Abstract
Background:
A sound understanding of pelvic anatomy is essential for training in obstetrics and gynaecology (OBGYN) and for practising in the field post-qualification. There is a growing concern that surgery residents have an inadequate knowledge of anatomy and little confidence in their approach to the subject.
Objective:
This study aims to explain the use of an anatomy workshop to deliver a unique and self-designed innovative instruction method that employs cutting-edge resources to enhance OBGYN residents’ comprehension of clinical anatomy and to discuss why this approach works.
Methodology:
The workshop emphasised the clinical and surgical anatomy of the female pelvis using 3-D virtual dissections, relevant plastinated specimens and also bony pelvic models that had been developed in house. Anatomists and OBGYN consultants facilitated the workshop. The students’ knowledge of anatomy and their perceptions of the subject were evaluated by pre- and post-tests and a five-point Likert scale, respectively. A mixed methods analysis was applied.
Results:
Of the 42 participants, 26 (61.9%) completed both the pre- and post-test. The overall difference (mean percentage) between the pre- and post-test performance was 25.41%. There was a significant difference in the residents’ knowledge of anatomy between the pre- and post-workshop (
Conclusion:
The active learning workshop enabled by multidisciplinary teaching and the innovative tools employed resulted in improved outcomes in knowledge of anatomy, confidence and learning satisfaction. Reintroduction of anatomy concepts during OBGYN residency training is needed to improve surgical training and patient care.
Keywords
Introduction
The execution of clinical or surgical procedures demands the recall and application of anatomy. 1 For example, a working knowledge of the pelvic anatomy including the different types of pelvis, organisation of pelvic viscera and their relationships to neurovascular structures is essential for obstetrics and gynaecology (OBGYN) residents and practising specialists. 2 Similarly, anatomy has a significant role in clinical specialities such as radiology 3 and certain surgical specialities. 4 There is a rising concern about the decline of knowledge of and competence in human anatomy among undergraduate medical students, junior doctors and residents.5-8 This may be attributed to multiple factors, for example, changes to the anatomy curriculum, a reduction in the teaching time allocated to the subject and constraints in relation to teaching tools and faculty. 9
It was found that a large percentage of the medical students self-reported that their retention and transfer of knowledge about anatomy was a challenge throughout the clinical years. 5 Another study showed a significant decline in retention of knowledge about the pelvic anatomy among Year 3 medical students prior to commencing the general surgical and OBGYN rotations. 10 Similar results were found in a study that involved junior OBGYN residents. 11 A recent study reported the perceptions of 109 residents from different clinical and surgical specialities with regard to the need for a knowledge of clinically relevant anatomy during the residency programme. The outcomes from the data indicated that OBGYN residents preferred to learn female pelvic anatomy during their residency training. 12 Cameron et al. explored the perceptions of junior doctors who were undertaking the graduate diploma in surgical anatomy. They felt that the main motivation for taking this course was the perceived benefit to their profession and an opportunity to enter and succeed in an area of specialist training. 13 Overall, the literature provides evidence of inadequate competence in anatomy among junior doctors and indicates there is a need to revisit this subject during the surgery residency training programme.
An inadequate knowledge of anatomy among medical practitioners may result in complications such as damage to underlying structures during surgery and, in turn, this could lead to medico-legal litigations. 14 It could also have a detrimental effect on their ability to practice clinical medicine and on the quality of medical care they provide.
The amount of anatomy instruction received during the preclinical years is also an important contributing factor. Research reports have shown that a high proportion of newly qualified doctors and residents express concern that the anatomy instruction received during their preclinical years was inadequate.11,15 Residents from different surgical specialities felt that a robust anatomy curriculum, which would help them prepare better for the residency training, was needed in medical school. 16 In addition, in recent years, there have been changes to the residency training programmes with the introduction of duty hours and alterations to the duration of training. This has limited surgical exposure to real-time anatomy because of the reduced time spent in the operating theatre.
Numerous recommendations have been made to alleviate this situation, including the vertical integration of basic sciences throughout the medical curriculum 17 and developing advanced courses using web- or cadaveric-based simulations.18-20 An electronic- and laboratory-based anatomy curriculum was introduced for Year 3 undergraduate medical students who were attending the core OBGYN clerkship. These approaches resulted in a significant improvement of students’ knowledge of anatomy. 19
Similarly, anatomy courses are recommended for OBGYN residents to rectify the knowledge deficiency that might be due to inadequate exposure to anatomy during their undergraduate training.11,21 Formerly, either the cadaveric dissection or wet cadaveric prosection approach was employed to reinforce knowledge of anatomy in OBGYN residents.16,21,22 However, because of a lack of access to wet cadaveric materials, as in this case, effective alternative tools and a different pedagogy are necessary to reintroduce anatomy concepts during OBGYN residency training.
We developed and delivered a unique workshop that employed cutting-edge resources and instruction from a diverse team to enhance the comprehension of clinical anatomy among OBGYN residents. Hence, this study aims to explain how the workshop was organised and to discuss why this approach works.
Materials and methods
Context
OBGYN residency training is offered by SingHealth and has adopted the US training philosophy. It is a six-year programme during which OBGYN residents are exposed to a wide range of clinical experiences and sub-speciality postings. As per the structure of the OBGYN residency programme, residents in years 1–4 (R1–R4) are considered as junior residents (JRs) and those in years 5 and 6 (R5 and R6) as senior residents (SRs). During the training, the OBGYN residents are expected to amass a range of surgical skills. Acquiring a strong foundation in surgery requires an excellent theoretical knowledge of surgical anatomy and basic surgical principles, enabling conduct of safe surgery and prevention of complications.
Knowledge of surgical anatomy is gained and consolidated while assisting and undertaking surgical procedures throughout the residency training. Competency in surgical procedures during this training is assessed by case logs and objective structured assessments of technical skills (OSATs).
The purpose of the anatomy workshop was to equip OBGYN residents with a comprehensive knowledge of the female pelvic anatomy and its relevant clinical/surgical application in OBGYN practice. The objectives of the workshop were that OBGYN residents should be able to:
recall and reinforce an advanced knowledge of the female pelvic anatomy, including relevant bones, types of female pelvis, muscles, female genital tract, urinary and lower gastrointestinal tracts, blood vessels, nerves and important relationships and variations thereof;
apply concepts of anatomy and key anatomical relationships during clinical examination and OBGYN surgical procedures;
identify the female pelvic organs, relationships and key neurovascular structures in plastinated prosections and virtual dissection.
The following three work stations were planned to cover the learning objectives.
Station 1: Anterior abdominal wall, pelvic floor, perineum and relevant clinical anatomy;
Station 2: Female pelvic viscera, neurovascular structures and relevant clinical anatomy;
Station 3: Applied anatomy of the female pelvis and fetal skull in relation to the mechanism of labour in different fetal presentations.
Study participants
The workshop was conducted as a part of the national training programme for residents in years 1–6 who were registered for the SingHealth OBGYN residency training programme in Singapore. Information detailing the workshop aims and methods was disseminated to all residents well in advance. All residents were required to attend the workshop. Of the eligible residents, 42 participated in the workshop, which was held at the Anatomy Learning Centre at the Lee Kong Chian School of Medicine in Singapore. The rest (
Organisation of the workshop
Figure 1 provides an overview of the workshop. A pre-test was conducted before the commencement of the learning activity to evaluate residents’ baseline knowledge of pelvic anatomy and its application to various clinical scenarios. The test comprised 25 questions in the single best answer format and encompassed the topics covered in the three stations. The questions were written by both anatomists and clinicians to balance the inclusion of both anatomical and clinical applications. The number of questions for stations 1, 2 and 3 were 8, 9 and 8, respectively. After the pre-test, the participants were divided randomly into three groups to take turns at the three stations. All the stations were equipped with relevant resources such as plastinated cadaveric specimens, plastic models and paper-based models of the different types of female pelvises, as well as a centralised Anatomage Table (Anatomage Inc., San Jose, CA). Each station was designed for interactive teaching, which was facilitated by an anatomist and an OBGYN specialist. Each group spent one hour at each station and then rotated between the stations. At the end of the workshop, the participants completed the post-test, which consisted of the same 25 questions as the pre-test. The participants’ feedback was captured by means of a five-point Likert scale (5=strongly agree to 1=strongly disagree) questionnaire to investigate the effectiveness of the workshop.

Workshop activities.
A mixed methods analysis was employed to analyse the educational value of the workshop. The responses for the pre- and post-test were tabulated in MS Excel for each station as well as for each student. The mean and standard error mean (SEM) for both the pre- and post-test were calculated. Residents who completed both the pre- and the post-test were considered for the analysis. A Student’s two-tailed
Results
There were 42 participants, of whom 36 were female (85.71%) and 6 were male (14.29%). The age range was 24–44 years at the time of the study.
Performance of participants in pre- and post-tests
All the registered participants (
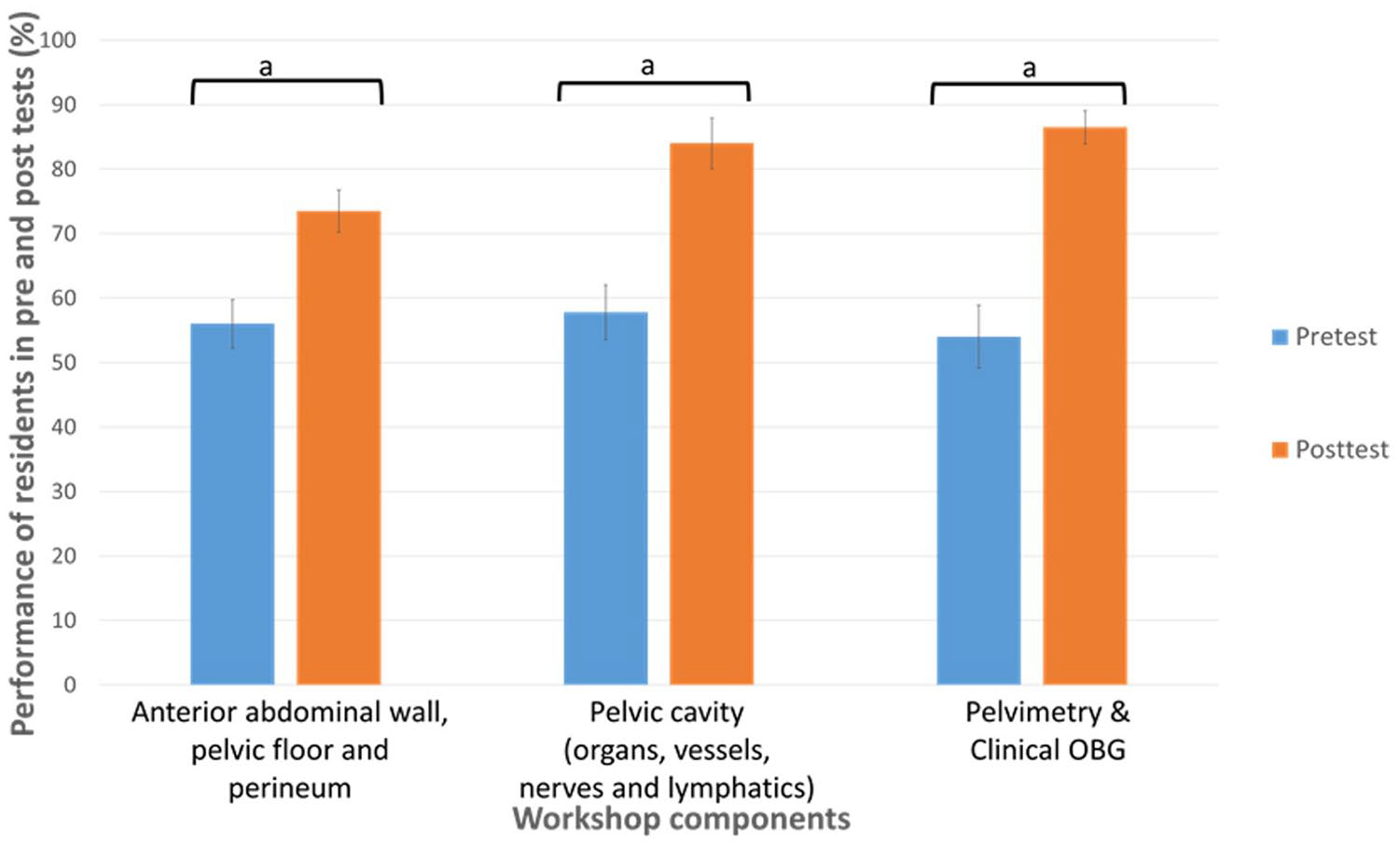
Showing the significant difference between the pre- and post-test mean scores in the three stations of the pelvic anatomy workshop.
There was no significant difference between the JRs and the SRs when their mean percentage scores from the pre-test were compared (JRs=mean+SEM 55.75±3.25; SRs=55.6±5.91;
Cohen’s
Feedback survey
Ten participants (23.8%) completed the survey questionnaire. Overall, all the participants enjoyed the workshop and felt it was very useful for enhancing their knowledge and understanding of anatomy. The participants’ responses are summarised in Table 1. The majority of the participants either agreed or strongly agreed that the content and teaching resources were meaningful and useful for their learning. In terms of learning gain, the majority of students felt they had acquired new knowledge (90%) and the confidence to apply this in the workplace (100%). One of the participants commented that ‘this was hands down the best NTP [national training programme] session I’ve attended. It was engaging and really fun!’
Residents’ perceptions of the workshop.
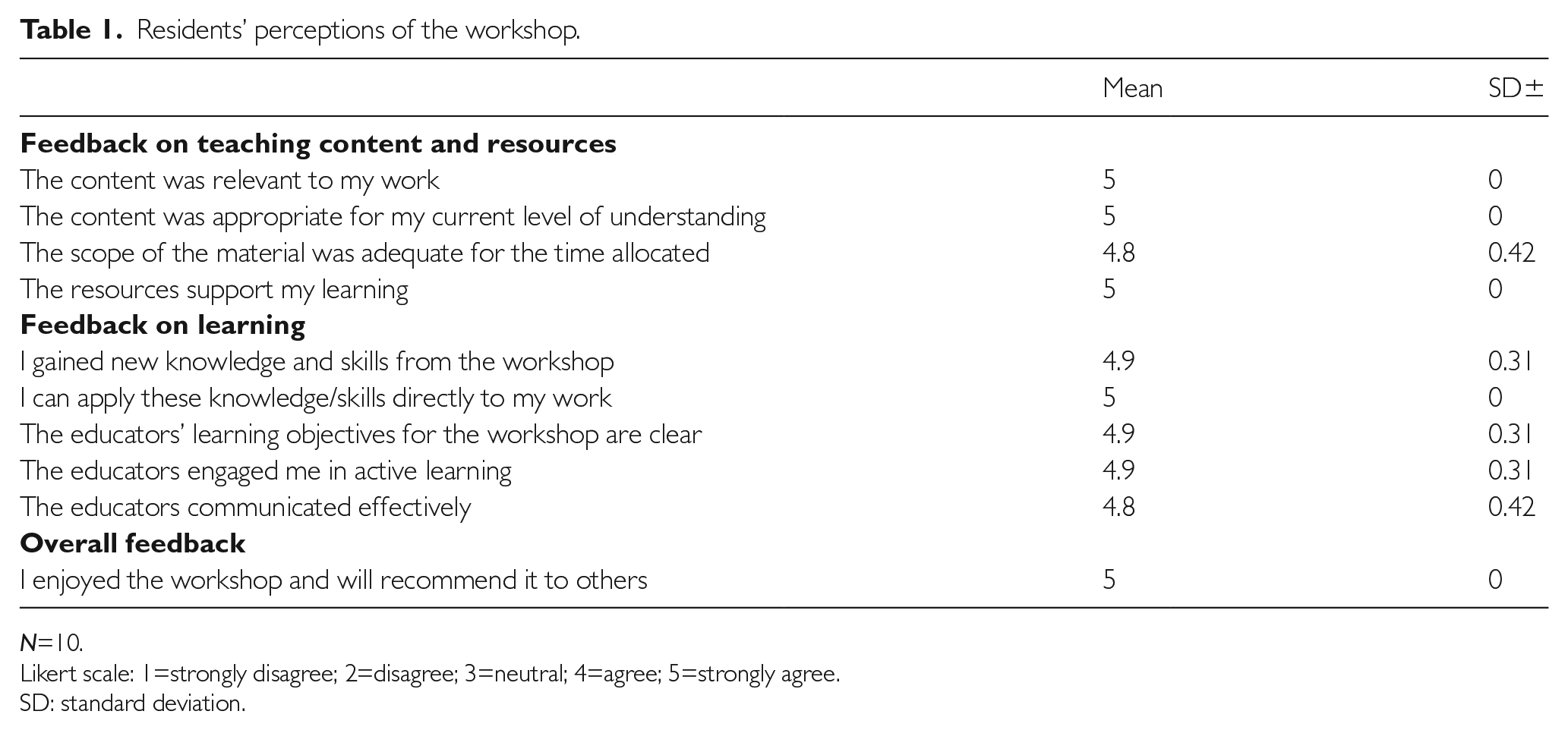
Likert scale: 1=strongly disagree; 2=disagree; 3=neutral; 4=agree; 5=strongly agree.
SD: standard deviation.
Most participants agreed that the educators engaged effectively (90%) and communicated well (80%) with them. The majority of the participants recommended the workshop should be held at least once a year (70%), and particularly during the first year of the residency programme (90%).
Discussion
This study reports that an anatomy workshop employing modern resources and instruction from a diverse team is an effective learning strategy for enhancing OBGYN residents’ understanding of pelvic anatomy and its clinical application. A formal education in anatomy is less common in residency programmes. It is mostly achieved by self-study, or through instruction delivered by senior trainees or surgeons, the latter being limited by time constraints. 23 It would be desirable to have structured courses, as in the present study, to rectify the gap in residents’ knowledge of anatomy and to further develop their surgical skills. 16 , 24
The main objective of the study was to evaluate the use of an anatomy workshop for improving OBGYN residents’ knowledge of pelvic anatomy. The observations in this study demonstrate that the pre-test scores were significantly lower than the post-test scores. The lower baseline scores may indicate that residents had an inadequate knowledge of pelvic anatomy. This could be attributed to a number of factors: the time gap between undergraduate studies and residency programmes; superficial learning with regard to or a lack of emphasis on anatomy in the modern undergraduate medical curriculum; and the lack of formal anatomy teaching in the residency programme.9,15 After the workshop, there was a significant improvement in residents’ performance in the anatomy test, affirming a positive outcome in relation to enhancing their knowledge of anatomy. These results concur with those from previous studies, in which residents were exposed to cadaveric dissection, took part in a surgical skills training programme or were involved in clay modelling of the pelvic structures.25,26 Although there was no significant difference between the JRs and SRs in overall performance, the JRs did perform better than the SRs. This is consistent with the study by Carton et al., 22 but differs from the study by Mizrahi et al. 11 The performance difference between the JRs and SRs in this study could be attributed to the lower number of SRs rather than their knowledge.
In recent years, anatomy learning tools have taken on a completely new form. The literature highlights the use of interactive learning tools to improve students’ learning because they present complex information in multiple formats. 27 In addition, various cost-effective anatomy models have been designed and are being used for learning. 28 The most meaningful way of providing a three-dimensional understanding of pelvic anatomy (the foundation of various gynaecological procedures) to the residents, is the multimodal approach. 29 In the present study, residents were exposed to innovative teaching tools such as plastinated human prosections, a virtual dissector (the Anatomage Table, see Figure 3), plastic models, handmade paper-based models of the different types of female pelvis (see Figure 4) and low-fidelity vaginal delivery simulators. Residents were experiencing most of these new tools for the first time and were impressed with the quality of clinically relevant dissections that could be carried out on plastinated specimens and a 3-D virtual human body. We presented several clinical scenarios, for example, episiotomy, pudendal nerve block and ureter and inferior epigastric artery injury during hysterectomy and laparoscopy, by employing structured virtual dissection and cross-sections using the Anatomage Table. This means tissues were removed virtually layer by layer from particular anatomical regions and the anatomical structures were correlated with relevant surgical procedures. Participants were also asked to identify the surgically relevant structures and their relationship to one another in the plastinated specimens to reinforce their comprehension of 3-D anatomy. CT data from selected cases were also uploaded to the Anatomage Table. This has a built-in algorithm that converts digital imaging and communication in medicine (DICOM) into 3-D models. This enabled residents to gain a better understanding of patient-specific anatomy and pathology, and their implications during surgery. We believe that high-fidelity 3-D anatomical models and prosected plastinated specimens help residents better appreciate the complex anatomy and spatial understanding of 3-D relationships. This was confirmed by the participants’ qualitative feedback on the learning tools.
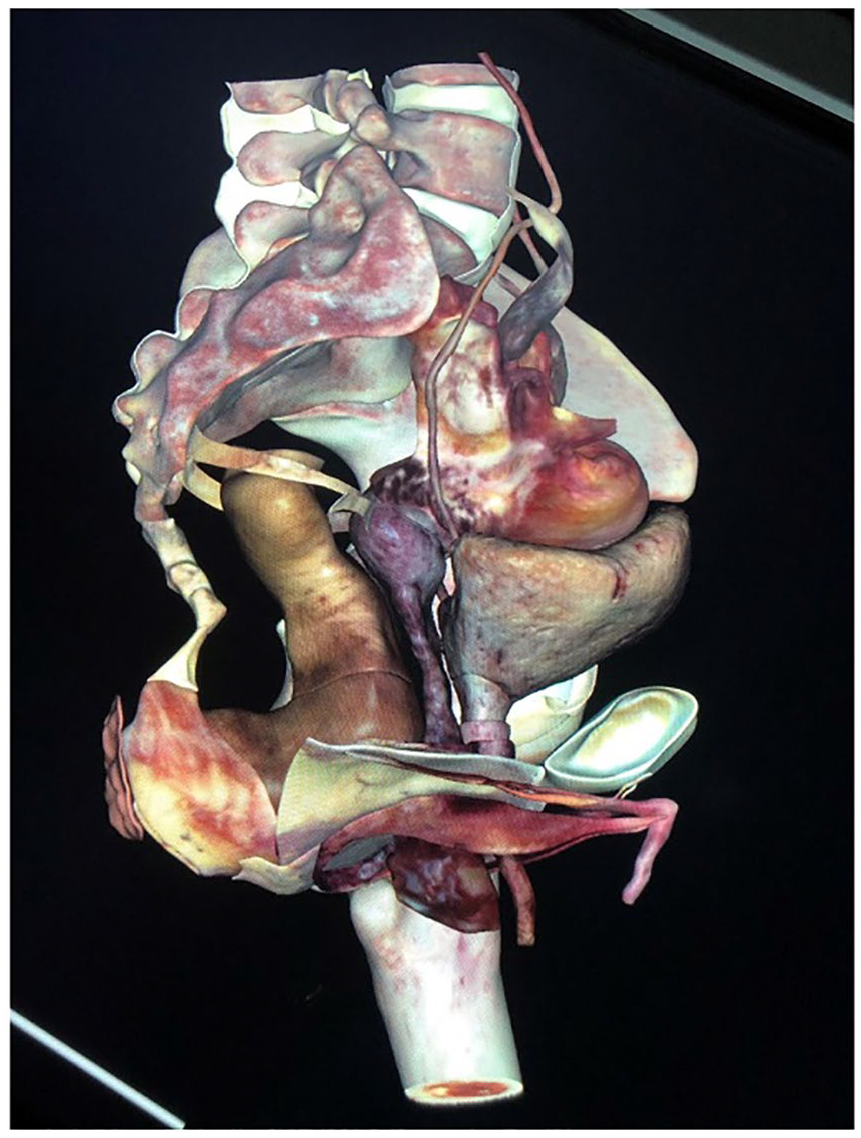
Virtual dissection of female pelvis using the Anatomage Table.

Paper models of the different types of pelvis. A: Gynecoid type; B: Anthropoid type; C: Android type; D: Platyploid type.
In addition, the teaching team comprising both anatomists and practising surgeons is a good combination for conducting anatomy sessions because the residents get the best of both worlds. A multidisciplinary faculty teaching approach is beneficial for students’ learning, blending principles of both basic and surgical sciences to develop a strong foundation in surgical skills, and enabling the safe conduct of surgery. 30 Reintroducing gross anatomy concepts using innovative teaching tools and methods during residency as in the present study can narrow the knowledge gap and improve surgical training. 31
Limitations
There are some limitations of this study. First, the participants’ knowledge of anatomy was tested immediately after the workshop; at this point, the performance scores were higher, as would be expected. The long-term recall and retention of anatomical concepts needs to be explored. Second, the study was monocentric (the residents were from the SingHealth OBGYN residency programme only). The OBGYN residents from the National Health Group programme did not participate in the workshop. A workshop involving residents from both the OBGYN training programmes in Singapore may have provided more insights into the effectiveness of the workshop. Third, 61.9% of participants completed both the pre- and post-test questionnaire, whereas only 23.8% (
Conclusion
There is a need to incorporate formal anatomy courses into surgical-based residency training programmes to address knowledge gaps that residents from different medical specialities may have. The active learning environment, multidisciplinary teaching and innovative contemporary tools were shown to have a positive impact on participants’ learning, and this translated into improved learning outcomes. Further studies are needed to explore the longitudinal impact of the workshop in terms of residents’ knowledge, clinical judgement and competence in the clinical environment. Revisiting anatomy during residency is valuable not only for improving surgical training but for enriching the existing residency training programme curriculum.
Footnotes
Acknowledgements
The authors would like to thank Mr Darren Lim Men Shun, the senior laboratory manager at LKCMedicine in Singapore, and Dr Lim Yu Hui and Dr Ng Yifan (registrars and MOs) and Ms Kam Limin and Ms Charlene Ong Liam Yen (administrators) from the KKH Women and Children’s Hospital in Singapore for their support for the study.
Authors’ contributions
SRM and MM initiated the plan to organise the workshop for OBGYN residents. SRM and RV were the anatomy content experts from LKC Medicine, and MM, RK, IA and JK were the clinical OBGYN content experts who facilitated the workshop. SRM and RV researched the literature, conceptualised the study, obtained the ethical approval and performed the data analysis. SRM and RV wrote the manuscript and MM, RK, IA and JK provided an intellectual contribution and reviewed it critically. All authors reviewed and approved the final version of the manuscript.
Availability of data and materials
The datasets generated during the current study have been obtained from the online responses of the participants to the pre-test, post-test and survey questionnaire.
Ethical approval
Ethical approval to report this case was obtained from the Institute Review Board at Nanyang Technological University (IRB-2019-09-011).
Informed consent
The consent form was waived because the study was considered to be part of the evaluation of an educational course.
Declaration of conflicting interests
The authors have no conflicts of interest to declare.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
