Abstract
Chronic infusion of prostacyclin (PGI2) via a Broviac central venous line (CVL) is attended by risk of CVL-related complications, but we know of only one report regarding CVL-associated bloodstream infection (BSI) with PGI2 in children and none regarding other complications. We conducted a retrospective cohort study involving pediatric patients with pulmonary hypertension treated with chronic intravenous infusion of PGI2 at Boston Children's Hospital and determined the rate (per 1,000 line-days) of various CVL-related complications. We also determined how often complications necessitated line replacement and hospitalization, time to replacement of CVLs, and interpatient variability in the incidence of complications. From 1999 until 2014, 26 patients meeting follow-up criteria had PGI2 infusion, representing 43,855 line-days; mean follow-up was 56 months (range, 1.4–161 months). The CVL complication rates (per 1,000 line-days) were as follows: CVL-BSI, 0.25; superficial line infection, 0.48; impaired integrity, 0.59; occlusion, 0.09; and malposition, 0.32. The total complication rate was 1.73 cases per 1,000 line-days. All CVL-BSI and malposition cases were treated with CVL removal and replacement. Of CVLs with impaired integrity, 23 could be repaired and 3 required replacement. Six of 21 superficial CVL infections required replacement of the CVL. Three of 4 occluded CVLs were replaced. CVL complications occasioned 65 hospitalizations. There was marked interpatient variability in the rate of complications, much but not all of which appeared to be related to duration of CVL placement. We conclude that non-BSI complications are very significant and that efforts to teach and emphasize other aspects of line care are therefore very important.
Chronic intravenous infusion of the prostacyclin (PGI2) analogues epoprostanol and treprostinil, usually through a Broviac central venous line (CVL), has been the most effective therapy for severe pulmonary arterial hypertension (PAH) since 1996, 1 but it is attended with the risk of CVL-related complications. There are multiple reports focused on CVL-related bloodstream infections (BSIs) in adults2–5 but only a single report regarding CVL-BSI with PGI2 infusion in mostly pediatric patients (although the age of the patients is not given), 6 and we know of no information regarding the incidence of other complications (e.g., CVL superficial infection, fracture, displacement, and occlusion) in this setting. Children may be at different risk than adults for CVL complications owing to high activity levels, being less mindful of the need for CVL protection, and possibly other factors. Noninfectious complications are also important, as they frequently require hospital visit, admission, or CVL replacement, and their rate of occurrence may substantially exceed that of CVL-BSI.7,8 A better understanding of non-BSI complications associated with CVLs in pediatric patients receiving PGI2 analogues could lead to strategies to reduce such events. Also, an alternative means of administering parenteral PGI2 (subcutaneous infusion of treprostinil) eliminates CVL-related complications but is attended with problems of its own.9,10 Choosing between alternate means of delivery might best be based, in part, upon the relative risks of complications associated with each method.
We conducted a retrospective cohort study involving pediatric patients treated with chronic intravenous infusion of PGI2 in the Pulmonary Hypertension Program at Boston Children's Hospital (BCH). We determined the rate (normalized to 1,000 line-days) of CVL-BSI, CVL superficial infections, CVL impaired integrity (fractures and/or perforations), CVL occlusion, and CVL retraction. We also determined how often these complications necessitated line replacement and hospitalization, the time-to-replacement (all causes) of the CVLs, and interpatient variability in the risk of complications.
METHODS
Hospital records were retrospectively reviewed for all patients less than 18 years old at the time of initiation of chronic intravenous infusion of epoprostanol and/or treprostinil for PAH who were subsequently followed up at BCH. CVL placement occurred between May 1999 and January 2014; follow-up extended to March 31, 2014. Only patients who were discharged from the hospital with ongoing PGI2 therapy with at least 60 days of follow-up were included. Patients who were treated with PGI2 but not discharged with ongoing therapy or patients who were followed up at referring institutions were excluded from the study. Three patients had their CVL placed at another institution but were followed up at BCH; if the exact date of placement could not be ascertained, a latest possible date was assigned on the basis of available information.
A variety of demographic and clinical factors were captured, including types of CVL-related complication, CVL complications per 1,000 catheter-days, and infectious organisms identified. We assessed the relationship between the analogue of PGI2 infused and the risk of CVL-BSI and the organisms responsible. CVL survival after initial CVL placement (taking into account all-cause need for replacement) was determined.
All patients had a tunneled single-lumen Broviac catheter that was inserted in a subclavian or internal jugular vein or tributary. Epoprostanol diluent was used for treprostinil dilution. 11 Criteria for diagnosing CVL-BSI were fever and at least 1 peripheral blood sample with a positive culture result. CVL-BSIs were treated in all cases with intravenous antibiotics, CVL removal, and (after the blood was sterilized) CVL replacement. Superficial CVL infection was diagnosed with the presence of redness with or without suppuration at the CVL exit site or along its track; such infections were treated with enteral with or without intravenous antibiotics. Fractures and/or perforations of the CVL (referred to as impaired integrity) were repaired with a commercially available kit whenever possible. CVL occlusions were defined by inability to infuse through or draw back from the CVL. CVL malpositions were instances in which the CVL was dislodged or retracted, inadvertently or through patient growth, sufficiently far that it had to be replaced.
Statistical analysis
Time from the first CVL placement to replacement (necessitated by a complication) was determined by Kaplan-Meier analysis. Linear regression analysis was used to determine the relationship between the number of CVL complications and the number of line-days. This retrospective review was approved by the BCH institutional review board.
RESULTS
From May 1999 until January 2014, 26 patients were discharged after initiation of chronic PGI2 intravenous infusion and were followed up at BCH for at least 60 days as outpatients. All had group 1 pulmonary arterial hypertension (PAH); characteristics of this cohort are listed in Table 1. During the period of follow-up, 14 patients had their CVL intentionally removed for reasons unrelated to a CVL complication (2 because of miscellaneous technical issues, 7 because of lung transplantation, and 2 because of clinical improvement obviating the need for PGI2; 3 patients died with the CVL in place; Fig. 1).
Characteristics of patients and follow-up
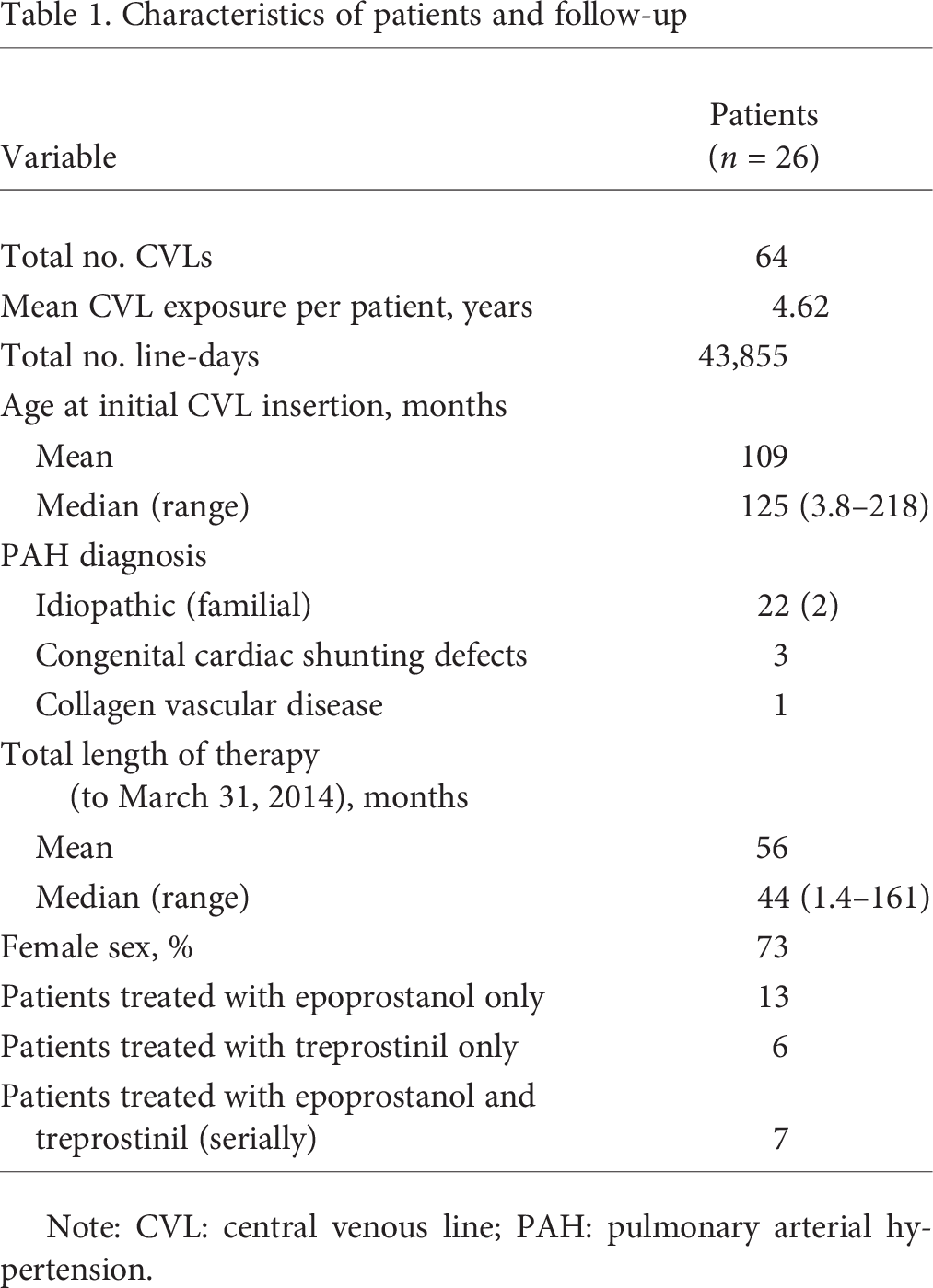
Note: CVL: central venous line; PAH: pulmonary arterial hypertension.
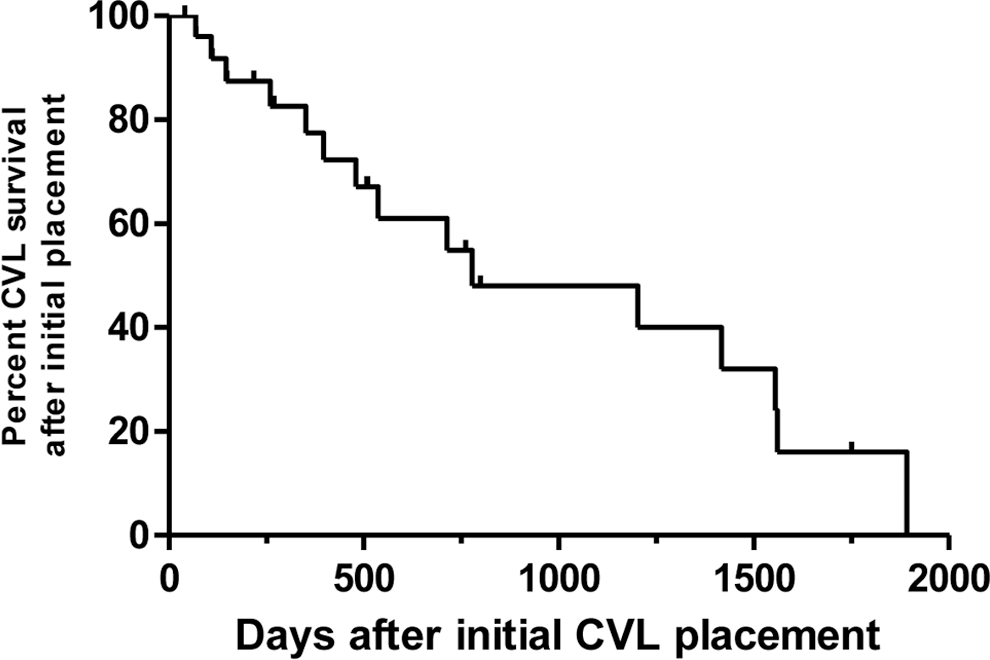
Kaplan-Meier analysis of central venous line (CVL) survival from time of initial placement of the CVL until removal due to complication. Patients whose CVL was electively removed, who had lung transplantation, or who died were censured.
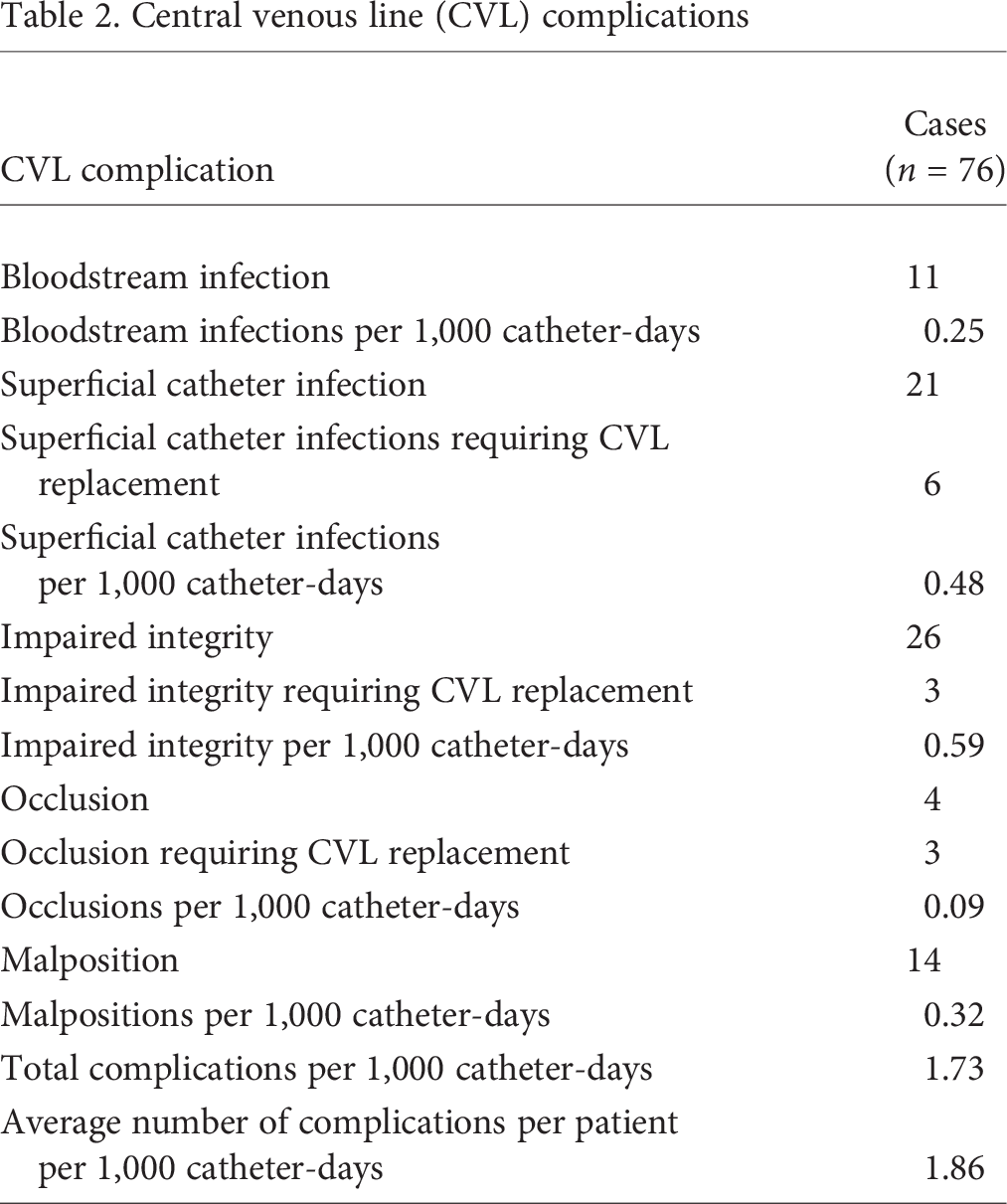
Table 2 contains a summary of the CVL complications; the CVL complications normalized to CVL-days for each individual patient are depicted in Figure 2. Of the cases of impaired integrity, 23 CVLs could be repaired, but 3 required replacement. Of the 21 superficial line infections, 6 required CVL removal and replacement. Three of the 4 occluded CVLs necessitated replacement. CVL complications necessitated 65 hospitalizations.
Central venous line (CVL) complications
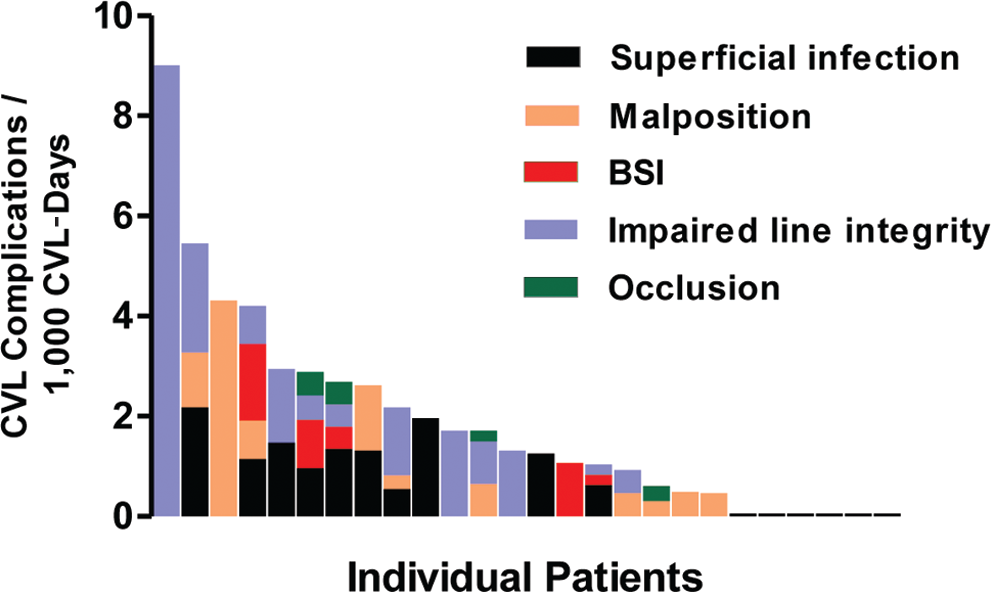
Central venous line (CVL) complications per 1,000 catheter-days for each patient. Six patients had no CVL complications. BSI: bloodstream infection.
CVL-BSI for epoprostanol and treprostinil and the organisms involved are listed in Table 3; the rates of BSI for the two analogues were little different, but there was a predominance of gram-negative organisms with treprostinil.
Comparison of central venous line–associated bloodstream infections (BSIs) in patients treated with prostacyclin (PGI2) analogues

DISCUSSION
Intravenous PGI2 analogues have greatly improved the quality and duration of life for many patients with PAH, but the requisite CVL poses a significant burden and poorly quantified risk of complication for those so treated. We aimed to better understand these CVL complications by reviewing our experience with this therapy. Our overall rate of CVL-BSI (0.25 cases per 1,000 catheter-days) is remarkably similar to that reported by Ivy et al. 6 among pediatric patients after instituting enhanced preventative measures (0.24 cases per 1,000 catheter-days), although we report a greater number of CVL-days (43,855 vs. 8,308). The REVEAL registry reported that the rate of CVL-BSI for patients ≤18 years old (n = 83 patients; the number of patient-days was not given) was no different than the rate for adults (0.20 cases per 1,000 CVL-days), but the exact number was not given. 2
The incidence of CVL-BSI among adults treated with PGI2 analogues is 0.1–1.13 cases per 1,000 catheter-days.5,12 The REVEAL registry report is the largest, with 1,063 patients >18 years old with at least 5 years of follow-up (the number of CVL-days was not given). 2 As noted above, the overall rate of CVL-BSI was 0.20 cases per 1,000 line-days (epoprostanol = 0:12, treprostinil = 0:36), with more gram-negative infections associated with the latter analogue.
It was apparent by at least 2006 that treprostinil was associated with a higher rate of CVL-BSI than epoprostanol, especially with gram-negative organisms.3–5 The reason for this was initially unclear,3,6,11 but in vitro studies showing that the pH-basic epoprostanol diluent (pH 10.2–10.8) was far more effective in suppressing bacterial growth than the normal saline diluent initially recommended for treprostinil (pH 6.0–7.2) suggested a possible explanation.6,11,13 Consistent with this notion, a prospective study (with a historical control group) found that use of epoprostanol diluent with treprostinil substantially reduced the rate of gram-negative CVL-BSI and possibly reduced the overall rate of CVL-BSI (P = 0:06). 11 A similar association of gram-negative infection with neutral pH diluent was observed in a retrospective study involving intravenous iloprost. 5 Our rates of BSIs per 1,000 catheter-days (0.21 for epoprostanol and 0.32 for treprostinil) are similar to those reported by Ivy et al. 6 among pediatric patients (epoprostanol = 0:33; treprostinil = 0:19). We also observed a predominance of gram-negative infections among the patients in the treprostinil group (Table 3). Because we used epoprostanol diluent for all of our patients in the treprostinil group, the predominance of gram-negative organisms in this group might suggest that more than pH may be relevant (at least in our patient cohort).
The rate of complications due to causes other than CVL-associated BSI was considerably higher than the rate of CVL-associated BSI. Other reports of Broviac catheters used to treat children for other indications (e.g., oncological or hematologic disorders or parenteral nutrition) have also reported a greater rate of mechanical complications than of BSIs. For example, Fratino et al. 7 reported that infectious complications (not all of which were BSIs) occurred at a rate of 0.46 cases per 1,000 line-days, whereas catheter dislodgement, rupture, or occlusion occurred at a rate of 0.97 cases per 1,000 line-days. Cesaro and co-workers 8 reported a mechanical complication rate of 4.5 cases per 1,000 line-days and a rate of infection of 1.7 cases per 1,000 line-days among pediatric hematology and oncology patients with Broviac catheters. On the other hand, two reports (one involving pediatric patients and another involving adults) indicated a higher rate of infectious than mechanical complications associated with Broviac catheters.14,15 Regardless of their nature, CVL complications were expensive and burdensome, as they resulted in 65 hospitalizations. There was marked variability from patient to patient in the rate of CVL-related complications (Fig. 2). It is perhaps not surprising that the length of time that the CVL is in place is related to the number of complications (Fig. 3), although this regression analysis suggests that other factors are also important.
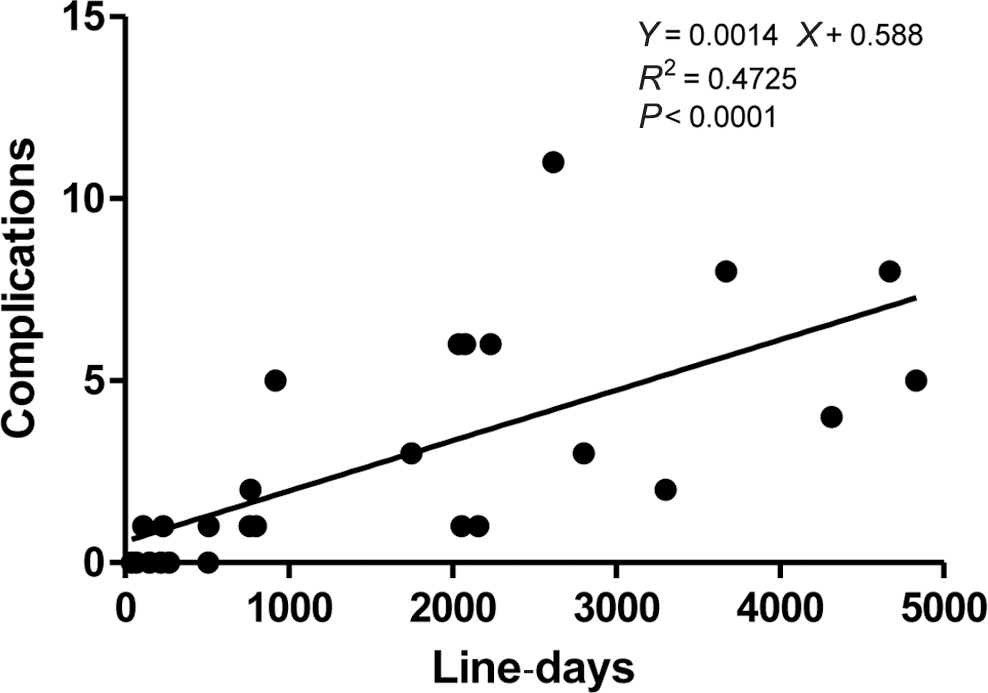
The number of central venous line (CVL) complications is associated with the number of CVL-days.
We conclude that CVL-BSIs can be important adverse events for patients treated with PGI2 analogues but are only one of multiple types of CVL-associated complications that necessitate interventions and sometimes hospitalization. Meticulous CVL care aimed at minimizing the risk of infection is important, but so too is reducing the likelihood that the CVL will be fractured or dislodged. We suggest that the following may be helpful in reducing mechanical complications related to the CVL: (1) Inform patients and/or families that, although strict measures to prevent infection are of critical importance, experience shows that injury to the CVL is at least as likely to occur; reinforce the idea that the catheters will experience failure with repeated stress. (2) Show families how to secure the catheter and connector in a way that minimizes stretching, compression, kinking, and repeated mechanical stress at the same location of the CVL (i.e., contrive to limit such forces to the connector). (3) Finally, there may be room for improvement in the design of or materials used for Broviac catheters. For example, a thicker-walled extracorporeal segment of the catheter would resist fracture better. A protective sleeve of thin, tough, and flexible plastic to reduce bending, torsion, and other loads on the catheter, presuming it could be appropriately secured, may be helpful.
Footnotes
ACKNOWLEDGMENTS
The authors would like to acknowledge the expert assistance of Ms. Lynne Patkin in preparation of the manuscript.
