skeletal muscle bioenergetics by 31P-MRS during and after exercise that could either be explained by mitochondrial OXHOS dysfunction or impaired oxygen delivery to the mitochondria. We went on to show in the same patients, there were normal levels of mitochondrial respiratory chain protein abundance as well as preserved enzymatic activity in skeletal muscle, irrespective of disease burden. Therefore, these findings suggest oxygen delivery rather than utilization to the skeletal muscle is affecting muscle function and impairing exercise capacity.
COX/SDH histochemistry is the gold standard method to interrogate COX and SDH activities in individual muscle fibers. The qualitative analysis of sequentially labelled muscle sections obtained from IPAH patients revealed that both complex II and IV activities were normal. This was confirmed by quadruple immunofluorescence, a new state-of-the-art methodology that is a very sensitive and accurately quantifies abundance of complex I and IV subunits of the OXPHOS system in each individual muscle myofiber, with correction for mitochondrial mass. 7 We observed normal levels of complex I and IV in all nine IPAH patients. We studied IPAH patients who were clinically stable and free from significant co-morbidities which could be considered a drawback. Nevertheless, we should note that three of the patients were on intravenous therapy (Iloprost®), including one patient who underwent lung transplantation within one year of the muscle biopsy. Therefore, our study supports the assertion there is no skeletal muscle mitochondrial OXPHOS dysfunction in IPAH.
The abnormal skeletal muscle bioenergetics observed in 31P-MRS are likely due to impaired oxygen delivery to the muscle mitochondria. The reduced oxygen delivery could be due to central and peripheral factors as shown in previous studies including reduced cardiac output, decreased muscle capillarization, diminished angiogenesis, and abnormal peripheral microcirculation. 9 Indirect evidence in IPAH exists of impaired oxygen delivery to utilization mismatch at the onset of exercise affecting oxygen uptake kinetics (VO2). 10 As a result, energy (ATP) is generated in the muscle through oxygen-independent pathways leading to accumulation of by-products that may cause muscle fatigue. Currently we are unclear about the dominant mechanism impairing both oxygen delivery and extraction during exercise in IPAH. Exercise training has been shown to be beneficial in improving cardiac output, muscle capillarization, exercise endurance capacity, and muscle strength in IPAH.11,12 Our findings support the potential benefits of structured exercise training programs to improving central and peripheral factors in oxygen delivery to the muscle mitochondria. Furthermore, there are no licensed pharmacological therapies available in improving peripheral factors affecting oxygen transport pathway and, currently, support the role of exercise in IPAH. However, there is evidence that dietary nitrate has an impact on skeletal muscle vascular and metabolic control during exercise with efficacy in the pre-clinical and clinical chronic heart failure. 13 Therefore, further research is much needed to determine if there is a role for pharmacology to improve peripheral skeletal muscle function during exercise in IPAH.
In conclusion, impaired exercise capacity and skeletal muscle bioenergetics is not explained by mitochondrial OXPHOS dysfunction in IPAH, suggesting oxygen delivery rather than utilization as the main factor contributing to exercise intolerance. Improving exercise capacity in IPAH requires addressing the primary impediments including cardiac output, muscle capillarization, and peripheral microcirculation for adequate oxygen delivery to the skeletal muscle. Further research into both pharmacology and exercise prescriptions to improve peripheral factors that affect the oxygen transport pathway in IPAH is much needed.
Footnotes
Conflict of interest
The author(s) declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
