Abstract
Background:
Depression and binge eating contributes to less weight loss after bariatric surgery. The lack of standardized assessment of depression and binge eating in bariatric patients makes it hard to identify and provide treatment to relevant patients. This study aimed to enhance the accuracy of identifying binge eating and depression in bariatric patients before surgery. We determined the agreement of brief screening tools for depression, binge eating and quality of life with established questionnaires used in psychological assessment of bariatric patients.
Methods:
In total, 120 patients completed both screening tools and established questionnaires before surgery during their psychological assessment sessions. Cohen’s kappa was conducted to determine whether Patient Health Questionnaire-2 agreed with the Beck Depression Inventory II in identifying depression; and if Patient Health Questionnaire-Binge agreed with the Binge Eating Scale in identifying binge eating. To investigate the degree of agreeableness between the RAND 36-Item Health Survey and Moorehead–Ardelt Quality of Life Questionnaire II on quality of life, Bland Altman analysis was performed.
Results:
Our results show that agreement between Patient Health Questionnaire-2 and Beck Depression Inventory II (k=0.35) was fair. We found that agreement between Patient Health Questionnaire-Binge and Binge Eating Scale (k=0.41) was moderate.
Conclusions:
These results indicate that the respective brief instruments’ identification of depression and binge eating is comparable to established questionnaires. Our results play a role in offering brief screening tools to be included at different points of assessment, together with established questionnaires and clinical interviews for a more accurate and comprehensive assessment.
Introduction
Approximately 20–30% of patients that undergo bariatric surgery regain weight after 18 months to 2 years.1,2 Psychiatric comorbidities contribute to an inability to maintain weight loss after surgery and psychosocial issues such as inadequate coping strategies, psychological inability to adjust to physiological and dietary changes, and poorer quality of life (QoL) after surgery.3–5 Leptin is a hormone that reduces appetite. 6 Exposure to chronic stress and a high-fat diet resulted in significant reduction of the protein of leptin receptor in the hypothalamus. 7 The reduction of leptin receptor or leptin resistance may increase appetite during stress and result in weight gain. Neuropeptide Y also plays a pivotal role in appetite stimulation and obesity. 8 Stress is associated with elevated neuropeptide Y levels, 9 which increase appetite and lead to weight gain. As such, poorer weight outcomes after bariatric surgery observed when pre-existing psychiatric conditions worsen after surgery may be associated with hormonal and neurobiological marker changes.10,11 Consequently, pre-surgical psychological assessment has been recommended to identify patients that need pre- or post-surgical psychological and medical interventions.10,11
In bariatric surgery patients, the lifetime prevalence of major depressive disorder (MDD) ranges from 22–55%.4,12,13 Pre-surgical depression accounts for 17% of the variance weight loss four years after surgery. 14 In particular, pre-surgical sub-clinical cognitive and affective symptoms of depression predicted less weight loss at six and 12 months after surgery. 15 Furthermore, pre-surgical depressive symptom improvements after surgery diminish over time.4,14 Pre-surgical depression also contributes to post-surgical depression,4,14 which accounts for a further 2.2–4.2% of variance in sub-optimal weight loss after surgery.4,12,16 Although some studies indicated pre-surgical depression has limited predictive value on weight outcomes,4,16 an integrative review implied methodological differences contributed to such findings. As such, various authors have urged assessment for and treatment of pre-surgical depression.10,11,17
The prevalence of Binge Eating Disorder (BED) in bariatric patients ranges from 15% to 56%, whereas subclinical the prevalence of BED ranges from 6% to 64%.18–20 Pre-surgical BED predicts a higher body mass index (BMI),16,17,20,21 less weight loss16,19,20,22 and co-morbid depression and anxiety post-surgery. 23 Although some studies reported pre-surgical BED was not predictive of weight loss after surgery 24 and suggested there is remission of BED post-surgery, such trends were limited to 12 months after surgery.25,26 Overall, studies point to pre-surgical BED affecting weight outcomes in the longer term after surgery. Identifying patients with BED before surgery to provide them with treatment remains important.
Systematic review suggests that bariatric surgery’s impact on patients’ QoL is inconsistent. 27 Improvements in QoL post-surgery have been reported, but QoL declined two years post-surgery and remained below the population norm. 28 The impact of QoL on weight change is also unclear.12,29,30 Pre-surgical depression and BED have contributed to poorer QoL, 5 however, the relationship between pre-surgical depression, BED, QoL and weight change post-surgery needs further clarification.
Psychological treatment for psychiatric issues in bariatric patients has been associated with more weight loss after surgery. However, there is no standardized psychological assessment method to identify bariatric patients for psychological treatment.1,31 Psychological assessment is not routinely administered. 12 Structured diagnostic interviews are the gold standard in assessing psychiatric conditions but only two studies have included them within psychological assessments of bariatric patients. 32 Others have used self-report inventories or clinical interviews instead. Patients have also expressed fatigue in filling out self-report inventories and going through structured diagnostic interviews. 33
In addition to mental health examinations by psychologists or trained mental health professionals, screening measures could enhance the accuracy of identifying bariatric patients with psychological issues if included as part of the pre-operative screening process. 24 Screening measures administered at a doctor consultation before the mental health examination session may help to reduce participant fatigue. However, there are limited studies on screening questions used in the bariatric surgery population.29,34,35 Previous studies only examined the correlation of screening questions Patient Health Questionnaire (PHQ) and PHQ-9 with established questionnaires.12,29,34,35 Only one other study used, but did not examine, the psychometric properties of a shorter screening instrument, PHQ-2, in the bariatric population. 35 To establish the psychometric relevance of screening questions, there is a need to investigate their agreement with established questionnaires used in the bariatric population.
The importance and urgency of screening for depression and psychopathology is further highlighted by a higher suicide rate in the bariatric population, 36 where psychopathology and depression have been known to increase suicide risk. 37 Bariatric surgery patients improve their mood, QoL and BED after receiving psychological interventions.38,39 As such, screening for depression and psychopathology has been recommended pre- and post-bariatric surgery so that psychological interventions can be rendered when necessary. 37
Psychopathology is related to physiological markers, impacts weight loss outcomes and contributes to a higher suicide rate in bariatric patients. The optimal strategy for evaluating patients’ mental health prior to bariatric surgery needs further investigation. 24 In addition to clinical interviews, it has been recommended to include screeners in the process. 24 Hence, it is important to establish the agreement of psychological and QoL screening instruments with established measures. The current paper’s broad aims are to determine:
the degree of agreeableness between PHQ-2 and Beck Depression Inventory II (BDI-II), PHQ-Binge and Binge Eating Scale (BES) in identifying clinical versus non-clinical symptoms;
the degree of agreeableness between Moorehead–Ardelt Quality of Life Questionnaire II (M-A QoLQII) and RAND 36-Item Health Survey (RAND 36) in measuring QoL; and
the relationship between PHQ-2, PHQ-Binge, BDI-II, BES and outcome measures such as M-A QoLQII, RAND 36 and weight changes after surgery. Given that only 40% of patients return for follow-up visits within 12 months post-surgery, 40 we decided to follow weight changes until 6 months after surgery to have a more representative sample of post-surgery patients.
The specific hypotheses include:
there is significant degree of agreeableness between PHQ-2 and BDI-II, PHQ-Binge and BES, M-A QoLQII and RAND 36; and
PHQ-2, PHQ-Binge, BDI-II and BES are significantly related to M-A QoLQII, RAND 36 and weight changes 6 months after surgery.
Methods
Study sample
Patients were recruited from those referred for pre-operative psychological evaluation at Singapore General Hospital between September 2014 and December 2016. Ethical approval was obtained from Singapore Health Services’ SingHealth Institutional Review Board. Informed consent was obtained from all participants. Participants met the following inclusion criteria.
Eligible for bariatric surgery criteria based on clinical assessments by individual surgeons and meeting the criteria for surgery according to the Obesity Clinical Practice Guidelines published by the Ministry of Health, Singapore. The guidelines state that bariatric surgery is indicated in Asian patients with a BMI>37.5 without metabolic comorbidities and in those with a BMI>32.5 and metabolic comorbidities (e.g., type 2 diabetes mellitus, hyperlipidemia, etc.). 41
Above the age of 21, of sound mind and intelligence, and able to give informed consent.
Participants were excluded if they were:
(a) below the age of 21;
(b) unable to provide informed consent, had serious mental health conditions of psychosis, active suicidal thoughts, active hallucinations and/or delusion, delirium, or were educationally subnormal; or
(c) terminally ill.
Screeners were administered during patients’ first doctor’s visit. Questionnaires were administered during the pre-operative psychological evaluation with psychologists. Demographic, height and weight data were collected before surgery. Weight was measured again at a subsequent follow-up appointment 6 months after surgery.
The BMI of patients was calculated at baseline and 6 months post-surgery based on their height and weight. Weight changes were examined through:
(a) percentage excess BMI lost (%EBMIL) 6 months after surgery, by calculating excess BMI>25 kg/m2 lost 6 months after surgery compared with baseline; and
(b) percentage of total weight loss (%TWL) 6 months after surgery.
BDI-II is widely used to measure depression in research and with the bariatric population. 20 BDI-II has 21 items, each scored on a four-point scale (0 to 3). The scores range from 0 to 63. Scores of 0–19 indicate non-clinical depressive symptoms, whereas scores >19 indicate clinical symptoms. BDI-II’s reliability coefficient is 0.88, indicating high internal consistency among items. 42
PHQ-2 is a screener for depression with two items. Scores range from 0 to 6. Scores of <3 were classified as non-clinical; >3 was classified as clinical depression. PHQ-2 has a sensitivity of 82.9, specificity of 90.0 and a positive predictive value of 38.4 for MDD. 12 However, PHQ-2, a shorter screening questionnaire for depression developed from PHQ-9, has not been evaluated for its applicability to the bariatric population.
BES is a 16-item questionnaire that measures the behavioral aspects of binge eating and associated feelings and thoughts. It demonstrates good internal consistency reliability, as well as validity. BES has been found to be valid in identifying binge eating in bariatric patients. 34 Scores of ≤17 were grouped as non-binge eating, scores of >18 were grouped as clinical binge eating.
PHQ-Binge is a three-item screener for binge eating. It includes uncontrollability when eating, consuming an unusual amount of food within two hours and frequency of such behaviours over three months. Patients indicate ‘yes’ or ‘no’ to the questions. A ‘yes’ to all three items is classified as clinical binge eating. PHQ-Binge has been used to establish the prevalence of binge eating in bariatric patients but its agreement with standard measure, the BES, has not yet been established. 29
RAND 36 is used to assess QoL and has been used with bariatric surgery population previously. 43 RAND 36 measures eight health concepts relating to QoL: physical functioning; role functioning affected by physical health; role functioning affected by emotional health; energy/fatigue; emotional well-being; social functioning; pain; and general health and health change. Seven out of eight of RAND 36’s subscales have been found to be highly reliable. 44
M-A QoLQII is a brief screening tool that measures QoL specific to the bariatric population. M-A QoLQII consist of six items on a 10-point Likert scale ranging from −0.5 to +0.5, measuring a patient’s subjective impression of: general self-esteem; physical activity; social contacts; satisfaction concerning work; pleasure related to sexuality; and focus on eating behaviour. It yields an overall QoL score and has a Cronbach’s alpha coefficient of 0.84.45,46
To assess the normality of patients’ scores on the screeners and questionnaires and their weight changes, Shapiro-Wilk test was used. To investigate the degree of agreeableness between PHQ-2 and BDI-II and between PHQ-Binge and BES, Cohen’s kappa was conducted. To calculate the relevant confidence intervals, t-tests were also performed. To investigate the degree of agreeableness between RAND 36 subscales and M-A QoLQII, Bland–Altman analysis was conducted. To investigate if PHQ-2, PHQ-Binge, BDI-II and BES are predictive of M-A QoLQII, RAND 36, %EBML and %TWL 6 months after surgery, multiple regression analysis was conducted.
Results
Shapiro-Wilk test indicated that our data were normally distributed. A total of 120 participants aged 37±10 with a pre-surgery weight of 110.9±12.8 kg (BMI 41.3±4.8 kg/m2) participated in the study. They were predominantly female (64.0%) and Chinese (64.0%). Their baseline and demographic characteristics are presented in Table 1. Their mean %EBMIL was 34.4±19.3 and their mean %TWL was 22.4±2.7.
Baseline and demographics.
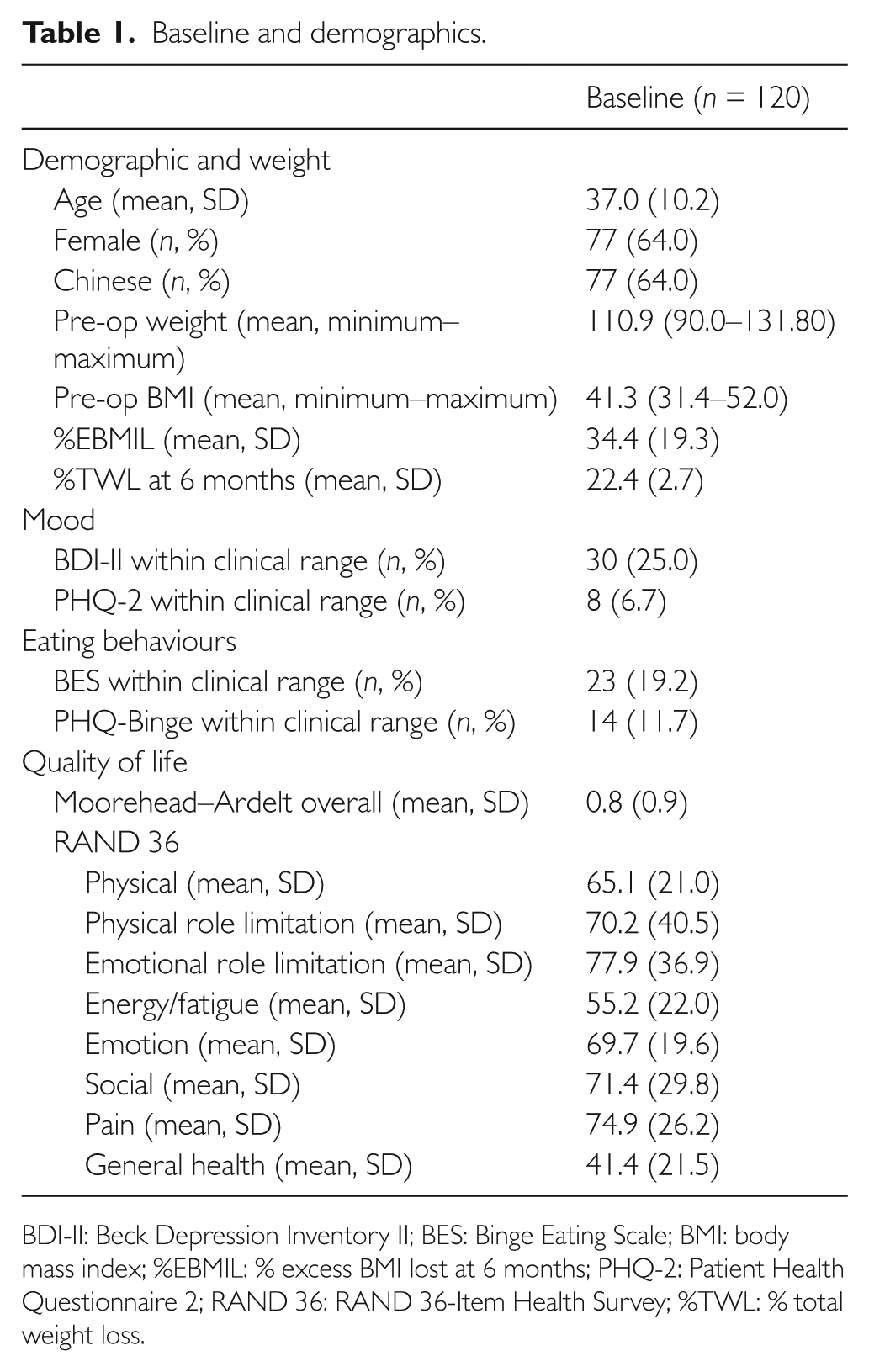
BDI-II: Beck Depression Inventory II; BES: Binge Eating Scale; BMI: body mass index; %EBMIL: % excess BMI lost at 6 months; PHQ-2: Patient Health Questionnaire 2; RAND 36: RAND 36-Item Health Survey; %TWL: % total weight loss.
Cohen’s kappa was run to determine agreement between PHQ-2 and BDI-II on identifying clinical depression. Based on Viera and Garrett’s description on the level of agreement for Cohen’s kappa, there was fair agreement between PHQ-2 and BDI-II, k=0.35 (95% confidence interval (CI), 0.395–1.72), p<0.0005. This provides support to our hypothesis that there is significant degree of agreeableness between PHQ-2 and BDI-II. Cohen’s kappa was also performed to examine for agreement between PHQ-Binge and BES on identifying clinical binge eating. The agreement between PHQ-Binge and BES was k=0.412 (95% CI, 0.533–2.33) p<0.0005, providing support to our hypothesis that there is significant degree of agreeableness between PHQ-Binge and BES.
Bland Altman analysis using a one-sample t-test indicated a difference in scores between M-A QoLQII and respective RAND 36 subscales, which were significantly different from zero (Table 2). This suggests they are not in agreement and meant they are measuring different aspects of QoL. Further Bland Altman analysis using linear regression indicated proportionate bias between M-A QoLQII and RAND 36 subscales, and highlighted the lack of agreement between them (Table 2). M-A QoLQII and most RAND 36 subscales had significant positive correlations, except for social, physical and role functioning limitation due to emotional health (Table 3). Hence, our hypothesis that there is agreement between M-A QoLQII and RAND 36 is not supported even though they are significantly correlated. Therefore, even though M-A QoLQII and RAND 36 are associated positively, they are not measuring the same construct but are in fact measuring different aspects of QoL.
Bland Altman analysis for RAND 36 and M-A QoLQII.
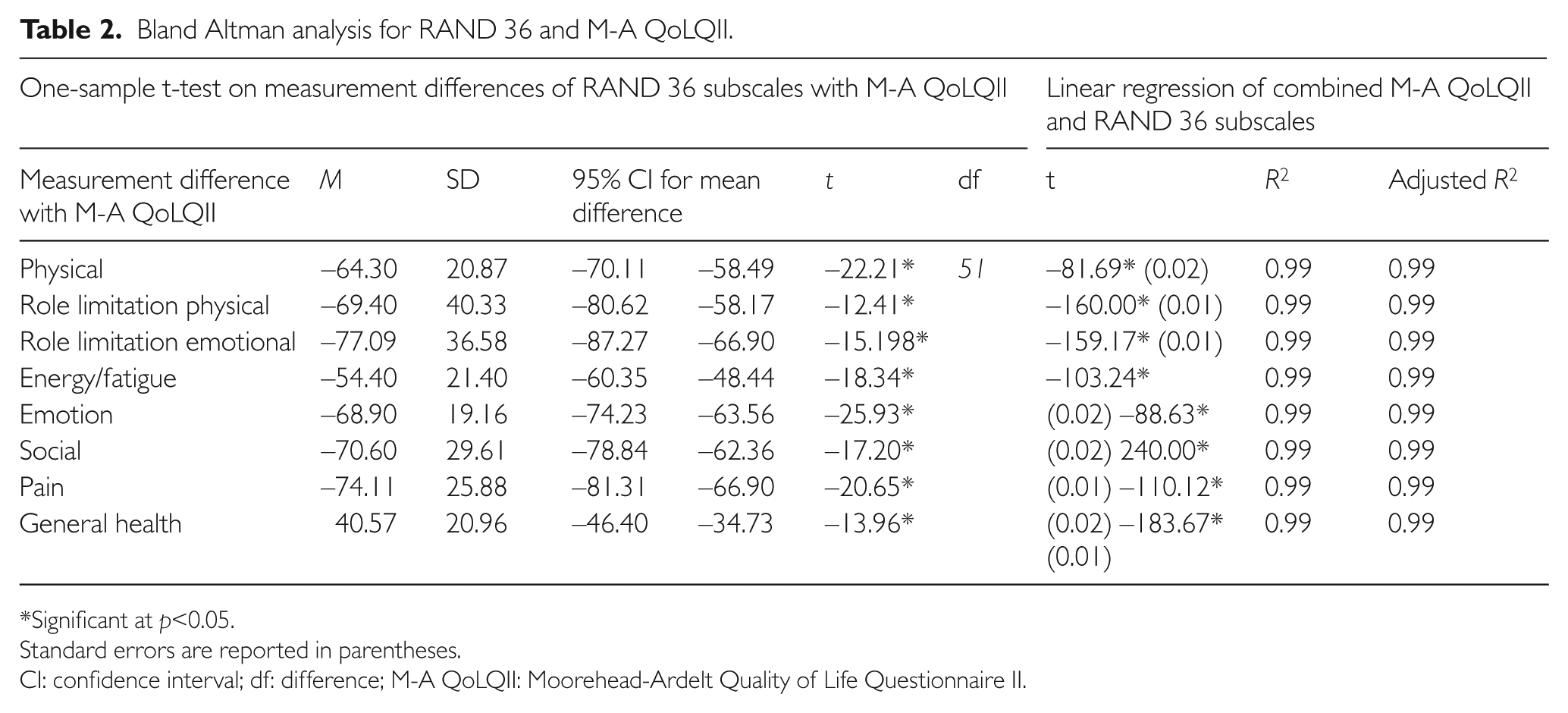
Significant at p<0.05.
Standard errors are reported in parentheses.
CI: confidence interval; df: difference; M-A QoLQII: Moorehead-Ardelt Quality of Life Questionnaire II.
M-A QoLQII and RAND 36 subscale correlations.

Significant at p<0.05.
Significant at p<0.01.
M-A QoLQII: Moorehead-Ardelt Quality of Life Questionnaire II.
From the multiple regression performed, BDI-II was predictive of RAND 36 subscales of: role limitation due to physical health, role limitation due to emotional health, emotion, social, pain and general health at baseline (Table 4). PHQ-Binge and BES were predictive of the social subscale of RAND 36 (Table 4) and %TWL 6 months after surgery (Table 5). PHQ-2 was not predictive of any of the RAND 36 subscales or M-A QoLQII. Neither of the screeners (PHQ-2, PHQ-Binge) or standard tools (BDI-II, BES) were predictive of M-A QoLQII. Our study found mixed results on the predictability of QoL and weight changes based on the psychosocial measures. This suggests our second hypothesis that PHQ-2, PHQ-Binge, BDI-II and BES are significantly related to M-A QoLQII, RAND 36 and weight changes 6 months after surgery is only partially supported.
RAND 36 subscale regression analysis.

*Significant at p<0.05.
BDI-II: Beck Depression Inventory II; BES: Binge Eating Scale; BMI: body mass index; %EBMIL: % excess BMI lost at 6 months; PHQ-2: Patient Health Questionnaire 2; RAND 36: RAND 36-Item Health Survey; %TWL: % total weight loss.
Baseline and %TWL regression analysis.
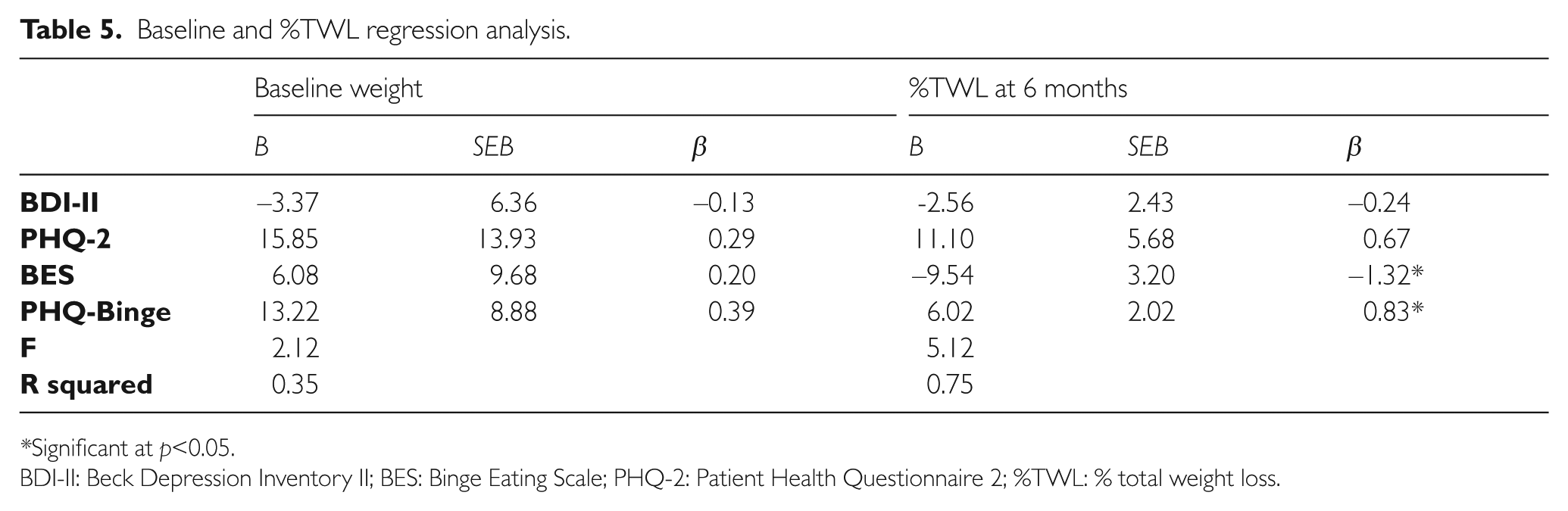
*Significant at p<0.05.
BDI-II: Beck Depression Inventory II; BES: Binge Eating Scale; PHQ-2: Patient Health Questionnaire 2; %TWL: % total weight loss.
Discussion
Our study aimed to contribute to optimal strategy for evaluating patients’ mental health prior to bariatric surgery through investigating the agreement of brief screeners with established questionnaires. Our results provide support for our hypotheses that brief screeners for depression (PHQ-2) and binge eating (PHQ-Binge) agreed with respective established questionnaires (BDI-II and BES) in differentiating between clinical vs. non-clinical symptoms. Our results did not support that screeners for QoL (M-A QoLQII) agree with established questionnaires (RAND 36). There was also only partial support for our hypothesis that psychiatric screeners and established tools predicted weight loss and QoL.
Our study suggests that PHQ-2 could be a valid and reliable brief screening instrument of depression in bariatric surgery patients. Previous studies have only looked at the operating characteristics of PHQ-9 and correlations of the PHQ-9 to standard measures such as the Mini-International Neuropsychiatric Interview (MINI) and BDI-II.12,35 Results from our study extend previous research by exploring the use of PHQ-2, an even shorter screening tool of depression developed from PHQ-9, for bariatric surgery patients. 29 The results of the current study also contribute to a previous study that uses PHQ-2 on the bariatric population but did not examine its agreement with an established questionnaire. 47
PHQ-Binge has not been validated in the bariatric surgery population, even though it has been used in previous studies. 29 Our work extends previous studies, providing support that PHQ-Binge could be a valid screening of binge-eating symptoms in bariatric surgery patients as there is agreement between PHQ-Binge and BES.29,48
One recent study explored the use of the VA Binge Eating Screener (VA-BES), a single-item screener, compared to the Questionnaire of Eating and Weight Patterns – Revised (QEWP-R) and demonstrated the utility and validity of VA-BES to screen for binge eating. 47 Our study adds to these studies examining the use of brief measures to screen for binge eating. It remains to be further investigated if VA-BES can agree with PHQ-Binge and BES. QEWP-R assesses behavioral components of problematic eating patterns other than binge eating. 49 Agreement between PHQ-Binge, QEWP-R and VA-BES remains to be further examined to clarify if PHQ-Binge would be valid in screening problematic eating patterns in addition to binge-eating symptoms.
Both QoL measures M-A QoLQII and RAND 36 were significantly correlated on most measures, but had nil agreement. This meant that although they measure QoL, they measure different, associated aspects of QoL. This is similar to a previous study’s finding that M-A QoLQII and RAND 36 were fundamentally measuring different aspects of QoL. 47 As such, our study also confirms previous studies’ recommendations that RAND 36 should be used for measuring generic QoL whereas M-A QoLQII should be used to measure bariatric-specific QoL measures. 45 Previous research on QoL after bariatric surgery is mixed. 33 Some studies found that the impact of physical and mental QoL is significantly different after bariatric surgery when using RAND 36, whereas others did not.12, 29 In light of the need to further investigate the impact of bariatric surgery on QoL, we propose that clinicians and researchers select the QoL measure according to which aspect of QoL they aim to assess: generic or disease specific. Based on the results of our study, M-A QoLQII would not be as useful as RAND 36 to assess for generic QoL; however, it would be useful to measure bariatric-specific QoL.
Our study provides some clarification on the current mixed results regarding pre-surgery binge-eating behaviours predicting post-surgery outcomes, by providing support that pre-surgery binge eating predicts weight outcomes.16,17,20 PHQ-Binge and BES of the current study were found to be predictive of %TWL 6 months after surgery, but not with %BMIL after the same time. Similar to previous research, the current study did not find any other baseline variable that could predict weight loss. 49 Contrary to results of other studies, our findings did not indicate that pre-surgery depression was predictive of weight outcomes or QoL.4,50,51 Overall, our findings support previous reports that highlighted the need to identify and provide relevant treatment for binge eating in the bariatric population.16–20
Limitations of this study include its small sample size, which limits generalizability to the bariatric surgery patient population. The majority of participants were female, who have been found to have a stronger association between obesity and depression. 52 Female bariatric patients may be particularly at risk of developing depression. As such, our sample may have skewed our results towards an association with depression. Previous research indicated that medical comorbidities were related to psychopathology but the nature of it remains mixed and needs further investigation.18,53 Due to the small sample size we were unable to ascertain if the number of medical comorbidities affected psychopathology or vice versa and for any influence on the agreement between screening questions and established questionnaires. 53 The predictor variables were only collected at baseline. Hence, we were unable to understand the longitudinal trends of the predictor variables over time. For instance, we did not measure how the mood and eating behaviours of patients changed over time after surgery. We were also unable to track the impact of post-surgery binge eating and depression on outcomes. The outcome variable of QoL was only collected 6 months after surgery so we were unable to track longer-term changes. Future research should include a longer follow up and look at the longitudinal trends of weight change after bariatric surgery, as well as mood, eating behaviours and QoL. Examining the screeners’ agreement with clinical interviews can also help to further examine the reliability of screeners. We will continue to follow up with participants from the current study up to two years after surgery and hope to report on the analysis of longitudinal trends observed.
In summary, our results provide support that PHQ-2 and PHQ-Binge screeners can be valid and reliable tools to screen for symptoms of depression and binge eating in the bariatric surgery population. The impact of psychiatric conditions of binge eating and depression on weight outcomes and QoL is still mixed and calls for a more cautious approach via examining psychiatric conditions and providing relevant psychological treatment. We propose that screening instruments should not replace established questionnaires or be used as the sole method of assessment. Instead, screeners can be used together with established questionnaires at different points of the assessment process. This can provide a more comprehensive and optimal strategy that prevents participant fatigue in filling out questionnaires and helps identify patients that may need psychological intervention.
Footnotes
Declaration of conflicting interests
The authors report no proprietary or commercial interest in any product mentioned or concept discussed in this article. The authors have no conflicting interests to report.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the Singapore Health Services’ SingHealth Institutional Review Board and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards, the Code of Ethics of the World Medical Association (Declaration of Helsinki) for experiments involving humans, and the Uniform Requirements for Manuscripts Submitted to Biomedical Journals. We have also complied with APA ethical standards in the treatment of their sample, human or animal, or to describe the details of treatment.
Informed consent
Informed consent was obtained from all individual participants included in the study.
