Abstract
Clinical evidence suggests that Zika virus contributes to Guillain-Barré syndrome that causes temporary paralysis. We utilized a recently described Zika virus mouse model of temporary flaccid paralysis to address the hypothesis that treatment with an N-methyl-D-aspartate receptor antagonist, memantine, can reduce the incidence of paralysis. Aged interferon alpha/beta-receptor knockout mice were used because of their sublethal susceptibility to Zika virus infection. Fifteen to twenty-five percent of mice infected with a Puerto Rico strain of Zika virus develop acute flaccid paralysis beginning at days 8–9 and peaked at days 10–12. Mice recover from paralysis within a week of onset. In two independent studies, twice daily oral administration of memantine at 60 mg/kg/day on days 4 through 9 after viral challenge significantly reduced the incidence of paralysis. No efficacy was observed with treatments from days 9 through 12. Memantine treatment in cell culture or mice did not affect viral titers. These data indicate that early treatment of memantine before onset of paralysis is efficacious, but treatments beyond the onset of paralysis were not efficacious. The effect of this N-methyl-D-aspartate receptor antagonist on the incidence of Zika virus-induced paralysis may provide guidance for investigations on the mechanism of paralysis.
Keywords
Introduction
Congenital Zika syndrome and Guillain-Barré syndrome in adults are two serious outcomes associated with Zika virus outbreaks.1–4 Guillain-Barré syndrome is a reversible, acute peripheral neuropathy involving temporary paralysis. The mechanism by which Zika virus causes paralysis in Guillain-Barré syndrome is unknown. A recent mouse model of Zika virus-induced temporary paralysis has provided an opportunity to evaluate cellular mechanisms. 5 Since Zika virus does not cause robust disease in adult laboratory mice, interferon αβ-receptor (IFNAR−/−) knockout mice were used. Infection is lethal in young IFNAR−/− mice, but infection in aged mice greater than 4-months-old is sublethal. In these mice, hindlimb acute flaccid paralysis developed in 15–25% of infected mice beginning on days 8–9 and peaking on days 10–11. Within a week of onset, mice recover from paralysis.
Unlike more pathogenic flaviviruses, like West Nile virus or Japanese encephalitis virus, that infect and destroy motor neurons in the spinal cord, 5 Zika virus infection in aged IFNAR-/- mice does not destroy motor neurons. Zika virus immunoreactivity cannot be readily detected with colocalization of motor neuron-immunoreactive markers in the lumbosacral spinal cords of paralyzed mice, yet there is some Zika virus immunoreactivity outside of motor neurons. Ultrastructural analysis by electron microscopy reveal that pre-synaptic terminals becomes detached or retracted from alpha-motor neurons in paralyzed mice at a statistically significant level. The synapses are then re-associated upon recovery of paralysis. The biochemical mechanisms by which these events occur is uninvestigated.
To begin mechanistic studies, we evaluated memantine for efficacy. Memantine is an N-methyl-D-aspartate receptor antagonist and is an indication for treatment of moderate to severe Alzheimer’s disease. The premise for this efficacy study is that memantine and other agonists (dizocilpine (MK-801), agmatine sulfate, ifenprodil) prevent neuronal death in cell culture without affecting Zika virus replication, and prevent the increase of virus induced-intraocular pressure and reduce neurodegeneration in the brains of interferon-receptor deficient mice.6,7 In a subsequent neuronal cell culture study, blocking of the N-methyl-D-aspartate receptor by ifenprodil reduced neuronal cell death coincident with reduced influx of Ca+2. 8
Methods
In the first of three memantine treatment experiments, male and female IFNAR-/- mice at 4.2- to 5.3-months-old were block-randomized between groups according to weight and gender and injected subcutaneously (s.c.) on both sides for a total of 1,340 pfu of ZIKV per mouse (PRVABC59, Human/2015/Puerto Rico, BEI Resources passaged 2 times in Vero 76 cells in MEM with 50 µg/mL gentamicin) or sham (uninfected cells prepared and diluted the same as the viral inoculum). Although one strain of ZIKV were not evaluated, there was no a priori reason to believe that memantine would be efficacious with other viral strains because memantine is probably targeting cellular processes, and not the virus specifically. Beginning at 4 days after viral challenge, mice were treated twice daily by oral gavage (p.o.). Treatments continued through day 9. Volumes of treatment solution were adjusted for weights of individual mice to achieve 60 mg/kg/day dosage. The numbers of mice were n = 16 for the ZIKV-memantine group, n = 14 for the ZIKV-vehicle group, n = 3 for the sham-memantine group, and n = 3 for the sham-vehicle group. Details of the other two experiments shown in figure legends are similar to this first experiment. Data were analyzed using generalized estimating equation with compound symmetry structure of the working correlation matrix. Binary outcome of motor deficit is modelled with logit link function. Analysis was performed using PROC GENMOD in SAS/STAT 15.1 (SAS Institute Inc., Cary, NC). Animal studies were accordance with the approval of the Institutional Animal Care and Use Committee of Utah State University.
Mice were analyzed using the viral paresis scale 9 for signs of tail and hindlimb paresis/paralysis using a sensitive, open-field assay modified from the Basso Mouse Scale used to assess paralysis in spinal cord-injured mice 10 and a test used to track paralysis in amyotrophic lateral sclerosis mouse models. 11 Each mouse was placed on a tabletop and allowed to roam freely for 4 minutes. Hindlimb function was scored on a 7-point scale 9 by researchers who were blinded to the infection status of each group. In this study, mice with VPS of 5 or 6 were paralyzed in either or both hindlimbs.
Results
Memantine treated from day 4 through day 9 significantly reduced the prevalence of paralysis (p = 0.020) (Figure 1(a)). The number of paralysis-mouse-days was also statistically reduced at p = 0.0010 and p = 0.0001, respectively (Figure 1(b)). Since the incidences of paralysis of placebo-treated mice (6/18, 33%) was low, the statistical power was weak. To validate the reproducibility of these data, a second independent experiment was performed. We increased the numbers of mice in each infected group from 18 and 20, to 26 each. Even though the incidence of paralysis in the placebo-treated group was again low at 19% (5/26), memantine was still efficacious in reducing the prevalence of paralysis (p = 0.040) (Figure 1(d)). We were able to overcome the statistical challenge of a low incidence of paralysis by performing two independent experiments, increasing the number of mice in each infected group to 26, and using an appropriate statistical model. Data were also analyzed by calculating the paralysis-mouse-days. By Fischer’s exact P stack analysis, memantine also significantly improved the paralysis outcome (Figure 1(e)) (p = 0.0089, respectively). This statistical test of the percentage of paralyzed mice also revealed statistical significance (p = 0.0381) in experiment #1, but not experiment #2. As previously observed, 5 most animals survive (Figure 1(c) and (f)) and recover from paralysis (Figure 1(a) and (d)).
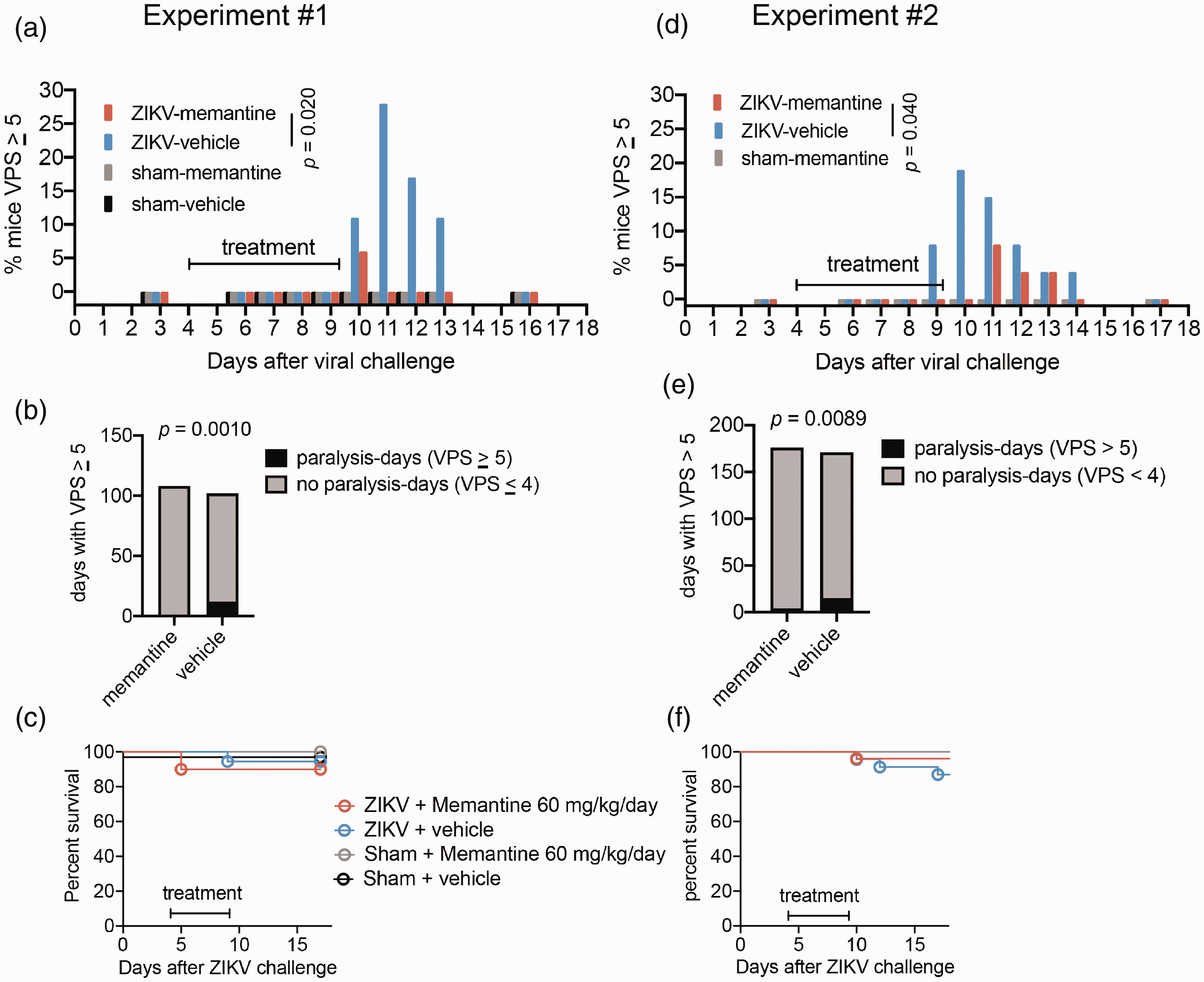
Memantine (60 mg/kg/day) twice daily oral gavage (p.o.) treatments on days 4 to 9 after Zika virus challenge reduced the prevalence of (a, d) paralysis and (b, e) paralysis mouse-days in two independent experimental trials. Paralysis was identified in mice having VPS ≥5 on either or both hindlimbs. Paralysis mouse-days were calculated by the number of paralyzed mice on each day between 9 and 12 days for each group divided by the total number of mice on each day between 9 and 12 days per group. (c, f) Survival was high (>80%). The age of the IFNAR−/− mice in experiment #1 were 4.2- to 5.3-months-old. n = 20 ZIKV-memantine group; n = 18 ZIKV-vehicle group; n = 9 sham-memantine group; n = 9 sham-vehicle group.
To determine if memantine could treat existing paralysis, treatment was initiated at day 9 and extended through peak days of paralysis through day 14. However, memantine was ineffective; statistical differences in paralysis were not observed (Figure 2).
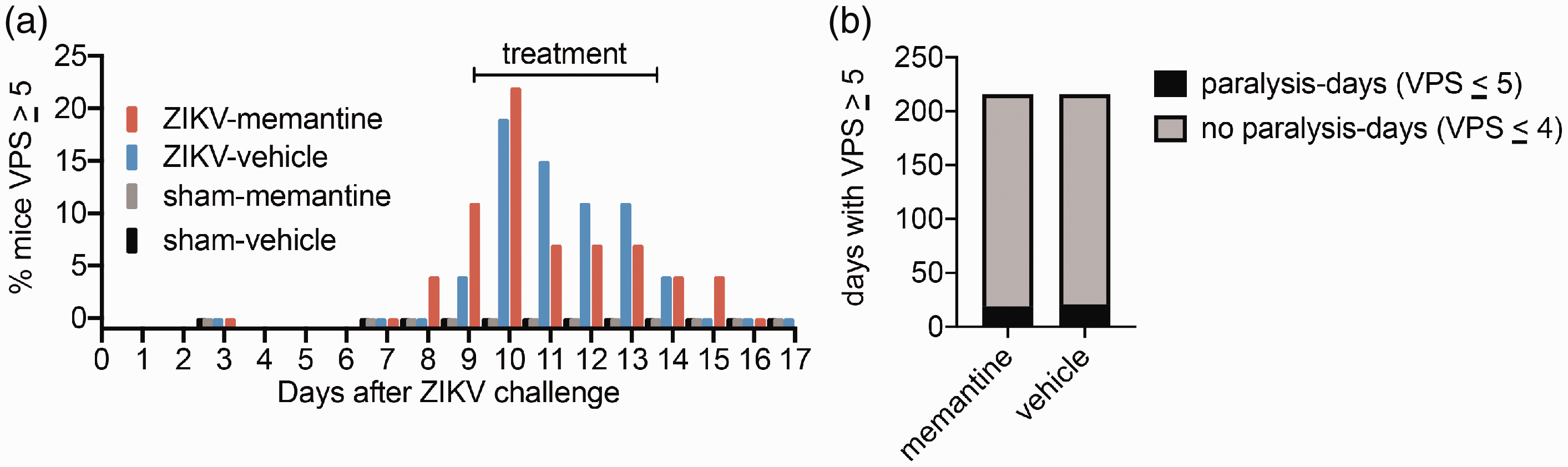
Memantine (60 mg/kg/day) twice daily oral gavage (p.o.) treatments on days 9 to 12 after Zika virus (ZIKV) challenge did not affect the prevalence of (a) paralysis or (b) paralysis-mouse-days. Paralysis were identified in mice having VPS ≥ 5 on either or both hindlimbs. The age of the IFNAR−/− mice were 3.9 to 4.1-months. n = 27 ZIKV-memantine group; n = 27 ZIKV-vehicle group; n = 4 sham-memantine group; n = 4 sham-vehicle group. The experimental protocol was the same as in Figure 1, except memantine was treated from day 9 through the morning of day 12. The data of the ZIKV-memantine group were not statistically different from those of the ZIKV-vehicle group.
We eliminated the possibility that memantine’s mechanism of action was to reduce viral load as measured in cell culture (50% effective concentration >7.8 µg/mL; 50% cytotoxic concentration = 7.8 µg/mL) or in the spinal cords of mice (Figure 3), which confirmed previous results observed in primary neuronal cell culture. 6
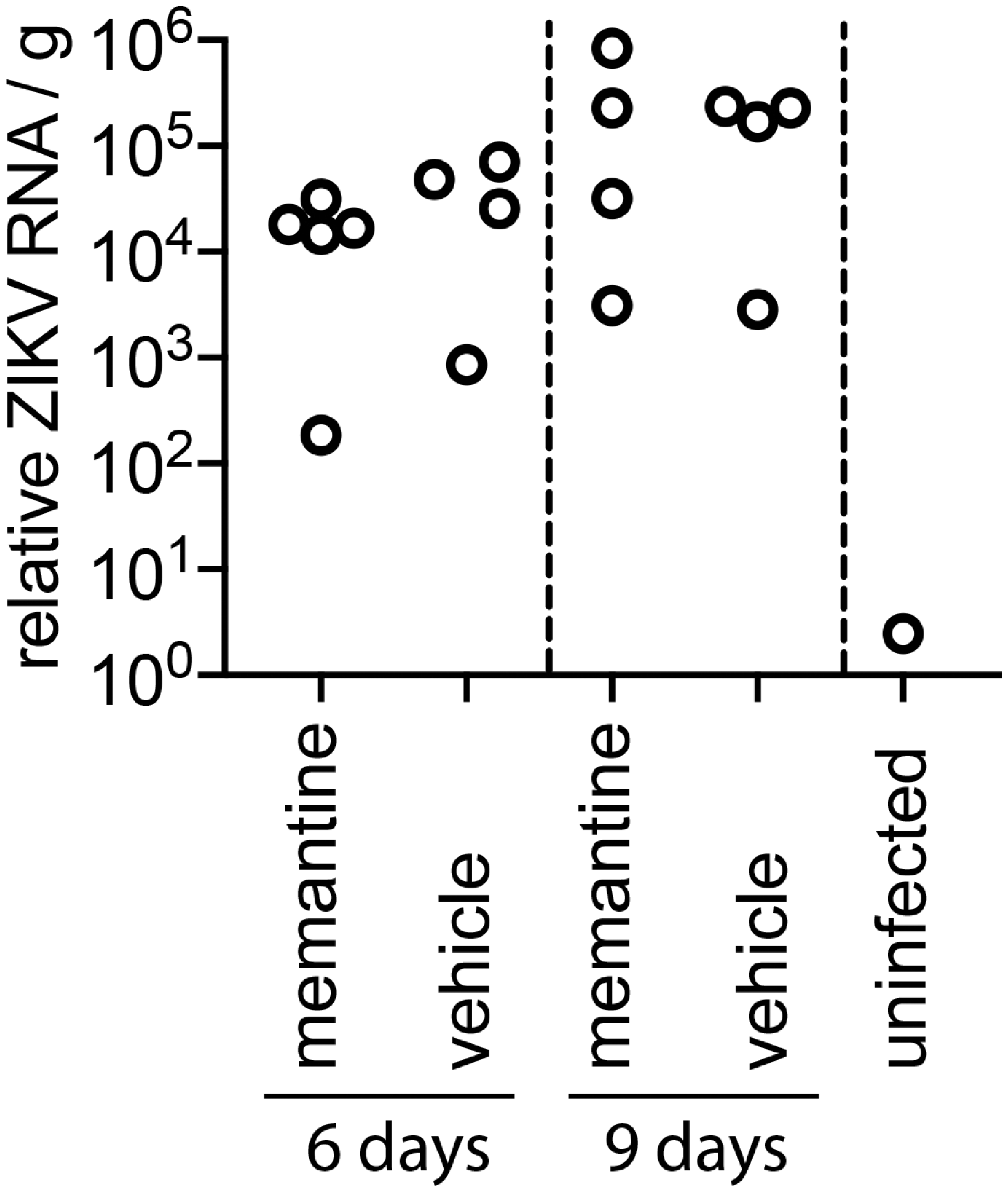
ZIKV RNA unaffected by memantine treatment in the lumbosacral spinal cord collected at 6 and 9 days after viral challenge.
Discussion
The primary purpose of this study was to investigate the possible role of N-methyl-D-aspartate receptor in the development of temporary paralysis caused by ZIKV using memantine, an inhibitor of this receptor. In two independent experiments, memantine reduced the incidence of paralysis, which suggests that activation of this receptor is associated with paralysis. A distinguishing pathological event in this mouse model is that pre-synaptic terminals becomes detached or retracted from alpha-motor neurons in paralyzed mice. 5 The synapses are then re-associated upon recovery of paralysis. A hypothesis for future studies, therefore, is that glutamate excitotoxicity mediated by N-methyl-D-aspartate receptors signals synaptic retraction and paralysis, and that resolution of glutamate excitotoxicity might reverse the paralysis of ZIKV-induced Guillain-Barré syndrome.
A limitation of the study is the necessary use of interferon non-responsive mice. A series of publications following the ZIKV outbreak found that adult wild-type laboratory mice are not susceptible to ZIKV infection, but mice that lack type 1 and/or type 2 interferon receptors are susceptible to lethal infection.12–16 These interferon non-responsive models do have flaws, but they may also have some relevance to human ZIKV infections. Like many viruses, ZIKV gains advantages in human hosts by inhibiting interferon responses.17–19 Because the virus may not be able to inhibit mouse-specific interferon pathways,20 blocking interferon response in transgenic mice allows the virus to similarly replicate as it does in human subjects.
These data indicate that early treatment of memantine before onset of paralysis is efficacious, but treatments beyond the onset of paralysis were not efficacious. The effect of this N-methyl-D-aspartate receptor antagonist on the incidence of Zika virus-induced paralysis may provide guidance for investigations on the mechanism of paralysis.
Footnotes
Acknowledgements
We thank the following individuals from the Institute for Antiviral Research at Utah State University for their excellent technical assistance: Dallan Blotter for conducting thorough VPS scoring; Brittney Downs, Dallan Blotter and Kade Roberts for performing viral tissue titers, Matthew McKinnon for ZIKV RT-PCR, Parker Webber for managing IFNAR−/− mouse colony; Ashley Dagley for overseeing technician training and animal studies; Jaxton Birky, Ben Elgan, Carlee Frank, Dallan Blotter, Kade Roberts, Nicole Anderson, Parker Webber and Ryden Crowther for conducting animal studies; and Nicole Anderson for proof-reading the manuscript.
Author’s contribution
JDM, VS and ALRO conceived the study and experimental design. JDM, VS, and HW acquired, analyzed and interpreted the data. XD modeled and analyzed the statistics. JDM wrote the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The work was supported by Public Health Service (PHS) research grants 1R21NS090133 to J.D.M. from the National Institute of Neurological Disorders and Stroke (NINDS), National Institutes of Health (NIH), and PHS grant 5R33AI101483 and contract HHSN272201000039I/HHSN27200004 to J.D.M. from the Virology Branch, National Institute of Allergy and Infectious Diseases (NIAID), NIH, Utah Agriculture Research Station research grant UTA01176 to J.D.M., Fundação de Amparo à Pesquisa do Estado de São Paulo – FAPESP, Brazil, proc. 2014/06892–3; Conselho Nacional de Desenvolvimento Científico e Tecnológico – CNPq, Brazil, proc. 303085/2017–7, A.R.L.de O. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
