Abstract
Background:
Obesity is associated with obstructive sleep apnoea (OSA). Weight loss is an effective treatment. Bariatric surgery for obese, symptomatic OSA patients results in weight loss and improvement in lung function and sleep apnoea. This study aimed to determine the effectiveness of bariatric surgery in improving the respiratory mechanics and sleep apnoea using a lung function test and sleep study.
Methods:
A prospective study was conducted at the Pusat Perubatan Universiti Kebangsaan Malaysia Medical Centre involving adults undergoing bariatric work-up, attending respiratory clinic or admitted for bariatric work-up. We included subjects with a body mass index (BMI) >35 kg/m2 and Apnoea–Hypopnoea Index (AHI) of >5 events/hour. Subjects were assessed at baseline and at 12±2 weeks post bariatric surgery using the following methods: a partial sleep study, lung function test, six-minute walk test (6MWT) and Epworth Sleepiness Scale (ESS) score.
Results:
Twelve subjects were analysed. Their mean age was 36±5.7 years, and eight (67%) were female. The baseline mean AHI was 24.75±9.51 events/hour, the nadir mean oxygen saturation during sleep (SpO2) was 83.6±3.8%, the mean ESS score was 16±4, the mean forced expiratory volume in one second (FEV1) was 2.66±0.35 L, the mean forced vital capacity (FVC) was 3.23±0.45 L, the mean total lung capacity (TLC) was 4.97±1.19 L, the mean expiratory reserve volume (ERV) was 0.5±0.46 L, the mean residual volume (RV) was 1.46±0.91 L, the mean adjusted diffusing lung capacity for carbon monoxide (DLCO Adj) was 22.71±5.22 mL/mmHg/min, the mean adjusted diffusing lung capacity corrected for alveolar volume (DLVA Adj) was 5.61±0.90 mL/mmHg/min and the mean 6MWT was 293±49 m. Post surgery (12±2 weeks), the mean BMI decreased from 45.5 kg/m2 to 39.7 kg/m2, with a clinically significant improvement in AHI, ESS score, nadir SpO2, FEV1, FVC, TLC, ERV, RV, DLCO Adj, DLVA Adj and 6MWT (p<0.05).
Conclusion:
Bariatric surgery improves sleep apnoea and lung function and reduces daytime somnolence.
Introduction
Obesity is a recognised global epidemic and public health concern. 1 The prevalence of obesity has increased almost threefold in the past three decades. 2 The obesity rate in Malaysia is three to four times higher than other Asian countries. 3 The National Health and Morbidity Surveys (NHMSs) done in 1996, 2006, 2011 and 2015 showed an increasing trend of obesity in adult Malaysians from 4.0% to 17.7%.4,5
Obesity affects the respiratory mechanics. With increasing body weight, lung volume is reduced, 6 causing dyspnoea in up to 80% of obese patients. The decrease in lung volume is reflected in a restrictive lung pattern on lung function parameters. 7 Studies have proven that a decrease in expiratory reserve volume (ERV) is exponential to the increase in body mass index (BMI). 8 Obesity causes a reduction in the mobility of the diaphragm, which leads to an increase in areas of lung atelectasis and ventilation/perfusion mismatch.9,10
Obesity plays a key role in the development of obstructive sleep apnoea (OSA). 11 The prevalence of sleep apnoea in obesity ranges from 55% to 100%. Excess fat deposition anterolateral to the upper airway appears to be greater in OSA patients compared to the general population. 12 Leptin is a hormone that is produced by adipose tissue. Obesity is typically associated with increased levels of leptin. Leptin resistance is also a possible cause of obesity in OSA patients. 13
Obese patients frequently complain of dyspnoea and a lack of physical activity. 14 This lack of physical activity combined with a sedentary lifestyle predisposes them to more weight gain. The six-minute walk test (6MWT) can be used to assess the functional exercise capacity. This is a self-paced test which is easily done, relatively cheap and well tolerated, as subjects can choose their own intensity of exercise and are allowed to stop and rest as needed. 15
The main aim in managing obesity is achieving sufficient and sustained weight loss. This can be done by a combination of diet, lifestyle changes, pharmacotherapy or surgical intervention. The available bariatric procedures are Roux-en-Y gastric bypass (RYGB), laparoscopic sleeve gastrectomy (SG) or biliopancreatic diversion. Bariatric surgery is an important adjunctive therapy, as it offers sustained weight loss and has been shown to improve clinical outcomes such as mortality. 16 Bariatric surgery has also been reported to show a substantial improvement in the Apnoea–Hypopnoea Index (AHI) post surgery. 11 The National Institute for Health and Care Excellence (NICE) guidelines recommend bariatric surgery as a treatment option for adults with a BMI ⩾40 kg/m2 or between 35 and 39.9 kg/m2 in the presence of significant co-morbidities. 17 SG and RYGB are two popular choices of bariatric surgery with similar effects on metabolic parameters, ingestive behaviours and gut hormone secretions. 18
The aim of this study was to determine the effectiveness of laparoscopic SG in improving the sleep parameters (i.e. AHI, nadir oxygen saturation during sleep (SpO2 nadir) and Epsworth Sleepiness Scale (ESS) score) and pulmonary parameters (i.e. forced expiratory volume in one second (FEV1), forced vital capacity (FVC), total lung capacity (TLC), ERV, residual volume (RV), adjusted diffusing lung capacity for carbon monoxide (DLCO Adj) and adjusted diffusing lung capacity corrected for alveolar volume (DLVA Adj)). The secondary aim was to determine the correlation between degree of weight loss and the improvement in physical activity measured by the 6MWT.
Methods
This was a prospective longitudinal study conducted between May and September 2019 following approval from the Research Ethics Committee Hospital Canselor Tuanku Muhriz Pusat Perubatan Universiti Kebangsaan Malaysia (PPUKM; research code FF-2019-151) and the Ministry of Health Malaysia (NMRR Research ID 50566). A flow diagram of the study design is shown in Figure 1.

Study flow chart.
The inclusion criteria were adults aged ⩾18 years attending a bariatric work-up clinic or respiratory clinic or admitted for bariatric surgery work-up with morbid obesity (i.e. a BMI >35 kg/m2) and OSA (AHI >5 events/hour). We excluded subjects who did not consent or who had underlying obesity hypoventilation syndrome (OHS) without OSA or who had underlying co-morbidities that worsen apnoea symptoms such as congestive cardiac failure, active malignancy, narcolepsy, active alcohol or drug abuse, treatment-refractory dementia, psychotic illness and active use of drugs that disturb the sleep architecture (i.e. hypnotics or stimulants of central nervous system). All subjects provided written informed consent.
Subjects were evaluated prior to bariatric surgery and were reassessed 12±2 weeks after bariatric surgery. Demographic data (age, sex and ethnicity), anthropometric data (height, weight and BMI), subjective data (ESS) and objective data (partial sleep study, full lung function tests and 6MWT) were collected.
We performed an in-lab sleep study type 3 polysomnography (PSG) using the SOMNOtouch™ (Somnotec, Selangor, Malaysia). Attachment of the device was done by trained respiratory sleep technicians. The full lung function test was performed using the Vmax™ Autobox System (DanMedik, Selangor, Malaysia) and complied with the American Thoracic Society and European Respiratory Society guidelines. All subjects were monitored by a trained respiratory technician throughout the procedure. The 6MWT was conducted at the PPUKM respiratory laboratory. Subjects were instructed to walk as far as possible in six minutes back and forth over a six-metre walking course due to infrastructure limitation in our respiratory laboratory. The ESS is a self-administered validated questionnaire comprising an eight-item scale. Subjects were asked to rate the likelihood of dozing in eight different daily lifestyle activities from 0 (would never dose) to 3 (high chance of dozing). Higher cumulative scores indicate greater excessive daytime somnolence.
Taking the power of the study to be 80% with an alpha of 0.05, a standard deviation of AHI 22.8 events/hour from a published study by Lettieri et al. 19 and interpreting using the power table, the resulted sample size was estimated to be 15 patients, with an anticipated withdrawal rate of 10%. The total number of patients needed was therefore 17 patients.
All data collected are shown as mean±standard deviation when applicable. All tests are two-tailed, and a p-value of <0.05 was presumed to represent statistical significance. A paired t-test was used to compare pre- and postoperative results. Pearson correlation coefficients were used to analyse variables of anthropometric measures, lung functions tests (FEV1, FVC, ERV, RV, DLCO Adj, DLVA Adj and TLC) and 6MWT results. All analysis was performed using IBM SPSS Statistics for Windows v 25.0 (IBM Corp., Armonk, NY). As this was an exploratory study, a control for multiple comparisons was not considered.
Results
Thirty-five patients were eligible for the study. After being counselled on the objectives and procedures, 20 subjects consented to participate. Two subjects did not undergo the surgery, while another six subjects did not turn up for follow-up. Among the reasons for not attending post-bariatric reassessment was migration to different cities and logistical issues.
The demographic and anthropometric characteristics of the subjects are shown in Table 1. The ratio of males to females was 1:2. The mean age was 36.2±5.7 years. Malays comprised 83% of the subjects, while the rest were Indians. The main ethnic group in Malaysia was not represented in this study. The baseline mean weight was 124.1±21.8 kg, and the mean BMI was 45.5±5.8 kg/m2. All subjects underwent laparoscopic SG, with an average length of stay of five days. There was a significant weight reduction, with a mean weight difference of 16.7±5.0 kg, a mean percentage of weight loss (%WL) of 13.48±3.53 and a mean BMI difference of 5.75±1.33 kg/m2.
Demographic and anthropometric data of subjects.

DM: diabetes mellitus; GERD: gastroesophageal reflux disease.
Out of 12 subjects with morbid obesity and OSA, 33% had hypertension, 25% had underlying type 2 diabetes mellitus (DM) and dyslipidaemia and 16% had gastroesophageal reflux disease. Ninety-two per cent of subjects had at least one co-morbidity.
The values of pulmonary parameters, sleep parameters and the 6MWT pre and post bariatric surgery are presented in Table 2. All subjects who underwent bariatric surgery showed a marked improvement pre and post bariatric surgery. Pre bariatric surgery, 58% of subjects had severe OSA, 25% had moderate OSA and 17% had mild OSA. Post bariatric surgery, 17% had no OSA, 50% had mild OSA and 25% had moderate OSA. However, 8% had persistent severe OSA. There was a significant reduction in AHI, with a mean difference of 13.08±5.71 events/hour post bariatric surgery. The correlation between improvement in AHI and reduction in weight is shown in Figure 2. Subjective measurement based on ESS score also showed an improvement, with a mean difference of 8.2±3.4 post bariatric surgery (Figure 3).
Comparison of sleep, pulmonary parameters and 6-MWT pre and post bariatric surgery.

Wilcoxon signed rank test.
AHI: Apnoea–Hypopnoea Index; SpO2: nadir mean oxygen saturation during sleep; ESS: Epworth Sleepiness Scale; FEV1: forced expiratory volume in one second; FVC: forced vital capacity; TLC: total lung capacity; ERV: expiratory reserve volume; RV: residual volume; DLCO Adj: adjusted diffusing lung capacity for carbon monoxide; DLVA Adj: adjusted diffusing lung capacity corrected for alveolar volume; 6MWT: six-minute walk test.
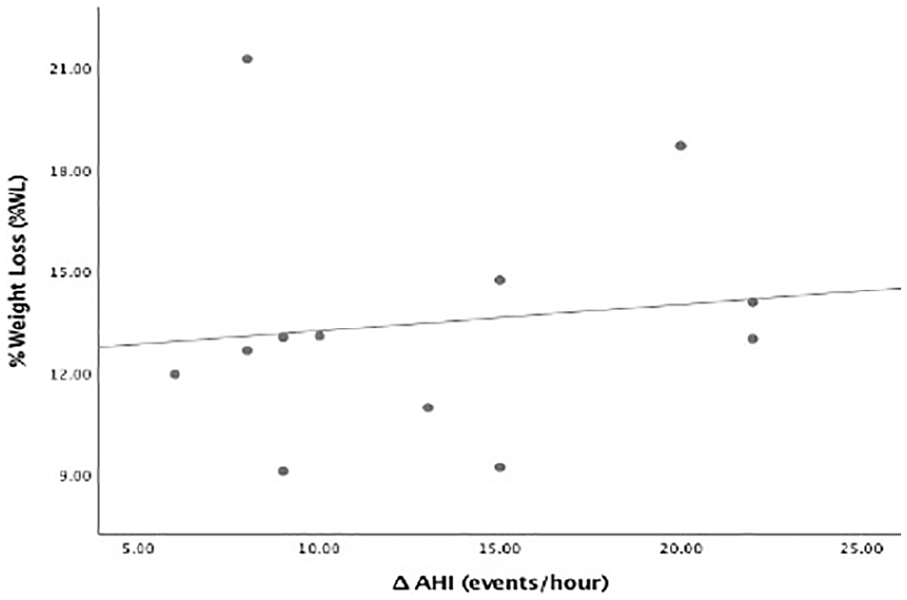
Correlation between percentage weight loss and the difference in the Apnoea–Hypopnoea Index post bariatric surgery.

Distribution of Epworth Sleepiness Scale score.
Analysis of pulmonary parameters showed an increase in RV, ERV and TLC by a mean percentage of 12%, 23% and 4%, respectively (Figure 4). These results are best explained by the improvement in lungs restriction due to weight loss. The improvement in extra-pulmonary restrictions led to an increased available unit area of lung parenchyma and was shown by a marked improvement in DLVA (Figure 5).

Comparison of total lung capacity, expiratory reserve volume and residual volume.
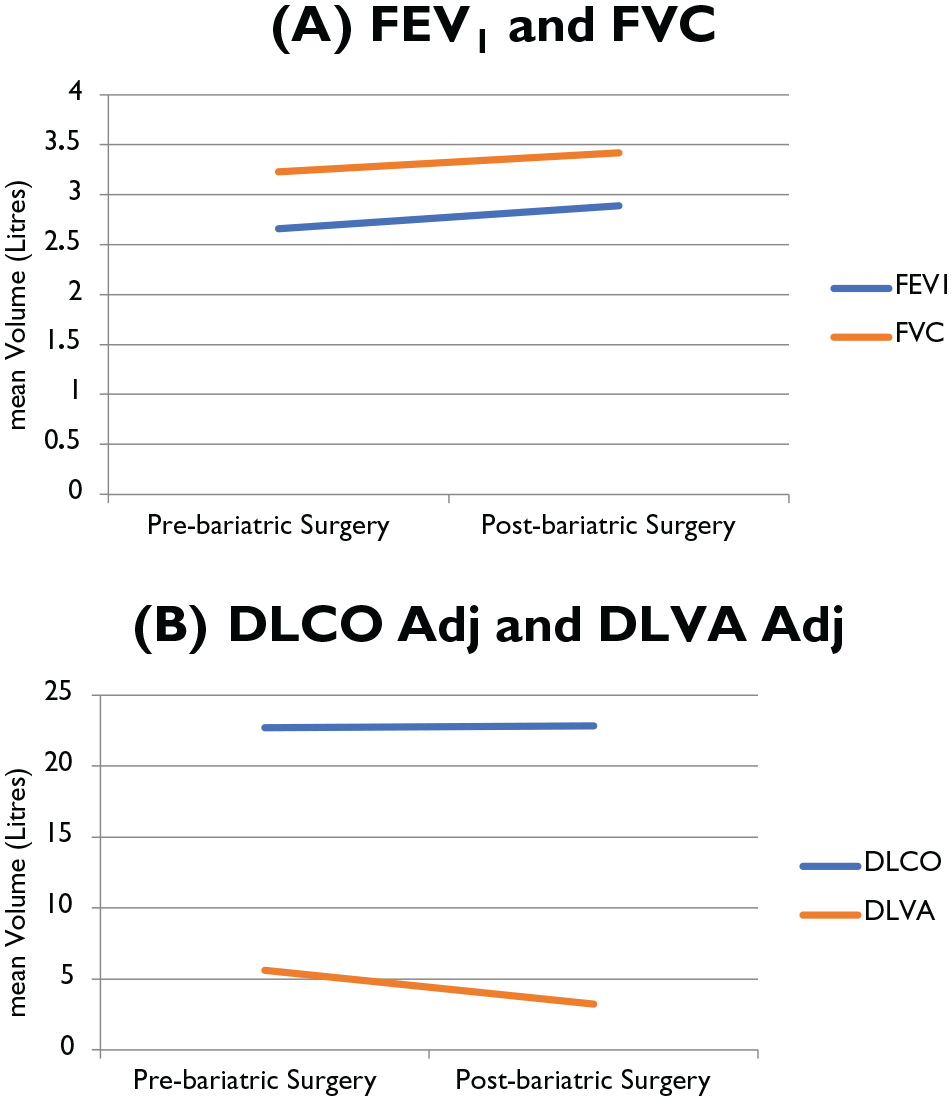
Effects of weight loss on pulmonary parameters. (a) Improvement of forced expiratory volume in one second and forced vital capacity post bariatric surgery. (b) Improvement of adjusted diffusing lung capacity corrected for alveolar volume post bariatric surgery with preserved adjusted diffusing lung capacity for carbon monoxide.
The distance traversed by all subjects pre and post bariatric surgery showed a marked improvement in correlation with the degree of weight loss, as shown in Table 2 and Figure 6. All subjects completed the 6MWT without premature breaks, and there were no complications seen during the procedure.

Correlation between weight loss and improvement in the six-minute walk test.
The main complications seen in our subjects post laparoscopic SG were bloatedness, regurgitation and nausea. All 12 subjects reported similar symptoms in the first six weeks, but only four subjects had persistent symptoms after 12 weeks of surgery. In our study, none of the 12 subjects reported major complications post surgery.
Discussion
Obesity is a global health problem that has been linked with non-communicable diseases such as cardiovascular and metabolic diseases, immunological disorders, chronic kidney disease and sleep apnoea. 20 Obesity affects an individual’s productivity and quality of life and leads to early disability, early retirement and even premature death. 21 Our subjects were slightly younger compared to Western countries, with a mean age of 36±6 years. 8 The incidence of obesity was higher in females and those of Malay ethnicity in our study. This is consistent with the NHMS 2015 data where females had a higher prevalence (20.6%) compared to males (15%). In that survey, the prevalence of obesity was highest in Indians (27.1%). Our study had 10 Malay, two Indians and no Chinese subjects.
Consistent with previous studies, 4 92% of our subjects reported at least one co-morbidity. Of the 12 subjects, four had underlying hypertension, three had type 2 DM and three had dyslipidaemia. It is hypothesised that obesity leads to increase visceral fat, which results in increase expression of angiotensin II and angiotensin I, predisposing them to hypertension. High insulin resistance with failure of insulin production increases the risk of type 2 DM in obese patients. 22 Although we did not look for the effect of bariatric surgery on major co-morbidities, studies and meta-analyses have proven that bariatric surgery decreases the prevalence of hypertension, type 2 DM and dyslipidaemia.23,24
Achieving a sufficient and sustainable weight reduction is the main treatment strategy against obesity. Lifestyle modification alone has good short-term results, but up to 66% of patients regain weight within one year. Pharmacotherapy in conjunction with lifestyle interventions has shown a better outcome. However, maintaining a sustained weight loss is still difficult, and many fail to achieve this. 25 Bariatric surgery as an adjunctive treatment has demonstrated a sustainable and greater degree of weight loss compared to conventional therapy alone. This is especially true in SG and RYGB. 18 SG was the preferred method at our centre, as most of our subjects had a BMI >35 kg/m2 with at least one co-morbidity. SG has been shown to be an easier and safer technique which can be performed with different degrees of intestinal bypass. 18 SG has also been shown to improve risk according to the American Association of Anesthesiologists, and when combined with the laparoscopic approach, it can further reduce major complications post operation and is generally better tolerated.18,26 Twelve of our subjects complained of bloatedness, regurgitation and nausea post laparoscopic SG. The number of subjects with these symptoms decreased, with only four subjects with persistent symptoms after 12 weeks. While symptoms of regurgitation may have an effect on FEV1, this was not the case in our study.
Our study showed a mean weight loss of 16.7±5 kg within three months. Reports have shown that the peak average percentage of weight loss is seen at nine months and is sustained for more than 18 months. 27 The steepest inclination degree of weight loss is seen in the first six months post bariatric surgery and plateaus after 12 months. 27
Weight loss has been shown to have a clinically relevant effect on OSA at one year, and this effect has been seen even at four years of follow-up.28,29 A prospective multi-centre study involving 132 patients showed that OSA was cured in 45% of cases and cured or improved in 78% of cases after bariatric surgery. 30 The improvement in OSA appears to be greater in patients with more severe disease. 31 From our results, the AHI reduced from a mean AHI of 24.75 events/hour to 16.7 events/hour post bariatric surgery. The improvement in AHI correlated with weight loss, as the more weight loss achieved by the, the greater the reduction in AHI. In comparison to other studies, 11 our study was conducted using a type 3 unattended PSG. As such, we were unable to identify subjects who may have overlap OSA with OHS. The prevalence of OHS in the obese population is estimated to be between 8% and 20%, and patients are typically morbidly obese with severe OSA and hypersomnolence. 32 This may explain why our subjects only showed an improvement in mean nadir SpO2 of only 2% after bariatric surgery.
Continuous positive airway pressure (CPAP) therapy remains the gold standard treatment for OSA. It is recommended that CPAP therapy be initiated early prior to bariatric surgery 33 and continued until reassessment of OSA is done after surgery. 19 In our study, only one subject agreed and was commenced on CPAP therapy and continued on it after the surgery, while the rest were not keen due to logistical and cost issues. In our study, we demonstrated a significant improvement in AHI and symptoms based on the ESS pre and post bariatric surgery. These findings are similar to previous studies, 11 although these studies were conducted over a longer duration, and the mean AHI was higher at 54.69 events/hour. In our study, there were subjects with baseline severe OSA that had persistent AHI >5 events/hour, despite an improvement in ESS score after achieving sufficient weight loss post bariatric surgery. This group of patients, termed as non-sleepy OSA, is challenging for clinicians to treat. A review of the non-sleepy OSA subgroup of patients by Montserrat et al. showed conflicting results, and more evidence is needed before initiating CPAP therapy. 34 Most of these patients do not adhere to long-term CPAP therapy, as they deny symptoms of excessive daytime somnolence, with 70% of patients having elevated levels of AHI post bariatric surgery, with a mean ESS score of 10.8±4.10, who discontinue CPAP therapy on their own. 19
Obesity is associated with a decrease in lung function. In a study involving 113 patients, symptoms of OSA as well as pulmonary function measured with spirometry were found to improve significantly five years after bariatric surgery. 35 Consistent with previous reports, 8 our study also demonstrated a marked improvement in ERV post bariatric surgery, with increments in TLC and RV. Obesity was proven to reduce the ERV, leading to an increase in dyspnoea and respiratory drive, and in turn an increase in the inspiratory reserve volume. It is also postulated that reduction in ERV leads to an increase area in atelectasis. Achieving adequate weight loss reverses the process and thus improves the ERV. 8 Our results are best explained by an improvement in diaphragm mobility due to a reduction in extra-pulmonary restriction and, as a result of a reduction in extra-pulmonary restriction, the available unit area of lung parenchyma for respiration improved. This was demonstrated in our study based on the marked improvement in DLVA Adj, while the DLCO Adj was preserved. To the best of our knowledge, this is the first study to use DLVA Adj to consolidate the hypothesis of the effect of obesity on respiratory mechanics.
Walking is a fundamental activity of life and reflects the capacity of an individual to undertake daily activities. In our study, we used the 6MWT as a surrogate quantifier for physical activity. It is neither specific nor sensitive, but the 6MWT has three distinct advantages. It is simple, affordable and can be done by obese subjects who are unable to tolerate maximum exercise capacity such as cycling or using a treadmill. In our study, we found an increment ranging from 40 to 80 m post bariatric surgery. The distance achieved appeared to be better with a higher degree of weight loss. In comparison with previous studies, 36 where an average increment of 150 m was seen in subjects post bariatric surgery, we believe that our results were less because our subjects failed to achieve their maximum possible weight loss. Previous studies 37 took longer (6 or 12 months) post bariatric surgery before repeating the test.
OSA, like obesity, is a chronic progressive disease and is associated with a relapse in weight regain as reported in a meta-analysis which showed that at 20 years, only 48.9% of subjects had excess weight loss. 38 From our study, the role of bariatric surgery as a treatment strategy for weight reduction in obese patients should be further integrated and utilised in Malaysia. Bariatric surgery should not be considered as a ‘last option treatment’, nor should it be considered as a ‘cure all’. Laparoscopic SG is a safe and well-tolerated method of bariatric surgery. It is also associated with fast recovery and provides good outcome.
Our study showed the positive impact of bariatric surgery in reducing the AHI due to adequate and effective weight loss as early as three months post surgery. The reduction in abdominal girth and improvement in lung function reduces airway obstruction. For OSA patients who have difficulty tolerating CPAP or who do not adhere to CPAP therapy, bariatric surgery is a possible treatment option. For severe OSA patients, early initiation of CPAP at least four to six weeks prior to surgery and post surgery until further assessment of OSA by a respiratory physician before discontinuing CPAP therapy remains beneficial. 19 Based on our results, a reassessment of sleep apnoea can be done as early as three months and is comparable to studies 16 in which their reassessment was done at 6, 9 or 12 months.
Our results support the findings of a meta-analysis that showed that bariatric surgery compared to non-surgical treatment of obesity has a greater effect on weight loss. In the same study, waist circumference appeared to decrease more after bariatric surgery than after non-surgical treatment. 39
We did not use accelerometers, pedometers or the internal physical activity questionnaire as tools to quantify physical activity levels in our study. We chose the 6MWT because it is a safe, cheap and simple procedure and has been used as a clinical indicator for improvement of physical activity post bariatric surgery. 15 The 6MWT provides a quantitative measurement to assess the physical activity of each individual, while a quality-of-life questionnaire provides the qualitative index. Using both clinical instruments, the treating clinicians can gauge and prescribe a better physical rehabilitation programme post bariatric surgery in order to maximise the achievable weight loss post bariatric surgery.
This study has some limitations. The sharp incline in degree of weight loss during the first three months is likely to be influenced by short-term behavioural changes (i.e. healthy diet and increased physical activity). However, the short follow-up may underestimate the improvement in pulmonary parameters and sleep apnoea post bariatric surgery, as the patients might not yet have reached the maximum achievable and sustainable weight loss. Second, we did not address the dietary habits and the physical activity of our subjects. This may further underestimate the effects of bariatric surgery. Furthermore, in this study, type 3 PSG was used instead of type 1 PSG. A type 1 attended full PSG with an arterial blood gas measurement would provide more data and enable subjects with overlap OSA and OHS to be analysed. Another limitation is the small sample size of 12 subjects.
Conclusion
Obesity is a chronic progressive disease associated with metabolic conditions. In our study, laparoscopic bariatric surgery showed an improvement in AHI and pulmonary function parameters (e.g. lung volume, gas transfer and FEV1). This study describes the benefits of bariatric surgery in OSA patients as early as three months post surgery.
Footnotes
Acknowledgements
The authors would like to thank all participants for their involvement and cooperation during the course of this study. We are also grateful to Universiti Kebangsaan Malaysia for providing us fundamental grant with research code FF-2019-151.
Authors’ contributions
All authors were involved in literature review, study proposal submission to the Institutional Review Board, data collection, data analysis and paper write-up.
Availability of data and materials
The data sheets generated and analysed during the study are available from Dr Ahmad Adib Bin Mohd Nasir.
Ethical approval
Ethical approval to report these cases was obtained from the Research Ethics Committee of the Universiti Kebangsaan Malaysia (reference number: FF-2019-151).
Informed consent
Written informed consent was obtained from all participants before the study.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship and/or publication of this article: This research received grant from the Universiti Kebangsaan Malaysia (FF-2019-151).
