Abstract
Objectives:
We wanted to determine: (1) whether ADHD symptoms were more common in mothers of children with ADHD; (2) whether mothers of children with ADHD differed in their parenting strategies; and (3) whether there was a difference in care-giving arrangements for children with ADHD and without ADHD. This was done by comparing mothers of children with ADHD with mothers of children without ADHD in Singapore.
Methods:
Mothers of children with ADHD (
Results:
Mothers of children with ADHD did not report higher levels of current ADHD symptoms compared with the control group. However, they did use less adaptive parenting strategies. There were also no differences in the reported behaviours of children cared for by a paid worker and those cared for by mothers.
Conclusions:
Data support the Singapore Clinical Guidelines recommendations for the promotion of parenting skills, and referral to parenting programmes for parents of children with ADHD. The promotion of parenting skills and referral to parenting programmes for mothers of children with ADHD might include the option of electronic forms of programme delivery. The model of using paid help in the home, which is commonplace in Singapore, does not seem to disadvantage children with ADHD.
Introduction
Attention-Deficit/Hyperactivity Disorder (ADHD) is a developmental disorder with core underlying deficits in sustained attention, hyperactivity and impulse control. It is one of the most common mental health disorders of childhood, affecting approximately 2% to 10% of school-aged children. 1 A significant proportion of children with ADHD will experience school failure, and go on to develop delinquent activities and antisocial personalities which may persist into adulthood. The core ADHD deficits of inattention, hyperactivity and impulsivity mean that managing a child with ADHD is a challenging prospect for many parents.
Children with ADHD have varying degrees of impairment in the areas of school performance and socialisation, 2 including few close friendships and greater peer rejection. 3 ADHD symptoms tend to surface early in childhood, usually between three and seven years of age. 4 Rimestad et al. noted that while the diagnostic criteria for ADHD were originally developed with a primary focus on school-age children, they have also been used to diagnose ADHD in pre-school children. It is estimated that 2% to 6% of pre-schoolers meet the criteria. 5
A worldwide review found an ADHD prevalence rate of 5.29% with a range from about 1.5% to 10%, with the variability attributed partly to differences in the two main internationally recognised guidelines for diagnosis – the International Classification of Diseases and the Diagnostic and Statistical Manual of Mental Disorders. 1 Gender differences have been found, with the ratio of males to females ranging from 2:1 to 10:1. 6 The higher rate of males in clinical samples is sometimes thought to be due to referral bias, in that males are more likely than females to be aggressive, and aggressive behaviour is more likely to lead to referral. 7
Symptoms persist into adulthood for 30% to 80% of children diagnosed with ADHD.8–10 A systematic review found the prevalence of adult ADHD to be 2.5%. 11 Biederman et al. found a relatively high incidence of comorbid lifetime diagnoses of anxiety disorders (43% to 52%), major depressive disorder (31%), oppositional defiant disorder (29%), conduct disorder (20%), antisocial personality disorder (12%), alcohol (27%) and drug dependencies (18%) in their sample of clinic-referred adults with ADHD. 12 It is also likely that adults with ADHD may experience difficulty with parenting.7,13
The precise aetiology of ADHD is unknown. However, there is increasing evidence of neurobiological genetic influences, factors related to biological adversity and psychosocial factors.14,15 Additional factors that have been implicated are poor mother–child relationships and maternal psychopathology. 7 Evidence of a strong genetic basis for ADHD is demonstrated by twin studies, and family and adoption studies. Family studies have identified a two- to eightfold increase in the risk of ADHD in parents and siblings of children with ADHD. 16 It is estimated that 12–20% of mothers and 9–54% of fathers of children with ADHD may also have ADHD themselves. 7 This is an important consideration for the current study as parents who have ADHD themselves may have particular difficulty managing their children with ADHD.
Many mothers of children with ADHD report a diminished sense of parenting satisfaction; reduced confidence in their success in parenting; low levels of family support; and high levels of child demands.17,18 Hoza et al. found that treatment outcomes for children with ADHD were negatively affected by mothers’ low self-esteem and poor understanding of discipline and problem solving. 19 Mothers of children with ADHD also often engage in less effective parenting and experience heightened levels of stress in their parenting role.20–23
Ooi et al. examined the impact of parent–child attachment on aggression, social stress and self-esteem in a sample of clinically disordered boys with conditions such as ADHD within a child psychiatric clinic in Singapore. 24 They found that boys with a higher quality of parent–child attachment were less aggressive, had lower social stress and higher self-esteem.
Gomez and Vance examined ADHD symptoms across Malay and Chinese children in Malaysia, and found support for cross-cultural invariance for ADHD symptoms. 25 In Hong Kong ADHD subtype differences also supported the cross-cultural equivalence of the nosological distinctions in ADHD subtypes. 26
Methylphenidate has been found to be an effective strategy to manage ADHD symptoms in Asia. In Taiwan, 68–78% of children with ADHD who received methylphenidate showed improvements in their behaviour in the classroom and at home. Approximately 61–66% of children had improvements in academic learning. 27 Huang et al. examined the effectiveness of a behavioural parent training programme for Taiwanese parents of children with ADHD. Their study showed that ADHD symptoms and home behaviours of the children improved significantly after parent training. 28 So et al. found that a combination of behavioural treatment and low-dose methylphenidate was significantly more effective than a medication-only strategy in reducing symptoms of ADHD in Hong Kong. 29 This is consistent with the conclusion that the most effective way to address ADHD is by combining multiple treatments, in particular stimulant medication therapy with parent training.7,30
The ‘Parenting Project’ undertaken by the Singapore Children’s Society 31 examined child rearing in Singaporean families. Mothers were found to be the main care givers for most children, but a substantial proportion of children (approximately 20%) were cared for by paid workers. The data collected in a large-scale survey conducted by the National University of Singapore also found that about 21.9% of households employed at least one foreign domestic worker. In 52.9% of these households, the primary responsibility of the domestic worker was childcare. 32
The effect of having domestic foreign workers as care-givers in the Singaporean home is not entirely clear. It has been suggested there may be negative long-term effects on the values and work ethics of children brought up by foreign maids. They may become used to indulgences such as others picking up after them, and come to expect it. 33 Conversely, Cheo and Quah argued that having a foreign domestic worker as care-giver could have positive effects on the children. As the maid takes care of the household chores, the mother may theoretically have more contact time with her child after work hours. This may increase the chances of the development of positive mother–child attachment and interaction. 34
The general aim and purpose of the present study was to better understand parenting of children with ADHD in Singapore and provide recommendations for interventions. The key research questions were as follows. (1) Are ADHD symptoms more common in mothers of children with ADHD than in mothers of children without ADHD? (2) Do mothers of children with ADHD differ in their parenting strategies from mothers of children without ADHD? (3) Is there a difference in care-giving arrangements for children with ADHD and without ADHD?
Method
Participants
All the participants were Singaporeans, either holding Singapore citizenship or permanent residency. Two groups were recruited: (1) a control non-clinical community sample of mothers (
Apparatus
Mothers in the two groups completed questionnaires which asked about their personal characteristics, parenting behaviours, care arrangements for their child and their child’s characteristics and behaviours. The questionnaire included the CPRS-R:S; 35 the Conners’ Adult ADHD Rating Scale-Self Report (Short Version) (CAARS-S:S); 36 and the Alabama Parenting Scale (APS). 18
Severity of child behaviour
The CPRS-R:S 35 was used to measure the severity of the child’s behaviours. It assesses problem behaviours, ADHD and comorbid disorders in children and adolescents (aged 3–17 years) and contains 27 items. It provides scores for the following subscales: Oppositional (tendency to break rules, have difficulty with authority and become easily annoyed or angered); Cognitive Problems/Inattention (difficulties related to inattention, disorganisation, poor task completion and academic struggles); Hyperactivity (restlessness and impulsivity) and ADHD Index (used to identify children and adolescents who are at risk for a diagnosis of ADHD). Subscale scores are converted to T-scores with scores of 65 and above considered clinically significant. The psychometric properties of the scale include good internal reliability, high test–retest reliability and effective discriminatory power.35,37
Parenting practices
Parenting practices amongst Singaporean mothers were assessed using the Alabama Parenting Questionnaire (APQ). 18 The APQ uses 42, five-point Likert-type rating scales designed to assess parenting practices. It consists of five main parenting constructs: (1) Parent Involvement, (2) Positive Parenting, (3) Poor Monitoring/Supervision, (4) Inconsistent Discipline and (5) Corporal Punishment. Wells et al. assessed the APQ factor structures and found that the factors labelled Positive Involvement, Negative/Ineffective Discipline and Deficient Monitoring demonstrated good internal consistency. 38 The APQ was chosen because of its simplicity in administration and because it has been used in several studies as a self-reporting measure examining the relationship between parenting and problems in conduct.39,40
Maternal ADHD symptoms
CAARS-S:S was used to determine the incidence of ADHD symptoms in mothers. 36 It is a short self-report form containing 26 items. Subscale scores for the following areas can be determined: Inattention/Memory Problems, Hyperactivity/Restlessness, Impulsivity/Emotional Liability, Problems with Self-Concept, and ADHD Index. The answers are scored on a five-point scale and converted to T-scores, with scores of 65 and above considered clinically significant. This scale has been found to be a reliable and valid measure of ADHD symptoms for use with adults and has demonstrated good internal consistency and inter-rater reliability, as well as sensitivity to treatment outcome. 41
Child academic performance
Child academic performance was based on mothers’ reports of the child’s grades in school. The four bands used in the local school system in Singapore were subsumed into ‘Satisfactory’ and ‘Unsatisfactory’ categories. Academic performance in the two main subjects of English language and mathematics was examined. Since children with special needs had access to special accommodation in the classroom in Singapore, receipt of special accommodation (as reported by parents) was used as an indicator of the severity of a child’s problems with academic performance.
Care-giving arrangements
Care-giving arrangements were assessed using the procedure used by Shum-Cheung et al. 31 Mothers rated their satisfaction with the care-giver’s ability to: get the child to complete homework; get the child to complete daily routines such as bathing, eating; manage the child’s behaviours, prepare the child for school the next day; be aware of where the child is; and needs to be able to motivate the child to complete chores and help at home. Mothers rated their satisfaction with the care-giver using a five-point Likert-type scale.
Procedure
Participants were recruited from the following agencies: ADHD support groups, hospitals and private clinics that cater for individuals with ADHD, and also through snowball recruitment. Children were eligible if they were in primary school, with no age specified. The announcements of the study were made during a professional development course on special needs for local school teachers. As an incentive to participate, participants were placed in a draw for a Singapore $100 gift voucher. The clinical sample was given the option to receive feedback about their parenting approaches and how to improve upon them. As an added incentive, complimentary workshops for agencies providing five or more participants were offered. The questionnaires were distributed to participants through postal mail, agencies or via the internet. Ethics approval for this study was obtained from the university ethics committee.
Analyses
Data analysis was undertaken using the Statistical Package for the Social Sciences (SPSS). Power calculations showed that a sample size of 64 was required to detect an effect size of 0.3 with an alpha of .05 and power of 0.80 using
Results
Mother demographic data
Chi-square (χ2 ) and
Demographic data for mothers.

Child demographic data
A greater percentage of patients in the clinical group were boys, who were older (Table 2). They also did significantly less well academically and were more likely to receive special arrangements within the school setting.
Child demographic data.
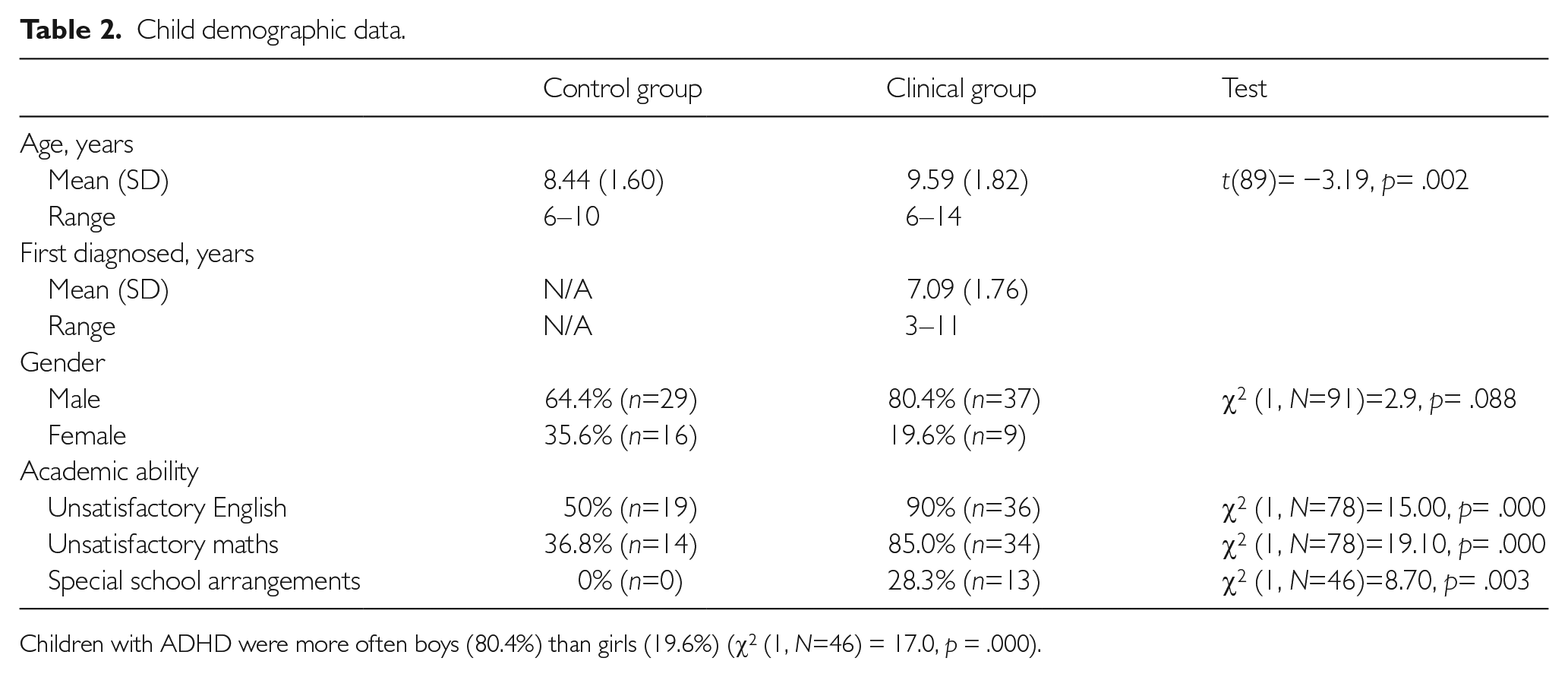
Children with ADHD were more often boys (80.4%) than girls (19.6%) (χ2 (1,
Severity of child behaviours
The clinical group had mean scores in the clinical range (T-scores of 65 or over) for all four indices. None of the mean scores in the control group were in the clinical range. Mean scores were significantly different between groups for all subscales. The ADHD clinical group performed more poorly on all indices as expected (Table 3).
Mean T-scores obtained by the control and clinical groups for specific subscales on the Conners’ Parent Rating Scale-Revised (Short Version).

Maternal ADHD symptoms
The mean maternal CAARS-S:S T-scores for both the control and clinical groups were below 65, indicating a lack of clinical significance for both groups (Table 4).
Mean T-scores obtained by control and clinical group mothers for the Conners’ Adult ADHD Rating Scale-Self Report (Short Version) (CAARS-S:S).

Parenting practices
With reference to the scores obtained on the APQ, the clinical group had significantly lower scores on the overall positive parenting subscale and significantly higher scores on the overall negative parenting subscale (Table 5).
Mean raw scores for parenting measures (subscales) on the Alabama Parenting Questionnaire obtained by the control and clinical groups.

Care-giving arrangements
About 20% of the control and clinical group children were cared for in the home by a paid worker. There were no differences in child behaviours associated with ADHD as measured by the CPRS-R:S in relation to receiving care-giving from mothers versus from persons other than the mother. The control group was significantly more satisfied with the care-giving arrangements (mean 23.24) than mothers of children with ADHD (mean 19.24) (
Percentage (frequency) of responses on specific items on satisfaction (‘very happy’ or ‘happy’) of care-giving across groups.

Discussion
Group comparisons on the CPRS-R:S confirmed that the clinical group scores were in the clinically significant range for all measures and the control group scores were not. The first research question asked whether ADHD symptoms were more common in mothers of children with ADHD than in mothers of children without ADHD. Maternal ADHD symptoms as measured by the CAARS-S:S were not higher in mothers of children with ADHD and scores were below that required for clinical significance in both groups. This finding was unexpected given the genetic nature of the disorder, as reported in the literature, and the reported association between ADHD symptoms in mothers and in children. For example, Middeldorp et al. showed that ‘parents whose children suffer from a variety of psychopathologies have a higher risk of experiencing depressive, avoidant personality, and ADH problems than adults in the general population’. Specifically, ‘maternal ADH was associated with offspring ADH with an effect size of 0.20’. 42 It is possible to postulate that mothers might have outgrown earlier ADHD symptoms.
The second research question asked whether mothers of children with ADHD differed in their parenting strategies from mothers of children without ADHD. There was clear evidence that mothers of children with ADHD engaged in significantly more negative parenting and significantly less positive parenting. This is consistent with Western literature.20,21
The third question asked whether there was a difference in care-giving arrangements for children with ADHD and without ADHD. It is important to note that there were no differences in the behaviours of children cared for by a paid worker and those cared for by a mother. This is interesting in the Singaporean context where the merits and shortcomings of using paid workers in the home are often debated and mothers play a much greater role in parenting than do fathers. 43
By adulthood, hyperactive children have been found to have less education, achieve lower grades, fail more of their courses or fail more to graduate than control groups.9,13 The clinical group children in the present study were also found to have lower academic performance. Pagani et al. showed that academic failure, and in particular grade retention, was associated with a significant loss of motivation to learn in school, reduced academic performance, significant peer relationship problems, and greater persistence and a potential worsening of anxious, inattentive and disruptive behaviours. 44 Such disadvantages, together with the finding that mothers of children with ADHD demonstrated inferior parenting skills, indicate the need for the provision of parenting programmes for this group in particular, although the finding that mothers of these children do not themselves have higher than normal ADHD symptoms means that the focus of parent training need not particularly emphasise self-management of ADHD symptoms.
Pelham and Fabiano reviewed the treatment literature and concluded that positive behavioural parent training was an effective and well-established treatment for children with ADHD. 45 Hence, positive parenting strategies serve as protective factors against child-disruptive behaviours, and negative parenting strategies. 18
Fung et al. described clinical practice guidelines developed by a multidisciplinary group for the treatment of ADHD in Singapore. 46 While these guidelines advise against some forms of psychological and other treatments in isolation (e.g. cognitive-behaviour therapy, social skills training) and provide cautions about some forms of pharmacological treatment, they also note that parent training should be offered for parents of pre-school children with ADHD and that parents should be referred to community-based parent training programmes.
The recommendation that parent training programmes should be promoted is supported by evidence of its efficacy. A meta-analysis of 14 studies with 576 participants demonstrated an overall beneficial effect of positive parenting upon the functional outcomes of young children with developmental disabilities.
47
Across the 14 studies reviewed, the random effects weighted average effect size was
The ‘Incredible Years’ programme and ‘Triple P’ are examples of evidence-based parenting programmes. The Singapore Ministry of Social and Family Development has evaluated ‘Triple P’ and plans to increase the outreach to 175 schools by 2018. Parents who completed the programme reported ‘greater parenting competence, lower parenting stress, improved emotional states and reduced behavioural problems in children’. 49 Both ‘Incredible Years’50–52 and ‘Triple P’53,54 have a strong empirical evidence base.
Taylor et el. evaluated a randomised controlled trial of a parenting intervention for parents of children with high levels of ADHD symptoms in school settings. 55 They found that recruitment to the study was difficult and that reaching the parents with the most need was challenging. Non-attending parents reported various barriers including fear of attending in a group. While there seems to be sufficient evidence to justify the recommendations of referral to parenting programmes, technology may offer an innovative alternative to face-to-face programmes. In a randomised controlled trial, Xie et al. found that parent training through videoconferencing was as effective as face-to-face training at improving parent ratings of ADHD (and other symptoms). 56 The videoconferencing approach was also well accepted by parents. Although geographic remoteness is not a problem for Singaporeans, the country is well served by its technology infrastructure, and the use of videoconference may offer a useful choice for parents.
Limitations
One limitation of this study is the recruitment method, which utilised a lottery incentive and targeted advertising. This may make the study prone to selection bias. The APQ has also not yet been validated with a Singaporean sample. This study relied on parents’ self -reporting and may thus suffer from subjectivity bias. The study was also not able to detect any prior ADHD diagnosis in the parents and ADHD symptoms can improve with age. Another limitation is the over-representation of Chinese mothers in the clinical group; its effect on the results is not known. Furthermore, as the control group relied on parental report regarding the absence of an ADHD diagnosis, it is possible that the group might have included children with undiagnosed ADHD.
Future work might include a norming study of any intended measure not already validated with a Singaporean sample, for example the APQ. The use of objective observational or other objective data to supplement parental report would also be worthwhile. Given our results on the effect of paid help, future research might also include an evaluation of offering empirically-supported parenting training to these paid helpers as well as to the parents themselves.
Conclusion
This study is novel as it includes the common local use of paid care-giving assistance in the home for children, while also examining mothers’ parenting practices and the possibility that mothers of children with ADHD might have significant levels of ADHD symptoms themselves.
The study found no evidence of higher maternal ADHD symptoms in mothers of children with ADHD as compared with mothers of children without ADHD. We also found that mothers of children with ADHD engaged in less adaptive parenting skills than mothers in the control group; and that there were no differences in the behaviours of children cared for by a paid worker compared with those cared for by a mother. Singapore clinical guidelines have recommended the promotion of parenting skills, and referral of parenting programmes for mothers of children with ADHD. These parenting programmes might sensibly include the option of electronic forms of programme delivery.
Footnotes
Acknowledgements
The first author collected the data and conducted the analyses. The second author supervised the research, and both authors contributed to writing the manuscript. Ethical approval: ethics approval was received from the university ethics committee. Participants signed an informed consent form.
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not for profit sectors.
