Abstract
Dermatofibrosarcoma protuberans (DFSP) is an infrequent cutaneous tumour that may involve subcutaneous fat and in some cases fascia, muscles and bone. The infrequent occurrence lessens its clinical awareness in addition to its clinical semblance to many common cutaneous lesions. It is characterized by proclivity for local recurrence. We evaluated the clinical presentation and treatment outcomes of six consecutive cases of DFSP with histologic diagnosis in the University of Calabar Teaching Hospital, Calabar seen between January 2013 and December 2022. This was compared with total cutaneous malignances in the same period. The six consecutive patients comprised of two males and four females (M = F: 1:2) whose ages ranged from 21 to 57 years (mean of 36.5 years) and accounted for 7% of cutaneous malignancies. The site distribution was trunk (back) involved in 3 (50%) of the patients, limbs 3 (50%); upper 1 (17%) and lower limb 2 (33%). Clinical presentation was in the form of firm cutaneous mass with some ulcerated lesions that bled and some fungated. 50 percent of the patients presented with recurrent lesions and in all there was no regional lymphadenopathy or evidence of metastasis. There was a patient with Neurofibromatosis- 1 who had a huge fungated limb lesion offered amputation, four had wide local excision and one incision biopsy. Follow up was poor and the period ranged from 2 to 14 months (mean 7 months). Dermatofibrosarcoma protuberans is an uncommon tumour with clinical semblance to other cutaneous lesions. Early presentation, preoperative histologic diagnosis will enhance the goal of ensuring adequate excision. Adjuvant therapy with Imatinib with or without adjuvant radiotherapy are recommended in the treatment plan in view of the frequency of late presentation with advanced recurrent lesions and poor follow up.
Introduction
Dermatofibrosarcoma protuberans (DFSP) is a rare superficial fibroblastic tumour of intermediate malignancy with an incidence of four in 1,000,000.1–3 Dermatofibrosarcoma protuberans was originally described by Duer and Ferrand in 1924. 4 It is the commonest dermal sarcoma yet constitutes less than 0.1% of malignant neoplasms and approximately 1.0 % of soft tissue sarcoma worldwide. This tumour occurs mostly in the middle aged adults 30–35 years with no gender predilection. 5 Dermatofibrosarcoma protuberans commonly occurs in the trunk (50%), the proximal limbs (37%) and the head and neck region (10–15%). 6 Chromosomal translocation is present in over 90% of the cases of DFSP. This translocation t (17; 22) (q22; q13) between chromosome 17 and chromosome 22 is key to the pathogenesis of this tumour. 7 It is characterized by proclivity for local recurrence (5 year, 25%) and aggressive growth pattern following incomplete resection 8 and low potential to metastasize (range, 1–4%). 9 Given its propensity for subclinical extension, the optimal treatment modality is Mohs micrographic surgery (MMS). 10 Despite optimal surgical therapy for patients with DFSP, most patients continue to develop local recurrences thus promoting the use of systemic treatment from onset.11,12 The chemotherapeutic agent Imatinib mesylate is currently FDA approved for adults with unresectable recurrent or metastatic DFSP. 13 However, patients have a 10-years disease specific survival (DSS) of nearly 99.1%. 1 We present six cases of DFSP to highlight the challenges of management in our setting located in the tropics and proffer possible solutions.
Case 1
Presented is a 57 years old female with a history of a recurrent swelling of 12 months duration located on the back. She had a previous surgery 2 years ago in a private hospital facility without histology and attributed the swelling to trauma. Later, she noticed another mass at the site of the previous surgery which progressively increased in size over a year following which she presented to our facility. Examination revealed a patient in general good health with a firm, nodular, oval mass on the back over the right lumbar region that measured 6 × 5 cm across its widest dimensions. This was located about 3 cm beneath the scar of the previous surgery, not attached to deeper structure and there was no regional lymphadenopathy. Chest examination and abdominal examination were unremarkable. Chest X-ray was normal and lumbosacral X-ray revealed a soft tissue mass with no bony involvement. She was offered wide local excision which revealed DFSP on histology with resection margins (peripheral and deep) reported as tumour free. She was counselled on the risk of recurrence and the need for follow up emphasized. Patient was lost to follow up in the outpatient clinic after 6 months of surgery.
Case 2
A 32 years old woman presented with right hip mass of 10 months duration. Mass started like a boil, progressively increased in size and became rapid in the last 3 months following treatment at an alternative medicine facility. Examination revealed a patient in good health with a painless, oval mass located on the right side of the hip that measured 12 × 8 cm across the widest dimensions. The overlying skin had scarification marks, the mass was not attached to the underlying structure and there was no regional lymphadenopathy. Chest examination and abdominal examination were unremarkable. X-ray of the hip showed a soft tissue mass without bony involvement. Patient had wide local excision and histology revealed DFSP with no comment on the resection margins. She was counselled on the risk of recurrence following which the need for a long term follow up was emphasized but was lost to follow up after 5 months of surgery.
Case 3
Presented is a 32 years old female who was seen in the outpatient department with a swelling located on the left leg of 5 months duration. The mass, earlier attributed to trauma progressively increased in size for which she sought initial traditional medical treatment to no avail. Examination revealed a firm, non-tender mass that measured 8 × 5 cm across the widest dimensions. The overlying skin was hyperpigmented and the mass was attached to the underlying structure. There was no regional lymphadenopathy, chest examination and abdominal examination were unremarkable. X-ray of the leg revealed a soft tissue mass without bony involvement. She had an incision biopsy that revealed DFSP showing tumour that extended from the dermis to the subcutis. Patient was scheduled for wide local excision but absconded within 2 months of presentation.
Case 4
Presented is a 39 years old female with a history of recurrent mass located on the back of 7 months duration. She had noticed a recurrent mass 6 months following a previous surgery in a peripheral hospital without histology. Examination revealed a patient in good health with a painless, firm, nodular mobile mass overlying the left scapular region, measured 9 × 7 cm across the widest dimensions located about 2 cm beneath the scar of the previous surgery. Chest examination and abdominal examination were unremarkable. There was no regional lymphadenopathy. Chest X-ray showed clear lung fields, the PA and lateral views showed a soft tissue shadow. He was offered wide local excision which revealed a histology of DFSP without comment on the resection margin. She was lost to follow up 7 months after surgery.
Case 5
A 21 years old male presented with a swelling on the right arm of 5 years duration. This mass progressively increased in size over the years but noticed a rapid increase in the last 2 months, it bled occasionally with offensive discharge. Patient was diagnosed earlier with Neurofibromatosis- 1. Examination revealed a patient with multiple café au laits macules and multiple cutaneous neurofibromas distributed over the head and neck, trunk and the extremities. He had a fungated, nodular and immobile mass on the forearm that measured 29 × 20 cm across the widest dimensions. There was no regional lymphadenopathy. Chest examination and abdominal examination were normal. X-ray of the right arm showed an extensive soft tissue mass, the bones appeared normal. He had an above right elbow amputation with an uneventful recovery. Histology reported a forearm mass with a dermal tumour composed of malignant spindle cells in storiform and herring bone pattern in a fibrocollagenous stroma- DFSP, Figure 1(a) and (b). Tumour cells infiltrated the fibrous septa and trapped subcutaneous lobules giving a honey comb appearance, Figure 1(c). He was seen for 14 months after surgery in clinic and subsequently lost to follow up. (a) & (b): H&E × 40 & ×100-malignant spindle cells in storiform and herring bone pattern in a fibrocollagenous stroma. (c) H&E ×40-tumour cells infiltrate the fibrous septa and trapped subcutaneous fat lobules giving a honey comb appearance-DFSP.
Case 6
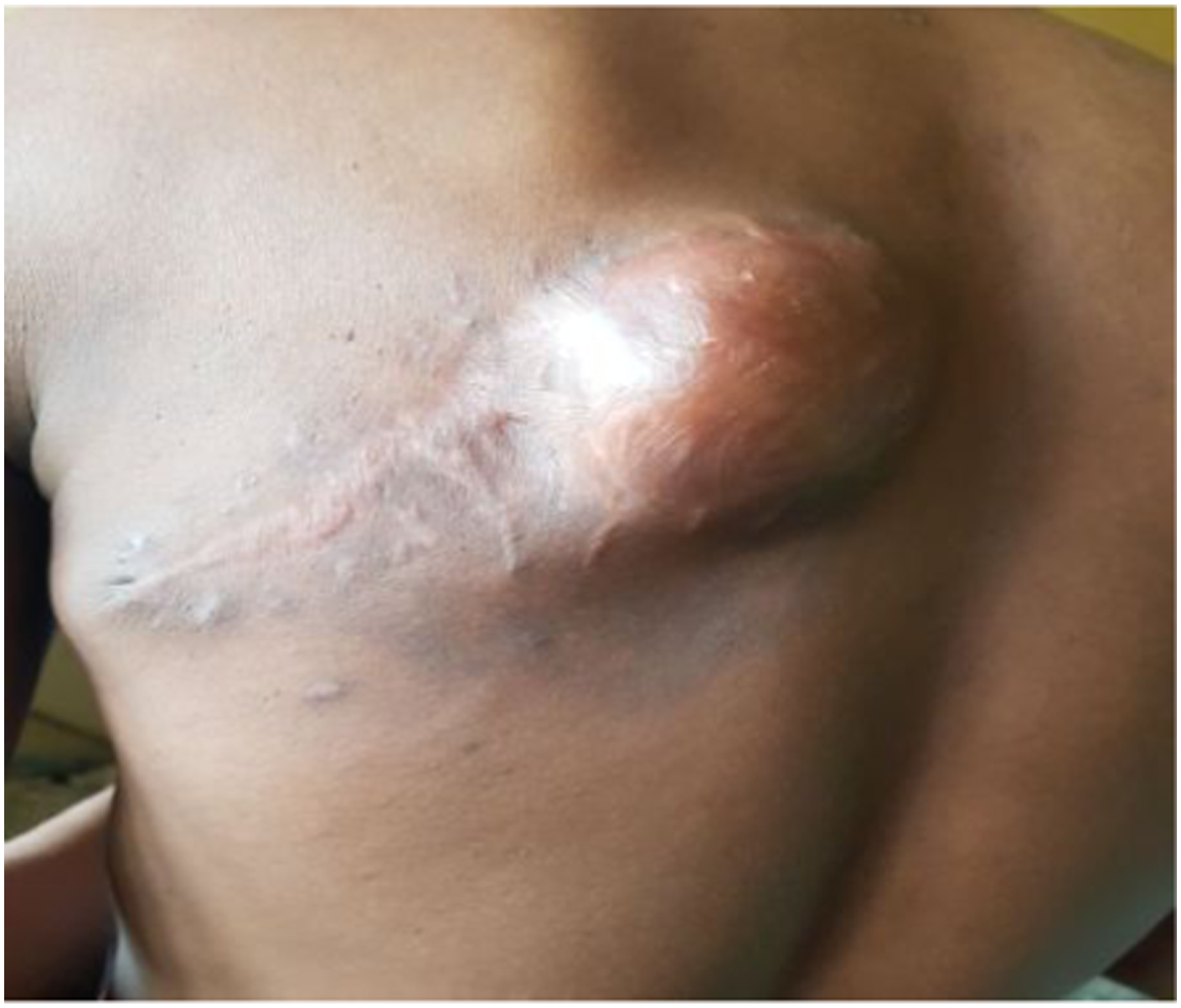
Presented is a 40 years old male with a recurrent swelling located on the left side of the back of 2 months duration. Had two previous surgeries for the same ailment a year ago and 5 months respectively in the same private hospital and was not informed of the nature of the lesion removed. Prior to presentation in our facility, he had sought for traditional medical therapy managed with scarification and topical herbs to no avail, Figure 2. Examination revealed a healthy-looking man with a swelling located on the left side of the back over the left scapular measuring 13 × 8 cm across the widest dimensions, Figure 3(a). Chest examination and abdominal examination were unremarkable. Chest X-ray showed clear lung fields and showed a soft tissue shadow of the mass, Figure 3(b). During work-up for surgery the lesion ruptured, bled, discharged foul smelling fluid. Had wide local excision with a histology of DFSP, no comment was made on the resection margins. Counselled for adjuvant therapy with imatinib but he defaulted and represented 2 months with a recurrent lesion, Figure 4. Currently lost to follow up 8 months after presentation to our facility. Clinical photograph of DFSP showing scarification marks. (a)-Clinical photograph of DFSP, (b)-chest X-ray-AP & lateral views, showing clear lung fields and soft tissue shadow. Clinical photograph of recurrent DFSP.

Discussion
Dermatofibrosarcoma protuberans comprises approximately 1% to 5% of all soft tissue sarcomas in adults and 18% of cutaneous soft tissue sarcomas. 14 In US, DFSP accounts for less than 0.1% of malignant neoplasm and approximately 1% of soft tissue sarcoma, 15 with annual incidence of 0.8–4.5 per million. 16 In this study, DFSP accounted for 7% of cutaneous malignancies which compares favorably with our previous study of 6.8%. 11 It is reported in all races with no racial predilection. 15 In this study there was a female preponderance with a M:F ratio of 1:2, this is in keeping with our previous study. 11 Several studies of DFSP reveal an almost equal sexual distribution or slight male predominance. However, a larger cancer registry of 2885 cases showed that females might have a slightly higher incidence.4,15 DFSP is reported to occur in adults aged 20–50 years and rarely reported in newborns and elderly individuals. 17 This compares with this study that reported the age range of 21–57 years with a mean of 36.5 years in keeping with our previous study with a mean age of 31.7 years (4th decade). However, the mean age could have been lower with age at first presentation as 50% of the patients presented late with recurrent lesions.
Chromosomal aberration contribute to the pathogenesis of DFSP. It involves a chromosomal fusion secondary to translocation between chromosomes 17 and 22. In over 90% of DFSP patients there is translocation that causes the upregulation of Platelet derived growth factor (PDGF) with subsequent tumour formation. The translocation represents the fusion of Collagen type1 Alpha1gene (COL1A1) on chromosome 17 and PDGFB gene on chromosome 22 that ultimately results in overproduction of PDGF, thus highlighting the rationale for the use of targeted therapy with Imatinib in the treatment of DSFP.11,18 In cases without the COLIA1/PDGFB translocation, a different chromosomal translocation still involving PDFGB on chromosome 22 has been demonstrated. 7 In 10–20% of patients with this tumour, trauma at the site seems to be incriminated15,16 as alluded to by some patients.
The infrequent occurrence of DFSP lessens their clinical awareness with diagnosis often made at histology. Commonly it presents as a firm protuberant mass on the trunk, proximal extremities, head and neck. 4 Initially mobile and later there may be fixation to deeper structures: fascia, muscle and bone. DFSP is a relatively uncommon soft tissue neoplasm with intermediate to low grade malignancy. It is a locally aggressive tumour with high recurrence rate 3 as demonstrated in 50% of the patients. This cutaneous malignancy that arises from the dermis invades deeper tissue: fat, fascia, muscle and bone. Most lesions occur over the trunk or proximal extremities,3,4,15 in keeping with the finding in this study. Other studies report that it rarely occurs above the neck and extremely rare on the breast. 19 Our earlier report revealed the Head and Neck as commoner than the extremities. 11 Late presentation was a common feature as traditional healers enjoy a lot of patronage in our setting with some who presented with complications of ulceration, pain, bleeding from large tumours 4 or huge fungated tumours from misdiagnosis and mismanagement. This was compounded by a similar experience in primary and secondary health care facilities often without facilities for histology. Despite this poor picture, none of the patients had regional lymphadenopathy or metastasis to the lungs. The six patients were all Stage 1 tumours.
The youngest patient with an upper extremity DFSP, a known Neurofibromatosis-1 (NF-1) patient presented with the largest tumour of 5 years duration. Notably both diseases involve aberrations in chromosome 17. NF-1 gene, a tumour suppressor gene that codes for Neurofibromin type 1 is also located on chromosome 17. Neurofibrosarcoma is a malignancy that occurs more frequently in patients with NF-1 though they may arise independently as earlier reported. 20 This is the first case of both entities (DFSP and NF-1) reported in the same patient in our facility with very few cases reported in literature. Both respond in some capacity to treatment with Imatinib. 18
DFSPs are great masqueraders as benign skin lesions and resembling other cutaneous malignant neoplasms4,7: lipoma, epidermal inclusion cyst, scars, dermatofibroma, neurofibroma, keloid, Kaposi sarcoma, cutaneous melanoma, metastatic cancer to skin, morphea including other soft tissue sarcomas and notably soft tissue leiomyosarcoma (LMS) of the extremities highlights the issue of a wide range of differential diagnoses and the need for preoperative histology including immunohistochemistry. 21 Peripheral LMS divided into cutaneous (dermal) and subcutaneous has been reported with the lower limb as a common site, thereby highlighting LMS as a differential diagnosis for DFSP affecting the limbs. 22
Summary of demographics, clinical, laboratory and treatment outcomes of patients.

WLE: wide local excision; CXR: chest X-ray; IHC: immunohistochemistry (not done); adjuvant therapy-nil. NF-1: neurofibromatosis-1.
*6 patients-7% of cutaneous malignancies.
Dai et al. 1 in a study of clinically relevant proteins of CD34, Vimentin, Ki-67, smooth muscle actin (SMA), muscle specific actin (MSA), S-100, Ckpan, Desmin, Bcl2, CD99 reported diffuse positivity for CD34, vimentin, SMA, MSA and S-100 including Ki-67. Notably, CKpan and desmin were negative. CD43 immunoreactivity in DFSP can be mistaken with other malignancies and even benign lesions. 4 Immunohistochemical staining for several potential targeted therapeutic indicators including enhancer of Zeste homolog2 (EZH2), epidermal growth factor receptor (EGFR), PDGF, programmed cell death (PD-L1) and vascular endothelial growth factor (VEGR) revealed positively expressed in some DFSP. Apatinib a novel VEGF receptor inhibitor has been shown to be a potential therapeutic option for metastatic DFSP. 1
Testing for the t (17; 22) translocation can be performed using Fluorescent in situ hybridization (FISH) or reverse transcriptase-polymerase chain reaction (RT-PCR). This is a useful screening tool for patients for targeted therapy. 7 MRI and FISH alongside with RT-PCR can be utilized for screening and the choice of the best treatment. 4
Treatment is primarily by surgical intervention; it is desirable that complete resection be achieved in the first attempt due to high risk of recurrence. 4 The standard for treatment of DFSP lesion is WLE with 2–4 cm clear margins down to and including fascia, though no universal recommendation for diameter in WLE has been established. 4 However, recent studies suggest Mohs micrographic surgery (MMS), the Gold standard is a better therapeutic option compared to wide local excision with lower rate of recurrence given the ability of DFSP lesion to be more widespread than apparent. 7
Non-surgical treatment is however indicated in cases of incomplete resection, recurrent, inoperable and metastatic lesions. Imatinib mesylate offer an alternative treatment option.25,26 This drug works by inhibiting the ATP binding to the PDGF receptor, a cell surface tyrosine receptor. Patient with plexiform neurofibroma in NF1 also have been successfully treated with Imatinib mesylate.27,28 Improved outcomes in locally advanced and recurrent DFSP with neoadjuvant treatment with imatinib facilitate resection in difficult tumours. 29 Imatinib is tolerated orally and does not appear to have a long term sequelae. Patients with highly infiltrative lesions are offered the opportunity of reducing their tumour size prior to surgery resulting in smaller postsurgical defect and less complicated scar. 29 DFSP is radiosensitive and Radiotherapy is a potential adjuvant therapy. 1 The issues with postoperative radiation are flap necrosis, oedema and delayed healing. 4 However, because of the infiltrating growth pattern of DFSP commonly extending beyond clinical margin, this accounts for high recurrence with tumour fascicles often interspersed with normal tissue in the secondary lesion. 30 Figure 4, demonstrates recurrence as most likely from residual tumour due to the above stated reasons, the scar tissue appears not to be involved in the recurrence which has been increasing in size. This patient is suitable for adjuvant therapy with imatinib. Multidisciplinary collaboration involving the surgery and medical oncologist, dermatologist, pathologist, plastic surgeon, radiation oncologist is indicated in locally advanced, recurrent and metastatic lesion (12).
Follow up (duration from surgery to last visit in clinic) was poor with an average period of 7 months (Table 1). This is a common and distressing feature in our setting partly attributed to poverty, cultural beliefs and high patronage alternative medical therapy. Long-Term monitoring is required in view of the peculiar tumour biology. Most recurrence occur within 3 years postoperative; recommended schedule for follow up is 3 monthly for 2 years, 6 months for 3 years and annually for life.7,15 In the light of the experience with poor follow up, recurrent lesions and late presentation with advanced lesions, adjuvant therapy with imatinib and radiotherapy should be included in the treatment plan of patients.
Overall prognosis is good with 10-years survival rate of 99.1%. 7 Morbidity due to local recurrence is a major challenge with metastasis rare. Risk of metastasis increase from incomplete resections and repeated surgical intervention. 4 We recorded no evidence of metastasis despite some large and complicated lesions. DFSP patients with metastatic disease live for an average of about 2 years from time of diagnosis. 7 Those older than 50 years are high risk with poor clinical outcome. 24 The risk associated with non-invasive DFSP is 0.5% while regional lymphadenopathy is a sign of poor prognosis. Histology with the features of fibrosarcomatous changes are poor prognostic indicator. 24 High mitotic rate, increased cellularity, black race, male sex and location on the head, neck or limb are risk factors for higher mortality rates. 7
Conclusion
Dermatofibrosarcoma protuberans is a rare and challenging lesion associated with significant morbidity associated with inadequate surgical treatment. This lesion presents as cutaneous swellings often misdiagnosed and mismanaged resulting in late presentation with large recurrent, sometimes haemorrhaging and fungated lesions with poor outcomes. Early presentation, diagnosis and treatment will improve outcomes. Inclusion of adjuvant therapy with Imatinib with or without adjuvant radiotherapy is recommended for inclusion in the treatment plan in view of the frequent morbidity of recurrence and frequent loss of patients to follow up.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
