Abstract
Low-grade fibromyxoid sarcoma is a rare soft tissue tumor which has been mostly reported in lower extremities; however, it can also occur in other parts of the body such as head and neck and abdominal wall, but its occurrence in the abdominal cavity and mesentery of bowel is an extremely rare event and has very rarely been reported. Herein, we report our experience with a 24-year-old lady with a huge mesenteric mass, turned out to be low-grade fibromyxoid sarcoma. This case is the largest one reported in the English literature. We will also discuss about the previously reported cases of low-grade fibromyxoid sarcoma in the English literature.
Introduction
low-grade fibromyxoid sarcoma (LGFMS) or Evans tumor has been described in 1987 by Evans as an indolent soft tissue tumor and potentially metastasizing tumor. 1 This tumor has distinctive histopathologic findings with bland morphology and an aggressive behaviour. 2 The most common location of this soft tissue tumor is lower extremities of young patients, especially thigh. It has been very rarely reported from other locations such as head and neck, lung and thorax, as well as intra-abdominal such as mesentery. 3 To the best of our knowledge, less than 20 cases of intra-abdominal and mesenteric LGFMS have been reported in the English literature in Evans. 4 Herein, we report our experience with a 24-year-old female with LGFMS of the small bowel mesentery.
Case report
A 24-year-old lady presented with abdominal pain and distension, since 1 month prior to admission. She had significant weight loss. However, except for abdominal bulging, no other positive finding has been detected in physical examination. She had positive history of two surgeries for hand and back lipoma.
Laboratory investigation showed anemia (Hemoglobin 9.2 g/L); however, all other hematologic and biochemical analyses were normal. All of the tumor markers were also normal. Sonography of the mass showed a heterogeneous mass in favor of malignant process (sarcoma).Computed tomography (CT) of abdomen showed a large multiloculated abdominal mass (50 × 30 cm) in the mesentery of small intestine (Figure 1).

Computed tomography of abdomen showed a large multiloculated abdominal mass (50 × 30 cm) in the mesentery of small intestine.
The patient has undergone surgery to excise the tumor. Complete excision of the tumor was performed from the mesentery of small bowel.
The received specimen in the pathology department was a huge mass with myxoid appearance (Figure 2). Microscopic sections of the tumor showed mostly bland fibroblasts with little atypia and lobular pattern in heterogeneous myxoid and collagenous stroma. Mitotic figures were low to intermediate (0–4/10HPF). No necrosis was present. Rare pericollagenous rosettes were identified (Figure3(a) and (b)). Immunohistochemistry was positive for vimentin and negative for BCl2, Desmin, S-100, smooth muscle action (SMA), c-Kit, beta-catenin, synaptophysin, and weakly positive for CD34. We did not have the set up for performing genetic study on the tumor specimen.
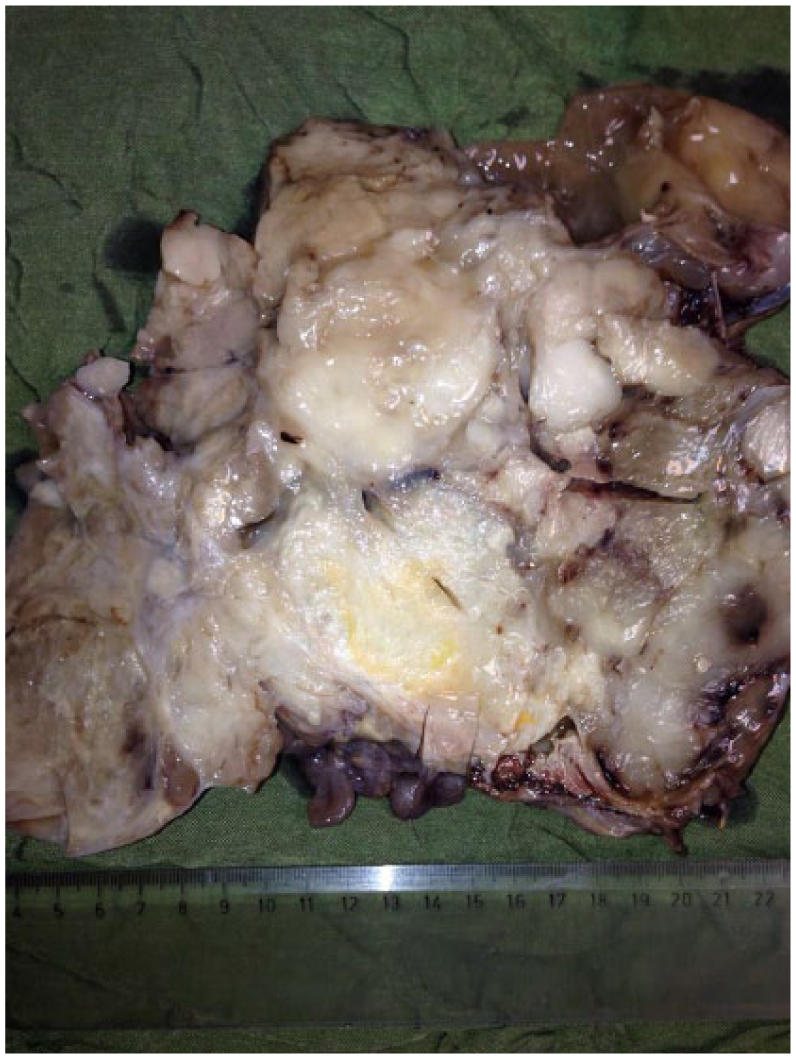
The received specimen in the pathology department was a huge mass with myxoid appearance.

(a) Microscopic sections of the tumor showed mostly bland fibroblasts with little atypia and lobular pattern in heterogeneous collagenous stroma (H&E × 250) and (b) Microscopic sections of the tumor showed mostly bland fibroblasts with little atypia and lobular pattern in heterogeneous myxoid stroma (H&E × 250).
The diagnosis of LGFMS was made and now after 6 months of follow-up after surgery no recurrence or metastasis has been detected. The patient is still under follow-up for early detection of recurrence or metastasis.
Ethical approval has been provided by the Ethical Committee of Shiraz University of Medical Sciences. The patient provided written and verbal informed consent for patient information and images to be published.
Discussion
LGFMS (Evans syndrome) is a rare soft tissue tumor, with paradoxical metastatic potential and benign morphologic appearance. It is characterized by distinctive heterogeneous myxoid and collagenous background and bland fibroblastic cell population. 4 It has been most frequently reported in young to middle-aged male patients.
The most common site of involvement is deep soft tissue of thigh; however, it has also been reported from head and neck, axilla, chest wall, and vertebra. 5 Occurrence of this tumor in the abdominal cavity and mesentery of intestine is an extremely rare event and to the best of our knowledge, only 17 cases of intra-abdominal (including gastrointestinal (GI) tract) and mesenteric LGFMS have been reported in the English literature. Table 1 shows the main characteristics of these 17 cases.
Characteristics of the 17 previously reported cases of LGFMS in the English literature.

LGFMS: low-grade fibromyxoid sarcoma; NR: not reported.
The most common presenting symptom has been abdominal mass and pain. 6 In the last 17 intra-abdominal reported cases, they have mostly presented in the young to middle age group (21–64 years of age).There has been nine males and eight females with intra-abdominal LGFMS.
Our case is the largest intra-abdominal LGFMS which has been reported and no case larger than 21 cm (8–21 cm) has been reported so far. 7
Diagnosis of this tumor by ultrasonography shows multilobular hypoechoic mass. CT imaging shows well-demarcated multilobular hypodense to muscle density mass. Fibrous component is similar to muscle and myxoid component is similar to water with low attenuation and hypointensity. Magnetic resonance imaging (MRI) identifies both fibrous and myxoid components of this rare intra-abdominal sarcoma.9,14,15 There are many differential diagnoses in imaging such as myxoid liposarcoma, myxofibrosarcoma (myxoid malignant fibrous histiocytoma), gastrointestinal stromal tumor (GIST), desmoid tumor, hemangioma, solitary fibrous tumor, and neurogenic tumor. Therefore, it is difficult to distinguish these tumors on CT and MRI scans. 9
Gold standard for the diagnosis of this tumor is histopathology, showing low to moderately cellular tumor with whorling pattern of tumor cells, composed of alternating myxoid and collagenous areas. 16 Pericollagenous rosettes with cells around a collagenous center can also be seen. 4
Differential diagnoses in histopathology of this tumor are sarcomas with mixed components of myxoid and fibroblastic cells such as myxoid liposarcoma, which contains myxoid and lipomatous components and also lipoblasts, which are not seen in LGFMS. 10 Other differential diagnoses are fibromatosis, perineuroma, neurofibroma, and myxofibrosarcoma. None of these soft tissue tumors contain collagenous rosettes which is characteristics of LGFMS. 11
Immunohistochemical study of LGFMS is not characteristic and shows only constant positivity for vimentin and occasional positivity for CD34. 2
In addition to morphology and immunohistichemistry, cytogenetic study and presence of translocation in chromosome 7, 16 t(7;16)(q34;p11), that is, FUS-CREB3L2 fusion gene can confirm the diagnosis, because it has been reported in >90% of the cases of LGFMS. 15
Another important point in this soft tissue tumor is its homology with hyalinizing spindle cell tumor with giant rosettes (HSCT) which has been proved to have the same fusion gene and translocation. There are controversial reports about this issue and some authors believe that HSCT is a variant of LGFMS with giant collagenous rosettes, but others separate these two tumors by the presence of epithelioid cells in HSCT. 16 Overall, metastasis has rarely been reported in HSCT, which is indicative of better prognosis of this tumor comparing with LGFMS. 17
The best treatment for LGFMS is surgery and excision of the tumor with long term follow up for detection of recurrence and late metastasis. Aggressive surgery and completeness of excision is a very important part of treatment and significantly decrease the risk of metastasis. 17
Conclusion
According to our experience with this case report, LGFMS should be included in the differential diagnoses of intra-abdominal sarcomas.
Footnotes
Conflict of interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Both verbal and written consent has been provided from the patient.
