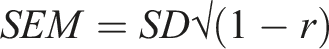Abstract
Background
Condition-specific measures of Health-Related Quality of Life (HRQoL) are more sensitive than generic tools. Sizing Them Up (STU) is a parent-proxy, obesity-specific HRQoL measure which was found to be reliable and valid internationally, but has yet to be utilised in Singapore.
Objectives
Our study aims to i) validate STU in adolescents seeking obesity therapy in KK Women’s and Children’s Hospital (KKH); and ii) determine demographic factors associated with STU scores.
Methods
We recruited 91 adolescents aged between 11 and 17 years old and their parents from KKH between June 2022 and January 2023. Parents completed STU and the generic Pediatric Quality of Life Inventory (PedsQL) upon recruitment, and repeated STU at least 2 weeks later.
Results
65% of participants were males, with a mean Body Mass Index (BMI) of 32.3 ± 5.1 kg/m2 and mean age of 13.6 ± 1.8 years old. STU demonstrated strong internal consistency (overall Cronbach’s α = 0.85) and moderate test-retest reliability (intraclass correlation coefficients = 0.30-0.70). There was high correlation between STU scores and i) the adolescents’ BMI; and ii) equivalent domains of PedsQL, suggesting moderate to strong construct and convergent validity respectively. Indian adolescents, lower parental education level and single parents were associated with poorer STU scores.
Conclusion
STU is a reliable, valid obesity-specific HRQoL measure in a local clinical population of adolescents undergoing obesity therapy, and can help clinicians to understand parents’ impression of the impact of obesity on their child. Knowing the demographic variables associated with STU can enable clinicians to identify adolescents whose HRQoL are disproportionately affected by obesity.
Introduction
Paediatric obesity is a growing public health problem both internationally and in Singapore. 16% of Singaporean school-going children and adolescents aged between 7 and 18 had overweight and obesity in 2021, up from 11% in 2013.1,2 While the medical complications from obesity are well-characterised amongst Singaporean adolescents,3,4 more needs to be understood about the obesity-related psychosocial complications. Adolescents with obesity in Singapore5,6 and overseas7,8 have reported poorer Health-Related Quality of Life (HRQoL) than their healthy weight peers. Furthermore, adolescents with obesity were observed to experience significant social and economic disadvantages later in life that could not be explained by their medical conditions, including lower educational attainment and household income. 9 Paediatric obesity also increases the burden for society with higher direct medical expenditure and indirect costs from lower productivity and psychosocial problems. 10 In line with Singapore’s shift towards a greater emphasis on preventive care under the nationwide Healthier SG initiative, effective timely management of adolescent obesity will be crucial to prevent its negative sequelae in adulthood. Consequently, beyond improving weight status and cardiometabolic health as part of adolescent obesity management, understanding the impact of obesity on the adolescents’ HRQoL will also be vital to inform interventions that can mitigate the psychosocial complications.
For the paediatric population, HRQoL is typically self-reported or assessed through parent-proxy reports. 11 Parents are important stakeholders in obesity treatment for adolescents, particularly in initiating access to medical services, 12 ensuring compliance with therapy, 13 and influencing their child to make healthier dietary choices and increase physical activity. 14 Parents also play significant roles in shaping their child’s self-esteem and providing psychosocial support. 15 However, these will first require them to have a good understanding of their child’s psychosocial functioning. Caregivers who reported poorer HRQoL for their child were shown to be more concerned about their child’s obesity and in turn more likely to seek medical attention for childhood obesity, independent of the child’s actual weight. 16 Yet, the agreement between parent-proxy and adolescent-reported HRQoL has been shown to be low to moderate, with parents being poor proxy for adolescents’ perception of HRQoL.5–7,17–22 It is therefore crucial that clinicians elicit parental perceptions of the impact of obesity on their child’s psychosocial health to correct any misconceptions that the parents may have for better parental engagement and effective obesity management.
In order to better understand the perceptions of Singaporean parents, there is first a need for locally validated parent-proxy HRQoL questionnaires, due to potential cultural differences in the expectations of local parents compared to those overseas. It has been argued that the perception of well-being in more individualistic societies in the West is different from that in collectivistic societies in Asia. 23 Such cultural nuances may also explain the differences in parent-proxy generic HRQoL scores of local adolescents with obesity vis-à-vis their counterparts in the United States. 6 Even within Singapore, a past study found significant differences in the HRQoL reported by adolescents of the three major racial groups that are independent of their health status or socio-economic level, suggesting strong cultural influences in HRQoL evaluation. 24
In past studies involving adolescents with obesity in Singapore, parent-reported HRQoL were mainly assessed using the generic Pediatric Quality of Life Inventory (PedsQL).5,6,25 Generic HRQoL tools allow for comparisons across diseases, as well as between individuals with and without a particular condition. For instance, adolescents with obesity reported poorer PedsQL scores than peers with diabetes mellitus and asthma, 26 contextualising the severity of the psychosocial complications of obesity against other chronic conditions. However, a systematic review found that condition-specific HRQoL instruments may be more responsive to therapeutic changes in HRQoL in randomised controlled trials as compared to generic tools. 27 In addition, condition-specific tools allow attribution of the reported scores to a specific disease state. Hence, there are benefits in using both generic and condition-specific HRQoL questionnaires clinically as well as in research. The Impact of Weight on Quality of Life Questionnaire (IWQOL) – Kids 28 and Sizing Me Up 29 are examples of self-reported, obesity-specific HRQoL tools which contextualise the reported HRQoL to the child’s weight and allow early detection of potential weight-related problems. Whereas for parent-reported HRQoL measure, Sizing Them Up (STU) has been validated in the United States 30 and Taiwan, 31 but has never been utilised in Singapore to the best of our knowledge.
Beyond determining local parents’ perceptions using the STU, it will be useful to determine factors correlated with poor STU scores, as these can direct interventions to improve the adolescents’ HRQoL. A study in the United States found differing scores on multiple STU domains between African-American and Caucasian adolescents even after adjusting for Body Mass Index (BMI), 30 but it remains to be seen if similar trends will be observed in our local ethnic groups. Studies using generic HRQoL measures have shown mixed findings regarding the psychosocial well-being of adolescents with obesity of different gender and socioeconomic status, 7 suggesting the need for further studies to clarify the association of these factors with the adolescents’ HRQoL. While parental obesity has been associated with higher risk of adolescent obesity, 32 the link with the adolescents’ HRQoL is less studied and can support current recommendations to address parental obesity as part of the management of adolescent obesity. 33
Given the gap in local literature on obesity-specific HRQoL and the importance of parental perceptions of the child’s HRQoL in determining their child’s access to healthcare services, we aim to evaluate the application of the STU in our local context to inform future clinical use. Our study aims to i) validate the parent-proxy, obesity-specific STU in Singaporean adolescents seeking obesity therapy in KK Women’s and Children’s Hospital (KKH) by determining its internal consistency, test-retest reliability, construct validity, and convergent validity through comparison with the widely used generic PedsQL; and ii) establish demographic factors that are associated with poorer STU scores. Our hypotheses are that the STU will show good internal consistency, test-retest reliability, construct validity and convergent validity with the PedsQL, and factors such as the adolescents’ race, gender, parental weight status and family’s socioeconomic status (represented by monthly household income, parental marital status, and parental education level) will be correlated with their STU scores. As STU is the first weight-specific HRQoL measure to be applied in our local population, convergent validity is determined using the PedsQL as reference, which was a common reference in overseas validation of the STU.30,31
Methods
Recruitment
Eligible adolescents and their parents were recruited from the Weight Management Clinic of KKH between June 2022 and January 2023. Inclusion criteria included adolescents aged between 11 and 17 years old who were on follow-up with the Weight Management Clinic for overweight or obesity (i.e. BMI at the 90th centile or more for gender and age based on Singapore’s growth charts). This age range was chosen to represent the bulk of the children being managed under KKH’s Weight Management Clinic. Parents who were unable to independently complete the questionnaires in English were excluded from the study. Written informed consent was obtained from all participants’ parents or legal guardians as well as adolescents aged 13 and above, while those aged 11 or 12 provided their assent. Ethical approval was obtained from the SingHealth Centralised Institutional Review Board. All participants received standard care with their paediatrician at the Weight Management Clinic for the period of the study, including dietary and physical activity counselling, monitoring of metabolic complications as well as pharmacotherapy as necessary. 4
Demographic and HRQoL questionnaires
Recruited parents or legal guardians completed a demographic survey, with questions about their marital status, educational qualifications, household income, as well as the self-reported height and weight of both parents. They also completed STU and PedsQL at the start of the study and repeated STU at least 2 weeks later for test-retest reliability, in line with the assessment interval used in the STU validation in United States 30 and that commonly used for other HRQoL tools. 34 To improve response rate for the retest, two text reminders were sent to the parents to remind them to complete the retest questionnaire online, or a member of the study team would attempt to meet the parents face-to-face if they had other appointments in KKH after the 2-week interval.
STU specifically assesses the impact of the adolescents’ weight, size, or shape on various aspects of their daily activities. Parents were asked to evaluate their child’s emotional functioning (7 questions), physical functioning (5 questions), experience of teasing or marginalisation (3 questions), positive attributes (4 questions), mealtime behaviour (2 questions), and school behaviour (1 question) in the past month across 22 questions using a four-point Likert scale (“never”, “sometimes”, “often”, “always”). Parents of adolescents aged 14 and above further completed six additional questions under the adolescent developmental adaptation module, which asked about the effects of their child’s weight on their dating and job search experiences. Scaled scores were calculated for each of the six scales (or seven including the adolescent developmental adaptation module), and a total QoL score was determined (excludes the adolescent developmental adaptation module) based on scoring guidelines by the STU authors. Each STU scale and the total QoL can be scored between 0 and 100, with higher scores indicating better psychosocial health. 30 However, no cut-off has been identified in literature as the threshold for good well-being, which could potentially pose as a challenge in interpreting the HRQoL scores. The STU was chosen over other obesity-specific HRQoL for our study as it has been validated in another Asian population in Taiwan 31 and may be hence more transferable to our local context.
PedsQL 4.0 evaluates the adolescents’ physical, emotional, social, and school functioning in the past month across 23 questions and can either be self- or parent-reported. In our study, parents rated their child’s functioning on a five-point Likert scale for each question (“never a problem” = 100 points, “almost never a problem” = 75 points, “sometimes a problem” = 50 points, “often a problem” = 25 points, “almost always a problem” = 0 points). An average score was then derived for each of the four domains, while the Psychosocial Health Summary score was the mean score across the emotional, social, and school functioning domains. The domain and summary scores were derived based on the scoring guidelines developed by the PedsQL authors, which were similarly applied in past studies and will allow for comparison of scores across populations. Similar to the STU, there is no pre-determined cut-off values but scores closer to 100 reflect better psychosocial well-being. 35 Ooi’s study of a community and clinical sample of adolescents with obesity has found good internal consistency of the parent-reported PedsQL in Singapore, with Cronbach’s α of 0.92 to 0.93. 5
Medical records
We extracted information regarding the adolescents’ anthropometry (height, weight, waist circumference, body fat percentage) and blood pressure measurements from their electronic medical records where available. The adolescents’ BMI percentage of the 95th percentile BMI (BMI95pct) was then calculated using age- and gender-specific Centers for Disease Control and Prevention (CDC) growth charts. 36 It has been shown that BMI95pct allows for better weight status differentiation when comparing children or adolescents with BMI in the extreme upper values. 37
Statistical analysis
Data analysis was carried out using STATA software version 17.0 for Windows (StataCorp, Texas, USA). Descriptive statistics were represented by means, standard deviations (SD) and percentages. The minimum clinically important difference (MCID) for each STU scale and total QoL score is defined as 1 standard error of measurement given by the formula below, where SD refers to the standard deviation of the baseline scores and r refers to the test-retest reliability coefficient of each scale.
38
Internal consistency of the STU was determined via Cronbach’s α for the overall STU questionnaire and each STU scale, with α ≥ 0.70 conventionally used to denote good internal consistency. 30 Intraclass correlation coefficients (ICC) were derived to establish test-retest reliability. ICC ≥0.90, 0.75≤ICC <0.90, 0.50≤ICC <0.75 and ICC <0.50 generally suggest excellent, good, moderate and poor reliability respectively, 39 though it should also be noted that varying time intervals between test and retest in different studies may affect the evaluation and comparability of reliability measures.
Multivariable linear regression was used to establish the association between STU scores and the adolescents’ i) BMI95pct to determine construct validity, and ii) race, gender, parental weight status (high-risk BMI in adults is defined as BMI ≥27.5 kg/m2 in Singapore), 40 monthly household income (median monthly household income from work for Singapore resident households was approximately $10,000 in 2023), 41 parental marital status, and parental education level (post-secondary qualifications refer to GCE ‘A’ levels, diploma, degree and above) as per our secondary aim. These demographic variables were chosen as they have been found in past literature to have a correlation with HRQoL and childhood obesity, including gender and parental income or education.7,8 Assessing social determinants of health are also recommended in clinical practice guidelines 42 as important considerations in assessment of childhood obesity. Variables are considered to be significantly associated with STU scores if the 95% Confidence Interval (CI) of its beta coefficient in the multivariable linear regression does not cross 0. Spearman correlation was used to compare the scores of equivalent domains in STU and PedsQL for convergent validity. Correlation coefficients ≥0.70 and <0.50 denote high and low correlation respectively, while correlation coefficients in between typically indicate moderate correlation. 43
To ensure data integrity, multiple members of the study team were involved in data entry, data reliability checks and data analysis, including counterchecking data with extreme values.
Results
Baseline participant characteristics
All adolescents who meet the age criterion were approached in KKH’s Weight Management Clinic by a member of the study team. Of 177 adolescents approached, 99 adolescents and their parents consented to participate, with 91 adolescents included in the final analysis (Figure 1). 1 participant who had missing responses in the HRQoL questionnaires despite text reminders was removed from the analysis, so as to allow for accurate calculation of the HRQoL scores. Flow diagram of participants.
Baseline characteristics of participants and their parents or legal guardians.

*Continuous variables were presented as mean ± standard deviation (SD), while categorical variables were presented as frequency (%).
Baseline characteristics of the parents or legal guardians of participating adolescents are also summarised in Table 1. Most of the parents answering the questionnaires were mothers. 67% of participating parents had post-secondary educational qualifications.
Parent-reported STU scores
Mean scores for each STU scale at the start of the study and during retest, and Cronbach’s α, test-retest reliability and minimum clinically important difference for each scale.

Internal consistency of STU
STU demonstrated strong internal consistency with an overall Cronbach’s α of 0.85. Individual scales had Cronbach’s α ranging between 0.52 (positive attributes scale) and 0.89 (emotional scale), as shown in Table 2.
Test-retest reliability of STU
Baseline characteristics of adolescents whose parents completed vs did not complete the repeat STU questionnaire.

*Chi-square test was used for categorical variables (presented as frequency, %) and two-sample t-test for continuous variables (presented as mean ± standard deviation).
Construct validity of STU
Regression coefficients b (95% confidence interval) from the multivariable linear regression with each STU scale.

Statistically significant p values (p < 0.05) in
Convergent validity of STU
Spearman correlation coefficients between STU and equivalent domains in PedsQL (Parent).

Association of STU scores with demographic variables
In the multivariable regression model (Table 4), Indian adolescents were rated more poorly by their parents in the school behaviour scale (regression coefficient = −8.0, 95% CI: −15.9 to −0.2, p = 0.045) as compared to their Chinese peers. Parents who have educational qualifications at or below secondary level also reported significantly poorer scores for their adolescent in the school behaviour scale as compared to parents with higher educational qualifications (regression coefficient = −5.8, 95% CI: −10.4 to −1.2, p = 0.014). Compared to dual parent households, single parents reported lower scores for their child under teasing or marginalisation (regression coefficient = −12.9, 95% CI = −22.9 to −3.0, p = 0.012), mealtime behaviour (regression coefficient = −15.4, 95% CI = −30.5 to −0.2, p = 0.047) and total QoL (regression coefficient = −8.7, 95% CI: −16.6 to −0.9, p = 0.029).
Discussion
Validation of STU
Our study demonstrated that STU has strong overall internal consistency, moderate test-retest reliability, good construct validity when correlated with the adolescents’ BMI, as well as strong convergent validity with PedsQL. In particular, test-retest reliability was relatively lower in the school behaviour scale, which was similarly observed during validation of the STU in Taiwan. 31 A possible factor for the relatively lower reliability of the school behaviour scale in our study could be because the test-retest intervals crossed into the school examination and holiday period for some respondents, which could have affected parental perceptions of school participation. Further qualitative studies will be required to explain the relatively lower test-retest reliability and guide interpretations of the school behaviour scale. All in all, our findings suggest that STU is a valid and reliable parent-proxy HRQoL tool which can potentially be applied in Singapore to quantify parents’ impression of the psychosocial complications of obesity in their child.
The importance of parental involvement in interventions addressing paediatrics obesity has been recognised globally, with family-based obesity treatment demonstrated to be more effective at promoting and maintaining weight loss in children with obesity. 42 Similarly, a family-based weight management programme for adolescents in Singapore has shown significant improvement in the adolescents’ anthropometric outcomes. 44 Having the STU validated locally can further promote its use clinically to facilitate parental involvement in the management of the psychosocial complications of paediatric obesity. This is in line with the recently launched 5-years Child and Maternal Health and Well-being Strategy in 2021 by our Ministry of Health, which aims to promote greater family-centric management of each child’s health. 45 As the STU contextualises the adolescents’ HRQoL against their weight, and also includes the positive attributes scale, it can facilitate discussions between clinicians, parents and adolescents through highlighting their strengths and more targeted areas that adolescents struggle with due to obesity.
Variables associated with STU
Race, parental education level, and parental marital status were found to be significantly associated with STU scores in our study, independent of other socioeconomic factors such as household income and gender. Our findings support past international studies in demonstrating racial differences in parents’ reporting of their child’s HRQoL.30,46 However, unlike our findings of differences in scores between Indian and Chinese parents, a past local study showed that parents of Malay adolescents with obesity in the community scored their child more poorly on the PedsQL than their Chinese counterparts independent of BMI. 6 Nonetheless, racial differences in HRQoL reporting are not unique to children with obesity, and have been highlighted in studies involving the general adolescent population 24 and adults. 47 These findings could be attributed to ethnic-specific health beliefs as well as expectations. 24 Future large-scale qualitative studies involving participants beyond our clinical population of treatment-seeking adolescents with obesity will be useful, so as to ascertain the factors underlying the ethnic differences in parental assessment of their child’s HRQoL and how they can affect adolescents’ response to weight management therapy. It is also worth noting that the racial breakdown of participants in our study (62% Chinese, 23% Malays, 10% Indians and 5% of other races) differs from the ethnic composition of our population (74% Chinese, 13.5% Malays, 9% Indians and 3.4% of other races) 48 which will require further studies to rationalise and determine if significant.
This is the first study to show an association between parental education level or marital status and parent-reported, obesity-specific HRQoL using the STU. While further research will be necessary to determine the mediators between these parental factors and their reporting of the adolescents’ HRQoL, parenting stress may potentially play a role. Parenting stress in caregivers of adolescents undergoing obesity therapy has been found to predict poorer parent-proxy HRQoL scores on the STU and IWQOL, 49 and parenting stress is likely higher amongst single parents. In addition, parents with lower education level were found to be less involved in their child’s schoolwork 50 and may have lower expectations for their child’s academic achievements, which could have in turn resulted in poorer school performance by the adolescents. 51 These findings further reinforce the importance of engaging parents as stakeholders in adolescent weight management programmes, with parental factors impacting various aspects of adolescents’ HRQoL.
Strengths and limitations of study
Our study is the first to administer STU to Singaporean adolescents with obesity. Validation of the questionnaire amongst adolescents seeking obesity treatment can facilitate its clinical use in the future, thereby providing clinicians with a more comprehensive assessment of the impact of obesity on a child’s HRQoL. Having locally validated HRQoL tools can enable clinicians and researchers to go beyond tracking weight and metabolic parameters to include the adolescents’ HRQoL as important health outcomes. In addition, understanding the factors associated with poor STU scores can help clinicians to risk-stratify parent-child dyads who may require more support in managing the psychosocial complications from obesity.
However, our study has its limitations as a cross-sectional study. Future administration of the STU at different timepoints in the adolescents’ weight management therapy will be needed to determine the sensitivity of the STU to changes in the adolescents’ weight and to track adolescents’ HRQoL progress with weight management interventions. Furthermore, parents who could not complete the STU in English were excluded from our study. This could have resulted in response bias. Future efforts to translate the STU into the official languages of Singapore will be useful to measure the quality of life amongst the different races. Further validation of the STU amongst adolescents in the community and with a larger sample size will also improve the generalisability of the results, given that our study was conducted in a single centre and has a smaller sample size compared to overseas validation studies. In addition, it will be useful to compare the STU scores to self-reported HRQoL by adolescents with obesity using Sizing Me Up, which was omitted from our study as it was targeted at younger children aged 5 to 13 years old. Lastly, research on the usability and acceptability of the STU measure in the clinical settings will be needed to inform and facilitate its adoption by clinicians.
Conclusion
STU has demonstrated good internal consistency, test-retest reliability, construct validity and convergent validity among adolescents undergoing weight management treatment in Singapore. Race, parental education level, and parental marital status were also significantly associated with STU scores. STU is a reliable, valid parent-proxy measure of obesity-specific HRQoL that may be used clinically and in research to assess parents’ perceptions of the impact of obesity on their child’s HRQoL.
Footnotes
Acknowledgements
We wish to thank the families and Weight Management Team in KK Women’s and Children’s Hospital for their participation in the study. In addition, we would like to thank Cincinnati Children’s Hospital Medical Center for allowing us to use Sizing Them Up in our research.
Author contributions
N.W.C.E. and C.C.S.E. were involved in the design of the study, data collection and analysis, as well as article writing. K.B.K. was involved in the design of the study, data collection as well as article writing. F.Q. was involved in the design of the statistical methodology, data analysis and article writing. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by the AM-ETHOS Duke-NUS Medical Student Fellowship Award Award number: (AM-ETHOS01/FY2022/05-A05).
Ethical statement
Data Availability Statement
The datasets used and analysed in the current study are available from the corresponding author on reasonable request.