Abstract
Background:
Lower extremity amputation (LEA) is defined as the complete loss in the transverse anatomical plane of any part of the lower limb. The objective of this study is to look at the trend and mortality trend of LEA performed in diabetes patients from 2008 to 2013.
Methods:
All patients age 15 and above with diabetes mellitus who had undergone LEAs (both major and minor) in Tan Tock Seng Hospital, Singapore from 1 January 2008 to 31 December 2013 were included. The outcomes of interest were deaths from all causes within 30 days and within 1 year.
Results:
Major LEA rate has increased from 11.0 per 100,000 population in 2008 to 13.3 per 100,000 population in 2013. The 30-day mortality rate ranges from 6.0% to 11.1% and the 1-year mortality rate ranges from 24.3% to 30.6%. Minor LEA rate has increased from 10.8 per 100,000 population in 2008 to 13.9 per 100,000 population in 2013. The 30-day mortality rate ranges from 1.5% to 3.7% and the 1-year mortality rate ranges from 9.7% to 18.3%.
Conclusions:
The trends in major and minor LEA are increasing. The 30-day and 1-year mortality for both major and minor LEA are comparable to figures reported worldwide. There is a need to re-look at preventive strategies to reduce LEA in diabetes patients in Singapore.
Introduction
Lower extremity amputation (LEA) is defined as the complete loss in the transverse anatomical plane of any part of the lower limb. LEA is performed to remove ischemic, infected, necrotic tissue or locally unresectable tumors. LEA can be divided into major (above ankle, through knee and up to hip amputations) and minor (foot and toes) amputations.
Patients with diabetes mellitus have a 10-fold higher risk for LEA compared with the general population. 1 In Singapore, it was reported in 2001 that approximately 700 LEAs were performed in patients with diabetes annually. 2 The current figures stand at 1500 LEAs annually in Singapore due to complications arising from diabetes mellitus. 3 Diabetes mellitus is also likely to cause patients to become severely disabled, to experience their initial amputation at a younger age (71.9 with diabetes versus 78.8 without diabetes), progress to higher level amputations and die at a younger age. 4
The prevalence of diabetes mellitus in Singapore has increased from 8.2% in 2004 to 11.3% in 2010 5 and is projected to increase to 15% in 2050. 6 Furthermore, it was found that 20% of adult diabetes patients in Singapore were diagnosed below the age of 40 years, 7 implying longer duration of disease and greater risks of LEA. Thus the burden of diabetes and LEA is likely to increase in the future. A recent study in Singapore also reported that the mean total direct costs per year of minor and major amputations were SGD $5161 and SGD $9695, respectively. 8 These costs exclude government subsidies which can be as high as 80% if the patients choose to stay in the highly subsidized wards of the public hospitals (Class C Ward). If indirect costs are included, the burden to society will be much higher than reported.
The prognosis of LEA is poor, especially in patients with diabetes mellitus, with the 1-year mortality rate ranging from 11.3% to as high as 50.2%4,9–11 in developed countries. However, there is limited data in the literature on the 1-year mortality of diabetes patients with LEA in Singapore.
The objective of this study is to look at the trends in 30-day and 1-year mortality rates for diabetes patients with LEA from 2008 to 2013. This will help estimate the burden of diabetes-related LEA and thus help plan for clinical services to cater for these patients in Singapore.
Methods
Data sources
We obtained data from the National Healthcare Group Diabetes Registry, 12 which was launched in 2007. All patients age 15 and above with diabetes mellitus that had undergone LEAs (both major and minor) in Tan Tock Seng Hospital from 1 January 2008 to 31 December 2013 were included. Tan Tock Seng Hospital is Singapore’s second largest acute care general hospital with over 1500 beds, 40 clinical and allied health departments, and 16 specialist centers. The hospital sees over 2000 patients at its specialist outpatient clinics and some 460 patients at its emergency department every day.
Identification of patients
To ensure comprehensive capture of all diabetes patients into the registry, the following rules, ranked in descending order, were used:
Rule 1, patients from existing standalone diabetes registries;
Rule 2, patients with diagnosis code of 250 (250.0–250.9) under the International Classification of Diseases, 9th Revision, Clinical Modification (ICD9CM), coded as either the primary or secondary diagnosis;
Rule 3, patients on anti-diabetes medication; and
Rule 4, patients with 2-hour blood sugar level of ⩾11.1 mmol/l on oral glucose tolerance test, or a random blood sugar level of ⩾11.1 mmol/l on two occasions within 2 years, or fasting plasma glucose ⩾7.0 on two occasions within 2 years, or random blood sugar level of ⩾11.1 mmol/l and fasting plasma glucose ⩾7.0 within 2 years. 11
Patient characteristics include age, gender, ethnicity, type of housing, marital status, comorbidities (hypertension, dyslipidemia, chronic kidney disease), and glycated hemoglobin.
Mortality data was obtained from the hospital records as well as the relevant local death registry, and the outcomes of interest were deaths from all causes within 30 days and within 1 year. The data extracted was until 31 January 2015.
Statistical analysis
Categorical variables were described using proportions (%) and continuous variables were described using mean and standard deviation (SD).
Crude rates for LEA were estimated by dividing the number of LEA done in each year in Tan Tock Seng Hospital by the population that Tan Tock Seng Hospital is responsible for (Ang Mo Kio, Bishan, Geylang, Hougang, Kallang, Novena, Rochor, Serangoon and Toa Payoh).13,14 Crude rates are presented as number of amputations per 100,000 population. Age-sex standardized rates were calculated using the Organization for Economic Co-operation and Development (OECD) 2010 population.
The trend for major amputations was assessed separately from minor amputations as minor amputations of the toes may be a result of improved patient surveillance and early detection of conditions that could otherwise require major amputations. 15 Linear regression was done to test for statistical significance in trend.
All analyses were conducted using STATA (StataCorp, College Station, TX, USA) statistical software, version 12.1. The study was approved by the NHG’s Domain-specific Ethics Review Board which is an independent committee constituting of medical, scientific and non-scientific members.
Results
Baseline characteristics
Baseline characteristics of patients with first LEA between 2008 and 2013 are shown in Table 1.The mean age of patients who underwent major and minor LEA is 65.8 years and 62.0 years, respectively. A higher proportion of those who underwent minor LEA is male (66.9%) compared with those who underwent major LEA (59.5%). Malays and Indians which represent 13.4% and 9.1% of the resident population in Singapore, 16 respectively, are over-represented in this study. Compared with patients who underwent minor LEA, patients who underwent major LEA had a higher proportion of comorbidities. In addition, the mean HbA1c in patients who underwent minor LEA was higher than for those who underwent major LEA.
Characteristics of diabetes patients with first LEA between 2008 and 2013.

LEA: lower extremity amputation; SD: standard deviation; CKD: .
LEA rates
The crude rates of LEA (major and minor) are shown in Figure 1. Minor LEA rate has increased from 10.8 per 100,000 population in 2008 to 13.9 per 100,000 population in 2013 (
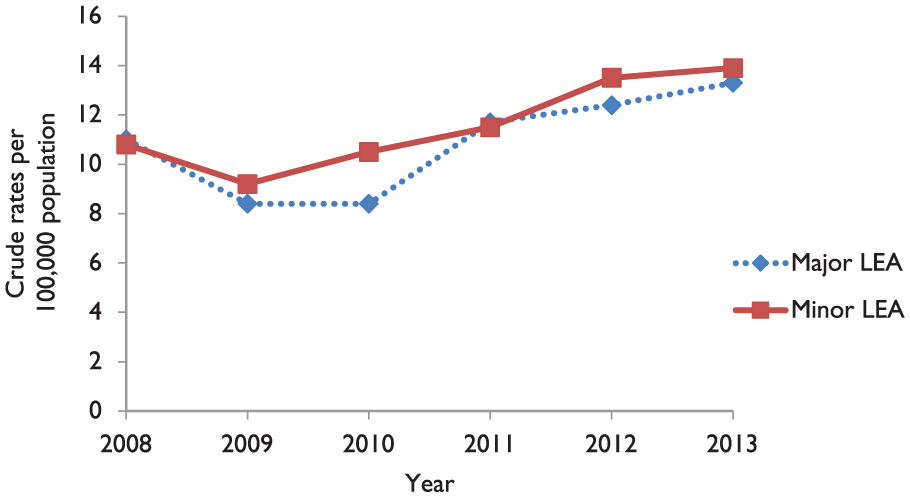
Crude rates of lower extremity amputations (LEA).
Mortality
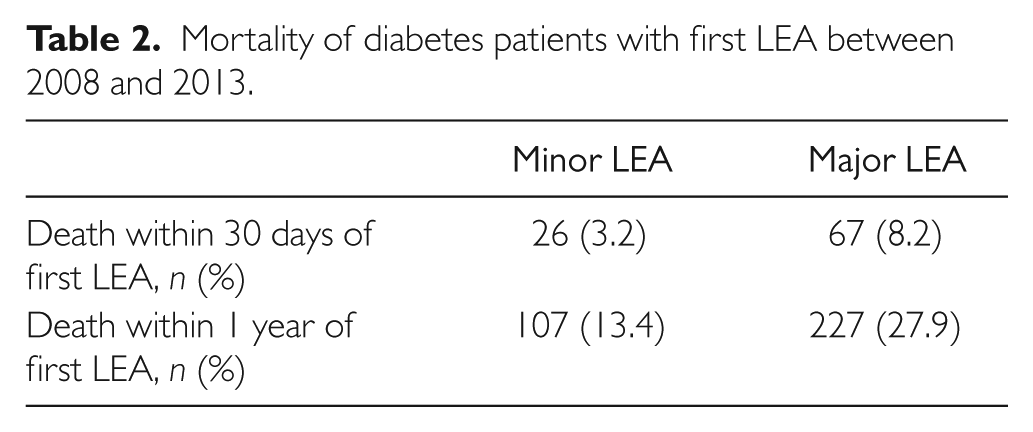
Patients who underwent minor LEA had a much lower 30-day mortality rate compared with patients who underwent a major LEA (Table 2). For minor LEA, the 30-day mortality rate ranges from 1.5% to 3.7% and the 1-year mortality rate ranged from 9.7% to 18.3% (Figure 2). For major amputations, the 30-day mortality rate ranges from 6.0% to 11.1% and the 1-year mortality rate ranges from 24.3% to 30.6% (Figure 2).
Mortality of diabetes patients with first LEA between 2008 and 2013.
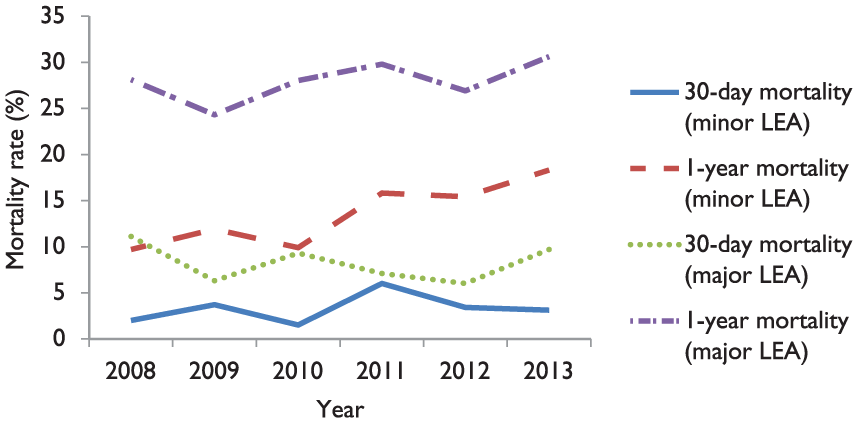
30-day and 1-year mortality for patients with LEA from 2008 to 2013.
The principal causes of death for minor and major LEA patients within 1 year of first LEA were similar, with ischemic heart diseases (26.9–28.0%), pneumonia (18.7–22.9%), diabetes mellitus (10.3–12.8%) and cerebrovascular diseases (6.2–7.5%) as the top four principal causes of death.
Discussion
Our data shows an increasing trend of LEA performed in diabetes patients from 2008 to 2014. The annual number of diabetes patients with LEA performed in Singapore resident population is approximately 934 in 2013 (obtained by applying the 2013 major and minor amputation rates in Tan Tock Seng Hospital to the resident population of Singapore aged 15 years and above), which is a 33.4% increase over the 700 LEA reported in 2001. 2 The age-sex standardized rate of major LEA in Singapore in 2013 was 14.8, which would put Singapore only below Israel and Slovenia among countries in the OECD. 17 Even if the amputation rate remains constant, we will still be facing increasing workload in managing these patients due to an increase in the number of diabetes patients over time. 6
The 30-day mortality for patients who underwent major or minor LEA is comparable to international figures of 4–22% reported in literature. 18 The 1-year mortality for patients who underwent major or minor LEA is comparable to international figures of 10–50% reported recently. 19 There is no clear trend in both the 30-day and 1-year mortality rates from 2008 to 2013 in our study.
Compared with the general population where the principal causes of death between 2008 and 2013 are cancer (28.5–30.5%), ischemic heart disease (15.5–20.1%), pneumonia (13.9–18.5%) and cerebrovascular disease (8.0–9.3%), a higher proportion of patients with LEA died from ischemic heart disease. Aggressive treatment of cardiovascular risk factors, if present, may be helpful to reduce these deaths. 20
Our study also found that the mean ages of patients undergoing major (65.8 years) and minor amputations (62.0 years) are younger than those found in many overseas studies.4,9-11 Our data showed that 51.2% of patients who underwent minor LEA and 40.8% of patients who underwent major LEA were aged less than 62 years. As the official retirement age in Singapore is 62 years, 21 patients who are still economically active but who have undergone an LEA will incur direct medical costs, as well as indirect costs from loss of productivity/salary. Thus preventive strategies for LEA, especially in younger patients, will have a positive impact on the reduction in the total cost from the societal point of view in Singapore.
Our study had overrepresentation of Malays and Indians compared with the population structure of Singapore, which is similar to earlier studies on LEA done in Singapore.22,23 This overrepresentation is a consequence of the higher proportion of diabetes patients from Malay and Indian ethnicities in Singapore. 5 Thus interventions to raise awareness about diabetes and its complications need to take into account the ethnic and cultural differences in the target populations to achieve reduction in LEA rates.
We also found that the mean HbA1c of patients who underwent major (8.6%) or minor LEA (9.2%) is higher than 7.0%, which is the target for most adults with type 1 or type 2 diabetes mellitus. 24 A meta-analysis has showed that high level of HbA1c is an important risk factor for LEA in patients with diabetes. 25 This suggests the need to optimize the glycemic control of diabetes patients to reduce LEA rates.
The strengths of this study are as follows: (1) the data was obtained from a large administrative database with accurate measurement of endpoints such as mortality; 13 (2) we have looked at a relatively long period (2008–2013) which will enable us to obtain stable mortality rates, as year-to-year variation may cause the rates to vary; and (3) the cause-of-death data was accurately captured from local death registry as well as in-hospital medical records.
This study suffers from certain limitations. This is a retrospective study and variables not captured at the start of the study would not be able to be used for analysis. We have looked at the LEA rates and mortality trend of only one tertiary hospital which may not be representative of all the hospitals of Singapore. As the population that Tan Tock Seng Hospital is responsible for could also have LEA done in other hospitals, the LEA rates calculated in this study are likely to be an underestimate.
Across the spectrum from pre-diabetes, to diabetes to the development of diabetes-related complications, there is a need to increase awareness of the benefits of preventive strategies in Singapore. One such strategy can be to improve the annual uptake of foot-screening rates of diabetes patients in Singapore, which has been shown to range from 53.0% to 69.5%. 26 This will help in detecting diabetic foot ulcers, and early treatment may help in preventing the need for LEA.
Footnotes
Declaration of conflicting interests
None declared.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
