Abstract
Metabolic (dysfunction)-associated fatty liver disease (MAFLD) is the most common chronic liver disease worldwide – with an estimated global prevalence of 37%. Different from nonalcoholic fatty liver disease (NAFLD), which is an exclusion diagnosis, MAFLD is defined by a set of positive criteria. This recent change in terminology is challenging because MAFLD and NAFLD denote two similar, albeit not identical, clinical populations. When the diagnostic criteria for MAFLD are applied, liver histology appears more severe and clinical outcomes are less favorable. However, the clinical management of MAFLD and NAFLD remains similar. While liver biopsy is still the reference standard for achieving a final diagnosis, noninvasive imaging- or biomarker-based diagnostic modalities are currently gaining momentum. However, liver biopsy should be recommended when diagnostic challenges exist. In this review, we compared the epidemiology, natural history, and diagnosis of MAFLD with respect to the traditional NAFLD definition.
Keywords
Introduction
Nonalcoholic fatty liver disease (NAFLD) – which is defined as deposition of fat in at least 5% of hepatocytes – encompasses a disease spectrum ranging from nonalcoholic fatty liver (NAFL) to cirrhosis. NAFLD is a diagnosis of exclusion that requires the absence of secondary causes of hepatic steatosis (e.g. alcohol consumption, use of steatogenic drugs, drug abuse, and autoimmune liver disease).
1
After the introduction of the acronym NAFLD by Ludwig in 1980,
2
there has been a continuing debate as to whether this terminology obscures – rather than illuminates – the real etiology of the disease. In recent years, it has been contended that the term NAFLD suffers from major shortcomings – including (1) an overestimation of the lack of alcohol consumption in the pathogenesis of the disease and (2) the neglected role of metabolic factors in disease etiology.3,4 This has prompted significant efforts for rebranding the disease in a more meaningful manner. In 2020, Eslam
The proposal of rebranding NAFLD as MAFLD has sparked a fierce scientific debate as to the most appropriate acronym. The new terminology has been combated by some hepatologists who contended that a lack of information regarding disease etiology was anticipated to have negative effects on drug development.
7
While the acronym NAFLD has not been abandoned yet, an increasing number of recent clinical studies have applied the positive definition of MAFLD and, in some cases, compared the findings with those obtained with the traditional exclusion diagnosis of NAFLD. A consistent finding is that, despite a large overlap, MAFLD and NAFLD do not define the same condition and should not be regarded as synonym.8,9 In this regard, a recent meta-analysis has shown that only 4% of the population under scrutiny was either MAFLD or NAFLD.
10
Starting from these premises, we designed the current review to compare the epidemiology, natural history, and diagnosis of MAFLD
Epidemiology
General prevalence and characteristics of MAFLD versus NAFLD
According to 2015 data,
11
the estimated global prevalence of NAFLD was approximately 25%. However, 95% of the study population included in this meta-analysis was from North America, and the diagnosis of hepatic steatosis relied on imaging modalities. On identifying NAFLD based on blood tests, the estimated prevalence appeared significantly lower.
11
A more recent meta-analysis by Chan
Comparison of MAFLD and NAFLD.
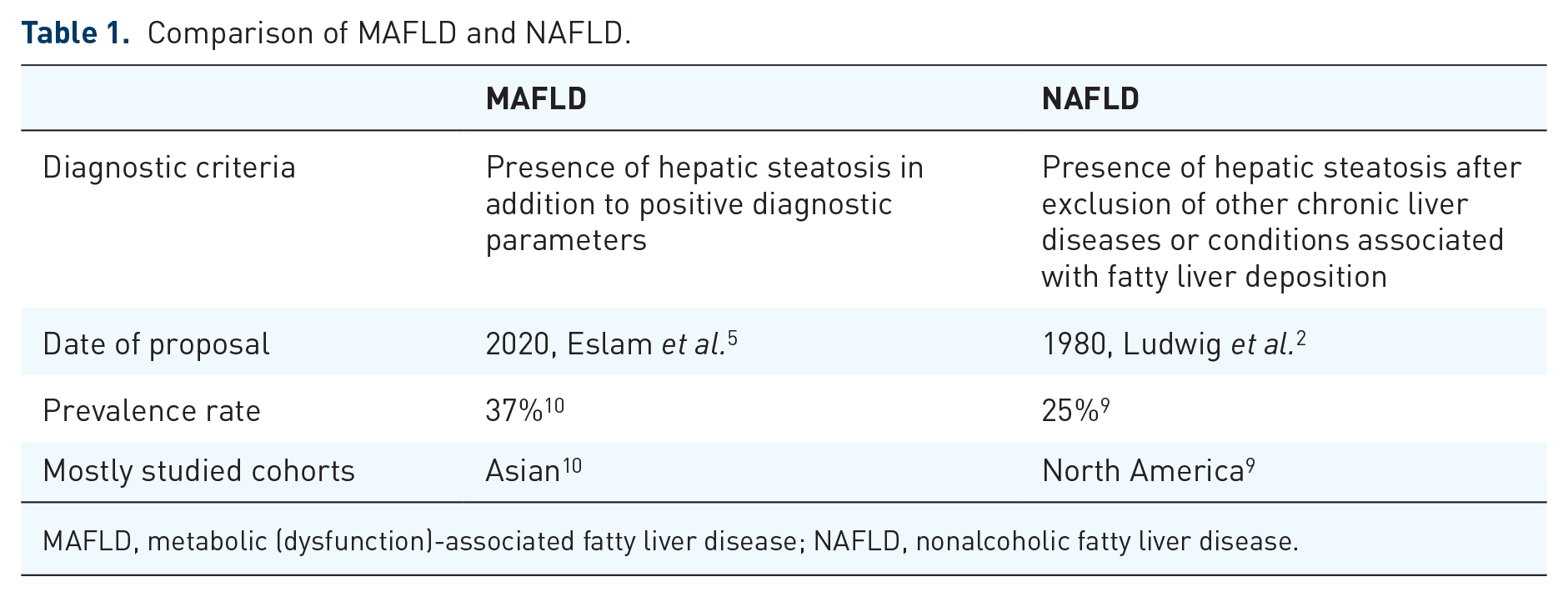
MAFLD, metabolic (dysfunction)-associated fatty liver disease; NAFLD, nonalcoholic fatty liver disease.
On analyzing the prevalence of MAFLD in overweight and obese individuals, Liu
Lin
In another study that relied on NHANES-III data,
17
MAFLD was associated with a 17% increased risk of all-cause mortality [hazard ratio (HR): 1.17; 95% confidence interval (CI): 1.04−1.32], whereas NAFLD was not (HR: 1.05; 95% CI: 0.95–1.17). Interestingly, MAFLD – but not NAFLD – was an independent risk factor for overall mortality even after adjusting for metabolic risk factors.
17
This has been recently confirmed by Nguyen
The recent change in nomenclature has been endorsed by several different stakeholders.
19
Of note, the positive definition of MAFLD has reduced patient confusion on disease etiology, ultimately facilitating both awareness and patient-physician communication.
3
In addition, the new terminology has emerged as an important tool for reducing stigmatization caused by the association of NAFLD with alcohol consumption.
20
Using a 25-item survey, Fouad
Current world data
Current knowledge concerning the prevalence of MAFLD is mainly informed by Asian studies. On examining 1016 Chinese patients using magnetic resonance imaging proton density fat fraction (MRI-PDFF), Wong
In a nationwide study carried out in 6775 subjects in South Korea, Kim
Fujii
A similar prevalence of MAFLD has been reported in Iran. Taheri
On analyzing a total of 909 patients, a multicenter study from Turkey reported that the prevalence of MAFLD was 45.5%. Notably, the enrolment involved patients with a history of dyspepsia but without known hepatic steatosis. The study cohort was therefore reflective of the general Turkish population. The prevalence rates of obesity, T2DM, metabolic syndrome, dyslipidemia, and hypertension in the study participants were 43.3%, 24.9%, 52.5%, 92.3%, and 31.9%, respectively.
31
In another Turkish study focusing on biopsy-proven MAFLD (
Baratta
Currently, data from African countries remain limited. Van Dijk
In 2012, the Australian Diabetes, Obesity, and Lifestyle study included 4747 Australian adults aged between 34 and 97 years who were considered representative of the general population.
35
The authors found that 37% of the study participants met the criteria for MAFLD; among them, the BARD score ruled out advanced fibrosis in 38% of cases. The main independent risk factors for a diagnosis of MAFLD were advanced age, male sex, T2DM, lower high-density lipoprotein (HDL) cholesterol levels, a high diastolic blood pressure, and a sedentary lifestyle.
35
On analyzing an Australian regional cohort, Kemp
Finally, a study conducted in the general population of Mexico examined 585 volunteers who had undergone laboratory tests, liver ultrasound, transient elastography, and calculation of FIB-4 index. 37 The diagnostic criteria for MAFLD were met by 41% of the study participants. In addition, the prevalence of advanced fibrosis was as high as 40%, that is, markedly above that reported for the world’s general population. 37
Incidence
Published data concerning the incidence of MAFLD remain scarce and mainly limited to Asian countries. Wong
Natural history
Patients with NAFLD show a stepwise increase in mortality rates according to the fibrosis stage;
41
therefore, the severity of hepatic fibrosis is currently recognized as the main prognostic determinant in this clinical entity. On analyzing 1773 adult patients with biopsy-proven NAFLD, Sanyal
MAFLD is a multisystemic disease in which a wide variety of extra-hepatic manifestations – including cardiovascular disease, chronic kidney disease, and extrahepatic malignancies – can occur. In addition, epidemiological evidence for a possible comorbidity between NAFLD and an impaired cognitive function has been reported.
45
Adverse cardiovascular events represent the leading cause of death in patients with MAFLD, followed by extra-hepatic malignancies and liver-related complications.
46
The MAFLD definition seems to outperform NAFLD in terms of identifying patients at high risk of extra-hepatic manifestations. For example, the NHANES-III (1988−1994) study revealed that MAFLD identified chronic kidney disease (CKD) in 29.60% of the participants compared with 26.56% when the traditional NAFLD criteria were used.
47
On analyzing an independent cohort of 27,371 subjects, Hashimoto
The association between both MAFLD and NAFLD with adverse cardiovascular outcomes is well established.39,49 In a large nationwide study, Lee
There is also evidence indicating that the extent of lung impairment is higher in MAFLD than in NAFLD. On analyzing 2543 middle-aged individuals recruited from 25 communities across four cities in China, Miao
Finally, colorectal malignancies are prevalent in patients with MAFLD.
53
Interestingly, their burden has been associated with the severity of both MAFLD and NAFLD.
54
In a multicenter retrospective study, Fukunaga
Diagnosis
Figure 1 depicts the current diagnostic algorithm for MAFLD. 5 In general, the diagnostic process relies on the detection of hepatic steatosis using noninvasive blood tests, imaging modalities, or liver histology. According to the Asian Pacific Association for the Study of the Liver, 56 screening of MAFLD with abdominal ultrasonography is recommended for patients with overweight/obesity, T2DM, and metabolic syndrome. However, the diagnosis of hepatic steatosis can be incidental. The detection and staging of liver fibrosis is also paramount for risk stratification. In the next sections, we will discuss the current diagnostic options for detecting MAFLD.

Diagnostic workflow for MAFLD.
Noninvasive blood tests
FLI is a common diagnostic algorithm for hepatic steatosis that includes BMI, waist circumference, triglycerides, and gamma-glutamyl transferase. An FLI < 30 can confidently rule out the presence of fatty liver, whereas an FLI > 60 denotes a high probability of steatosis. 57 Other less commonly used algorithms include the hepatic steatosis index, 58 SteatoTest, 59 lipid accumulation product, 60 NASH index, 61 NAFLD liver fat score, 62 triglyceride-glucose index, 63 serum keratin-18 fragments, 64 and the visceral adiposity index. 65 The utility of FLI for MAFLD screening has been recently validated in the NHANES III population where hepatic steatosis was identified by ultrasonography. 66 The results revealed a satisfactory performance of FLI (area under curve = 0.793; negative predictive value = 77%) in the detection of MAFLD. 66
As for the noninvasive screening of hepatic fibrosis, several blood-based panels have been proposed. The American Association for the Study of Liver Diseases and the European Association for the Study of the Liver recommended the use of the FIB-4 and the NFS for the screening of advanced fibrosis in patients with NAFLD.1,67 More recently, the Asian Pacific Association for the Study of the Liver maintained the same approach for MAFLD.
57
Other panels – including the alanine transaminase-to-platelet ratio index (APRI) and BARD – have been widely used for the screening of significant and advanced fibrosis.68,69 It is generally accepted that FIB-4 and NFS are superior to APRI and BARD in both MAFLD and NAFLD populations.70–73 On analyzing a cohort of 417 patients with biopsy-proven MAFLD, Wu
Although the use of FIB-4 and NFS should be preferred over other panels for the screening of advanced fibrosis, their application in patients with MAFLD is not without limitations. First, their main clinical utility lies in their ability to exclude – rather than identify – advanced fibrosis.
74
Second, age may significantly affect the diagnostic accuracy of both FIB-4 and NFS. In this regard, McPherson
Several more complex panels – including the enhanced liver fibrosis test (ELF), FibroMeter, FibroTest, and ADAPT (age, presence of diabetes, procollagen C3, and platelet count) – have been recently proposed for the detection of hepatic fibrosis.80–82 Of them, ADAPT has been validated according to the MAFLD diagnostic criteria and was found to outperform FIB-4, NFS, APRI, and BARD. 83 The stepwise use of ADAPT followed by liver stiffness measurement (LSM) with transient elastography resulted in a negative predictive value close to 100%. 83 Therefore, this diagnostic algorithm holds promise to reduce the number of liver biopsies. Similarly, it has been recently reported that the combined used of FIB-4 and ELF may result in 85% reduction of referrals to tertiary care centers. 84
Imaging modalities
Owing to its noninvasive nature, widespread availability, and low costs, abdominal ultrasonography remains the most extensively used imaging modality for the identification of hepatic steatosis. 85 However, its clinical usefulness for the detection of mild-to-moderate steatosis (<30%) is limited, and more sensitive methods – including controlled attenuation parameter (CAP) obtained from transient elastography86,87 – have been developed. Notably, the determination of CAP in obese individuals is feasible but requires the use of a specific XL probe.88,89 Currently, MRI-PDFF remains the reference standard for quantification of liver fat using imaging modalities; therefore, it has been extensively used as an endpoint in clinical trials. 90
As for the imaging detection of hepatic fibrosis, the use of LSM obtained from transient elastography is gaining momentum.91,92 Currently, FibroScan is recommended as a second-level diagnostic modality93,94 for patients deemed at indeterminate or high risk of advanced fibrosis based on FIB-4 scores (i.e. values ⩾1.3).95,96 A feasible diagnostic workflow for hepatic fibrosis is presented in Figure 2. Finally, magnetic resonance elastography is a highly accurate imaging modality for the assessment of liver fibrosis. Unfortunately, its high costs and poor availability have significantly limited its routine clinical use. 97

Diagnostic workflow for hepatic fibrosis in MAFLD.
Liver biopsy
In light of the continuous nature of hepatic inflammation, the definition of MAFLD avoids the traditional dichotomous classification of NASH
Conclusion
The recent rebranding of NAFLD to MAFLD has prompted research efforts to compare the two conditions with respect to a number of aspects. While large overlaps exist between the MAFLD and NAFLD populations, it is clear that the two terms do not denote the same clinical entity. In addition, although the diagnostic modalities remain similar, the two acronyms should not be used interchangeably. Notably, growing evidence indicates that patients with MAFLD tend to have less favorable outcomes than those with NAFLD.
