Abstract
Traumatic facial nerve paresis is an undesired sequel following temporal bone fractures. The choice of surgical approach for this condition is largely dependent on the site of the lesion. A 33-year-old woman presented with delayed facial nerve paresis following a motor vehicle accident, which did not show any improvement with conservative treatment for 3 months. Preoperatively, she had facial nerve paresis House–Brackmann grade V. She underwent endoscope-assisted facial nerve decompression involving the tympanic segment of the facial nerve. A standard postauricular mastoidectomy was performed. The mastoid segment of the facial nerve was identified but there was no obvious fracture or bony spicule seen. An extended posterior tympanotomy was done and endoscope was used by way of this corridor to examine the tympanic segment of the facial nerve until the second genu which appeared to be emaciated with lack of lustre. Finally, neurolysis was done under endoscopic guidance. She regained significant improvement in her facial nerve function 8 months postoperatively to House–Brackmann grade II.
Introduction
Temporal bone fracture can be classified into three categories: longitudinal, transverse or mixed types based on its relation to the long axis of the petrous bone. 1 The decision on either to treat conservatively or for surgical intervention is mainly based on clinical progression, deterioration of electrophysiological tests and supporting imaging findings. To date, there is no definite consensus on the timing of the surgical intervention. Surgical intervention is warranted in a scenario in which the patient develops an immediate and complete facial nerve paralysis with evidence of electroneurography (EnoG) test showing neural degeneration greater than 90%. 2 High resolution computed tomography (HRCT) of the temporal bone may serve to provide additional information by delineating the fracture line and its extension. The location of the fracture line is important in determining the surgical approach for facial nerve decompression.
Case report
A 33-year-old woman presented with delayed onset left facial weakness following a motor vehicle accident in which she was unconscious for 2 days. She noticed asymmetrical left facial features 3 days post trauma. There was associated bleeding over the left ear which halted spontaneously. There was coexisting reduced hearing over the left ear with intermittent tinnitus. Otherwise she did not register symptoms of vertigo. On examination, she had left facial nerve paresis House–Brackmann grade V. Otoscopic examination showed a dried blood clot in the left external auditory canal. She was given oral prednisolone 60 mg daily for 2 weeks and was referred for facial physiotherapy. HRCT of the temporal bone showed a longitudinal fracture crossing the mastoid air cells with possible involvement of the facial canal (Figure 1).
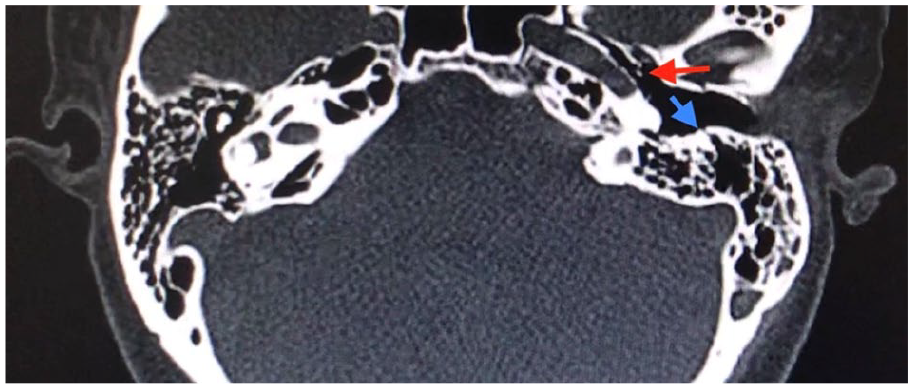
Preoperative high resolution computed tomography of the temporal bone shows longitudinal fracture involving the mastoid air cells and anterior wall of the external auditory canal as depicted by the blue arrow. There is a bony spicule seen at the tympanic segment of the facial nerve, as illustrated by the red arrow.
Initially, she was not keen for surgical intervention in view of the multiple injuries that she sustained following the motor vehicle accident. However, there was no improvement in her left facial nerve function despite conservative treatment for 3 months, which consisted of vigorous facial physiotherapy. Thus, she was referred to the otologic centre for further management. On review, the left facial nerve paresis House–Brackmann grade V remained (Figure 2(a) and (b)). A pure tone audiogram (PTA) revealed left mild to moderate conductive hearing loss while the right hearing was normal. A stapedial reflex test revealed absent acoustic reflex over the left ear. Schirmer’s test was normal suggesting that the site of lesion was distal to the second genu. In light of no improvement in facial nerve function, she was planned for left facial nerve decompression 2 weeks after being referred to the otologic centre.

Facial nerve function. (a) and (b) Preoperative facial nerve function shows House–Brackmann grade V facial nerve paresis. (c) and (d) Postoperatively, the facial nerve function improves to House–Brackmann grade II.
A postauricular incision was performed 1 cm posterior to the postauricular sulcus and cortical mastoidectomy was performed. The antrum was identified. The short process of incus and lateral semicircular canal served as landmarks for the second genu of the facial nerve. The mastoid segment of the facial nerve was traced to the stylomastoid foramen but there was no fracture line or bony spicule observed over this segment (Figure 3(a)). In parallel with the HRCT findings, there was a small bony chip seen indenting the distal segment of the tympanic segment of the facial nerve, just proximal to the second genu. The presence of the dome of the lateral semicircular canal yielded the view of the lesion site with an operating microscope. An extended posterior tympanotomy was undertaken, with 0° and 30° endoscopes being introduced by way of this corridor to inspect the tympanic segment of the facial nerve to the second genu. The incudostapedial joint was found to be disengaged. Thus, the incus was tilted gently to provide space for the endoscope, without removing it. The tympanic segment of the facial nerve looked emaciated with lack of lustre (Figure 3(b)). The second genu was preserved. On completion, a neurolysis over the tympanic segment of the facial nerve was successfully performed using endoscopic guidance. The incudostapedial joint was fixed into its position with supporting cartilage to ensure the hearing was restored.

Intraoperative findings. (a) Microscopic view shows normal appearance of the mastoid segment of the facial nerve (*). An extended posterior tympanotomy was performed. (b) Endoscopic view of the tympanic segment of the facial nerve (★) which appears emaciated by way of posterior tympanotomy. LSCC: lateral semicircular canal; PC: processus cochleariformis; SIn: short process of incus; TT: tegmen tympani.
Significant improvement was registered postoperatively with facial nerve function recovered to House–Brackmann grade II at 8 months after the operation (Figure 2(c) and (d)). The postoperative PTA showed mild to moderate conductive hearing loss over the affected ear.
Discussion
Several surgical approaches for facial nerve decompression have been performed under microscopic guidance. The transmastoid approach has been used for temporal bone fracture involving the facial nerve involving the tympanic segment of the facial nerve to the stylomastoid foramen. 1 Following cortical mastoidectomy, the mastoid segment of the facial nerve is traced from the second genu to where the nerve egresses through the stylomastoid foramen. The tympanic segment of the facial nerve is visualised by way of posterior tympanotomy. However, this approach has its limitations as the opening is relatively small and the presence of intact ossicles in the middle ear further impedes the space for surgical decompression of the nerve.
With regard to a fracture affecting the second genu or labyrinthine segment of the facial nerve, the middle cranial fossa approach is recommended if there is residual serviceable hearing. On the other hand, the translabyrinthine approach for facial nerve decompression can be considered when there is no serviceable hearing. 1 Both approaches provide great exposure of the facial nerve from the labyrinthine segment to the stylomastoid foramen. However, both procedures have some clinical drawbacks. The middle cranial fossa approach causes brain retraction and the need for dural floor reconstruction. The translabyrinthine approach is rather a salvage surgery in which the whole labyrinths are permanently removed causing permanent hearing impairment.
With the advent of the endoscope in the field of otology, various middle ear procedures have been successfully managed using this method. 3 It was discussed by Marchioni et al. in endoscopic cadaveric dissection on the anatomy of the tympanic segment of the facial nerve surgery by way of the transcanal approach. 4 The processus cochleariformis serves as an important landmark in identifying the second genu. In order to visualise the tympanic segment of the facial nerve better, the incus and head of the malleus need to be removed. In addition, the same authors incorporated the feasibility of this technique into clinical practice. 5 Similarly, Kahinga et al. shared their experience in total transcanal endoscopic facial nerve decompression involving the tympanic segment of the facial nerve, which showed promising results postoperatively. 6 The improvement in facial nerve function following transcanal endoscopic facial nerve decompression was reported to be 83.2%, with significant improvement in the postoperative air bone gap. 7 Another study mentioned the role of endoscope-assisted transmastoid approach facial nerve decompression involving the second genu and the labyrinthine segment of the facial nerve. 8
With regard to our case, the conventional transmastoid approach was initially performed. However, the lesion at the distal portion of the tympanic segment of the facial nerve was obstructed by the dome of the lateral semicircular canal with the surgical microscope. Therefore, the endoscope was used by way of the extended posterior tympanotomy as it offered various angulations within the middle ear space. This technique was similar to that described in the previous literature.4,5 The endoscope allows excellent visualisation of the middle ear structures as well as permitting a panoramic view of the operative fields. 9 However, there was slight modification in the current technique in view of the incudostapedial joint, which was found to be disarticulated. The incus was tilted rather than removing it for surgical access to visualise the whole length of the tympanic segment of the facial nerve. The incus was replaced in its position preventing worsening of hearing loss postoperatively, as evidenced by PTA. The impingement of bony spicule at the distal portion of the tympanic segment of the facial nerve was successfully removed and neurolysis along this segment was able to be performed under endoscopic guidance.
Conclusion
The application of endoscope-assisted facial nerve decompression enables the surgeon to visualise the concealed area along the course of the tympanic segment of the facial nerve as compared to the surgical view offered by the operating microscope. This technique should be considered as an option for facial nerve decompression as it offers a good outcome without compromising the hearing.
Footnotes
Acknowledgements
None.
Authors’ contributions
KM: Writing; TMITK: Conceptualisation and supervision; NAL: Data collection.
Availability of data and materials
Data sharing is not applicable to this article as no datasets were generated or analysed during the current study.
Conflict of interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient for their anonymised information to be published in this article.
