Abstract
Introduction:
Totally endoscopic ear surgery (TEES) is defined as exclusive application of endoscope transcanally in otologic surgery. This study is aimed to highlight indications and ear pathologies for TEES. In addition, intraoperative, early postoperative and delayed postoperative complications of TEES will be also described in this study.
Methodology:
This is a retrospective study of TEES performed by a single experienced and trained otologist in endoscopic ear surgery in a single institution between 1 July 2014 and 31 June 2018. A total of 43 patients were recruited in this study. Sociodemographic information, indications for TEES, ear pathologies, type of surgery performed and complications of TEES were analyzed.
Results:
The indications for TEES comprised middle ear lesion (65.1%), followed by second look surgery (14.0%), external auditory canal lesion (11.6%) and internal acoustic meatus lesion and surgery for conductive hearing loss which were 4.7%. Various external auditory canal pathologies encountered for TEES were ear canal osteoma (4.7%), acquired ear canal stenosis (2.3%) and tumor (4.7%). Regarding middle ear pathologies, limited atticoantral cholesteatoma accounted for most of the cases, 46.5%. Other middle ear lesions included adhesive otitis media (14.0%), recurrent cholesteatoma (14.0%), tumor (4.7%), otosclerosis (2.3%) and ossicular discontinuity (2.3%). Internal acoustic meatus lesion constituted 4.7% of cases. Some 4.7% of cases developed intraoperative complications, while early and delayed complications were 7.0%.
Conclusion:
TEES is a feasible surgical technique for diverse ear pathologies in the otologic specialty. It is also proven to be safe with good surgical outcomes.
Introduction
Endoscopic ear surgery (EES) is a recent technique in the field of otology. Although the operating microscope remains relevant in ear surgery, the use of endoscopes is a promising surgical technique for selected ear surgeries. The endoscope can be used either in conjunction with the operating microscope as part of a combined endoscopic–microscopic procedure, or by itself [totally endoscopic ear surgery (TEES)]. 1 Endoscopic ear surgery is now being employed for pediatric cases as well. 2
Among the advantages that TEES offers over traditional ear surgery is that the endoscope confers a wide-field view in comparison to the narrow-field view conferred by the operating microscope. In addition, endoscopes allow easy visualization of areas such as sinus tympani and hypotympanum in the middle ear that are otherwise difficult to reach with microscopes.1,3,4 A systematic review indicated that endoscopes can reveal the presence of residual cholesteatoma in up to 50% of cases, 5 with TEES also demonstrated to significantly shorten the operative time and rate of healing in attic cholesteatoma. 6 Although Kanona et al. reported a significant air bone gap improvement with EES compared with traditional methods, 7 this result could not be replicated in a subsequent study. 8
Limitations of TEES have been discussed in the literature in order to refine this surgical technique. Swarup et al. found most otologists expressed the need for better instruments in EES to improve the view of the difficult areas in the middle ear and to remove cholesteatomas, 9 arising from the one-handed method during TEES. 1 Another drawback of TEES is the complications due to the confined area of the surgical field. Despite these limitations, the complication rates for EES remain low. 10
The aim of this retrospective study is to highlight the indications and ear pathologies for TEES conducted in a hospital in Malaysia, and to analyze possible complications of the procedure. All these findings are important in order to improve the understanding of TEES, given its novelty in otology.
Methods
This is a 4-year retrospective review of TEES in Malaysia involving 43 patients. Data from all patients who underwent TEES in Hospital Sultan Ismail, Johor Bahru, Malaysia from 1 July 2014 to 31 June 2018 were used (obtained via the Otorhinolaryngology operative directory book). This study was approved by The Ministry of Health Medical Research and Ethics Committee (National Medical Research Register Identification Number: NMRR-18-3667-45566). Patients’ demographic data such as age, gender and race were documented. Patients below 18 years old were placed in the pediatric group. Details of the surgery as well as follow-up data were retrieved from the Hospital Patient’s Information System. The surgery was performed by an experienced surgeon who was trained in EES at an otologic center. A 4 mm, 18 cm 0-degree rigid John Hopkins endoscope was used intraoperatively most of the time (Figure 1). A 2.8 mm, 18 cm 0-degree rigid John Hopkins endoscope and a 2.8 mm, 18 cm 30-degree rigid John Hopkins endoscope was used whenever necessary, especially for viewing loops and corners in the middle ear space and antrum, respectively (Figure 2). The endoscope was connected to a Karl Storz 24” LED HD Monitor using Karl Storz Xenon light source which was set at 50% illumination.

A view of middle ear using 0-degree rigid endoscope.

Visualization of cholesteatoma at antrum using 30-degree endoscope.
The inclusion criteria were all patients who underwent exclusive EES that were approached transcanally only. In addition, the surgeries were performed by a single surgeon to avoid any bias in technique or outcome of the procedures. Exclusion criteria in this study were EES that were performed as combined otologic procedures, microscopic or combined microscopic approach for otologic surgeries. In this study, all types of tympanoplasty were also excluded as this procedure was conducted by many surgeons in the same hospital.
In this study, TEES was used in surgeries involving lesions in the external auditory canal, middle ear and lateral skull base, in surgeries for conductive hearing loss and second look surgeries. Ear pathologies were categorized based on whether they were external, middle or lateral skull base lesions. External auditory canal lesions were further subclassified into ear canal osteoma, acquired canal stenosis and external auditory canal tumor. Middle ear lesions included limited atticoantral cholesteatoma, adhesive otitis media, recurrent cholesteatoma, middle ear tumor, otosclerosis and ossicular discontinuity. As for the lateral skull base lesion, limited intracanalicular had been performed via transcanal endoscopic approach.
Potential intraoperative and postoperative complications of TEES were analyzed in this study. Preexisting dehiscences of the tegmen tympani, facial canal or labyrinthine fistula were not considered as complications. Similarly, removing ossicles to facilitate the procedure was not regarded as a complication. Early postoperative complication of TEES was defined as a complication that occurred immediately after to 6 months postoperatively, while delayed postoperative complication happened after 6 months postoperatively. Therefore, the minimum follow-up duration for all patients was 6 months following TEES.
Results
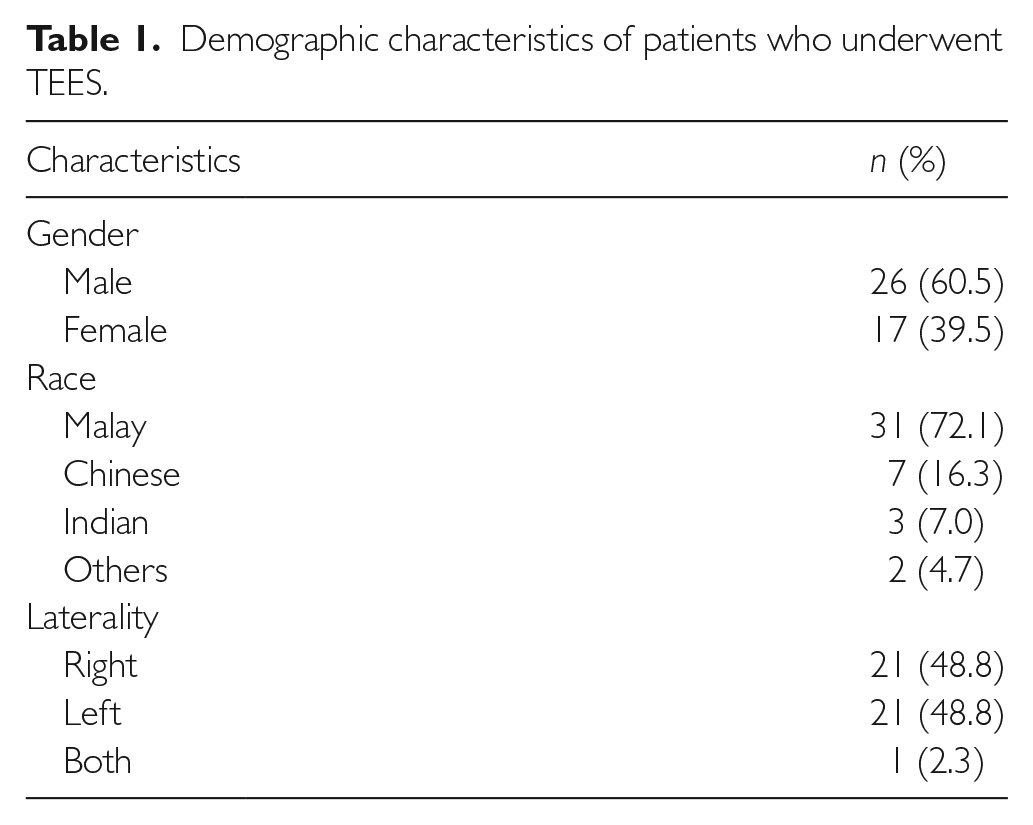
A total number of 43 patients had undergone TEES in Hospital Sultan Ismail, Johor Bahru, Malaysia between 1 June 2014 and 30 June 2018. The mean ± standard deviation age was 40.6 ± 17.2 years old with a range of 8–79 years old. TEES was successfully performed in five pediatric patients. Demographic characteristics including gender, race and laterality of ear involved during surgery were documented (Table 1). Information on TEEs performed (Table 2), as well as data indicating the underlying ear pathology for TEES and the type of surgery carried out (Table 3) were collected. Middle ear diseases contributed the majority of the cases. External auditory canal pathology and lateral skull base lesion conferred a small number of cases.
Demographic characteristics of patients who underwent TEES.
Indications for TEES.

Ear pathologies and type of surgery in which TEES were performed.
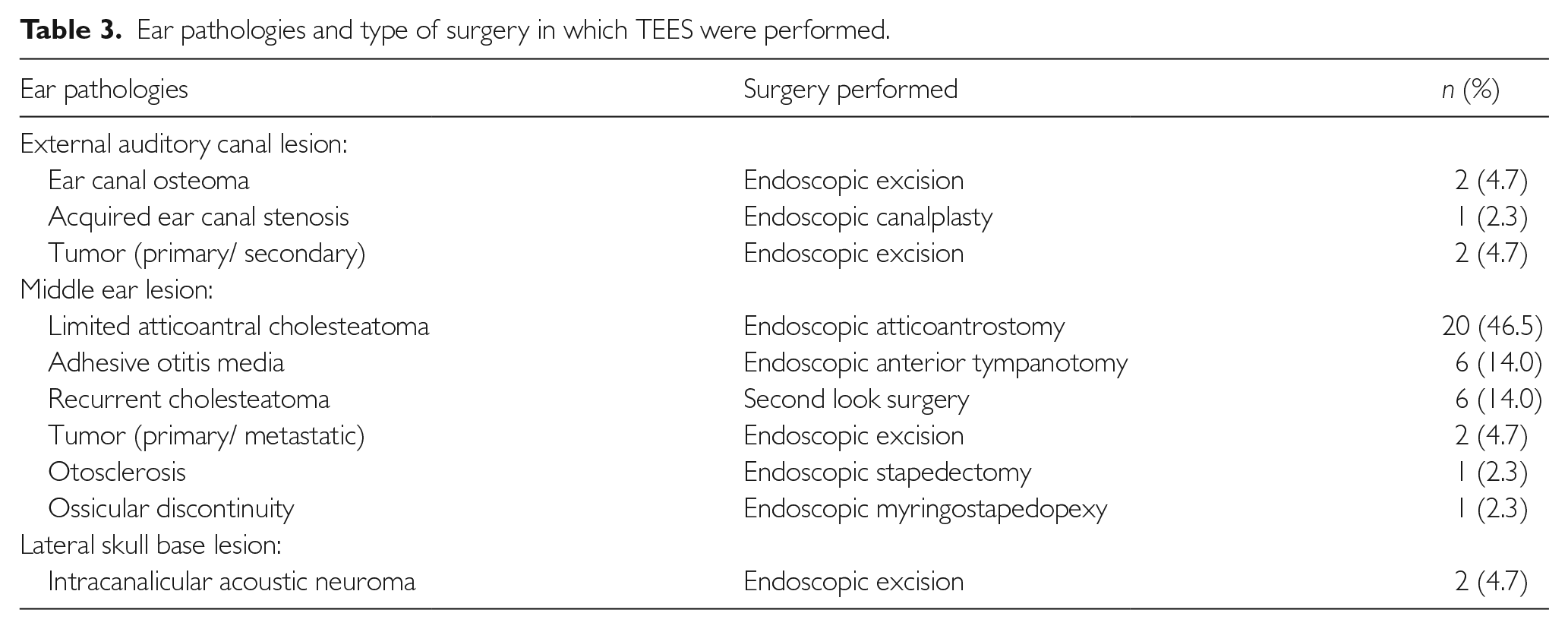
Two cases of external auditory canal squamous cell carcinoma were resected endoscopically. Both cases were Stage I disease (Pittsburg Staging T1N0M0). Intraoperatively, frozen sections were sent to ensure clear resection margin. In view of clear resection margin, postoperative radiotherapy was not given. Both cases had been followed up monthly for 6 and 12 months, respectively. To date, there has been no evidence of recurrences.
The complications of TEES were subdivided into intraoperative, early and delayed postoperative complications (Table 4). Regarding early postoperative complications, two patients developed ear discharge within 1 week following TEES, which completely resolved with systemic and topical antibiotics. None of them required hospitalization. One patient experienced transient facial nerve paresis on the sixth day post-TEES. She underwent totally transcanal endoscopic atticoantrostomy for limited atticoantral cholesteatoma. Varicella zoster antibody IgG titer was reactive. She was treated with tapering dose prednisolone. Complete recovery of the facial nerve function was observed 3 weeks postoperatively.
Intraoperative, early postoperative and delayed postoperative complications of TEES.

Some 7.0% of the cases documented delayed postoperative complications. There were two patients who sustained acquired stenosis of external auditory canal, in which one required a second look surgery. Permanent facial nerve palsy was observed in one patient who underwent TEES for intracanalicular acoustic neuroma. This patient developed facial nerve palsy House Brackmann Grade IV immediately after the operation. The surgeon attributed this complication to possible inadvertent injury to the intracanalicular segment of facial nerve while attempting to remove the tumor.
Discussion
EES was first described about 30 years ago by Thomassin et al. 11 Since then, studies have been conducted to evaluate the feasibility of using an endoscope in otologic surgery. This surgical technique is still new in the field of otology, and would represent a steep learning curve for most of otologists. TEES has been considered minimally invasive surgery (in view of avoiding skin incision and reducing soft tissue manipulation) compared with the microscopic postauricular approach of otologic surgery. 1 Although the evolution of TEES is promising, there is currently insufficient data to establish the feasibility of this technique. Thus, our study aims to produce the first Malaysian evaluation on TEES over the period of 4 years. To date, this is the first outcome on TEES reported on the South East Asian region.
The application of TEES in the external auditory canal is less frequently compared with middle ear diseases. Two cases in our study underwent transcanal endoscopic resection of squamous cell carcinoma of the external auditory canal (both T1N0M0 diseases based on Pittsburg staging). Evidence from the frozen section assessment stated that all tumor margins were clear. Close follow-ups were arranged for both cases to monitor for any recurrence. After following up for 6 and 12 months, respectively, there was no evidence of recurrence based on clinical and radiological findings. To date, there has not been any reported case of endoscopic transcanal excision of malignant tumor in the literature. At present, more cases are needed to support TEES as a viable procedure in managing otologic oncological diseases, especially with regards to the adequacy of the resection margin as well as the need for postoperative radiotherapy.
Among middle ear problems, atticoantral cholesteatoma made up a great majority of cases. Preoperative high-resolution computed tomography (HRCT) of temporal bone is essential for the decision making of TEES. In our center, TEES was offered whenever the HRCT scan revealed limited atticoantral diseases. Utilizing endoscopy in an atticoantral cholesteatoma surgery confers the advantage of improved visualization of the hidden areas in middle ear cavity such as anterior epitympanum and sinus tympani.12-14 The 0-degree endoscope was used to assess the middle ear cholesteatoma, while the attic and antrum cholesteatomas were best inspected using 30-degree and 45-degree endoscope. 12 The use of TEES in the management of attic cholesteatoma demonstrated a reduction in postoperative pain and faster healing: Magliulo and Ianella also indicated a lower incidence of residual cholesteatoma following TEES. 6 However, Ayache et al. found that TEES did not demonstrate significant reduction in residual cholesteatoma during second look surgery compared with surgery performed using an operating microscope. 15 At present, TEES is readily incorporated in lateral skull base lesions. Increasingly, several neuro-otologic lesions such as intracanalicular acoustic neuroma are managed via an endoscopic transcanal approach.16,17 Although the number of cases reported in the literature is small, this technique has progressed tremendously in the otologic field. Similarly, there were only two patients who underwent this type of surgery at our center. The surgery rendered access to the internal acoustic meatus transpromontorily. Unlike the conventional technique, employing TEES for acoustic neuroma surgery offers many advantages such as avoiding external surgical scars, lowering the risk of cerebrospinal fluid leakage and hastening the postoperative recovery. 17 Despite its advantages, this technique is currently reserved for intracanalicular or small cerebellopontine angle tumor only.
In this study, intraoperative, early and delayed postoperative complications of TEES were analyzed. Comparing our results with the studies of Marchioni et al. and Yiannakis et al. reveals our complication rate to be higher.8,10 A possible explanation is the small number of cases used in our study (compared with 825 cases used by Marchioni et al. and the 103 cases used by Yiannakis et al.).
Two cases had intraoperative complications, both resulting from inadvertent chorda tympani injury. The complications occurred in raising the tympanomeatal flap, especially at the area of chordal eminence. With regards to early postoperative complications, two patients developed postoperative infections which were completely resolved with oral and topical antibiotics. One patient experienced transient facial nerve paresis caused by varicella zoster infection. This finding was in accordance with other reported cases following conventional mastoidectomy.18,19
Regarding delayed postoperative complications, one patient developed permanent incomplete facial nerve palsy following endoscopic transcanal removal of intracanalicular acoustic neuroma. A possible explanation for this was the intracanalicular portion of facial nerve being enwrapped by the tumor, causing inadvertent permanent injury to the facial nerve. Although considered a major complication, it is difficult to conclude that TEES is not a viable option for the removal of intracanalicular acoustic neuroma on the basis of only two cases performed in our center. In comparison, Moon et al. reported the absence of major complications following TEES in intracanalicular acoustic neuroma in a series of seven cases. 17
In this study, we highlighted the incidence of external auditory canal stenosis following TEES. To the best of our knowledge, this complication has never been acknowledged in the literature. We postulate that excessive soft tissue inflammation while raising up the tympanomeatal flap and possible thermal damage while using endoscope with xenon light sources could have been contributing factors to this problem. Although studies have shown that light-emitting diode and xenon light sources can be safely used in TEES, surgeons must still take precautions. These include reducing the light intensity, applying suctioning throughout the procedure and intermittently taking out the endoscope from the ear canal to allow cooling effects to the surrounding soft tissue to avoid injury.20,21
This present study had some limitations. The sample size was small and this study was conducted retrospectively. In the future, prospective studies with a larger sample size are needed to authenticate current findings. Apart from that, this current study involved only one surgeon at a single institution. We propose more initiatives to train experienced otologists in TEES that will yield better understanding and surgical outcome success rate. Instrumentations in TEES are crucial to ensure the feasibility of this approach in reaching ear pathology in concealed areas. 22 Therefore, specially designed instruments for TEES are warranted to improve surgical practice, as the approach differs from conventional mastoidectomy.
Conclusion
This study has demonstrated the feasibility of TEES in otologic practice. Various indications of TEES and ear pathologies were described. It also highlighted the low rate of intraoperative, early and delayed postoperative complications of TEES encountered at this center. Our results complement the applications of TEES in numerous ear conditions worldwide. As the knowledge and understanding of TEES are still developing, many aspects, including continuous hands-on training, proper instrumentations and technologies in EES, are yet to be explored.
Footnotes
Acknowledgements
None
Authors’ contributions
Khairunnisak Misron was responsible for study design, data collection and writing the manuscript. Tengku Mohamed Izam Tengku Kamalden was responsible for the conception and intellectual development of the manuscript.
Availability of data and materials
Not applicable.
Conflict of interest
The authors declare that there is no conflict of interest.
Ethical approval
Not applicable.
Informed consent
Not applicable.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
