Abstract
Treatment of pediatric pulmonary hypertension (PH) with IV prostanoids has greatly improved outcomes but requires a central line, posing inherent infection risk. This study examines the types of infections, infection rates, and importantly the effect of line management strategies on reinfection in children receiving IV prostanoids for PH. This study is a retrospective review of all pediatric PH patients receiving intravenous epoprostenol (EPO) or treprostinil (TRE) at one academic tertiary care center between 2000 and 2014. No patients declined participation in the study or were otherwise excluded. Infectious complications were characterized by organism(s), infection rates, time to next infection, and line management decisions (salvage vs. replace). Of the 40 patients followed, 13 sustained 38 infections involving 49 pathogens, with a predominance of gram-positive (GP) organisms (n = 35). The pooled infection rate was 1.06 per 1000 prostanoid days with no difference between EPO and TRE. No significant difference in reinfection rate was observed when comparing line salvage to replacement, regardless of organism type. Both overall and organism-type comparisons suggest longer time between line infections following line salvage compared with line replacement (732 vs. 410 days overall; 793 vs. 363 days for GP; 611 vs. 581 days for gram-negative [GN]; P > 0.05 for all comparisons). Central line replacement following blood stream infections in pediatric PH patients does not improve subsequent infection rates or time to next infection, and may lead to unnecessary risks associated with line replacement, including potential loss of vascular access. A revised approach to central line infections in pediatric PH is proposed.
Pulmonary hypertension (PH) is an incurable disease defined by abnormal elevation of the pulmonary artery pressure (PAP) and pulmonary vascular resistance (PVR). If untreated, it ultimately progresses to right heart failure and death with a median survival of 4–12 years.1,2 Over the past decade, several classes of therapeutics have become available, with intravenous prostanoids epoprostenol (EPO) and treprostinil (TRE) as the suggested therapy for patients with severe PH. 3 Treatment has improved survival; the 2012 Registry to Evaluate Early and Long Term PAH Disease Management reported survival in treated patients of 96%, 84%, and 74%, at one, three, and five years, respectively.4,5 In pediatric patients receiving prostanoids, five-year transplant-free survival is now 70%3 compared to 25% a decade ago.6,7 While equally efficacious, TRE has significant safety and convenience benefits compared to EPO; as a result, providers have shifted towards more frequent use of TRE in the pediatric population.
Continuous intravenous prostanoid therapy is delivered through a tunneled central line. Parents learn sterile techniques and are responsible for medication preparation, line care, and drug infusion. The central line is entered every 1–2 days when the new medication is prepared. Central line associated blood stream infection (CLABSI) rates are in the range of 0.1–1.1 per 1000 treatment days in PH patients.8–15 With the initial use of TRE, centers documented a greater risk of infection with TRE compared with EPO, particularly with gram-negative (GN) organisms.9,14–16 Subsequent changes to the diluent used in mixing the medication, the use of a closed hub system, and maintenance of a dry catheter hub system have significantly decreased this disparity. 17
Unlike central lines typically required for short-term or intermittent use, those for PH patients are life-saving and many rely on these drugs for years to maintain their functional status.5,9 Therefore, the decision to replace a central line carries different implications in PH patients. Strategies shown to be effective in reducing infection rates in other populations are not viable options here, as prostanoid infusions should not be interrupted for any significant period of time. 18 These constraints and the potential lifelong necessity of this intravenous therapy for survival mandate the prevention of unnecessary line replacements for patients with PH. The Infectious Disease Society of America (IDSA) guidelines on central catheter infections 19 does not specifically provide appropriate guidance for the management of line infections in this patient population and evidence-based guidelines are lacking for pediatric PH central line infections. Recent reports have appropriately raised concerns regarding unnecessary line removal in the general population.20,21 In this study, we examine central line infection rates in a large pediatric PH population receiving prostanoid therapy and the impact of line replacement versus salvage on infection rates.
Methods
Study population
A retrospective review was conducted of pediatric PH patients (age < 18 years at the time of first central line placement) cared for at Lucile Salter Packard Children’s Hospital (LPCH) at Stanford between 2000 and 2014. Patients were included if they were seen at LPCH at least twice while receiving prostanoids. If a patient’s central line was placed and/or an infection was treated at an outside hospital, those records were obtained. Care provided by outside institutions was driven by those providing the care. In many, but not all cases, the LPCH PH team (primary team managing prostanoid therapy) was included in the discussions.
Research Electronic Data Capture (REDCap) was used to collect basic demographics, central line characteristics and infection organism, New York Heart Association (NYHA) functional class (used to determine disease severity), and prostanoid type at time of infection. Stanford University’s Institutional Review Board approved the study and consent was obtained for each participant.
Central line infection rates
Treatment days were counted from the day of line placement until the patient exited the study, as defined by either drug or IV discontinuation, transplant, death, or transition out of the pediatric PH clinic. Line infections were defined by a positive blood culture with any organism, including common commensals. A catheter tip culture was not required to confirm infection. Two positive cultures > 14 days apart were considered separate infections; suspected infections (elevated white blood cell count and/or fever with negative blood cultures) and site infections were excluded. 22 Replacement was defined as complete removal of the existing line and initiation of a new site with a new line. After each infection, the number of days until the next event was determined. If the line management decision (salvage versus replacement) was followed by a second infection, the rate was calculated as 1 (infection) divided by the number of days until the next infection. If the line management decision was not followed by another infection, then the rate was set as 0. The rates were then stratified by the line management decision. Further, to determine if line salvage or replacement was associated with a higher reinfection rate, the number of days to next infection following a line management decision was determined.
Statistics
Fisher’s exact test was used for categorical variables and the two-tailed t test for continuous variables. Demographics were compared between individuals who were infection-free and those who experienced ≥ 1 infection. Comparisons were made between the mean infection rates following the decision to replace or salvage a central line using a two-tailed unpaired t test. We used Fisher’s exact test to compare the number of infections between EPO and TRE, and between gram-positive (GP) and GN infections.
Results
General characteristics
Characteristics of the pediatric pulmonary hypertension cohorts.
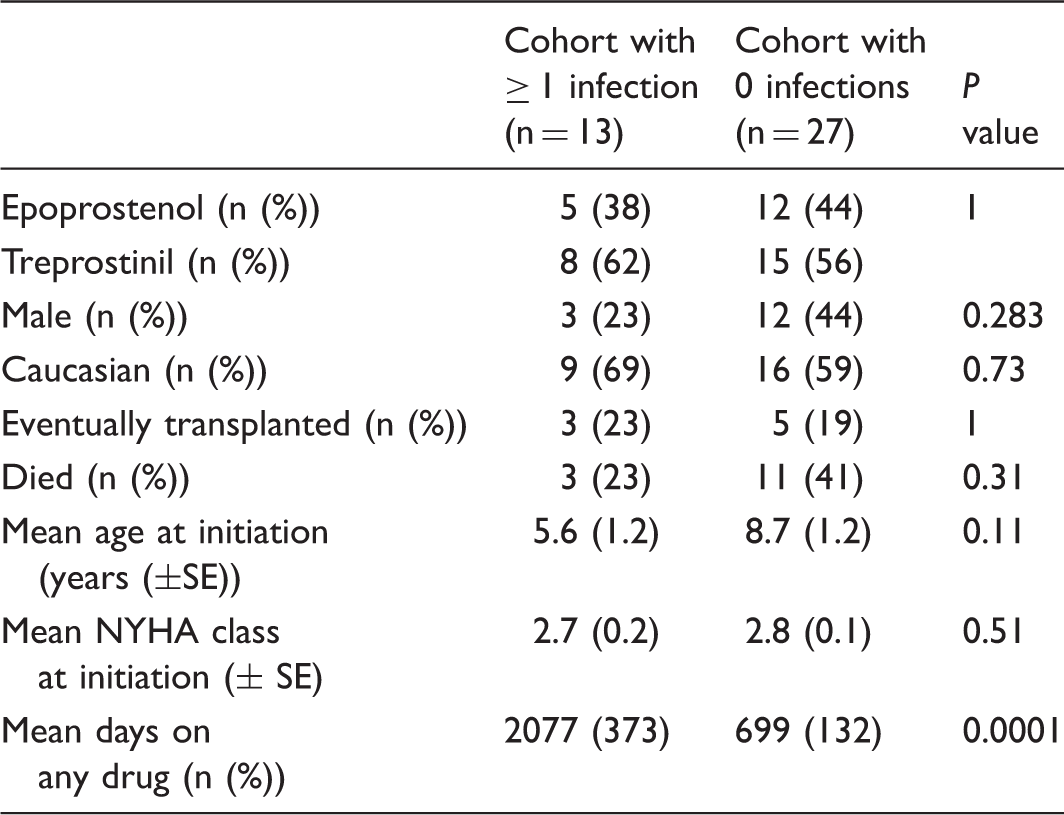
P values calculated using Fisher’s exact test comparing characteristics of cohort with ≥ 1 infection with the cohort with 0 infections.
Central line infections
Central line and prostanoid treatment characteristics.
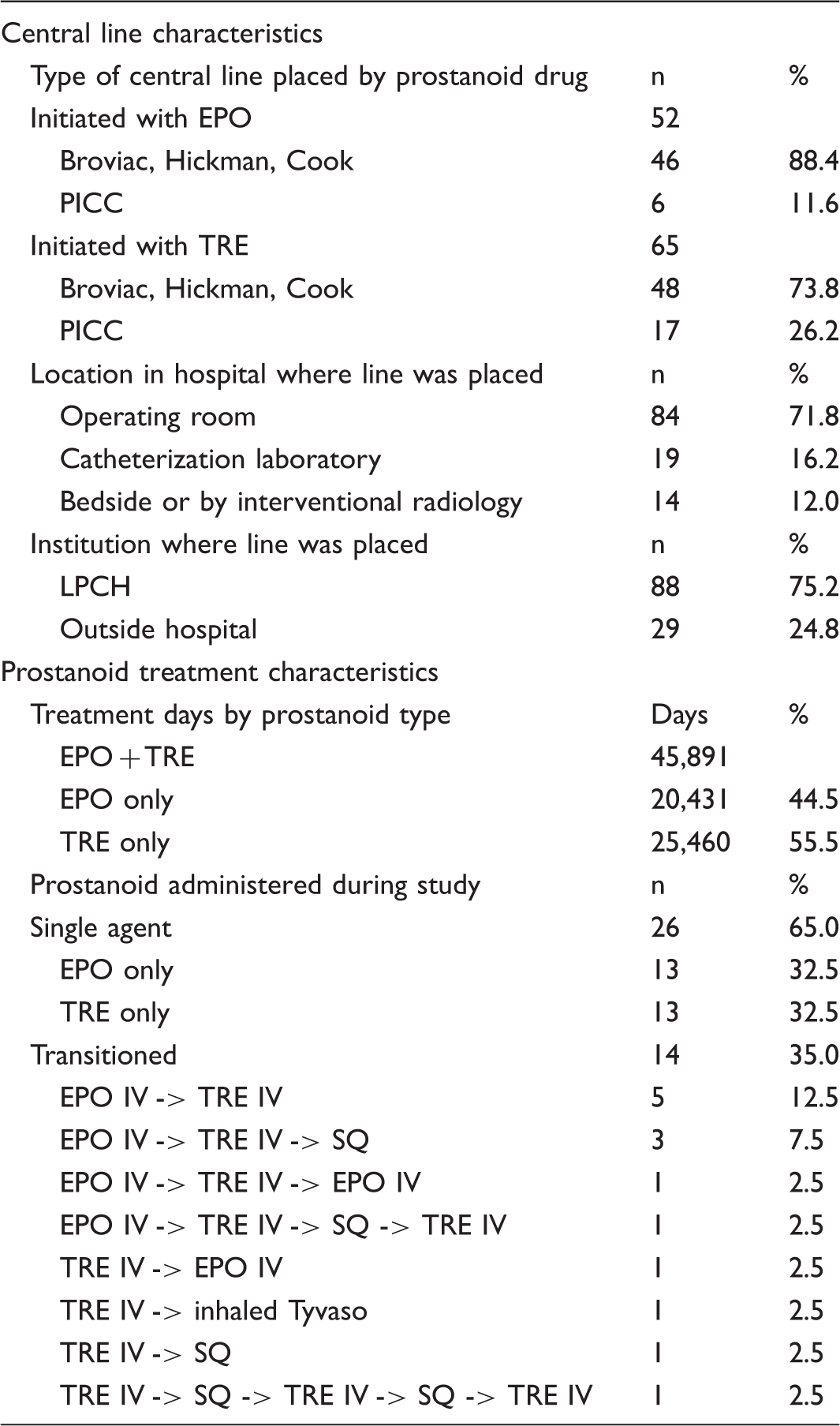
EPO, epoprostenol; TRE, treprostinil; IV, intravenous; SQ, subcutaneous.
Twenty-seven patients experienced no bloodstream infections (67%); six (15%) had one episode and seven (18%) had more than one episode. The infection-free and infected cohort did not differ by age, race, gender, or NYHA class. The infection-free cohort spent significantly fewer days on drug (699 vs. 2077, P < 0.01) (Table 1).
Organisms isolated in each of the prostanoid cohorts are summarized in Fig. 1. In the 13 patients with ≥ 1 infection, 38 episodes yielded 49 pathogens (35 GP, 14 GN) cultured. Ten episodes were polymicrobial: two grew three pathogens; nine grew two pathogens; only one polymicrobial infection included both a GN and GP pathogen. When there was a documented catheter tip culture (three episodes), it grew the same organism as the blood culture.
Organism-specific central line infections associated with trepostinil and epoprostenol treatment. Shown are the specific organisms isolated for each central line infection associated with trepostinil (left panel) and epoprostenol (right panel) treatment. The pie charts indicate the percentage of the total infections that were gram-negative (stripes) or gram positive (solid black), and each category is defined further by a list of organisms in the associated table. P values were calculated using student’s t-test to compare the mean number of GP and GN infections between the trepostinil and epoprostenol cohorts.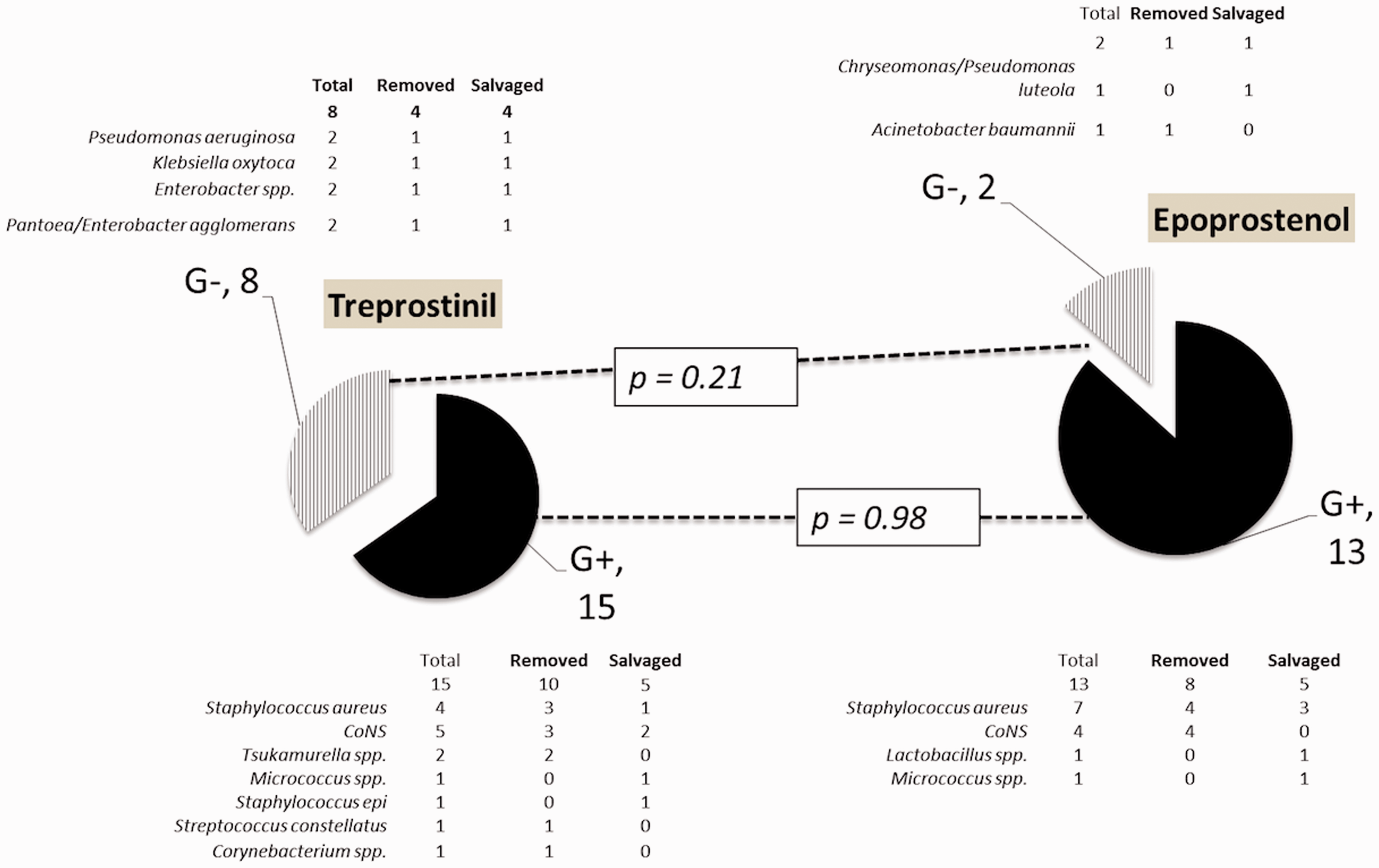
Median length of antibiotic treatment was identical (14 days) between those infections resulting in line replacement and salvage, generally reflecting the guidance set forth by the aforementioned 2009 IDSA CLABSI standards. 19 Average length of treatment was insignificantly longer in the replacement group (17.4 days vs. 15.3, P = 0.63). The overwhelming majority of patients received only intravenous antibiotics, typically some combination of Vancomycin with a third-generation or fourth-generation cephalosporin. Four received concomitant oral antibiotics (mostly Ciprofloxacin) and only two received exclusively oral antibiotics.
Central line infection rates
The pooled infection rate was 0.83 per 1000 prostanoid days (0.73 EPO vs. 0.90 TRE, P = 0.64). The two most common pathogens in both groups were Staphylococcus aureus (S. aureus) (47% EPO, 27% TRE) and coagulase-negative Staphylococci (CoNS) (27% EPO, 33% TRE). GP infection rates were similar between EPO and TRE (0.63 and 0.59/1000 days, respectively, P = 0.98), while the GN infection rates tended to be lower in those receiving EPO compared with TRE (0.1 vs. 0.31/1000 days, P = 0.21).
Central line reinfection rates stratified by line salvage or replacement
Line infection rates for the 38 episodes are shown in Fig. 2. No significant difference (P = 0.63) in reinfection rate was seen when comparing rates after line salvage to replacement (9.4 vs. 7.1 per 1000 line days) (Fig. 2a). In addition, there was no significant difference in infection rate following the line management when grouped by organism type (GP reinfection rates: 8.5 when replaced vs. 7.2 when salvaged; GN reinfection rates: 2.34 vs. 13.8, salvage vs. replace, respectively) (Fig. 2b).
Central line infection rate following central line salvage compared to central line replacement. Shown are the mean infection rates (±SE) after an infection episode led to central line salvage (solid black bars) or replacement (stripes bars) for all infections (a) and by GP organisms compared with GN organisms (b). P values were calculated using student’s t-test to compare the mean infection rate of all organisms, and of GP and GN infections between the central line salvage compared to central line replacement cohorts.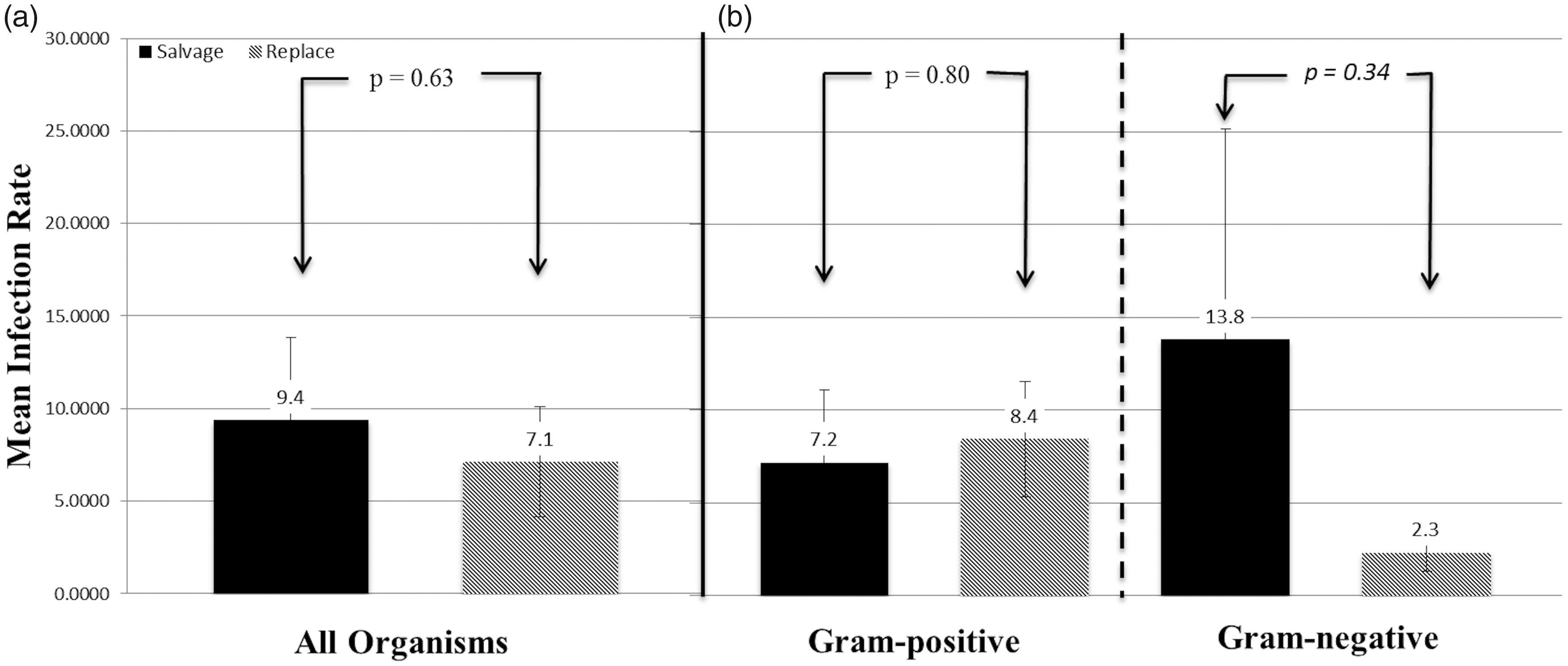
The mean number of days to next infection/study exit following a line management decision is shown in Fig. 3. For both organisms (Fig. 3a) and organism-type (Fig. 3b), comparisons suggest a longer time until next infection/study exit following line salvage compared to line replacement (732 days vs. 410 days until next infection overall; 793 days vs. 363 days for GP; 611 days vs. 581 days until next infection for GN), though these differences were not significant (P > 0.05 for all comparisons).
Mean number of days to next infection following central line salvage compared with central line replacement. Shown are the mean number of days until the next infection (±SE) after an infection episode led to either central line salvage (solid black bars) or replacement (stripes bars) for all infections (a) and by GP organisms compared with GN organisms (b). P values were calculated using student’s t-test to compare the mean number of days until next infection of all organisms, and of GP and GN infections between the central line salvage compared to central line replacement cohorts.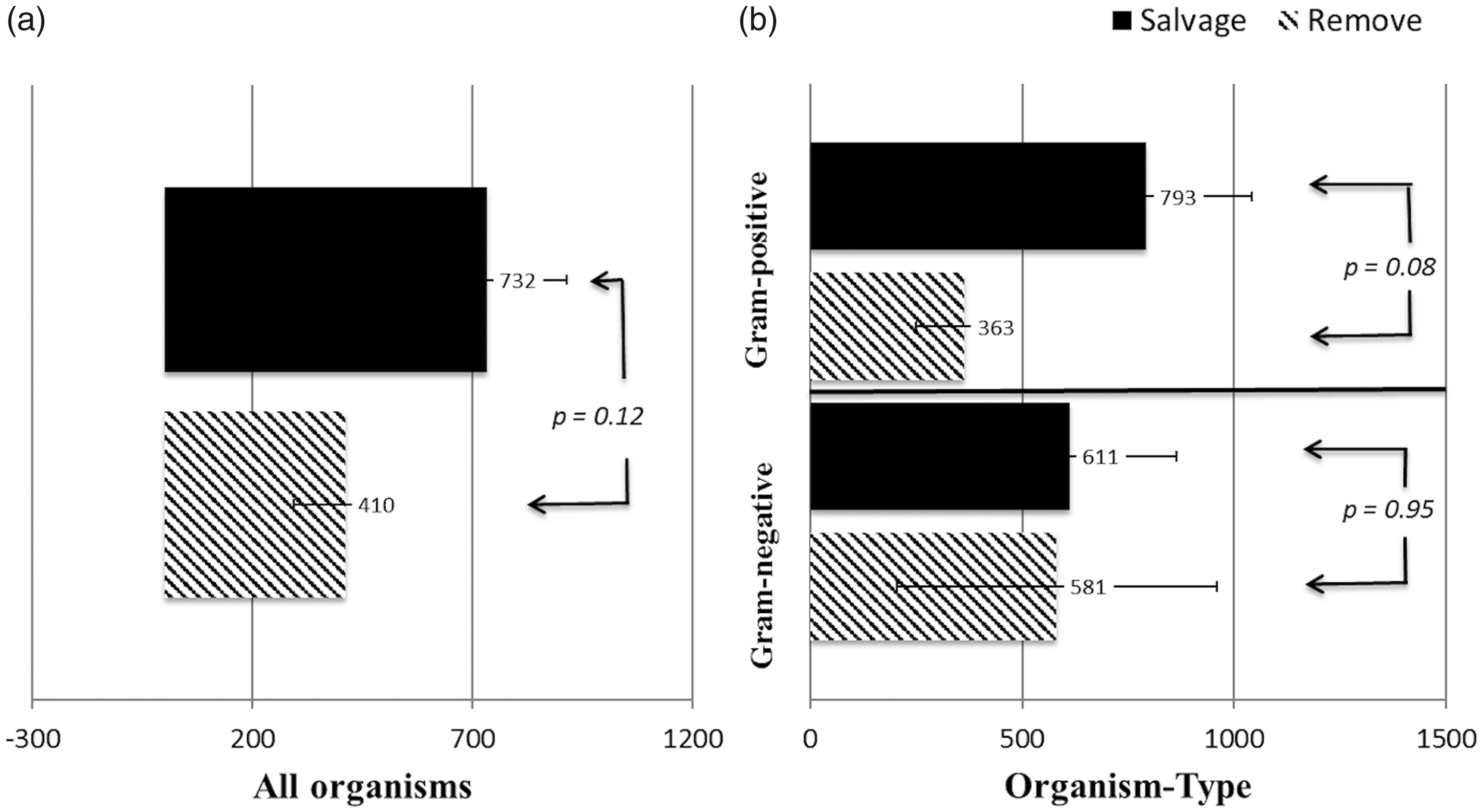
Staphylococcus aureus line infection reinfection outcomes by line management.

P values calculated using Fisher’s exact test comparing reinfection numbers after line replacement compared with after line salvage.
Notably, our trends for both replacement and salvage oscillate over time and do not suggest that the 2009 CLABSI standards strongly biased our results towards salvage, with five salvage and four replacement decisions made between 2010 and 2014.
Discussion
Pulmonary hypertension (PH) is a life-threatening disease associated with significant morbidity and mortality.4,5 Treatment with prostanoids poses unique challenges dictated by their extremely short half-life and requirement for continuous infusion. Thus, children receiving IV prostanoids are at risk of CLABSI. 14
Evidence before this study and added value of this study
While studies have documented the CLABSI rates among PH patients receiving IV prostanoids,8–12,14,15 few studies have analyzed pediatric PH populations. 17 This study examines not only the types of infections and infection rates in children receiving IV prostanoid drugs, but also the effect of line management strategies on reinfection.
The results from the current study show an overall infection rate of 0.83/1000 days in all patients receiving IV prostanoid therapy, with only 13 of 40 patients experiencing a line infection. This rate is comparable to or better when compared with previous PH studies and is a relatively low infection rate compared to other studies documenting CLABSI rates for children who depend on central lines for survival.8–15,17,20
This study attempted to define the risk factors for line infection by comparing the characteristics of those who experienced a line infection with those who did not. Our analysis shows that the characteristics of the two groups are similar, except for the number of days on drug. Previous studies corroborate this finding that longer catheter exposure carries a continued infection risk. 9 Surprisingly, younger age and more severe disease (NHYA class) were not associated with increased risk; therefore “total medicine days” was the only significant identifiable risk factor for CLABSI in our cohort.
Seven patients experienced 32 of the 38 reported infections; these “frequent infection” patients may have been clinically different from the remainder of patients. To address this, we compared the five patients who experienced more than two infections to the eight patients who experienced 1–2 infections, using the same analysis from Table 1. We found no statistically significant difference in any of the characteristics between the two groups, including “total medicine days.”
We found that our “frequent infection” patients each underwent both line management strategies. We compared the type of PH (idiopathic versus non-idiopathic) within salvage and removal decisions; we found no statistically significant difference. Together, these suggest that our decisions were not biased by indication (nor biased by patient).
Importantly, we showed that the infection rate was not impacted by whether a line was replaced or salvaged. Prior studies in this population have not investigated the implications of salvage-versus-replacement decisions. One study demonstrated an institutional bias for line removal in adult PH patients receiving IV iloprost, 20 while others reported successful treatment in catheter-related bloodstream infection (CRBSI) with line retention in other patient or general populations.8,23
Critical to the decision to retain or replace a line is the reinfection risk. To examine this, we focused on the following issues: (1) generally, should infected lines be salvaged or replaced; (2) do specific organisms necessitate line replacement; (3) are infection rates particular to prostanoid type necessitating line replacement for one treatment but not the other; and (4) are the types of organisms different depending on medication type, thus guiding empiric antimicrobial therapy?
Our data demonstrated no difference in overall rate of infection following the decision to replace a line compared to line salvage. Nor was there a difference in time to next infection (reinfection rate), and line salvage showed a longer time to reinfection compared with line replacement. In this study, infection with GP or GN organisms showed no effect on line infection rates, reinfection rates, or length of time until next infection regardless of line management. The line reinfection rates were essentially the same following line salvage and replacement for GP; however, the reinfection rate for GN was weighted towards higher reinfection rates after line salvage. This may reflect a trend, but due to low numbers of GN organisms, was not statistically significant.
Despite existing guidelines, 24 with the exception of a few pathogens, the decision to replace a central line is typically at the discretion of the provider. Our low number of total infections complicated the comparisons within organism groups. However, for our most-common pathogen, S. aureus, we found that the decision to salvage or replace a line occurred with no significant difference in frequency. The 11 S. aureus infections resulted in seven line replacements and four line salvages with a slight bias toward replacement; however, two line replacements involved polymicrobial infections which may have biased the decision toward replacement. This intra-organism variability supports the need for further investigation of CLABSI in this patient population. From these S. aureus infections, we found no significant difference in the number of subsequent infections or in the number of relapses with the same organism, regardless of line salvage or replacement. However, our results showed all S. aureus reinfections followed line salvage.
(3 and 4) Previous studies have suggested that infection rates are higher with TRE than EPO and that the rate of TRE-associated GN infections is higher.25,26 The results of the current study agree with these findings: we observed a slightly higher rate of TRE-associated infections with a higher proportion of GN infections in the TRE group, though neither was statistically significant.
Despite the higher incidence of GN infections in the TRE group, there was still a predominance of GP organisms in both groups, which is consistent with previous studies 19 and aligns with the usual pathophysiology of catheter infections caused predominately by GP organisms colonizing the skin.9,14–16 This finding is important to guide empiric antibiotic choice, which according to this study, should target GP organisms first with a low threshold to expand to GN coverage in children receiving TRE who have no or poor clinical response to initial antimicrobial therapy.
Implications of the available evidence
The results of the current study provide information regarding the necessity for removal of infected catheters. Our data suggest that the outcomes are not better when lines are replaced rather than salvaged. The nature of pediatric PH, which requires continuous prostanoid therapy for long periods of time, highlights the importance of carefully considering whether the infected central line should be salvaged or replaced. This study supports the consideration for line salvage in most instances regardless of the infectious organism in this patient population. In the absence of a PH-specific protocol, this study demonstrates that even in an unbiased situation, neither the organism nor the decision to remove or salvage the line impacted outcomes. Considering that line salvage did not impact infection rate in a negative way, and that line removal involves a procedure that increases the risk of losing vascular access, our experience suggests that salvage should be the favored approach. In addition, guidelines for targeted preliminary antimicrobial therapy can also be garnered by the predominance of GP organisms isolated in this study population.
The most significant limitation to our study is the low number of infections despite the large number of catheter days. A second limitation is the fact that some organisms require discontinuation of the line, i.e. Tsukamurella. This organism is included in two episodes of infection in our study and implies that two GP infections were perhaps evaluated with a different bias than the more open-ended approach applied to other organisms. Another limitation is our institutional bias, which influenced the decisions made for children cared for at other institutions (consultation with our PH physician is the norm). None of our patients had their lines replaced by rewiring, which might have carried separate unique reinfection risk. Finally, we chose to include in our study BSI with organisms that are often considered common commensals (in particular, CoNS, Corynebacterium, and Micrococcus). We included these organisms because in 8/13 episodes where the “commensal/contaminant” was either the lead or the only organism, the line was replaced. We felt that eliminating these episodes would both underrepresent the infection experience at our center and limit its application at other centers where similar commensal/contaminant BSI line management decisions occur. Despite these biases, the high number of total line days and the consistent care that the patients received strengthen the validity of these results. A multi-center reproduction of our analysis would help to apply these findings to the pediatric PH population and others who rely on central lines.
In conclusion, our study shows a relatively low rate of line infections in these children, a predominance of GP organisms when lines are infected, and no advantage to line replacement for management of line infections. This constellation of findings would support initial management of uncomplicated line infections to include empiric antimicrobial therapy targeting GP organisms delivered with the line in place.
Footnotes
Acknowledgements
The authors thank the families who participated in this study.
Conflict of interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
