Abstract
The simultaneous occurrence of manic and depressive features has been recognized since classical times, but the term ‘mixed state’ was first used by Kraepelin at the end of the 19th century. From the 1980s, until the advent of the Diagnostic and Statistical Manual of Mental Disorders, fifth edition (DSM-5), psychiatric disorders were classified using a categorical approach. However, it was recognized that such an approach was too rigid to encompass the range of symptomatology encountered in clinical practice. Therefore, a dimensional approach was adopted in DSM-5, in which affective states are considered to be distributed across a continuum ranging from pure mania to pure depression. In addition, the copresence of symptoms of the opposite pole are captured using a ‘with mixed features’ specifier, applied when three or more nonoverlapping subthreshold symptoms of the opposite pole are present. Mixed features are common in patients with mood episodes, complicating the course of illness, reducing treatment response and worsening outcomes. However, research in this area is scarce and treatment options are limited. Current evidence indicates that antidepressants should be avoided for the treatment of bipolar mixed states. Evidence for bipolar mixed states supports the use of several second-generation antipsychotics, valproate and electroconvulsive therapy. One randomized controlled trial has demonstrated the efficacy of lurasidone, compared with placebo, in patients with major depressive disorder with mixed features, and there is limited evidence supporting the use of ziprasidone in such patients. Further research is required to determine whether other antipsychotic agents, or additional therapeutic approaches, might also be effective in this setting.
Introduction
Roger S. McIntyre, Mood Disorders Psychopharmacology Unit, University of Toronto, Canada
The concept of mixed states is of historical, conceptual, diagnostic and therapeutic relevance to psychiatry. 1 Its origins began in the classical writings of Hippocrates and Plato and, later, continued in the writings of Heinroth, Falfret, Kahlbaum, Weygandt and Kraepelin. 1 The early nosological theme was combinatorial; Kraepelin, for example, conceptualized affective states as a continuum of three dimensions of mood–thought–volition, resulting in the definition of six types of mixed state (depressive or anxious mania, excited depression, manic with thought poverty, manic stupor, depression with flight of ideas and inhibited mania), in addition to pure mania and pure depression. 2 Kraepelin’s dimensional approach prevailed until 1980, when the Diagnostic and Statistical Manual of Mental Disorders, third edition (DSM-III), balkanized manic depression into major depressive disorder (MDD) and bipolar disorder (BD), effectively ‘orphaning’ mixed states into distinct diagnostic categories. 1
This categorical approach continued into subsequent DSM iterations, until the advent of DSM-5, which adopted a neo-Kraepelian ‘mixed-categorical-dimensional’ approach, whereby categorical diagnoses were supplemented dimensionally.3,4 Thus, in DSM-5, affective states are considered to be distributed across a continuum ranging from pure mania to pure depression. The copresence of symptoms of the opposite pole are captured using a ‘with mixed features’ specifier, which is applied when three or more nonoverlapping subthreshold symptoms of the opposite pole are present (Figure 1).3–5

DSM-5: moving from a categorical to a dimensional approach to classification of mood disorders.
The approach adopted in DSM-5 is pragmatic but linear, since it implies that mania and depression are at opposite poles of a spectrum. However, mania and depression are not negatively correlated and often occur together, frequently manifesting as overarousal, anxiety and/or agitation, indicating that an orthogonal, rather than linear, approach to nosology may be more appropriate. Along with arousal and anxiety, affective lability, manifesting as irritability, is the modal presenting feature of mixed features. Moreover, data have demonstrated that affective lability is penetrant through families, with the occurrence of familial panic episodes (panic attacks and panic disorders) increasing an individual’s likelihood of rapid mood cycling. 6
MDD with mixed features presents unique challenges in terms of diagnosis and treatment. The DSM-5 field trials found a low level of inter-rater reliability on the diagnostic phenotype of MDD, in comparison with BD-I and BD-II, indicating that the more depression prone an individual’s phenotype, the more likely they are to be misdiagnosed and/or treated inappropriately. 7 Furthermore, results from the International Mood Disorders Collaborative Project showed that mixed features are commonly encountered in adults with both MDD and BD: approximately one quarter of those diagnosed with MDD and one third of those diagnosed with BD-I or BD-II met the DSM-5 criteria for mixed features. 8 Therefore, many patients with mixed features are likely to experience misdiagnosis, diagnostic delay and/or inappropriate treatment.
MDD with mixed features results in a substantial burden to both individuals and society. Compared with those with MDD, patients with MDD with mixed features have significantly higher rates of suicidal ideation, suicidality, anxiety disorders and substance use disorders; they also receive significantly higher levels of polypharmacy, a proxy for the severity of this phenotype (Figure 2). 9 Healthcare resource utilization, in terms of outpatient visits, inpatient stays, emergency department use and pharmacy costs, is also significantly higher for patients with MDD with mixed features than for those with MDD. 9 In addition, MDD with mixed features has a serious impact on patients’ physical health, increasing the risk of cardiovascular disease, in comparison with other types of mood disorder. 8

Suicidality, comorbidities and medication use in patients with major depressive disorder (MDD) with mixed features, compared with those with MDD: real-world assessment at 1-year follow up.
This article is based on a symposium, convened during the 30th Annual European College of Neuropsychopharmacology Congress (September 2017, Paris, France), which sought to discuss the implications of the DSM-5 approach to classifying mood disorders, in terms of diagnosis and treatment, with a particular focus on the challenges associated with managing patients with mixed features in clinical practice.
Addressing patients’ needs across the spectrum of mood disorders
Allan H. Young, Institute of Psychiatry, Psychology and Neuroscience, King’s College London, UK
The shift towards a ‘continuum’ approach to mood disorders, adopted in DSM-5, arose because the real-world presentation of mixed states was not aligned with the definition of mixed states in the DSM fourth edition text revision (DSM-IV-TR). In particular, subsyndromal ‘opposite pole’ symptoms are known to be common in MDD and BD, but are not accounted for in DSM-IV-TR. 10 It was also evident that there was a high rate of misdiagnosis of BD and that many patients were receiving inappropriate therapy. 5 Therefore, DSM-5 conceptualizes mania and depression as falling along a continuous spectrum, with the mixed features specifier acting as a bridge between BD and MDD.3,11
A long-term (mean 17.5 years) follow-up study conducted by Fiedorowicz and colleagues demonstrated that approximately 25% of patients initially diagnosed with MDD went on to experience hypomania or mania, resulting in a revision of their diagnoses to BD-I or BD-II, and that the presence of subthreshold hypomania symptoms predicted progression from unipolar depression to bipolar depression (Figure 3). 12 When these data were analyzed in terms of the number of subthreshold symptoms, there was clear separation between patients with at least three versus less than three subthreshold hypomania symptoms, in terms of likelihood of experiencing a hypomanic or manic episode (Figure 3). 12 Such evidence helped inform the diagnostic criteria adopted in DSM-5, which require the presence of at least three nonoverlapping subthreshold symptoms of the opposite pole to be present for the mixed features specifier to be applied. 3

Kaplan–Meier survival curves for time to change in diagnosis for patients with major depressive disorder (n = 550).
Importance of identifying patients with mixed features
The importance of recognizing patients with mixed features is underscored by evidence demonstrating that, compared with those with unipolar depression, individuals with MDD with mixed features experience a higher lifetime number of depressive episodes, 13 are less likely to respond to antidepressants, 14 experience a higher prevalence of anxiety and substance-use disorders, 13 have increased comorbidity, 15 and are at increased risk of suicide. 16 In addition, they are more likely to be unemployed or disabled and have a disproportionally higher rate of cardiovascular disease. 8
The evidence is similar for patients with BD with mixed features. In a prospective, multinational, naturalistic study of 1035 patients with BD-I (DSM-IV-TR criteria) experiencing a current manic episode with onset within the previous 3 months, 348 (33.6%) were shown to meet DSM-5 criteria for mixed features, having at least three depressive symptoms. 17 Patients with BD with mixed features experienced higher levels of agitation than those with between zero and two depressive symptoms (95% versus 92%), and significantly higher levels of anxiety (99% versus 78%; p < 0.05) and irritability (97% versus 91%; p < 0.05). 17 Thus, although agitation, anxiety and irritability are excluded from the subthreshold symptoms considered when assessing a patient for the presence of mixed features (since they are not specific to either pole of the spectrum), they are nevertheless very common amongst patients with mixed features. Furthermore, the study demonstrated that patients with mixed features had a significantly increased risk of attempting suicide, compared with those with between zero and two depressive symptoms, both during their current manic episode (38% versus 9%; p < 0.05) and during their lifetime (54% versus 26%; p < 0.05). 17 The study also found that the proportion of physicians reporting dissatisfaction with the treatment response of their patients was significantly higher for patients with mixed features, compared with those with between zero and two depressive symptoms (22% versus 14%; p < 0.05). 17
Does DSM-5 adequately identify those with mixed features?
The BRIDGE-II-MIX Study was a multicenter, multinational, cross-sectional study of 2811 adult patients experiencing a major depressive episode (MDE), according to DSM-IV-TR criteria. 18 Its objectives were to estimate the frequency of mixed states in patients with MDE using conceptually different definitions, and to compare the clinical validity of these definitions. 18 These definitions were: (1) DSM-5 criteria for MDE with mixed features (DSM-5-MFS); (2) DSM-5 subthreshold criteria for MDE with mixed features (subthreshold DSM-5-MFS); and (3) Research-Based Diagnostic Criteria for depressive mixed states (RBDC-MFS). Criteria for DSM-5-MFS comprised MDE plus at least three nonoverlapping hypomanic criteria, while those for subthreshold DSM-5-MFS comprised MDE plus at least two nonoverlapping hypomanic criteria (Table 1). The RBDC-MFS criteria were designed to capture the full range of mixed symptoms, including those common to both ends of the mood spectrum, such as irritability and agitation (Table1). 18
BRIDGE-II-MIX Study: criteria 18 for depressive mixed states.
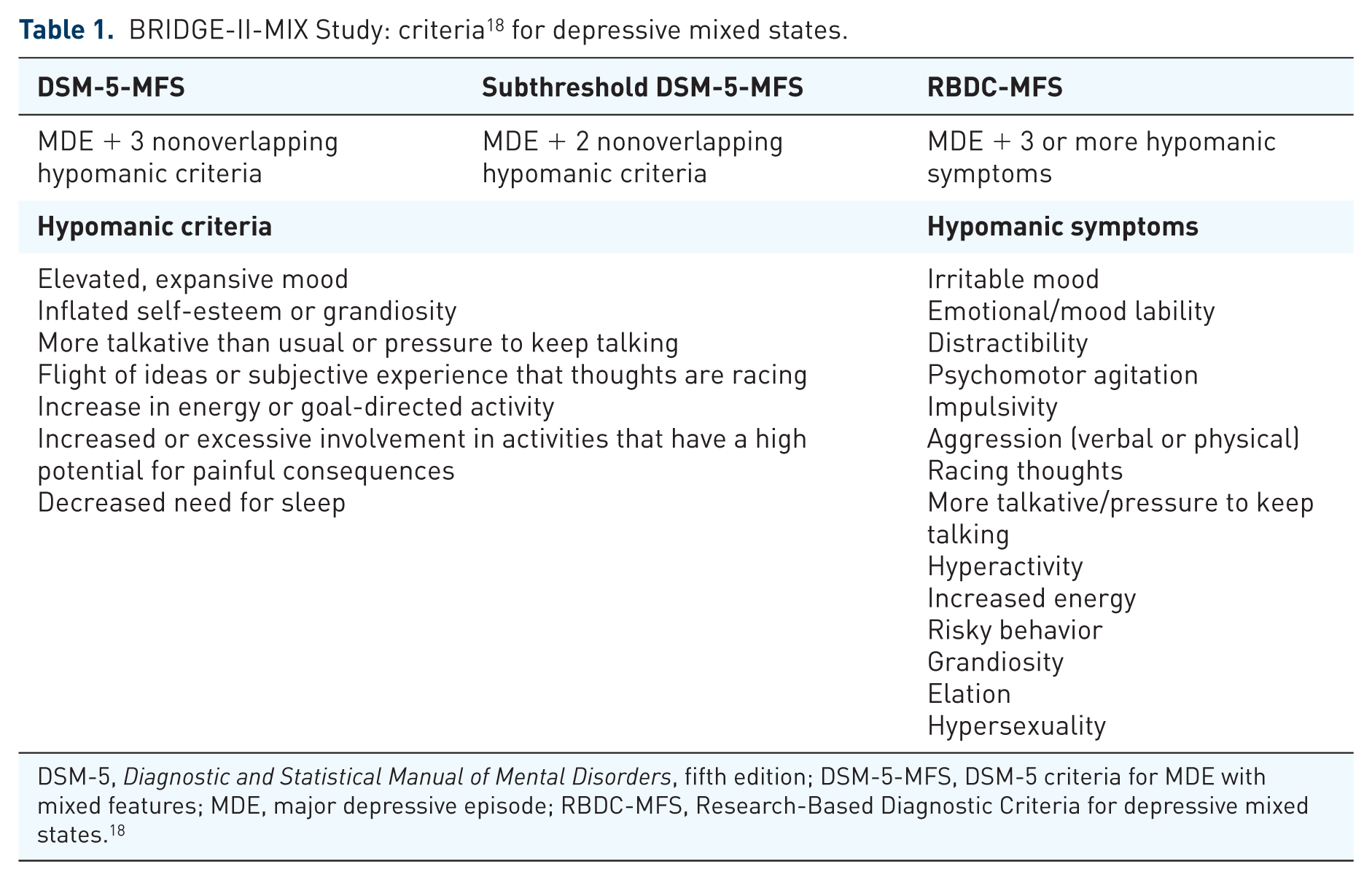
DSM-5, Diagnostic and Statistical Manual of Mental Disorders, fifth edition; DSM-5-MFS, DSM-5 criteria for MDE with mixed features; MDE, major depressive episode; RBDC-MFS, Research-Based Diagnostic Criteria for depressive mixed states. 18
Data were collected on sociodemographic variables, current/past psychiatric symptoms and clinical variables that are known risk factors for BD; clinical variables associated with mixed features were assessed using logistic regression. 18 Overall, the proportions of patients meeting the DSM-5-MFS, subthreshold DSM-5-MFS and RBDC-MFS criteria for mixed features were 7.5%, 15.4% and 29.1%, respectively. 18 All patients who met the DSM-5-MFS or subthreshold DSM-5-MFS criteria also met those for RBDC-MFS. 18 Although not included among the DSM-5-MFS and subthreshold DSM-5-MFS hypomanic criteria, irritability and agitation were present in a high proportion of patients with mixed features, regardless of how this was defined. 18 Of the patients diagnosed with mixed features according to DSM-5-MFS, subthreshold DSM-5-MFS and RBDC-MFS criteria, 81.1%, 75.0% and 84.2% had irritable mood, respectively, and 58.5%, 48.1% and 48.0% had psychomotor agitation, respectively. 18 In comparison with the DSM-5-MFS and subthreshold DSM-5-MFS criteria, the RBDC-MFS criteria not only identified a higher proportion of patients with mixed features, but also provided stronger associations with several readily assessable characteristics of BD, including the presence of anxiety disorders and the lifetime number of suicide attempts. 18 Taken together, these findings indicate that the DSM-5 mixed features specifier may leave many patients with mixed depression undiagnosed and, perhaps, inadequately treated. 18
The BRIDGE-II-MIX Study also provided further evidence that the presence of mixed features increases patients’ risk of suicidality. Of the 2811 patients with MDE recruited into the study, 628 (22.3%) had a history of suicide attempts and 2183 (77.7%) had no history. 19 When the clinical characteristics of these two subgroups were compared, a highly significant correlation was found between the risk of suicidality and the presence of depressive mixed features, as assessed using DSM-5-MFS criteria (odds ratio = 2.03; p < 0.0001). 19
Treatment challenges with mixed states
The Systematic Treatment Enhancement Pro-gram for Bipolar Disorder (STEP-BD) Study demonstrated that antidepressants are ineffective for mixed bipolar depression, since there was little difference in the recovery trajectory between patients who received or did not receive antidepressant treatment (Figure 4). 20 These findings may also have important implications for patients with MDD with mixed features, who similarly may not benefit from antidepressant treatment.

The Systematic Treatment Enhancement Program for Bipolar Disorder: Kaplan–Meier curve for time to recovery by antidepressant use.
Guidelines for the treatment of bipolar mixed states are limited. The World Federation of Societies of Biological Psychiatry (WFSBP) 2009 guidelines for acute mania recognize the lack of evidence for treatment of mixed states and highlight that antimanic efficacy does not necessarily imply efficacy on depressive symptoms; indeed, antimanic efficacy may in fact exacerbate depressive symptoms. 21 Similarly, WFSBP 2013 guidelines for the long-term treatment of BD state that ‘there is a virtual absence of separately extractable information regarding the prevention of hypomania or mixed states as separate entities.’ 22 The International Society for Bipolar Disorders (ISBD) 2013 guidelines on antidepressant use in BD state that antidepressants should be avoided during manic and depressive episodes with mixed features. 23 The ISBD guidelines also state that antidepressants should be avoided in BD patients with predominantly mixed states, and that previously prescribed antidepressants should be discontinued in patients currently experiencing mixed states. 23 The British Association for Psychopharmacology (BAP) 2016 guidelines state that when mixed features are present in a manic or hypomanic episode, the implications for treatment are uncertain, although ‘existing data from secondary analysis of trials for mixed episodes suggest that treatment as for mania is appropriate.’ 24 For the short-term treatment of mixed states, BAP 2016 guidelines acknowledge that the DSM-5 mixed features specifier will have implications for future trials, but they also acknowledge that, to date, very little has emerged that is of relevance to choice of treatment. 24 Consistent with ISBD guidelines, the BAP guidelines caution against either starting or continuing treatment with an antidepressant for mixed states. 24
The Canadian Network for Mood and Anxiety Treatments (CANMAT)/ISBD 2013 guidelines present some limited evidence for efficacy of antipsychotics in the treatment of mixed states in the acute setting (olanzapine, asenapine) and as maintenance therapy (olanzapine, ziprasidone, risperidone). 25 The CANMAT MDD 2016 guidelines incorporate MDD with mixed features and recommend lurasidone as first-line therapy. 26 The Florida Best Practice Psychotherapeutic Medication Guidelines 2016 were the first to recommend treatment for MDD with mixed features. 27 These guidelines recognize that there is currently a paucity of evidence for supporting treatment strategies and therefore include hierarchical levels of recommendation for treating MDD with mixed features, similar to treating MDD without mixed features. 27
Summary
Mood disorders are no longer categorized as discrete entities, but, rather, as points on a continuous spectrum. ‘Mixed features’ represents an important and understudied aspect of mood disorders, which is commonly encountered in adults with both MDD and BD. The presence of mixed features generally complicates the course of illness, reduces treatment response and worsens outcomes. The identification of MDD with mixed features is critical, since it is associated with an increased risk of suicidality and lack of response to antidepressants. There are currently no approved treatments for mixed states and only limited guidance on how mixed states should be treated, and these are generally based on post hoc analyses of studies that included patients with manic and mixed episodes.
Psychopharmacological interventions in mixed states: available evidence and clinical reality
Peter M. Haddad, Neuroscience and Psychiatry Unit, University of Manchester, UK
Aretaeus of Cappadocia first described manic–depressive illness as a single disease with two opposite constellations of symptoms. 2 At the end of the 19th century, Kraepelin and his pupil Weygandt recognized the simultaneous occurrence of manic and depressive features, and were the first to use the term ‘mixed states.’ 2 Indeed, Kraepelin regarded mixed states as the most common form of manic–depressive illness. 2 Prior to DSM-5, the importance of mixed states remained recognized clinically, but this did not translate into key diagnostic systems, which adopted a restrictive view regarding the diagnosis of mixed states. For example, DSM-IV-TR criteria for a mixed state required the simultaneous presence of full manic and depressive episodes for ⩾7 days in a person with BD-I, and anything short of meeting the full criteria for both episodes was ignored. Such an approach was not in keeping with clinical reality, since the most common presentation of mixed episodes is the presence of a few concomitant symptoms of the opposite polarity.28–33
The arrival of DSM-5 heralded a neo-Kraepelin approach. While still acknowledging that there are three key types of mood episode (mania, hypomania and major depression), DSM-5 no longer regards these as separate entities, and the presence of subthreshold symptoms of the opposite pole are recognized and captured using the mixed features specifier. 3 Importantly, this specifier can be used for manic, hypomanic and major depressive episodes. 3
Treatment of mixed states in bipolar disorder
Mixed mania has a worse clinical course than classic mania on many levels, as it is associated with an increased frequency of episodes, greater likelihood of future mixed episodes, greater likelihood of rapid cycling and episodes of longer duration, compared with classic mania. Mixed mania is also associated with greater functional impairment, increased suicidality and higher levels of comorbidity including cardiovascular disease, substance abuse (especially alcohol and cannabis), borderline personality disorder and anxiety disorders. In addition, mixed mania has a poorer response to treatment (especially to lithium) than classic mania.17,34–38
In contrast to mania and depression, there is little guidance on the efficacy of specific drug treatments for bipolar mixed states. Evidence is based on post hoc analyses of randomized controlled trials (RCTs) of second-generation antipsychotics licensed for the treatment of mania, which recruited patients with pure mania or a mixed syndrome. Most studies have addressed the acute treatment of mixed states, but some have investigated maintenance treatment.
Short-term RCTs have demonstrated that aripiprazole (a dopamine partial agonist) is efficacious in the treatment of acute manic and mixed episodes, and long-term maintenance trials have shown that it is also effective in relapse prevention in patients with recurrent manic and mixed episodes.39,40 It may therefore be useful in BD patients with mixed states, and has the added advantage of having a favorable safety and tolerability profile.40,41 Asenapine, which has a pharmacodynamic effect on several dopaminergic and serotonergic receptors, has demonstrated superiority over placebo for the treatment of manic and mixed episodes in several short-term monotherapy trials. 34 In addition, a cost-effectiveness study demonstrated that asenapine was superior to olanzapine (in terms of quality-adjusted life years) as a maintenance treatment for BD-I patients with mixed episodes. 42 A potential drawback of asenapine is that it is administered as a sublingual tablet, 43 which is unpopular with some patients. A post hoc analysis of pooled data from three placebo-controlled trials demonstrated that olanzapine was efficacious in the treatment of BD-I mania [assessed as change from baseline to week 3 in the Young Mania Rating Scale (YMRS) total score] in patients both with and without mixed features, defined by DSM-5. 44 Greatest efficacy was observed in patients with mixed features who had relatively severe depressive symptoms. 44 Quetiapine is approved for the treatment of mania, bipolar depression and the maintenance phases of BD.45,46 An 8-week study of patients with bipolar II disorder, currently experiencing mixed hypomanic symptoms, showed that quetiapine was significantly more effective than placebo in the treatment of total and depressive symptoms but that there was no difference in the treatment of hypomanic symptoms. 47 A post hoc analysis of two maintenance studies conducted in patients with stable BD-I demonstrated that quetiapine plus lithium/valproate significantly increased time to recurrence of mood events versus placebo in patients who had mixed symptoms at study entry, and time to occurrence of mixed-mood events in patients with any mood episode at study entry. 48 The efficacy of ziprasidone as monotherapy for the acute treatment of manic and mixed episodes was demonstrated in two 3-week RCTs. 49 In these trials, ziprasidone was shown to be significantly more effective than placebo in improving manic symptoms as early as day 2. 49 In addition, two 1-year open-label extension studies demonstrated that it is effective both as monotherapy and an adjunctive treatment to lithium in the prevention of manic and mixed episodes. 49 No RCTs have assessed the efficacy of risperidone in the treatment of bipolar mixed states. 34 However, risperidone has demonstrated efficacy in open-label studies in people with mixed states, particularly for the treatment of manic symptoms.50,51 Lurasidone is approved in the USA for the treatment of acute bipolar I depression and schizophrenia. 52 In Europe, it is only approved for the treatment of schizophrenia. 53 A post hoc analysis of a placebo-controlled RCT demonstrated that lurasidone is efficacious in the treatment of patients with bipolar depression with mixed features. 54
Lithium is effective in classic euphoric mania, 34 but shows a poor response in dysphoric mania.55–57 Valproate has demonstrated efficacy in pure and dysphoric mania as a monotherapy or as adjunctive treatment to a second-generation antipsychotic. 34 Although valproate may be a potentially useful treatment option for mixed mania, its use in women is severely limited by its high teratogenic potential and the risk of developmental disorders in infants exposed to it in utero. 58 Valproate should not be prescribed to women of child-bearing potential unless other treatments are ineffective or not tolerated and the woman is using effective contraception, has been made fully aware of the risks to the unborn child should she become pregnant, and has given informed consent. 59
In pooled, post hoc analysis, carbamazepine was superior to placebo in the treatment of mania and mixed states. 60 Lamotrigine has demonstrated efficacy in the acute treatment of bipolar depression 61 and also in preventing relapse of bipolar depression. 62 However, lamotrigine has not demonstrated efficacy in mixed states. 34 Other antiepileptic drugs, including topiramate, gabapentin and pregabalin, have no RCT evidence of effectiveness in mixed states or other domains of BD. 34 Antidepressants are ineffective in treating mixed bipolar depression (as well as ‘pure’ bipolar depression) and may increase manic symptoms,34,63 especially if prescribed without a mood stabilizer. 64 Electroconvulsive therapy is a potentially useful therapeutic option in refractory mixed states, but only when other options are ineffective. 65
Treatment of major depressive disorder with subsyndromal hypomania
Hypomanic symptoms commonly occur with depression, with up to 40% of MDD patients experiencing some degree of subthreshold bipolar features. 66 However, evidence for the pharmacological treatment of MDD with mixed features is limited. A 6-week RCT demonstrated that ziprasidone was significantly more effective than placebo for the treatment of acute depressive mixed states (assessed using the Montgomery–Åsberg Depression Rating Scale [MADRS]) in 73 patients with MDD or BD-II. 67 Efficacy was more pronounced in patients with BD-II versus MDD (p = 0.036). 67
In addition, one RCT assessed the efficacy of lurasidone specifically for the treatment of MDD with mixed features. 68 Patients with MDD and two or three protocol-defined manic symptoms, with no past history of mania or hypomania, were randomized to receive 6 weeks of treatment with either lurasidone 18.5–55.5 mg/day (n = 109) or placebo (n = 100). 68 At baseline, the most common ‘core’ manic symptoms were racing thoughts (66.8%) and pressured speech (61.1%). 68 There was also a high prevalence of ‘nonspecific’ manic symptoms at baseline, such as irritability (57.3%), distractibility (59.2%) and psychomotor agitation (36.5%). 68 Lurasidone was significantly superior to placebo in change from baseline in MADRS total score (the primary endpoint), with significant separation from week 1 onwards (Figure 5A). 68 Similarly, lurasidone was significantly superior to placebo on the Clinical Global Impression–Severity (CGI-S) scale, with significant separation from week 1 (Figure 5B). 68

Change from baseline in (a) Montgomery–Åsberg Depression Rating Scale total score and (b) Clinical Global Impression–Severity scale score in patients with major depressive disorder with mixed features treated with lurasidone or placebo (Mixed Model for Repeated Measures; intention-to-treat population).
The proportion of patients who were MADRS responders (defined as ⩾50% reduction from baseline in MADRS total score at week 6 for the last observation carried forward [LOCF] population) was significantly greater for lurasidone than for placebo (64.8% versus 30.0%; p < 0.001), as was the proportion of patients who were MADRS remitters (defined as MADRS total score ⩽12 at week 6 [LOCF]; 49.1% versus 23.0%; p < 0.001). 68 Lurasidone was also significantly superior to placebo on YMRS total score and Hamilton Anxiety Rating Scale-A total score. 68
Overall, lurasidone was well tolerated. 68 Only five adverse events were reported by ⩾5% of patients in either group and the only adverse events reported more frequently with lurasidone compared with placebo were nausea (6.4% versus 2.0%) and sedation/somnolence (5.5% versus 1.0%). 68 Mean changes from baseline in weight, body mass index, and levels of lipids, glucose and prolactin were low in both groups. 68 In addition, the overall rate of discontinuation was lower with lurasidone than with placebo (6.4% versus 14.7%), as was the rate of discontinuation due to adverse events (2.8% versus 4.9%). 68 This study provides evidence of efficacy, together with favorable tolerability, for a pharmacological treatment for MDD with mixed features. It is also notable that lurasidone demonstrated high effect sizes in this setting at a relatively low-dose level (the effective dose range for schizophrenia being 37–148 mg/day). 53 Further research is required to confirm the findings of this single study and to ascertain the effects of other antipsychotics in the treatment of MDD with mixed features.
Summary
Mixed states have been described as representing ‘a nosological dilemma, a diagnostic challenge and a neglected area of research.’ 69 Although this still remains the case, progress has been made. DSM-5 has heralded a move back to a Kraepelinian dimensional view of affective disorders, comprising a spectrum ranging from pure depression to pure mania. Bipolar mixed states are common, have a worse prognosis than pure manic states, and a poorer response to treatment than pure mania and depression. In terms of treatment options, evidence supports the use of several second-generation antipsychotics, valproate and electroconvulsive therapy, although combined treatment is often necessary. Importantly, the use of antidepressants for treating bipolar mixed states should be avoided. There are currently no approved treatments for MDD with mixed features; however, one RCT has demonstrated the effectiveness of lurasidone, compared with placebo, on multiple efficacy outcomes. It remains to be determined whether other antipsychotic agents could be similarly effective in patients with MDD with mixed features.
Questions and answers panel discussion
Roger S. McIntyre, Allan H. Young and Peter M. Haddad
The panel was asked whether the effectiveness of some antipsychotics in the treatment of mixed unipolar depression may indicate that this condition is in fact BD. Although there is some evidence for the efficacy of ziprasidone and lurasidone in the treatment of depressive mixed states, it was agreed by the panel that it is inappropriate to define a disorder in terms of response to treatment, since no symptoms in psychiatry are pathognomonic and individual treatments cross diagnostic boundaries. There is also some evidence in BD that suggests some first-generation antipsychotics may exacerbate depressive symptoms.70–72 For example, in a double-blind study, patients who had recently remitted from a manic episode following treatment with perphenazine in addition to a mood stabilizer (lithium, valproate, or carbamazepine) were randomized to receive perphenazine or placebo for an additional 6 months (while continuing treatment with a mood stabilizer). 70 Those who continued perphenazine treatment were more likely than those who received placebo to experience depressive symptoms and have a shorter time to depressive relapse. 70 A meta-analysis comparing five atypical antipsychotics with haloperidol for the treatment of acute mania found that the risk of switch to depression was 42% less with atypicals than with than with haloperidol. 72 The presence of hypomanic symptoms has become highly associated with BD as an unintended consequence of dividing the manic–depressive spectrum into unipolar and bipolar disorders. However, long-term data have demonstrated that a substantial proportion of MDD patients with subthreshold hypomanic symptoms maintain an MDD diagnosis over 2 years plus of follow up. 12 Hypomanic symptoms in MDD are particularly represented by arousal, hyperarousal and activation, but such symptoms do not define BD in this group.
The National Institute for Health and Care Excellence (NICE) guidelines are seen by many as the ‘pinnacle’ of evidence-based guidelines, and the speakers were asked for their opinions of the most recent NICE bipolar guidelines. NICE guidelines differ from other guidelines in being supported by more resources, conducting their own meta-analysis, and in taking input from a wide variety of stakeholders. These are clear strengths. In most areas, the recommendations of NICE are complementary to the recommendations of other guidelines for the treatment of BD. However, there are differences. In particular, psychological therapies with evidence of effectiveness in unipolar depression (specifically, cognitive behavioral therapy) were recommended by NICE for treating bipolar depression, largely on the basis of extrapolation; there is very limited evidence of their effectiveness in bipolar depression. In addition, there was inconsistency in the way in which pharmacological evidence was assessed by NICE; for example, combination therapy with lithium and valproate was recommended as an option for maintenance treatment in BD when lithium monotherapy has been ineffective, despite no clear evidence to demonstrate a benefit for combination therapy versus lithium alone. 73 Feedback regarding the contradictions and flaws of these guidelines has been presented to NICE and robustly addressed in the literature. 74
It was queried whether there is evidence linking child abuse with the occurrence of mixed features. Although there is no direct evidence of a specific link between child abuse and mixed features, the panel felt that such a link represents a ‘tenable hypothesis’, since there is clear evidence linking childhood trauma with mixed features, certain personality disorders, adult ‘flip’ disorders and poor response to treatment.75–79 Moreover, there is evidence linking childhood trauma to the development of obesity, diabetes and the metabolic syndrome in adults with unipolar depression and BD. 80 Such ‘stress phenotypes’ are known to drive the psychopathology that subserves both mania and depression, and the development of mixed features. 8
Since olanzapine/fluoxetine combination therapy has received approval in the USA for bipolar depression, the question arose as to whether there is evidence for its efficacy in mixed features. The panel was unaware of any such evidence and highlighted that a major disadvantage of olanzapine is its adverse cardiometabolic profile (particularly in terms of weight gain), which can cause major health problems over the long term.
Lurasidone has demonstrated efficacy in the treatment of depressive and hypomanic symptoms in patients with MDD or bipolar depression, and it was queried whether it is also efficacious in acute bipolar mania. Although lurasidone has not been specifically trialed for the treatment of acute bipolar mania, the panel was in agreement that it is likely to be efficacious in this setting, given that multiple D2 receptor antagonists have been trialed in mania and have consistently been shown as effective. 81
The question of treating anxiety in BD was discussed. The panel acknowledged that comorbid anxiety is very common in BD and is often difficult to treat. Evidence has shown that during a depressive episode, the severity of anxiety increases as the severity of hypomanic symptoms increases; and that during a manic episode, the severity of anxiety increases as the severity of depressive symptoms increases. Anxiety is therefore a common target across the spectrum of mania and depression, particularly when mixed features are present. Moreover, anxiety is highly associated with suicidality and a low rate of recovery and must, therefore, be treated. Pregabalin and gabapentin are not antimanic but have demonstrated anxiolytic efficacy,82,83 with pregabalin being licensed for the treatment of generalized anxiety disorder. These agents are relatively well tolerated and have few drug interactions.84,85 Moreover, they are not associated with a risk of switching (the main reason precluding the use of selective serotonin reuptake inhibitors in this setting).83,86 Although gabapentinoids may therefore be useful for treating anxiety in BD, the risk of dependence and potential misuse must be considered.87,88
Finally, recommendations regarding treatment options for adults with bipolar depression with mixed features were discussed. There is evidence for the efficacy of certain antipsychotics, namely, quetiapine and lurasidone, in the treatment of adults with bipolar depression with mixed features. 47,54 There is also evidence supporting the use of combination therapy with lamotrigine plus lithium 89 and lamotrigine plus quetiapine in this setting. 90 Acute treatment decisions should anticipate long-term physical health sequelae and priority given to treatments that are less likely to physically harm patients, particularly with regards to weight gain and metabolic disturbance. Lamotrigine and lurasidone have advantages over quetiapine in this regard. Lithium is a useful option if used long term but is associated with the risk of hypothyroidism (which may occur acutely) and long-term renal dysfunction. 91 Lithium is also associated with a risk of rapid rebound illness if treatment is stopped abruptly or adherence is poor. 92
Footnotes
Acknowledgements
Medical writing assistance was provided by John Scopes of mXm Medical Communications, Tonbridge, UK.
Funding
The authors disclosed receipt of the following financial support for the research, authorship and/or publication of this article: The symposium was organized and funded by Sumitomo Dainippon Pharma and Sunovion Pharmaceuticals. Medical writing assistance was funded by Sunovion Pharmaceuticals.
Conflict of interest statement
The authors declared the following potential conflicts of interest with respect to the research, authorship and/or publication of this article:
Roger McIntyre has received advisory board and speaker fees from Lundbeck, Pfizer, AstraZeneca, Eli-Lilly, Janssen Ortho, Purdue Pharma, Johnson & Johnson, Moksha8 Pharmaceuticals, Sunovion, Mitsubishi, Takeda, Forest Laboratories, Otsuka, Bristol-Myers Squibb and Shire; research grants from Lundbeck, Janssen Ortho, Shire, Purdue, AstraZeneca, Pfizer, Otsuka and Allergan; and research grants or nonprofit funds from the Stanley Medical Research Institute.
Allan Young is employed by the Centre for Affective Disorders, Institute of Psychiatry, Psychology and Neuroscience, King’s College London, and is an Honorary Consultant at the Maudsley Hospital (NHS, UK). He has received advisory board and speaker fees from Allergan, AstraZeneca, Bionomics, BrainCells Inc., Bristol-Myers Squibb, Eli Lilly, GlaxoSmithKline, Janssen, Lundbeck, Novartis, Otsuka Pharma-ceutical Co., Pharmaceutica, Pfizer, Roche, Sanofi-Aventis, Servier Laboratories, Sunovion and Wyeth. He has no shareholdings in pharmaceutical companies. He was lead investigator for the Embolden Study (AstraZeneca), BCI Neuroplasticity Study and Aripiprazole Mania Study, and has been involved in investigator-initiated studies for AstraZeneca, Eli Lilly and Wyeth. He has received grant funding (past and present) from NIMH (USA), CIHR (Canada), NARSAD (USA), Stanley Medical Research Institute (USA), MRC (UK), Wellcome Trust (UK), Royal College of Physicians (Edinburgh), BMA (UK), VGH & UBC Foundation (Canada), WEDC (Canada), CCS Depression Research Fund (Canada) and MSFHR (Canada).
In the last 3 years, Peter Haddad has received payment for lecturing and/or consultancy from pharmaceutical companies including Allergan, Galen, Janssen, Lilly, Lundbeck, NewBridge Pharmaceutical, Otsuka, Quantum Pharma-ceuticals, Servier, Sunovion, Takeda and Teva. He has also received industry sponsorship to attend educational meetings.
