Abstract
Peritoneal mesotheliomas are very rare tumors. Their prognosis is poor, average survival does not exceed 1 year after peritoneal cytoreduction. Systemic chemotherapy is considered to have no proven value in the management of peritoneal mesotheliomas. Objective responses with systemic chemotherapy are very rare. We report here a case of an advanced peritoneal mesothelioma which achieved an unexpected partial response with chemotherapy, allowing the patient to have a right colectomy. The patient was referred to a specialized center on HIPEC, but taking in account the long awaiting interval, the HIPEC was judged to be inefficient and then the poursuit of 6 cycles of systemic chemotherapy was decided. The patient is still alive without any symptom and with a good performance status at 59 months after diagnosis. Throughout our case, we provide an encouraging evidence of the role of initial systemic chemotherapy in the downstaging of initially unresectable primary malignant mesothelioma and in the improvement of overall survival.
Introduction
Peritoneal malignant mesotheliomas are rare and reputed to have a poor prognosis. 1 But since the advent of peritoneal cytoreduction associated with Hyperthermic Intraperitoneal Chemotherapy (HIPEC), their prognosis has significantly improved.2,3 Those therapeutics, offered as first-intention treatment, are nevertheless associated with high morbidity, essentially related to extensive cytoreduction. 4 As for systemic chemotherapy, it was considered without proven interest.
We report the observation of a man in whom a malignant mesothelioma has been diagnosed by biopsy during laparoscopy for exsudative ascites. The significant regression of the lesions then the stability during 30 months under systemic chemotherapy motivated a new exploratory laparoscopy, a colectomy, and then continuing the systemic chemotherapy. Our case is exposed and written according to the SCARE guidelines. 5 It illustrates the role of initial systemic chemotherapy in the downstaging of unresectable primary malignant mesothelioma and in the enhance of survival rate.
Case report
A 60-year-old male patient with no history of exposure to asbestos or any other cytotoxic agent was admitted to the Internal Medicine Department for exploration of a general condition deterioration and ascites of great abundance. The exsudative nature of his ascites suggested either peritoneal tuberculosis or carcinosis.
CT scan confirmed abundant ascites, and revealed a thickening of the digestive tract with a cake-like appearance dense fatty epiploic mass, but it was still not cutting across the diagnosis of carcinosis or peritoneal tuberculosis (Figure 1(a) and (b)).

(a and b) CT scan showing abundant ascites and a thickening of the digestive tract with a cake-like appearance dense fatty epiploic mass.
Koch bacillus’s test (mycobacterium tuberculosis test) results were negative and endoscopic examinations did not find any suspicious colic or gastric lesions.
An exploratory laparoscopy was therefore performed. It confirmed the presence of a great abundant ascites, a cake-like epiploic appearance under the liver, a thickening of the entire large omentum and diffuse lesional nodules throughout the digestive tract. An epiploic biopsy was performed, the histopathological examination was in favor of malignant peritoneal mesothelioma.
After discussion in a and in view of the significant extension of the lesions, a palliative systemic chemotherapy was decided.
The patient received 3 cycles of well tolerated full dose pemetrexed (500 mg/m2) and cisplatin (100 mg/m2) with a partial response according to RECIST1.1 criteria. Ascites has completely disappeared (Figure 2). It was decided to continue with the same regimen for three other cycles but those drugs could not be provided to the patient because of health insurance issues. In consequence, chemotherapy regimen was switched to paclitaxel (175 mg/m2) and carboplatin (AUC5) every 21 days. The patient received 3 cycles of this chemotherapy regimen. CT-scan showed stable disease, but our patient suffered from grade 3 peripheral neuropathy. A monochemotherapy with carboplatin (AUC 5) was then maintained for 5 cycles with no significant change on CT-scan (Figure 3). Otherwise, the patient performance status was improving.

CT scan after 3 cycles of chemotherapy (pemetrexed and cisplatine) showing a partial response.
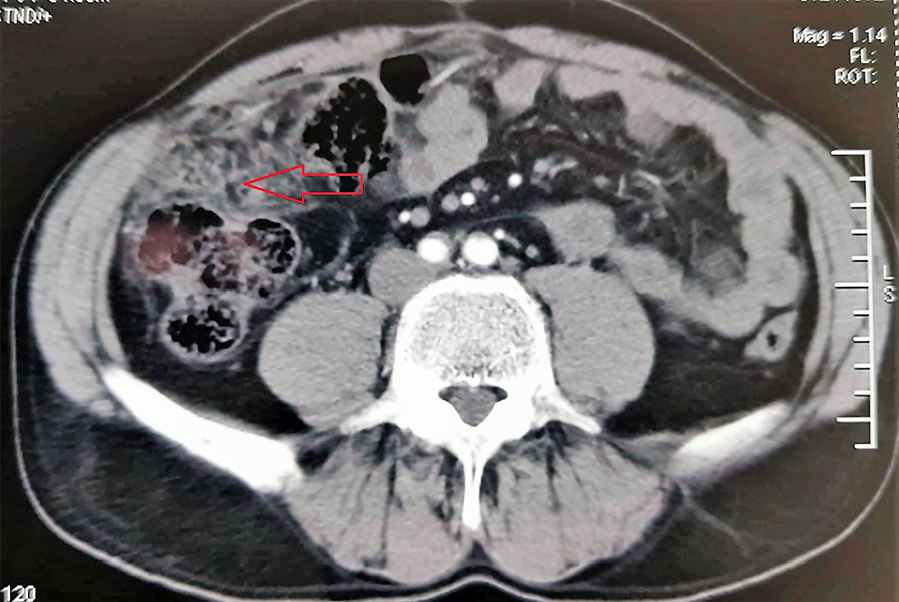
CT scan after 5 cycles of Carboplatine showing a stability of the epiploic mass (arrow).
At 2 years and a half from the beginning of the chemotherapy, the patient was in excellent general condition. As a result, a surgical procedure was discussed again in a multidisciplinary consultation meeting. Indeed, a second laparoscopy was performed. It showed no ascites or peritoneal nodules. Nevertheless, an epiploic mass adhering to the right colic flexure was found in the right hypochondrium and was judged clearly resectable. However, its mobilization under laparoscopy seemed to be difficult and entailed a risk of tumor rupture, hence conversion to laparotomy was chosen. Surgical procedures were monobloc resection consisting of right colectomy and epiploic mass resection (Figure 4). The surgical margins were macroscopically quite distant from the tumor.
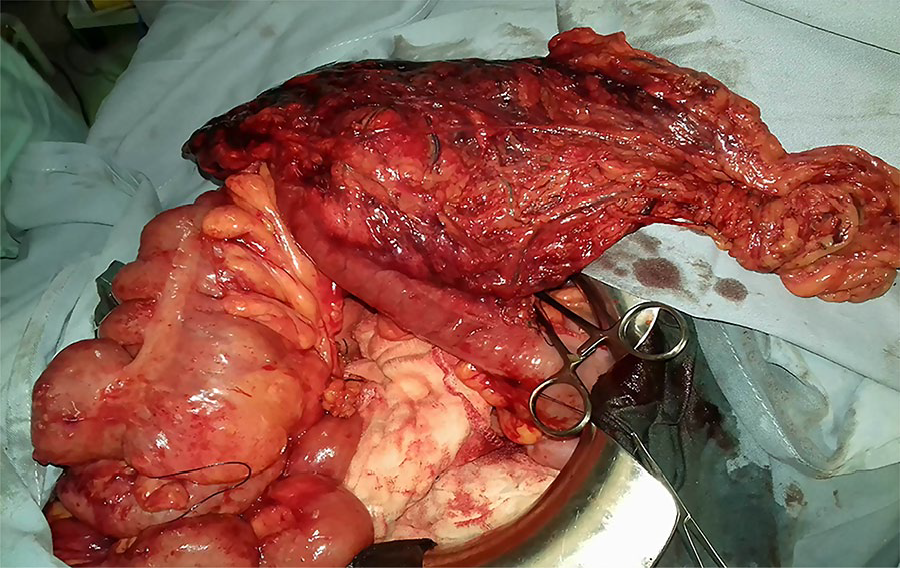
Right colectomy and epiploic mass resection.
Anatomopathological examination of the specimen confirmed the same histological nature (Figure 5). The immunohistochemical examination showed expression of carletinnie, mesothelin, and cytokeratin (Figure 6). The surgical margins were satisfactory.

Histological aspects of a malignant mesothelioma.

Immunohistochemical examination showing expression of carletinnie, mesotheline, and cytokeratin.
Hence, the case was discussed again in a multidisciplinary consultation meeting an HIPEC was indicated. The patient was referred to a specialized center on HIPEC, but taking in account the long awaiting interval, the HIPEC was judged to be inefficient and then the poursuit of 6 cycles of systemic chemotherapy was decided.
The patient was regularly followed at outpatient clinic and he underwent CT body scan every 6 months which didn’t show progression of his disease. At 5 years from diagnosis the patient remains in excellent general condition.
Discussion
Peritoneal mesothelioma represents 10% to 20% of all mesotheliomas. 1 Its relationship with asbestos exposure is less established than for pleural mesothelioma. Its incidence appears to be increasing in some countries. 6
The prognosis for peritoneal mesothelioma is poor, average survival does not exceed 1 year after peritoneal cytoreduction. 7
This prognosis has improved significantly since the advent of extended cytoreduction associated with HIPEC4,8 and has achieved more than 5 years of overall survival in the most recent series.9,10
However, extensive peritoneal cytoreduction followed by HIPEC is associated with high morbidity ranging between 30% and 50% and reaching 75% in some series. 4
This high morbidity is mainly due to extensive peritoinectomy. It would therefore be desirable to limit the hearing of macroscopic peritoneal lesions by neoadjuvant treatment.
The therapeutic decision can be based, as in our patient, on the results of laparoscopic exploration. 11 While extensive cytoreduction appears impracticable, systemic chemotherapy seems to be the best left option, although it was for a long time been considered disappointing in the treatment of malignant mesothelioma. 1
Indeed, a study published in 2013 using an Italian database of 105 patients, has shown that preoperative chemotherapy did not appear to improve neither survival nor the rate of complete resection compared to extended cytoreduction associated with HIPEC alone. 12 In 2008, a study showed a 26-months’ survival with a response rate at 15% under chemotherapy based on pemetrexed and gemcitabine. The maximum of overall survival reached in this study was 36 months. 13 Recently in 2017 a study involving 24 patients treated with pemetrexed and cisplatin has described two complete responses and nine partial responses with a median overall survival of 15.6 months 14
In a case report published in 2012, a 24-months’ survival was obtained thanks to three lines of chemotherapy based on pemetrexed and cisplatin. This was considered the most prolonged survival under chemotherapy alone. 15 Our patient had survived 59 months after two chemotherapy lines and is still alive after a right hemicolectomy alone.
These facts illustrate the importance of initial systemic chemotherapy in enhancing survival rates for cases of primary malignant mesothelioma initially judged to be unresectable.
Conclusion
To our knowledge, an overall survival of 59 months, with tumor stability and maintenance of an excellent performance status, has never been reported. We provided, throughout our case, an encouraging evidence for the use of systemic chemotherapy for patients with initially unresectable disease.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Our institution does not require ethical approval for reporting individual cases or case series.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Verbal informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
