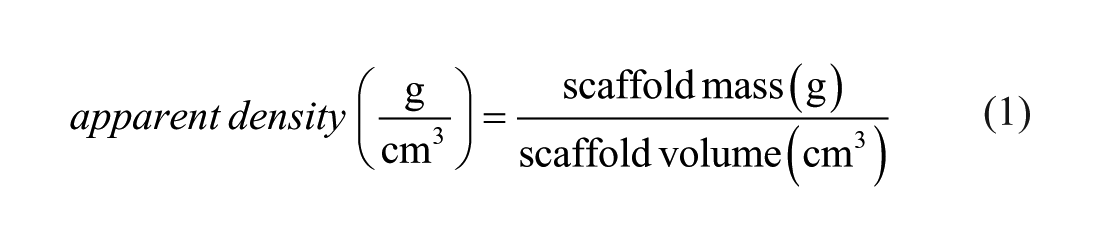Abstract
Reconstruction of the human auricle remains a challenge to plastic surgeons, and current approaches are not ideal. Tissue engineering provides a promising alternative. This study aims to evaluate the chondrogenic potential of bone marrow–derived mesenchymal stem cells on a novel, auricular-shaped polymer. The proposed polyhedral oligomeric silsesquioxane-modified poly(hexanolactone/carbonate)urethane/urea nanocomposite polymer has already been transplanted in patients as the world’s first synthetic trachea, tear duct and vascular bypass graft. The nanocomposite scaffold was fabricated via a coagulation/salt-leaching method and shaped into an auricle. Adult bone marrow–derived mesenchymal stem cells were isolated, cultured and seeded onto the scaffold. On day 21, samples were sent for scanning electron microscopy, histology and immunofluorescence to assess for neocartilage formation. Cell viability assay confirmed cytocompatability and normal patterns of cellular growth at 7, 14 and 21 days after culture. This study demonstrates the potential of a novel polyhedral oligomeric silsesquioxane-modified poly(hexanolactone/carbonate)urethane/urea scaffold for culturing bone marrow–derived mesenchymal stem cells in chondrogenic medium to produce an auricular-shaped construct. This is supported by scanning electron microscopy, histological and immunofluorescence analysis revealing markers of chondrogenesis including collagen type II, SOX-9, glycosaminoglycan and elastin. To the best of our knowledge, this is the first report of stem cell application on an auricular-shaped scaffold for tissue engineering purposes. Although many obstacles remain in producing a functional auricle, this is a promising step forward.
Introduction
Reconstructive surgery of the entire external ear remains one of the greatest challenges for the plastic surgeon. 1 The principal pathologies requiring ear reconstructive surgery include resection following malignancy, microtia/anotia (a congenital deformity of the pinna whereby it is either underdeveloped or absent) and trauma. The poor mitotic activity of chondrocytes and their avascular nature results in a limited regenerative capacity. 2 The ideal situation would be to have a readily available ‘bespoke’ auricle, which is aesthetically identical to the contralateral ear and shows long-term durability.
The current gold standard treatment for total auricular reconstruction involves a surgical procedure, whereby the surgeon hand-carves autologous costal cartilage into the shape of the auricle. Unfortunately, although results can be reasonable, this technique is highly dependent upon the skill of the surgeon, and donor-site morbidity is significant. 3
Alloplastic implants, most commonly porous polyethylene, Medpor®, have the advantage of being widely available, requiring a shortened operation time and maintaining a predetermined shape. 4 There are limitations on their use however, namely, risk of infection, long-term durability and extrusion. A tissue engineering approach can create structurally stable auricles that are far superior in matching the native ear with regard to functionality and aesthetics than the current treatment options.
Autologous chondrocytes, both xenogenic and human, are a sensible choice of cell source for the tissue-engineered auricle.5–8 Approximately 10 × 107 cells are required to seed an adult-size auricle; however, chondrocytes tend to replicate slowly and therefore need to be expanded in vitro. 9 Furthermore, chondrocytes are prone to de-differentiation, whereby they lose their phenotype resulting in inferior cartilage. 10 What appears to be a recurring theme, however, is that the tissue-engineered auricles tend not to maintain their size and shape, lack flexibility (due to less elastin and collagen type II content) and we have not seen success in the immunocompetent animal model.
Currently, despite some positive work with stem cells and cartilage tissue engineering,11–13 there has been no report in the literature of a tissue-engineered auricle using stem cells. Mesenchymal stem cells (MSCs) have the ability to differentiate into osteoblasts, adipocytes and chondrocytes. Their isolation from bone marrow is widely documented, and small cell numbers are sufficient for preliminary tissue culture. 14 Problems arise with stem cell culture as, due to the fact that they are poorly understood, it can be difficult to direct them to a particular differentiation pathway. Furthermore, uncontrolled proliferation may result in tumour formation. 15 Several studies have shown that bone marrow–derived mesenchymal stem cells (BMSCs) clearly have the potential of forming neocartilage in a three-dimensional (3-D) environment.16–18 More recently, a group has shown that BMSCs produced a greater yield of higher quality neocartilage in cartilage defects in rabbits, compared to MSCs derived from adipose tissue, periosteum and muscle. 19 Despite the lack of work with stem cells and auricular scaffolds, polylactic-co-glycolic acid (PLGA) scaffolds (shaped as human nasal alar cartilage) seeded with rabbit BMSCs revealed evidence of neocartilage formation at 4 weeks. 20
Several factors have been employed in auricular tissue engineering to improve cell yield. There is considerable evidence to suggest that growth factors, either in the chondrogenic media or incorporated into the scaffold itself, enhances neocartilage formation. Inducers such as dexamethasone and tissue growth factor–β3 (TGF-β3) have been shown to be vital for cell proliferation, survival and chondrogenesis. 21 Bioreactors, both spinner and rotating, have been shown to increase the yield of neocartilage formation within a reduced time period.7,22
Choosing the right scaffold from which the auricle is to be constructed is crucial. Scaffolds may be entirely synthetic, biological or a combination of the two. 23 The scaffold should be non-toxic, maintain cell phenotype, allow good cell adherence and have an appropriate degradation rate while retaining mechanical strength. However, it is essential that the polymer is pliable enough to be carved into an intricately shaped auricle. Finally, the polymer of choice has to be cost-effective and easily available for widespread use.
The great advantage with synthetic polymers is that their chemical and physical properties may be modified in order to provide the optimum scaffold for cells. Their mechanical strength is also an advantage over their biological counterparts. Of the synthetic polymers, those derived from poly(α-hydroxy esters) have been most commonly used and have supported neocartilage formation. 7 However, a cytokine-led inflammatory reaction with considerable loss of construct shape and size has been documented in various studies where an immunocompetent model is used.7,24
By incorporating polyhedral oligomeric silsesquioxane nanocages with poly(carbonate urethane) (polyhedral oligomeric silsesquioxane-modified poly(hexanolactone/carbonate)urethane/urea (POSS-PCU)), our research group has developed a novel, non-biodegradable polymer. Prior studies have shown excellent cell compatibility (including with stem cells), antithrombogenic properties and durability.25–27 As a consequence, a reduced inflammatory response has been noted. Furthermore, the nanocage structure of POSS-PCU is said to impart strength to the polymer which is essential for tissue engineering purposes. Very recently, the world’s first entirely synthetic trachea composed of POSS-PCU and the patients’ own stem cells, designed by our group, was successfully transplanted at the Karolinska University Hospital in Sweden. 28 The patient is currently doing well. Further to this application, POSS-PCU has shown promise in lacrimal duct conduits and bypass grafts.29,30
The aim of this study was to create a POSS-PCU adult-size auricular construct and characterise this polymer in terms of porosity, pore size, morphology and tensile strength. Once seeded with BMSCs, chondrogenesis was evaluated using scanning electron microscopy (SEM), histology and immunofluorescence.
Materials and methods
Nanocomposite polymer synthesis
In order to form 2% POSS-PCU (i.e. concentration of POSS nanocage particle incorporated into the PCU scaffold), the protocol described in the patent was strictly adhered to Seifalian et al. 31 Briefly, polycarbonate polyol, 1000 mwt, and trans-cyclohexanechloroydrinisobutyl-silsesquioxane were placed in a 1000-mL reaction flask equipped with mechanical stirrer and nitrogen inlet. For the POSS cage to dissolve into the polyol, the mixture required heating followed by cooling. Flake 4,4′-methylenebis(phenyl isocyanate) (MDI) was added to the polyol blend and reacted, under nitrogen, for 5 min to form a pre-polymer. Subsequently, dimethylacetamide (DMAC) was added slowly to this pre-polymer in order to form a solution. Chain extension of the pre-polymer was carried out by the drop-wise addition of a mixture of ethylenediamine and diethylamine in DMAC to form a solution of POSS-PCU in DMAC. All reagents and chemicals were purchased from Sigma Aldrich (Gillingham, Dorset, UK).
Fabrication of porous auricular polymeric scaffold
The ear mould was based upon an adult human auricle with dimensions of approximately 7 cm × 4 cm. The negative mould, constructed from glass material (Glossary Co., London, UK) based on 3-D imaging, acted as a rigid cast in which the POSS-PCU polymer was added for shaping.
Auricular scaffolds (n = 3) were made by mixing porogen leaching with a coagulation method. Sodium chloride (NaCl) was dissolved in an 18 wt% solution of POSS-PCU in DMAC containing Tween 80 surfactant. Prior to this, the salt particles were sieved using stainless steel sieves (Fisher Scientific, Loughborough, UK) in order to achieve an average particle size of 200–300 µm. A viscous slurry of NaCl/POSS-PCU was produced by dispersing and degassing the mixture using a Thinky ARE 250 mixer (Intertonics, Kidlington, UK). The weight ratio of NaCl to POSS-PCU was controlled at 3:2.
The NaCl/POSS-PCU slurry was then cast onto the negative auricular glass mould and placed in distilled water for an initial period of 24 h. This process resulted in a formation of porous auricular scaffold via DMAC exchange with distilled water and leaching of NaCl. The auricular scaffold was then removed from the negative glass mould (when it retained precisely the complex contour of the auricle) and immersed in deionised water for a further 72 h to ensure complete removal of the remaining solvent and porogen (not confirmed experimentally). The resultant 3-D auricular scaffold was then trimmed into the shape of the positive mould using a surgical scalpel, air dried for 48 h and autoclaved for all experimental work. Mechanical characterisation was also conducted on POSS-PCU sheets fabricated in a similar method described above (n = 4).
Auricular nanocomposite scaffold characterisation
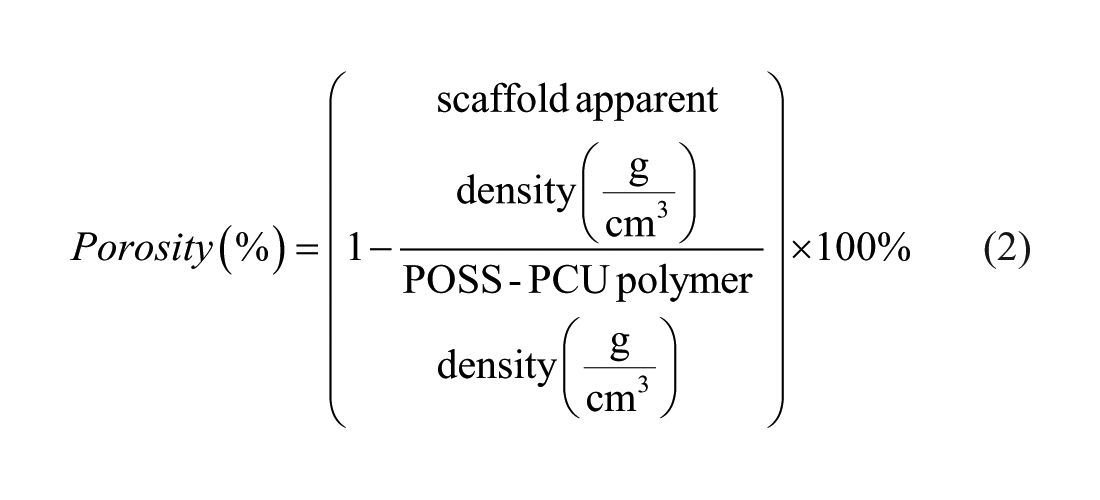
The average porosity of the POSS-PCU auricular scaffolds was calculated using specific equations below
We have assumed that the bulk density of our polymer is 1.15 g/cm3 (from previous work in our laboratory). 31 The porosity is expressed as a percentage.
Furthermore, surfaces and cross-sections of the synthesised auricular polymers were evaluated under SEM to assess pore size, shape and distribution. Briefly, the sample was post-fixed using 1% osmium tetroxide (Merck, Nottingham, UK) and washed with distilled water. Subsequently, the sample was dehydrated at room temperature in a series of graded acetone solutions. Following dehydration, the sample was transferred to tetramethylsilane for 5 min and then allowed to air dry. The sample was attached to aluminium stubs and coated with gold using a sputter coater (SC500 EM Scope) prior to SEM examination (Philips 501, Amsterdam, Netherlands). The samples were observed at different magnifications at 25 kV and analysed through ImageTool software for measurement of scaffold pore size.
Assessment of the elastic properties of the polymer was conducted using an Instron-5565 tensile tester (Instron, High Wycombe, UK). This was under uniaxial tension with dumbbell shaped specimens of dimension 20 mm × 4 mm (n = 5). Loading speed was set at 50 mm/min. Once subjected to a preload of 0.5 mN, data were collected as Young’s modulus, maximum tensile strength and elongation at break (with a stretching ratio of 25%).
Evaluation of chondrogenesis on auricular scaffold
BMSC isolation and culture
Bone marrow was harvested from the iliac crest of healthy adult donors (for allogenic transplant of haematological malignancy at the Royal Free Hospital, London, UK). Mononuclear cells were separated from the bone marrow sample by light density enrichment using lymphoprep (Axis-Shield, Dundee, UK). After two washes in phosphate-buffered saline (PBS), the mononuclear cells were re-suspended in medium containing α-minimum essential medium (MEM; Sigma Aldrich), 10% foetal bovine serum (FBS; Sigma Aldrich), 50 U/mL penicillin and 50 µg/mL streptomycin (Gibco, Scotland) at 37°C with 5% CO2. After overnight incubation, non-attached cells were removed by a series of PBS washes and subsequent medium changes. Thereafter, medium was exchanged every 3 to 4 days. At passage 3, adherent BMSCs were counted using trypan blue exclusion and a haemocytometer for downstream experiments.
Cell seeding and chondrogenic induction
BMSCs were seeded at 2 × 106/scaffold onto the auricular scaffolds (n = 3). Tissue culture polystyrene (TCP) acted as our positive control. To ensure that the cells fully penetrated the auricular scaffolds, they were injected via a sterile 10-mL syringe. The auricular scaffolds were washed with PBS and soaked in cell culture medium (CCM) for 24 h prior to cell seeding. The chondrogenic medium consisted of high-glucose Dulbecco’s modified Eagle medium (DMEM; Gibco, Scotland), 10 ng/mL TGF-β3 (Sigma Aldrich), 10−8 M dexamethasone (Sigma Aldrich), 50 µL/mL ascorbate-2-phosphate (Fluka, Gillingham, UK), Premix ITS+ (BD Biosciences, Oxford, UK), 50 U/mL penicillin and 50 µg/mL streptomycin (Gibco, Scotland). This medium was changed every 3 days, and constructs were kept in an incubator under static conditions.
One auricle was harvested at 7, 14 and 21 days for cell viability studies. The other two auricular scaffolds were harvested at 21 days for SEM, histological and immunofluorescence analysis. Each auricle was divided into nine even pieces (including both external and internal surfaces) for the following experiments.
Cell proliferation assay
The viability and proliferation of cultured BMSCs in chondrogenic medium was evaluated using the AB assay (AlamarBlue®, Serotec, Kidlington, UK). Briefly, 10% (v/v) of AB was added to the culture media of the cell-seeded ear scaffolds 4 h prior to the end of cell culture (7, 14 and 21 days). The absorbance was recorded using a spectrofluorometer (Thermo Lifesciences, Basingstoke, UK) set at 570 nm.
SEM
At day 21, six samples of BMSC seeded-auricular constructs were collected for SEM. After washing with PBS and fixing with 2% glutaraldehyde, the SEM protocol described above was followed.
Histological analysis
At day 21, six samples of BMSC seeded-auricular constructs and TCP were collected for histology. The specimens were fixed with 4% paraformaldehyde (Sigma Aldrich) following a wash with PBS, embedded in paraffin and sectioned using standard histochemical techniques. The samples were observed with a stereoscope microscopy imaging system (Nikon, SMZ 1500) fixed with a digital camera (Nikon, DXM1200). The following stains were used (Sigma Aldrich) to detect the presence of cell nuclei, glycosaminoglycan (GAG) and elastin fibres:
Haematoxylin and eosin: sections were deparaffinised, dehydrated with xylene and then rehydrated in graded ethanol over a 10-min period. Sections were washed in distilled water and stained with haematoxylin solution for 8 min. After washing in distilled water for 5 min, sections were decoloured in acid ethanol (30 s) and washed again in distilled water. This was followed by bluing in lithium carbonate solution for 30 s, rinsing in distilled water and staining with eosin for 2 min.
Safranin-O: sections were taken to water and stained with Weigert’s haematoxylin for 7 min. This was washed in distilled water until blue (5 min). Sections were checked microscopically and differentiated in acid alcohol if required. Following a wash with distilled water, sections were stained with fast green solution for 3 min, rinsed in 1% acetic acid, stained with 0.1% safranin-O for 5 min and rinsed again in 1% acetic acid.
Orcein: sections were treated with acidified potassium permanganate for 15 min, washed in distilled water and decolourised in 1% oxalic acid. This was followed by a further wash in distilled water and then 70% alcohol. The sections were then stained in orcein solution for 45 min, rinsed in 70% alcohol and dehydrated slowly.
Immunofluorescence analysis
At day 21, six samples of BMSC seeded-auricular constructs were collected for immunostaining. Samples were washed twice in PBS, fixed with 4% paraformaldehyde and washed another three times in PBS. Slides were then incubated with 4% fat-free milk in PBS for 20 min (to suppress non-specific binding of IgG), and subsequently the blocking solution was removed. Following a wash in PBS, sections were incubated, at room temperature, with the primary antibody rabbit anti-human polyclonal IgG (SOX-9, H-90) at a concentration of 1:100 with 1.5% fat-free milk for 60 min. After 3 washes with PBS, secondary antibody (goat anti-rabbit IgG (SOX-9)) conjugated to fluorescein isothiocyanate (FITC) in 1.5% fat-free milk was added to the samples and incubated for 45 min. After washing, slides were placed in propidium iodide at 1:1000 in PBS, mounted and examined using a confocal fluorescence/laser microscope (NikonD-ellipse C1 2100, Bio-Rad, Hemel Hempstead, UK). A similar protocol was followed for collagen type II immunostaining using a goat anti-human polyclonal IgG primary (N-19) and rabbit anti-goat IgG secondary conjugated to Texas Red. All antibodies were purchased from Santa Cruz Biotechnology, Dallas, USA.
Statistical analysis
All experimental results were analysed using IBM® SPSS® Statistics Version 20. Data were expressed as means ± standard deviation and analysed for statistical significance by independent-measure t-test, where p < 0.05 was considered statistically significant.
Results
Gross macroscopic appearance of auricular scaffold
The auricular-shaped POSS-PCU scaffold produced via coagulation/salt leaching had a very similar anatomical structure to the positive human auricle and with an almost identical size. The engineered auricle was resilient, smooth and had a whitish-pink colour. Following in vitro culture with BMSCs for 21 days, our auricle maintained its structural integrity, colour and texture (Figure 1).
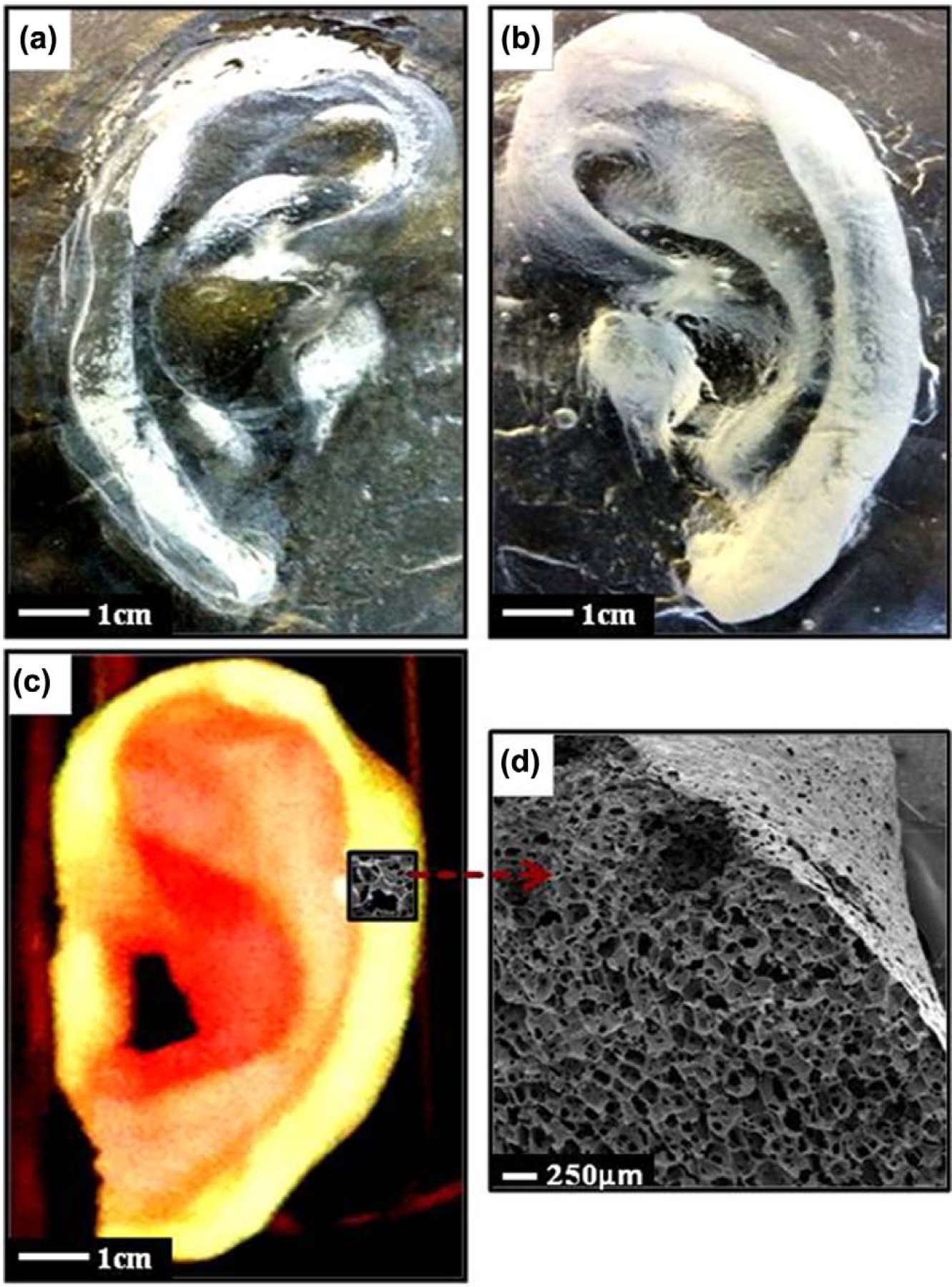
Images of a novel human-sized, glass mould–designed, porous auricular scaffold made from a nanocomposite POSS-PCU polymer: (a) outer part of the negative glass mould, (b) inner part of the glass mould, (c) a digital photograph of the resultant porous auricular scaffold produced and (d) SEM cross-section of the auricular scaffold fabricated using coagulation/particulate-leaching techniques.
Auricular nanocomposite scaffold characterisation
Surface and cross-sectional SEM morphology of the POSS-PCU scaffolds revealed a homogenous structure with evenly distributed interconnected pores, with an average pore size of 240.25 ± 6 µm and a porosity of 88.60% ± 0.05% (Figure 2). However, the surface was substantially less porous. Young’s modulus of the polymer was shown to be 0.55 ± 0.02 MPa when compared to native auricular cartilage 5.02 ± 0.04 MPa, which demonstrates the significant elastic nature of POSS-PCU. This elasticity does not compromise the structural integrity of POSS-PCU as shown by the tensile strength of 1.85 ± 0.22 MPa and elongation at break of 261.74% ± 27% (Table 1).

SEM micrographs of (a and b) surface and (c and d) cross-section morphologies of auricular POSS-PCU scaffold indicative of the effect of porogen (NaCl) leaching on construct structure and porosity.
Structural and mechanical characterisation of the POSS-PCU NC scaffold compared to human auricular cartilage.

Source: Human auricle values.
POSS-PCU: polyhedral oligomeric silsesquioxane-modified poly(hexanolactone/carbonate)urethane/urea; NC: nanocomposite.
Values are mean ± standard deviation (SD) (n = 4).
Evaluation of chondrogenesis on auricular scaffold
BMSC proliferation
There was a significant increase in the rate of proliferation on both POSS-PCU auricular scaffold and TCP at days 7, 14 and 21 (Figure 3). Although TCP proved to be significantly more conducive to cell proliferation than POSS-PCU, there were proportionally greater increases in cell proliferation at days 7, 14 and 21 with POSS-PCU.
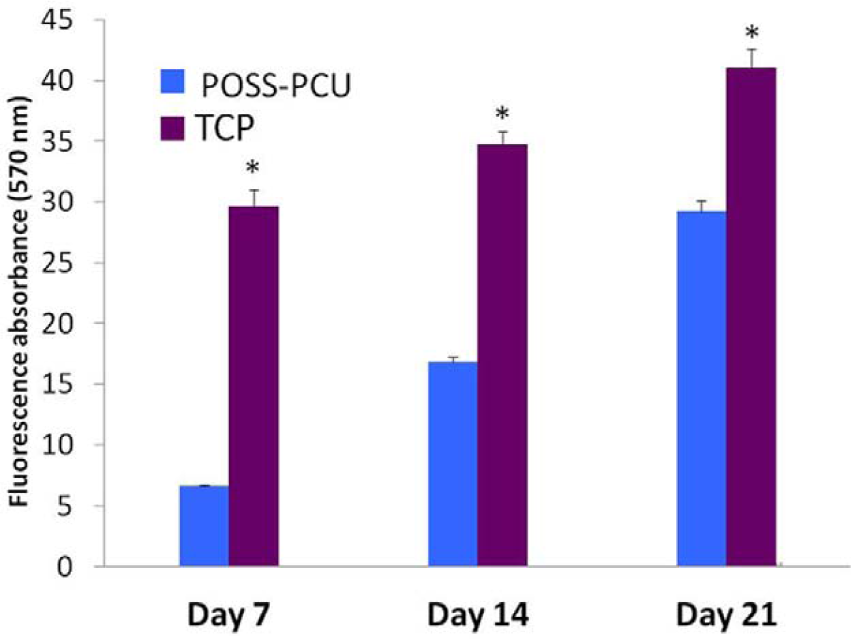
Proliferation of bone marrow–derived mesenchymal stem cells (BMSC) culture on POSS-PCU nanocomposite (blue) and tissue culture polystyrene (TCP) (purple) surfaces after 7, 14 and 21 days.
BMSC morphology with SEM
At day 21, BMSCs aggregated both on the surface of the polymer and within the construct. Cell numbers appear to be sparse and while some have adopted a round configuration consistent with chondrocytes, the majority have irregular MSC morphology with a small cell body and long, thin cell processes. There is the suggestion of extracellular matrix (ECM; web-like network) production inside the scaffold (Figure 4).

SEM micrographs of auricular scaffold samples seeded with BMSCs on day 21. Images were taken of (a and b) the surface and (c and d) cross-section of the polymer.
Histology
At day 21, there is clear evidence of early chondrogenesis on our auricle, assessed by the presence of prominent ECM constituents GAG (Figure 5(c)) and elastin (Figure 5(e)). The TCP control, as expected, shows significant chondrogenesis at this stage.

Histological analysis at day 21 with (a and b) haematoxylin and eosin, (c and d) safranin-O (e and f) and orcein staining. Plane conditions (i.e. tissue culture polystyrene) are presented as a comparison. There is evidence of early chondrogenesis on the POSS-PCU polymer highlighted by the presence of (a) cell nuclei, (c) GAG and (e) elastin. Calibration bar, 20 µm.
Immunofluorescence
At day 21, both POSS-PCU and TCP specimens showed evidence of significant staining for SOX-9 (green) and collagen type II (red) under the confocal microscope (Figure 6). There is nuclear localisation of SOX-9 and collagen II deposition within ECM. Further control slides incubated with secondary antibody only had no visible staining.
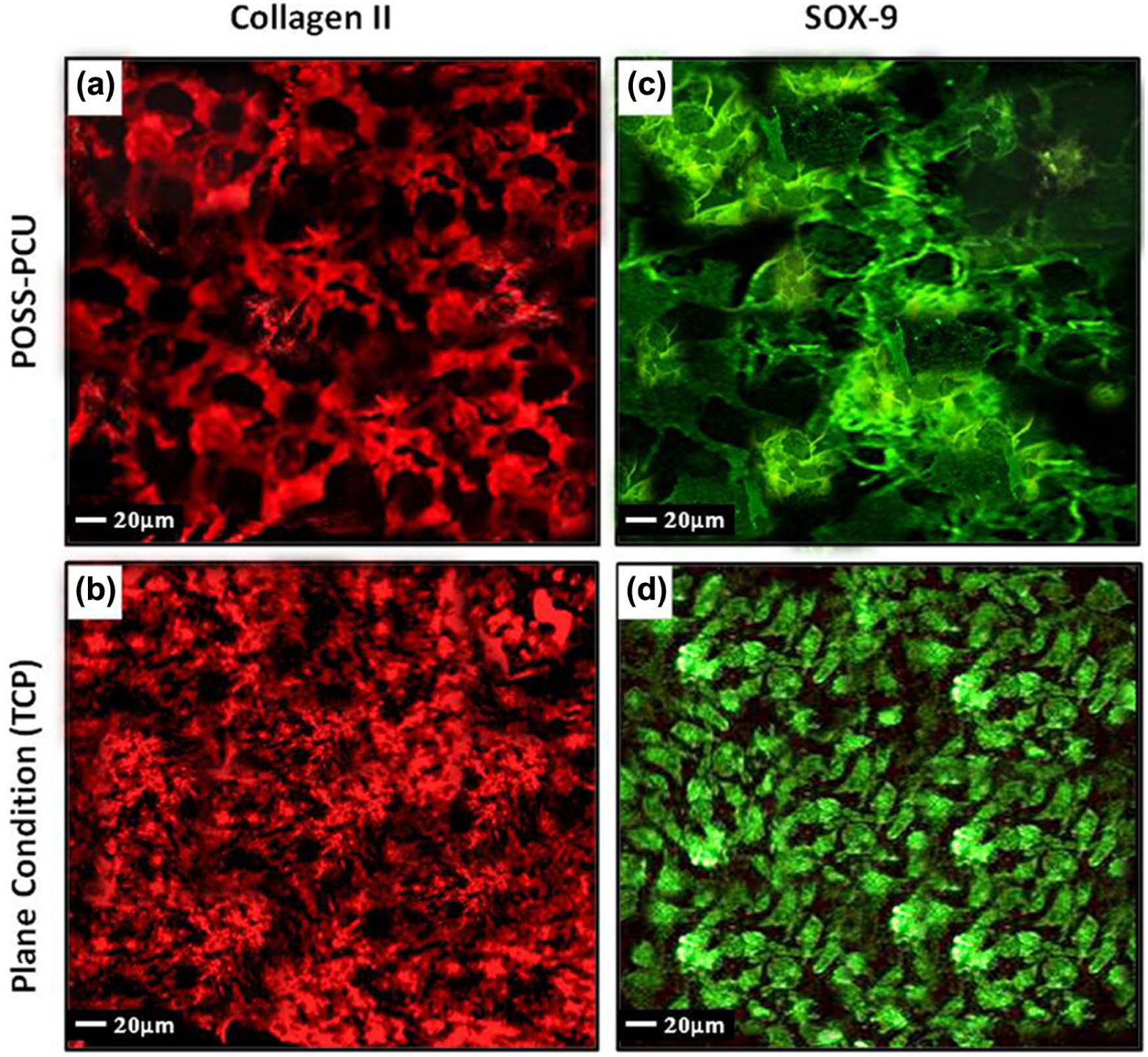
Immunofluorescence analysis at day 21 for (a and b) collagen type II and (c and d) SOX-9. Plane conditions (i.e. tissue culture polystyrene) are presented as a comparison. There is evidence of chondrogenesis on the POSS-PCU polymer. Calibration bar, 20 µm.
Discussion
This study investigated the in vitro feasibility of POSS-PCU auricular constructs as a scaffold for BMSCs, in the presence of chondrogenic medium, for purposes of cartilage tissue engineering. Neocartilage formation was evaluated through SEM imaging, histology and immunofluorescence analysis. In addition, characterisation of POSS-PCU polymer provided quantitative data on its mechanical properties. We have demonstrated successful fabrication of an auricular-shaped porous scaffold using a coagulation/salt-leaching method, and moreover, that BMSCs indeed showed chondrogenic potential when seeded onto the POSS-PCU nanocomposite (NC) constructs. Cell viability assay confirmed cytocompatability and normal patterns of cellular growth on POSS-PCU scaffolds. Cell metabolism was significantly higher on TCP, although this is expected as TCP is an optimised surface for cell growth.
Characterisation of the POSS-PCU scaffold revealed a high porosity in excess of 88%. This was achieved through the coagulation/salt-leaching technique which resulted in an average pore size of 240 µm. These porous nanostructures provide a favourable 3-D environment to accommodate BMSCs at high seeding densities and promote cellular condensation required for neocartilage formation. This high surface to volume ratio encourages cell attachment and cellular in-growth within the polymer structure both in vivo and in vitro. 33 A minimum porosity of 85% is required to provide the ideal microenvironment for cell nutrient exchange, ECM deposition and to minimise the harmful effects of waste products via diffusion gradients. 33 This homogenous NC structure, revealed by SEM imaging, confers mechanical strength to the polymer via efficient load transfer. 34 Furthermore, there was no evidence of any change in the gross morphology, size or consistency of the auricular scaffolds following 21 days of culture. Although this is a short time period and was performed in vitro, the fact that POSS-PCU is resistant to degradation may prove beneficial in maintaining long-term structural integrity. Previous work on POSS-PCU has revealed that its fabrication through a coagulation/salt-leaching method results in increased surface roughness which in turn provides an even greater surface area for protein attachment and subsequently cellular behaviour. 35
The mechanical analysis of the NC polymer highlighted the considerable elasticity of POSS-PCU (E-modulus of 0.55 MPa). It is this flexibility which is essential to auricular tissue engineering as previously engineered constructs have been brittle and rigid. 36 POSS-PCU has been shown to have a comparable tensile strength to that of native auricular cartilage (albeit slightly lower), and this is due to the incorporation of POSS nanocages into PCU. 34 The issue with comparing tensile strength of the NC polymer with native cartilage is that mature cartilage is fully cellularised, and this undoubtedly confers mechanical strength.
Due to the great potential of BMSCs to differentiate into a variety of cells, they are clearly an attractive option for tissue engineering. Encouragingly, the SEM images reveal cells that have infiltrated within the porous scaffold forming an intricate web-like structure representing early stages of ECM deposition. Cells exhibiting a polygonal morphology on SEM imaging are likely to be chondro-induced BMSCs where they have not yet adopted the typical round chondrocyte-like morphology. However, SEM images revealed that there are far fewer pores on the scaffold surface, thus making it more difficult for cells to fully infiltrate the structure (we attempted to overcome this by injecting cells). There did appear to be areas where BMSCs had adhered to the scaffold in aggregates. This is quite possibly due to BMSCs attempting to recreate the embryonic mesenchymal condensation process during the early stages of chondrogenesis. 37
Histological analysis also confirms the presence of chondrogenesis following the 21-day culture period. Areas of intense colouring for cell nuclei, GAG, collagen type II and elastin fibres in the POSS-PCU scaffold were evident. However, distribution of cells on the engineered construct was rather irregular, and this made interpretation difficult. Early matrix deposition is visible within the porous structure of POSS-PCU. Although studies have demonstrated zonal morphology reminiscent of native cartilage after 21 days culture using BMSC, this was not evident on the POSS-PCU polymer. 17 Several researchers have reported that engineered cartilage contains significantly less elastin and collagen than native cartilage (up to 60% less), 38 although this was not assessed in our experiment.
SOX-9 immunofluorescence imaging of the auricular scaffold revealed intense green fluorescence. SOX-9, a transcription factor containing the high-mobility group box domain, is expressed in chondrogenesis, and this largely overlaps with Col2a1 expression, a major cartilage matrix protein. Therefore, its intracellular localisation on immunofluorescence is very suggestive of chondrogenesis. There is a red fluorescent display for collagen type II which indicates the presence of collagen precursors within the cell and, to a limited extent (due to the fact that it is only day 21), in ECM. Sections with secondary antibody only were also imaged, and there was no significant fluorescence (results not presented).
Cell seeding density seems to be a crucial factor on the success of auricular engineered constructs. Currently, the most common method of promoting chondrogenesis in MSCs is high-density cell pellet culture as this is said to increase cell-to-cell interaction and therefore initiate chondrogenesis. 39 However, this method is not appropriate for tissue engineering because of its inferior mechanical properties. The auricular construct in this study was seeded with approximately 2 × 106 cells, but almost 100 times that are said to be required for a successful engineered construct. Due to the limited number of cells and the short time frame of 21 days, the auricles exhibited a relatively sparse population of cells that was not uniformly distributed. We had a limited BMSC supply (MSC harvest is in the region of 0.001%–0.01%), and there is a risk of de-differentiation with multiple passages.
Uniform cell distribution on this NC polymer was a concern in this study. We soaked the auricular scaffold in CCM for 24 h; however, other groups have preferred to coat their scaffolds in type I collagen or NaOH. Type I collagen has been shown to contain recognition sites for integrins, and these surface modifications could therefore promote uniform cell distribution on the polymer. 40 Bioreactors are known to encourage an even cell distribution, efficient transport of molecules within culture medium and generally improve the functional properties of neocartilage in vitro. Further studies with POSS-PCU may include an in vitro culture stage in a bioreactor followed by implanting the engineered auricle into an in vivo model. Another limitation derives from unexpected irregularities, outside of experimental parameters, associated with the donor-to-donor variability of MSCs. An in vitro model is limited by the lack of an in vivo niche which contributes to determining the lineage and fate of exogenously transplanted stem cells. 41 The most commonly used in vivo models for tissue engineering are mice and rabbits; however, they lack a functional T-cell immune system, are too small to implant an adult-sized ear and have a short life-span. POSS-PCU has already demonstrated good cell compatibility, degradative resistance, favourable viscoelastic properties and a lesser degree of immunogenicity both in vitro and in vivo. 25
Conclusion
This study has described an approach to auricular tissue engineering through seeding a novel NC polymer, POSS-PCU, with BMSCs. This study has demonstrated that this auricular-shaped NC scaffold supports the in vitro chondrogenic differentiation of BMSCs in medium containing TGF-β3. This is supported by cell proliferation assay, SEM, histological and immunofluorescence analysis.
Future studies could lie with the creation of ‘intelligent’ scaffolds and in vivo investigation. It has been demonstrated that POSS-PCU consists of an incorporated form of RGD (arginine-glycine-aspartic acid (Arg-Gly-Aspa)), a tri-peptide based on fibronectin, which encourages endothelial progenitor cell differentiation on its surface. 42 There are several studies that have investigated scaffolds with incorporated growth factors to good effect. 43 Recently, our group has shown POSS-PCU to have superior fibroblast attachment and proliferation when compared to the commercially available Medpor. 44 Culturing the BMSC scaffold with fibroblasts may improve fibrovascularisation and enhance cell attachment, which may subsequently reduce the risk of implant extrusion seen in previous studies.
Footnotes
Acknowledgements
Kavi H Patel and Leila Nayyer contributed equally to the research paper.
Declaration of conflicting interests
The authors have no conflicting interests to declare in relation to the content of this article.
Funding
This research partially funded by the Healing Foundation, London WC2A 3PE.
Ethical conduct of research
Fully informed consent has been obtained from participants involved.