Abstract
Introduction:
The prevalence of tuberculosis (TB) is rising in Singapore. The affected patients are provided with free directly observed therapy (DOT) at local polyclinics. The impact of DOT on their daily living activities (DLA) and quality of life (QOL) may affect their treatment adherence. The study aimed to evaluate the effect of DOT on the DLA and QOL of patients with TB and to quantify their socioeconomic burden.
Material and methods:
This questionnaire survey recruited adult multi-ethnic Asian patients with TB who were on DOT at nine local polyclinics. The questionnaire collected data on their demographic characteristics and DLA, anti-TB medications, the validated WHOQOL-BREF instrument, and socioeconomic costs. The associations between DOT and independent variables were tested using Student’s t-test and ANOVA.
Results:
The 356 patients recruited comprised 63% males with mean age of 43 years; 73% of them were employed, 73% reported increased travel time (mean 41 minutes/DOT visit) and DOT-related cost (mean S$260–S$389 for 6–9 months’ treatment); 47% indicated reduced participation in social functions and 45% felt that DOT had caused disruptions to their work, especially among younger patients. The WHOQOL-BREF scores were 13.3/20 “Physical Health”, 12.6/20 “Psychological”, 13.4/20 “Social Relationships” and 12.3/20 “Environment” domains, respectively. Some 52% of them rated their QOL as “good” or “very good”, 47% reported satisfaction with their health but 74% experienced negative feelings such as despair, anxiety and depression.
Conclusion:
The DOT affected patients’ DLA, QOL and increased their socioeconomic burden, which should be addressed by appropriate mitigating measures in the community.
Introduction
Tuberculosis (TB) is a communicable disease and remains a major global health problem. According to the World Health Organization (WHO), it is estimated that 9 million people were infected with TB in 2013, resulting in 1.5 million TB-related deaths. 1 In Singapore, TB is endemic and is a significant public health threat, given the highly urbanized community with dense housing estates that increase the risk of diseases spreading.
Many countries have introduced national programs to curb the spread and eliminate TB but success rates vary due to implementation issues. 2 The main strategy adopted by the Singapore Tuberculosis Elimination Program is to ensure that free directly observed therapy (DOT) is provided to the affected patients at public primary healthcare clinics (polyclinics), which are located in close proximity to patients’ homes. 3 The Ministry of Health has enacted the Infectious Disease Act, which mandates that all patients infected with TB complete the 6–9 months of DOT. Patients are often diagnosed and commence their prescribed anti-TB medication by physicians at the Tuberculosis Control Unit (TBCU). Once they are stabilized, they will be followed up in primary care under a shared care program between TBCU and polyclinics. Approximately 60% of them are referred to the polyclinics for continuity of DOT.
During DOT at the polyclinics, primary healthcare providers (predominantly nurses) supervise and observe the patients’ consumption of their anti-TB medications, according to the regimen (daily, twice daily or thrice per week) prescribed by TBCU. Patients with resistant strains receive additional parenteral administration of streptomycin. The overall objective of DOT is to ensure patients’ full adherence and completion of the entire multi-antibiotic therapeutic regime, but patients may default such treatment by failing to turn up at treatment sites. While a recall system is in place as a remedial measure to ensure continuity of treatment, patients who default DOT are at risk of spreading the disease and developing multi-drug-resistant TB (MDR-TB).
In recent years, local health authorities have reported a 22% rise in the incidence of TB from 1256 cases in 2007 to 1533 cases in 2011. The incidence rate had increased from 39.2 cases per 100,000 population in 2010 to 40.5 cases per 100,000 in 2011. 4 In addition, the emergence of MDR-TB poses an even more serious public health threat. Singapore had six new cases of MDR-TB in 2011 compared with three cases in 2010. MDR-TB often results from poor adherence to the anti-TB therapy and hence failure to achieve “microbiological cure”.
The development of MDR-TB requires even longer courses of DOT, which can potentially result in prolonged social isolation, loss of employment, and adverse long-term socioeconomic and psychological effects. 5
These negative effects will inevitably interfere with patients’ daily living activities (DLA; an individual’s daily routine activities at home, work, and recreation) and compromise their DOT adherence. 6 An earlier pilot survey by the authors had revealed that DOT affected the DLA of 60% of patients, which prompted the initiation of this study. Moreover, the rising incidences of TB and MDR-TB necessitate an urgent review of DOT and its impact on patients’ socioeconomic burden.
Tuberculosis infection itself is known to adversely impact on the quality of life (QOL; a person’s perception of his or her physical and mental health, covering broad domains including physical, psychological, economic, spiritual, and social well-being 7 ) of the affected patients.8,9 Moreover, the multiple anti-TB drug regimens in DOT, often with side-effects, may considerably affect patients’ QOL.
Aim of the study
The primary aim of this study was to determine the DLA and QOL of patients receiving DOT. The secondary aims were to identify and quantify the socioeconomic burden faced by these patients.
Methods
Design and setting
This cross-sectional questionnaire study was carried out at nine polyclinics located in the eastern and southern regions of the island: Bedok, Bukit Merah, Geylang, Marine Parade, Outram, Pasir Ris, Queenstown, Sengkang and Tampines.
Sample
The target subjects were adult multi-ethnic Asian patients aged 21 years and older, who were diagnosed with TB based on positive smear and culture at TBCU. They were recruited whilst receiving DOT, regardless of the period of treatment or drug regime, at the nine polyclinics. Patients who were cognitively impaired or refused consent were excluded.
Sample size calculation
A small pilot study was carried out at three of the polyclinics (Bedok, Bukit Merah and Outram). Based on our pilot data, we made a conservative hypothesis that 60% of the participants will encounter socioeconomic burden due to DOT. In order to prove this proportion with a 5% margin of error, we targeted to recruit 360 participants.
Recruitment
The investigators trained a team of nurse-collaborators at each study site, as well as trainee nurses from a local nursing school. The latter served as research assistants (RAs) to administer the questionnaire. The RAs screened the potential subjects for eligibility, explained the study’s intent and content using the approved participant information leaflets, and clarified their queries before obtaining their written informed consent. Each RA-administered questionnaire was completed within 15–20 minutes.
Instrument/questionnaire
The investigators tested the draft questionnaire on their nursing peers to determine their understanding of the World Health Organization Quality of Life instrument (WHOQOL-BREF) and other questions pertaining to the impact of DOT on DLA. Next, the draft questionnaires were administered on five patients at three pilot study sites to estimate the magnitude of the impact of DOT on DLA. The questionnaire was then finalized before submitting to the ethics board for approval.
The questionnaire comprised three segments, namely: (A) socio-demographic profile (21 items), (B) variables relating to DOT (24 items) and (C) the WHOQOL-BREF. WHOQOL-BREF has been developed and used for QOL assessment in different countries across the world, ranging from India, China to Europe. The WHOQOL-BREF is an internationally validated, 26-item instrument constructed from four domains: “Physical health” (seven items); “Psychological” (six items); “Social relations” (three items) and “Environment” (eight items). Each item is rated on a five-point response scale. Each domain enquires about the related facets which are listed in Table 5. Data within domains were computed to produce a domain score according to the WHO BREF guideline and then transformed to range between 4 and 20. Domain scores are scaled in a positive direction (i.e. higher scores denote higher QOL). Thus, aside from socioeconomic issues, the instrument is advantageous to determine the multi-dimensional assessment of the QOL of the patients.
Data analysis
The dimensions of the QOL tool were tested and the scores of BREF were derived following the official guidelines. 10 Descriptive statistics were computed for continuous variable such as age, education level, costs, travel times and reported with means and standard deviations. Categorical variables such as gender, ethnicity, education, household income and employment status were analyzed with ANOVA. Kruskal–Wallis equality-of-populations rank test was used for length of treatment and impact of DOT on DLA, psychosocial and economic variables. The associations of the effect of DOT on concerns, social and economic impact variables were tested using Student’s t-tests. The effects of DOT on their DLA and age were compared using correlation coefficients. The statistical level of significance was set at 0.05. The data were analyzed using STATA (StataCorp. 2011. Stata Statistical Software: Release 12. College Station, TX: StataCorp LP).
Ethics approval
The study was approved by the SingHealth Institutional Review Board (Reference: 2012/882/A).
Results
In total, 356 patients were recruited from the nine polyclinics from May 2013 to April 2014. Their demographic characteristics are presented in Table 1. They comprised 48% Chinese, 22% Malay, 7% Indians and 23% other ethnic groups (Eurasians and other foreigners). About 35% of the patients were migrant workers from the region, who were holders of employment-pass and work permits. An average household income of ⩽ $1500 was reported by 42% of the patients and 9% of the patients were receiving social welfare. About 70% of patients were on daily regimen for TB treatment and 30% on a thrice-weekly regimen.
Demographic and socio-economical characteristics of the patients.
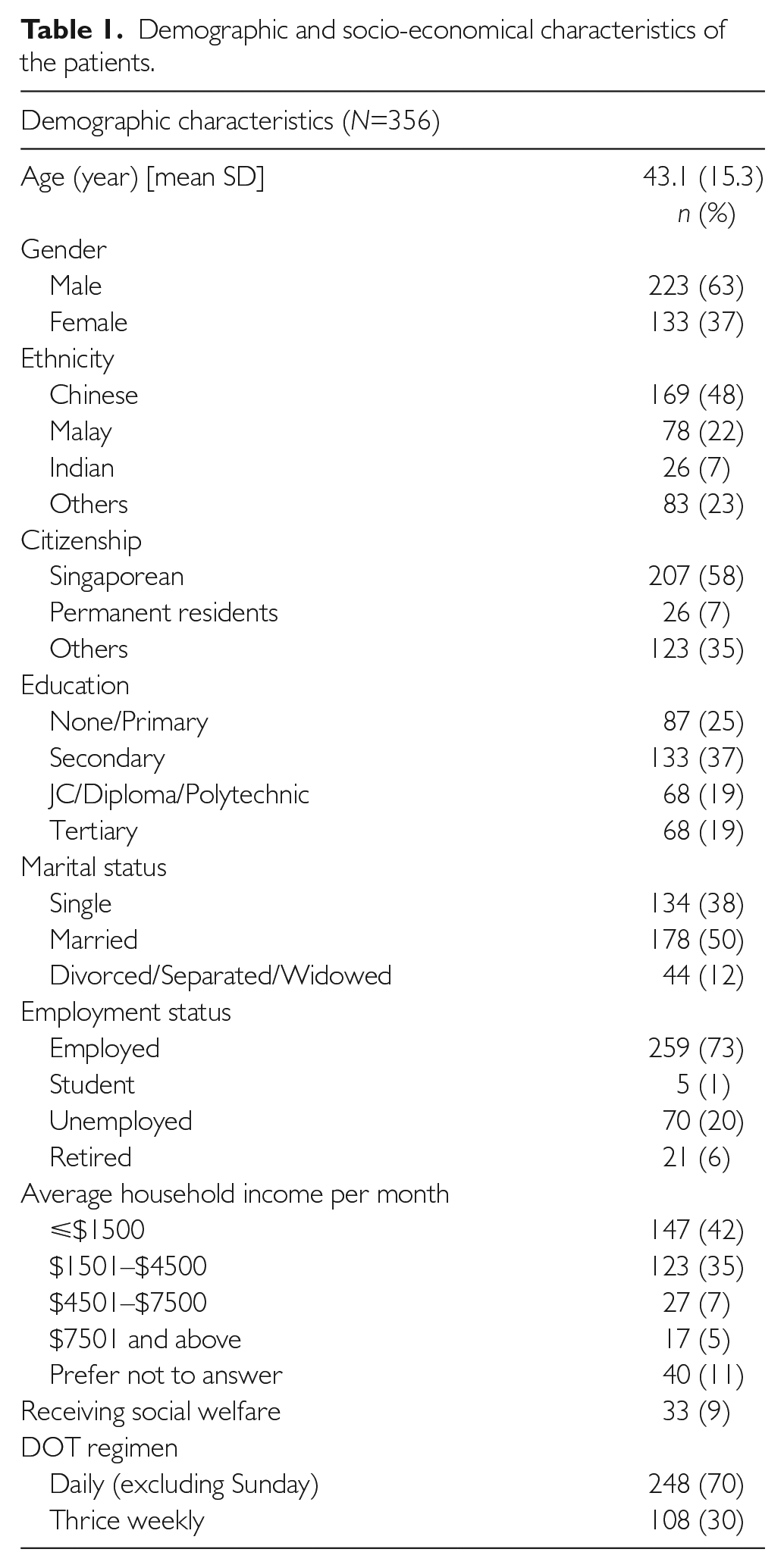
The patients in this study population had variable duration of DOT at the point of study enrolment. At recruitment to the study, half of the patients were on DOT for 36 days, with the overall mean duration of 74.1 days (SD 93.6).
Effect of DOT on DLA and employment
Directly observed therapy treatment was perceived by 45% of the patients to disrupt work, school and social activities (Table 2). Almost half of the patients (47%) revealed reduced social functions while 22% felt isolated during social functions (Table 3). Our survey showed 14% of them to perceive an adverse effect on sexual relationships with partner after the diagnosis of TB (Table 3).
Daily living activities.

For these questions, the total did not add up to 100% as they might not be applicable to patients.
Concerns, social and economic impact of patients on DOT.

Score of 1 indicates no impact and score of 10 indicates high impact.
Student’s t-tests
One in five (21%) of the patients felt that employers were disgruntled because DOT disrupted their work schedules and duties (Table 2). Nonetheless, most of the respondents (77%) denied that DOT had negatively affected their career opportunities and prospect for promotion.
Socioeconomic impact of DOT
Table 4 describes the social impact of DOT on the study population. About 63% of patients felt that DOT treatment had affected their daily life. The question on DOT affecting daily life is a 10-point Likert scale with response of 1 as “strongly disagree” and 10 as “strongly agree”. Younger patients reported higher negative effect of DOT on their daily life (correlation coefficient = −0.13, p = 0.015) and considered DOT to be highly disruptive (p = 0.002), as shown in Figure 1.The majority of the patients (93%) would reveal their DOT to other persons. Few reported being avoided by their family (2%), employers (5%), colleagues (5%) or friends (6%). About 12% claimed that they discontinued their job whilst on DOT. About one in six of the patients were embarrassed to take the medication at polyclinic (16%); one in 10 felt uncomfortable being observed by nurses during DOT (10%) and perceived additional burden to their accompanying relatives (9%); one in three were afraid to let others know of their treatment (34%). About one in five patients (19%) were concerned of the effectiveness of DOT (Table 3).
Social relationships.


Association between the effect of DOT on daily life and the age of the patients.
Most patients (72%) reported acceptance of the DOT regime for TB treatment in polyclinics, including the extra time incurred (73%). We analyzed the association of all the items in Table 3 against the effect of DOT on daily life and found statistically significant results in some items. Some 286 (81%) patients disagree that the DOT treatment may not be effective and was statistically not significant (p = 0.11) in terms of the effect of DOT on daily life. There was some association between acceptance of DOT regime and the effects on daily life (p = <0.01).
The duration of treatment was not significantly associated with poorer QOL, disruption of daily activities, and the acceptance of the treatment schedule. However, a trend is noted to indicate that the longer the patient was on DOT, the higher was the level of acceptance of treatment.
Increased financial burden and economic costs incurred by DOT were identified among patients (Table 3). About 27% of them disagreed to the extra travel time needed for DOT (p = <0.01) and 53% (p = 0.01) self-reported that they incurred more expenditure during DOT. Estimated mean cost on transport per visit for DOT was S$1.80. The mean cost of transport for 6 months was about S$260 and S$389 for 9 months if a patient traveled to the polyclinic 6 days per week.
The mean total traveling time from residence to polyclinic for DOT and treatment time was 41 minutes. On average, patients spent approximately 99 hours of travel time for 6 months of DOT treatment, which increased to 148 hours if treatment regime was extended to 9 months.
Quality of life (WHOQOL-BREF scores in four domains)
Overall, about half of the patients (52%) rated their QOL as “good” or “very good” and were satisfied with their health (47%) during DOT treatment (Table 5). The scores for the “Psychological” and “Environment” domains were lower than the “Physical Health’ and “Social relationships” domains (Table 5). A minority of them were not satisfied with their capacity for work (14%), energy for everyday life (15%), support from their friends (10%) or their access to health services (3%). However, 74% of patients reported to experience negative feelings such as despair, anxiety and depression.
WHO Quality of Life-BREF (WHOQOL-BREF) and scores.

Discussion
Directly observed therapy is now the standard of care for affected patients with TB in Singapore. The local focus of TB treatment has evolved from the reduction of mortality to the alleviation of morbidity in recent years in order to meet the rising expectation of the healthcare services from its population. Its impact on QOL, DLA and socioeconomic burden becomes more relevant to local patients.
Inevitably, DOT has been viewed by some patients as inconvenient and interfering with their life and work. 11 The daily life of 63% of respondents were affected by the 6–9 months’ duration of DOT (which is significantly longer to the 1–2 weeks of pharmacotherapy for most other acute infections). Nevertheless, most of them (73%) eventually accepted DOT, a number which increased the longer they were on the treatment. The healthcare setting can be modified to provide patients with a more favorable environment to continue their treatment. Administrative measures have been introduced in a group of local polyclinics to reduce patients’ wait time for the DOT, such as the abolition of front-end registration for their daily visit. On arrival at these polyclinics, patients can proceed to the treatment room, where nurses can attend to them promptly, so that they complete the treatment quickly and leave for their work place.
During the period of DOT treatment, traveling between residence or workplace and the polyclinics incurs additional costs to the patients. A study 12 also showed that DOT increased cost during treatment phase, which this study also alluded to in terms of travel expenditure. A small number of patients in this study had to discontinue their job due to DOT, which aggravated their finances. A local scheme to assist needy patients on DOT was launched in 2013 by offering them incentives such as supermarket shopping vouchers for completing their course of treatment. 13 Such a community-centric program is a welcome measure to support local patients. Whether it is effective in reducing their socioeconomic burden requires further evaluation. The data in this study will serve as baseline parameters to determine the effectiveness of such interventions.
Quality of life matters to patients, regardless of their localities. The use of WHOQOL-BREF in this study allows the comparison of the QOL of local patients on DOT with similarly affected patients in other communities. Compared with Dhuria et al., 14 the scores in this study were higher for the “Physical Health” (9.3 vs. 13.3/20); “Psychological” (9.8 vs. 12.6/20) and “Environment” (11.4 vs. 12.3/20) domains, but lower in the “Social Relationship” domain (14.4 vs. 13.4/20). The lower score could be attributed to a more ethnically and culturally diverse group of patients in Singapore, compared with a more homogeneous population in the Indian study. Almost a quarter of the patients in this study were foreigners, who may not have fit socially into the local population.
Overall, the study serves as a timely reminder to frontline healthcare workers to assist and support patients on DOT beyond the supervision of treatment. They can leverage on their almost daily interaction with their patients (especially those who are younger) to assess their socioeconomic burden, coping strategies and to identify resources and measures to overcome their barriers. They can also link those affected patients with the polyclinic medical social workers to render additional assistance during the treatment period.
However, the current patient education practices provided by the nurses are limited in scope, confined to clinical aspects of TB and its treatment. Liberalized immigration and rapid economic growth after 2005 have substantially altered the characteristics of patients with TB receiving DOT at the polyclinics. 15 Nurses face challenges in managing multi-ethnic patients with cultural diversity, in which almost a quarter of them are overseas workers. The training program of these nurses can be expanded to equip them to be culturally sensitive, and impart relevant counseling skills to help patients cope with their DOT. The curriculum should cover approaches to rectify patients’ misperceptions of the disease and to reduce their perceived or actual stigma arising from the treatment. 16
Strengths and limitation of the study
The questionnaire survey was carried out in all polyclinics within the institution to minimize selection bias of the subjects. All consecutive and eligible patients were invited to participate in this study to reduce bias.
Data such as travel time and cost related to DOT were self-reported by patients. The study did not carry out exact measurements of such variables in real time, which potentially constitute a study limitation.
Implications for future research, policy and practice
In this study, a proportion of the patients faced problems such as loss or discontinuation of job and disgruntled employers. Public health campaigns organized by the health and labor authorities, such as those held in conjunction with World TB Day, should focus in elevating the awareness of employers on TB epidemiology, DOT and its implications in workplace safety. 17
Incentive schemes can be considered to engage the employers to support their workers to regain their health during DOT, as TB is curable upon successful completion of treatment. This will not only improve patients’ welfare, it also increases the productivity of their workforce, as illustrated by the successful public health programs of American Thoracic Society/Centers for Disease Control and Prevention/Infectious Disease Society. 18
This study allows polyclinic healthcare professionals to gain insight on the psychosocial and financial issues faced by patients on DOT. It prompted an interest to explore new ideas to mitigate the various adverse effects of DOT, including the use of remote monitoring of DOT. The advent of new telecommunication technology provides opportunities to test out innovative interventions and incentives to enhance the management of TB, which will benefit both patients and healthcare providers. This requires further research to evaluate its safety and cost-effectiveness, and results from this study will be invaluable to the design of new modality of care delivery.
Conclusion
This study revealed that DOT resulted in variable adverse impact on patients’ career, traveling expenses, DLA and QOL. The primary healthcare providers, including the nurses, should proactively address the economic and psychosocial concerns of patient and to support them during the DOT therapy, especially during its early treatment phase. The findings of the study may also catalyze the development of new model of care for patients with TB in the community.
Footnotes
Acknowledgements
The authors are grateful to World Health Organization for granting the permission to use the WHOQOL-BREF questionnaire as well as the administrative support rendered by Ms Sibel Volkan. The authors also acknowledge the field work performed by the nursing students and their tutors from Ngee Ann Polytechnic and the tremendous effort by the staff nurses to recruit patients at the study sites.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This project was supported by SHP Research Support Programme - Seed Funding.
