Abstract
Secukinumab is an IL-17A antagonist that has proven efficacy in the treatment of patients with ankylosing spondylitis (AS) and psoriatic arthritis. Side effects of the drug include infections, skin rashes, and allergic reactions. Raynaud’s phenomenon (RP), a vasospastic syndrome and an important feature of different connective tissue diseases, is not an expected finding in AS patients. This article reports the development of secukinumab-related RP in a 35-year-old female patient with AS. Treatment with secukinumab was continued and RP was treated with low-dose aspirin and a calcium-channel blocker.
Introduction
Ankylosing spondylitis (AS) is a chronic inflammatory disease characterized by spinal and sacroiliac joint involvement. 1 It usually affects men at a young age, presenting with inflammatory back pain and morning stiffness. The first biological drugs with proven efficacy and safety for use with AS patients were anti-TNF-alpha antagonists. 2 Recently, the efficacy of anti-IL17A (secukinumab), another biological drug, has been demonstrated. 3 Secukinumab is a recombinant, high-affinity, human monoclonal antibody of the immunoglobulin G1/κ isotype that selectively binds to and neutralizes interleukin (IL)-17A. 4 Studies have shown that secukinumab is an effective treatment option for active AS and psoriatic arthritis patients. 5 However, accounts from clinical experience regarding the safety of this drug are lacking. The most frequently reported side effects are upper respiratory tract infection, herpes labialis, and diarrhea. Raynaud’s phenomenon (RP) is a well-defined clinical syndrome characterized by recurrent digital vasospasm triggered by exposure to chemical or emotional stress. 6 It is characterized by three unique color changes (pallor, cyanosis, and erythema) and may lead to ischemia and necrosis of the involved digits. 7 RP is classified as primary (as an isolated condition) or secondary (associated with an underlying disease). Secondary RP is most frequently associated with connective tissue diseases including systemic sclerosis, lupus, and Sjögren’s syndrome; it is not an expected finding in patients diagnosed with AS. Herein, we report the development of secukinumab-related RP in a 35-year-old female patient with AS.
Case report
In 2019, a 35-year-old female patient was referred to our rheumatology outpatient clinic with complaints of inflammatory lower back and hip pain and morning stiffness. Approximately 8 years earlier, she had been diagnosed with AS and received treatment in the form of medications including NSAIDs, leflunomide, and methotrexate. In 2016, anti-TNF-alpha drugs also were prescribed but resulted in no improvement of symptoms. In the year prior to her arrival at our clinic, treatment had consisted solely of NSAIDs and exercise.
At the time of physical examination, bilateral Flexion Abduction External Rotation (FABERE)Flexion Adduction Internal Rotation (FADIR) and sacroiliac joints compression tests were positive. The results of anthropometric measurement included hand–ground distance: 12 cm, occiput–wall distance: 2 cm, Shröber test: 3 cm, and chest expansion: 3 cm. Disease activity parameters (Bath Ankylosing Spondylitis Disease Activity Index (BASDAI): 8 cm, Bath Ankylosing Spondylitis Functional Index (BASFI): 6 cm) were found to be high. Laboratory tests revealed an erythrocyte sedimentation rate (ESR) of 54 mm/h (normal 0–20 mm/h), a C-reactive protein (CRP) rate of 15 mg/dl (normal 0–5 mg/dl), and a complete blood count compatible with chronic disease anemia; liver and kidney function tests and urinalysis were found to be normal. HLA-B27 was positive. Abdominal ultrasonography and chest X-ray were normal. Bilateral chronic sacroiliitis was evaluated as stage 2 on X-ray. Cervical, thoracic, and lumbar radiographs showed joint space narrowing and syndesmophytes. A sacroiliac joints MRI revealed bilateral chronic sacroiliitis and bone marrow edema in favor of active sacroiliitis. These clinical, laboratory, and radiological findings confirmed AS disease activation. Anti-TNF-alpha treatment was not considered as she had experienced no benefit from it previously. The anti-IL17A drug secukinumab was started according to standard AS protocol. In the third month of the treatment, the patient came to the control visit. While she reported significant regression of subjective complaints such as back/hip pain, and morning stiffness, within hours of receiving secukinumab, she also reported having experienced changes in the color (pallor, cyanosis, and erythema) of the fingers of both hands for a duration of 1 or 2 days. She said she had never experienced such symptoms before and that they had only occurred following the injection of secukinumab. Inspection revealed RP in the fingers of both hands (Figure 1). In the control laboratory tests, ESR: 13 mm/h and CRP: 1.5 mg/dl were detected. To explain the RP, other underlying pathologies were questioned and examined. Upon serological testing, rheumatoid factor, antinuclear antibody, extractable nuclear antigens, anticyclic citrullinated peptide antibody, antineutrophil cytoplasmic antibody, complement C3/C4, lupus anticoagulant, and anticardiolipin antibodies all were found to be negative. Both an upper extremity arterial system doppler ultrasonography and echocardiography were normal. In the absence of any underlying pathology and its occurrence only after secukinumab injection, it was determined to be secukinumab-related RP. Despite RP, the patient continued to receive secukinumab because of the significant regression of disease activity and the lack of an alternative drug choice. With low-dose aspirin and calcium channel blockers the severity and duration of RP were decreased, and symptoms brought under control. The patient’s general condition remains satisfactory and outpatient clinic follow-up continues.
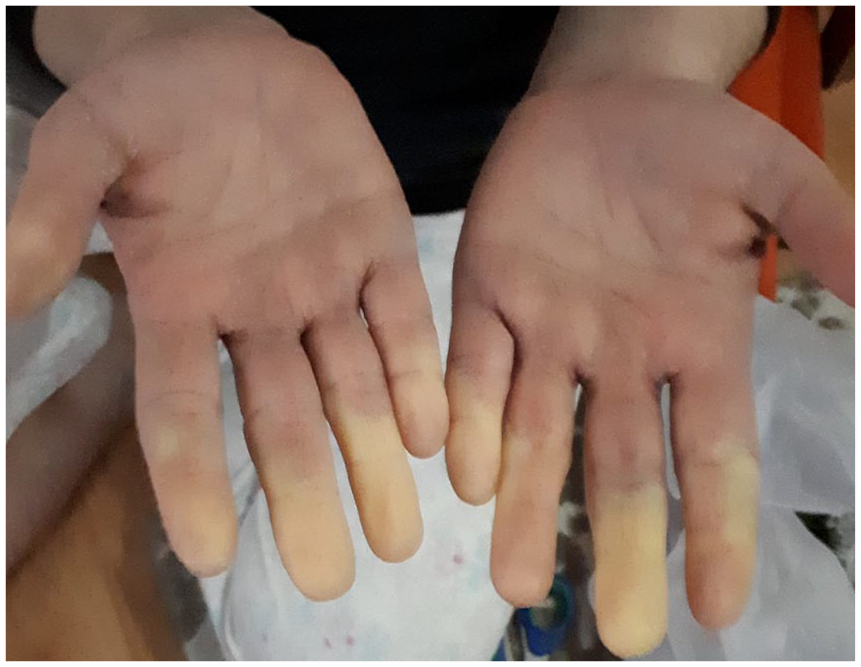
Raynaud’s phenomenon (three color changes) of the hand after secukinumab injection.
Discussion
This case of secukinumab-related RP in an active AS patient is the first to be reported in the literature. Because AS is a prototype of spondylarthritis, characterized by inflammatory lower back pain, enthesitis, and anterior uveitis, RP is not an expected finding. RP is a vasospastic syndrome more common in connective tissue diseases (scleroderma, lupus) and some types of vasculitis. The pathogenesis of RP has yet to be fully elucidated and whether autoantibodies have a role in RP remains unknown. While primary RP is usually a benign condition, secondary RP may be complicated by acral digital ulcers and gangrene, which may require medical and surgical treatment. 8 Although the mechanisms by which secukinumab causes RP are unknown, it may be speculated that the direct drug-induced vasospastic effect, binding of lymphocytes to endothelial cells, increased growth factor in fibroblastic endothelial cells, proliferation of these cells, and development of angiogenesis may be among them. 9 Simon and colleagues showed that lower levels of IL-17A are associated with a higher risk of vascular disorders. 10 In addition, the inhibition of IL-17A by the monoclonal antibody secukinumab results in an unexpected increase in the incidence of stroke and myocardial infarction compared with placebo. The authors conclude that despite sample size limitations, higher levels of IL-17A and less heart injury may have a protective effect of IL-17A on the vascular system. Drug-related RP development is reported in the literature. 11 The most commonly reported causes of RP are beta-blockers and chemotherapeutic drugs, while disease-modifying antirheumatic drugs (DMARDs) such as sulfasalazine and leflunomide are also reported (Table 1). Although the mechanisms of drug-related RP are unclear, increased vascular tone and sympathetic activation may be associated with endothelial dysfunction, neurotoxicity, or increased platelet aggregation. The identification and suspicion of drug-related symptoms are important clinically. In mild RP cases, discontinuation of the drug is sufficient with rapid improvement of symptoms. In severe cases, vascular ischemia, digital infarction, and necrosis may develop, requiring aggressive treatment. 12 In cases with drug-associated RP, a risk–benefit ratio assessment should be performed to determine whether or not to continue with the drug.
Most frequently reported drugs causing Raynaud’s phenomenon in the literature.

In conclusion, the present study reports secukinumab-associated RP in an AS patient for the first time in the literature. RP should be questioned before starting the drug and, if available, alternative therapies that do not alter peripheral blood flow should be considered. Patients receiving secukinumab should be monitored carefully and symptoms treated upon presentation. Further studies are needed to ascertain the prevalence and severity of the treatment of RP with secukinumab in AS patients.
Footnotes
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Conflict of interest statement
The author declares that there is no conflict of interest.
Statement on ethics approval
Ethics approval is not required for case reports at our institution.
Statement on informed consent
The author confirms that the patient provided written informed consent for the use and disclosure of their information in the present manuscript.
