Abstract
The aim of this study was to compare the body temperature measurements at tympanic, forehead and temporal sites using infrared thermometers. A total of 1576 consecutive visitors to Singapore General Hospital at two entry locations were included in this study. Pearson correlation and Bland–Altman mean difference between sites (95% confidence interval for limits of agreement) were calculated for the relationship between the three different sites of temperatures recorded (i.e. temporal, forehead and tympanic). Of all the visitors, 27 (1.7%) had fever. Moderate positive correlation was found between temporal and forehead temperature readings (r=0.602, mean difference (temporal – forehead), (95% limits of agreement) = 0.1 (−0.8, 0.7)), and there was very weak positive correlation between tympanic and temporal temperature readings (r=0.177, mean difference (temporal – tympanic), (95% limits of agreement) = −0.3 (−1.7, 1.1)). Sensitivity for temporal temperature readings (⩾37.5°C) to detect febrile visitors was 3.7%, specificity was 99.6%, positive predictive value was 14.3% and negative predictive value was 98.3%. Our results demonstrate that tympanic temperature readings should be used for fever screening instead of temporal or forehead readings.
In December 2019, a novel strain of coronavirus was discovered in the city of Wuhan, China, and it was later named Covid-19.1,2 Covid-19 has now resulted in a global pandemic. 3 One of the symptoms of patients with Covid-19 is that of fever, and this affects up to 89% of patients. 4 As part of the efforts to control the rapid spread of infectious diseases through the early identification of febrile patients, international bodies such as the World Health Organization and local health authorities (e.g. Ministry of Health) have recommended temperature screening at point of entry.5,6 Infrared thermometry allows for a quick, non-invasive and non-contact method of detecting fever.7,8 However, there have been previous studies that highlighted that infrared thermometry might not reliably detect patients with fever due to low sensitivity, 9 with skin surface temperature varying according to changes in skin perfusion. 10 Tympanic temperature readings have been found to be more accurate than skin temperature readings. 11
To determine if there were any differences between the temperature readings at different sites, we analysed the temperature readings of 1576 consecutive visitors to Singapore General Hospital at two indoor entry locations over 2 days (9 and 10 March 2020). For each visitor, three temperatures readings were each taken from the tympanic region, forehead and temporal region, respectively. Visitors were considered to be febrile if any of the temperature readings were 37.5°C or greater. The Microlife NC150 thermometer was used for temperature readings for the forehead and temporal region while the Coviden Genius 2 or 3 was used for the measurement of tympanic temperatures. For temporal temperature readings, the thermometer was aimed at the temple area (about 1 cm above the eyebrow) at a distance of between 3 and 5 cm. Forehead temperature readings were obtained from the centre of the forehead at a distance of no more than 5 cm. All three thermometers utilised infrared technology to measure temperature. Pearson correlation and mean difference between sites (95% limits of agreement; LoA) were calculated for the relationship between the three different sites of temperatures recorded. LoA was defined as mean difference ± 1.96 SDd, where SDd is standard deviation of the differences. Of all the visitors, 27 (1.7%) had fever. Moderate positive correlation was found between temporal and forehead temperature readings (r=0.602, mean difference (temporal – forehead), (95% LoA) = 0.1 (–0.8, 0.7)). There was very weak positive correlation between tympanic and temporal temperature readings (r=0.177, mean difference (temporal – tympanic), (95% LoA = −0.3 (−1.7, 1.1)). From LoA, we concluded that temporal reading can underestimate tympanic temperature by as much as 1.7°C and overestimate by as much as 1.1°C. This large maximum magnitude of 1.7°C for the underestimation far exceeds our acceptable absolute difference of 1.0°C. In patients with temporal temperature readings of less than 37.5°C, 1.7% (n=26) were later found to be febrile by tympanic temperature readings, of which the mean (range) tympanic temperatures were 37.7°C (37.5°C to 38.7°C). The sensitivity for temporal temperature readings (⩾37.5°C) to detect febrile visitors was 3.7%, specificity was 99.6%, positive predictive value was 14.3% and negative predictive value was 98.3%; 63.7% of temporal temperature readings were lower than those of tympanic temperature readings (Figure 1).
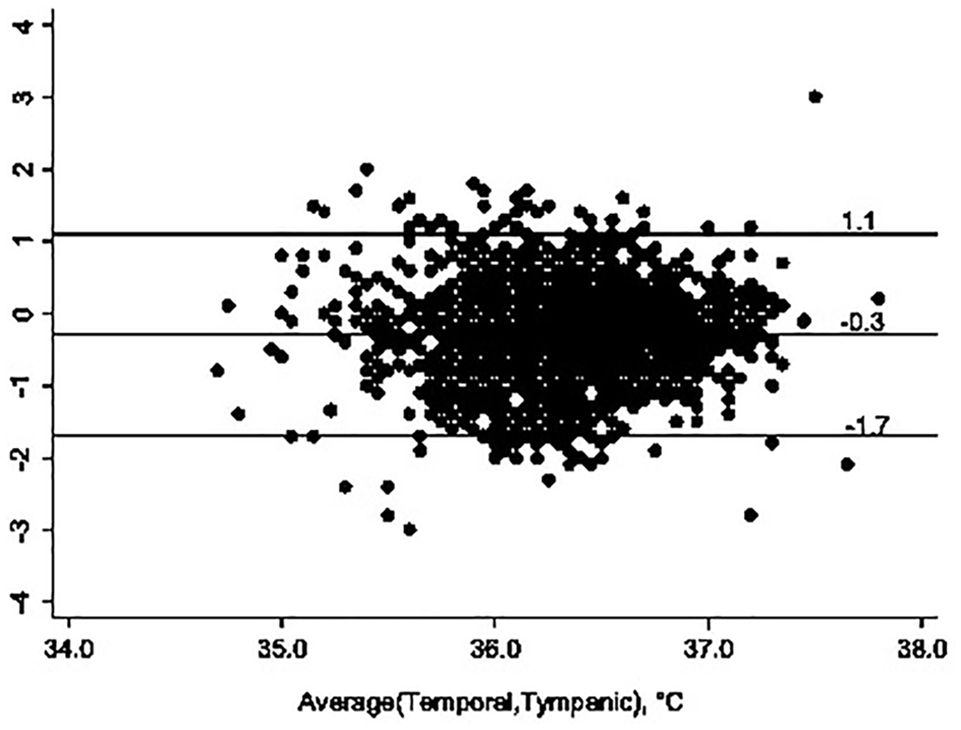
Bland and Altman plot of temporal and tympanic temperature readings showing the mean difference and 95% limits of agreement.
Our results demonstrate that temporal or forehead temperature readings are generally lower than those of tympanic temperature readings, and hence may not detect patients with fever. This is consistent with a previous study by Bijur et al., who found that tympanic temperatures were more precise than temporal thermometry, with a sensitivity of 68.3% to detect a rectal temperature equivalent of 38°C. 12 Furthermore, sweat and hair over the area to be measured have also resulted in lower temporal temperature readings.13,14 Also, according to the manufacturer’s manual for Microlife, patients and thermometer have to be in a similar ambient room condition for 30 minutes before taking the temperature. 15 This is not practically possible at a temperature screening point and hence could also result in inaccuracies in temporal or forehead temperature readings. One of the limitations of this study was there was no collection of demographic data, thus subgroup analyses by age, gender and race could not be performed.
In conclusion, tympanic temperatures should be used instead of temporal or forehead temperatures when screening visitors for fever.
Footnotes
Acknowledgements
The authors would like to acknowledge Ms Emily Tan for the collection of data for this study, Mr James Toi and Professor Julian Thumboo for their guidance in the manuscript.
Authors’ contributions
ES, SF and SKY conceived the study. WF and SF were involved in data analysis. WF and JKP wrote the first draft of the manuscript. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
Availability of data and materials
The datasets generated and/or analysed during the current study are available from the corresponding author.
Ethical approval
Our institution does not require ethical approval for reporting quality improvement projects.
Informed consent
Our institution does not require informed consent for reporting quality improvement projects.
Trial registration (where applicable)
Not applicable.
Conflict of interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
