Abstract
Background:
Hepatitis B virus (HBV) infection is a major global health concern. The prevalence among health-care workers (HCWs) is about 13% in Nigeria. Although the vaccine has been found to be effective in preventing infection in 90–95% of recipients, its uptake among HCW is low. The objective of this study was to determine the prevalence and vaccination status of HCW in a tertiary health facility in Southeast Nigeria.
Methods:
The study was conducted at Enugu State University Teaching Hospital (ESUTH) to mark the 2018 World Hepatitis Day. The HCWs were sensitised through handbills, posters, memo to the different departments and an awareness walk. HCWs who presented voluntarily were screened. Data were collected using a pro forma and analysed.
Results:
Out of the 1720 staff at ESUTH, 241 (14.0%) were screened; 33.2% were classified as clinical staff, 43.9% worked in clinical departments and 25.3% and 6.6% had been previously screened and vaccinated, respectively. Only 2.1% were positive for hepatitis B surface antigen. Previous screening for hepatitis B, working in clinical departments and being a core clinical health worker were factors that were significantly associated with previous vaccination status. Positive predictors included previous screening and working in clinical departments.
Conclusion/Recommendation:
This study revealed low HBV screening and vaccination uptake among HCWs in Enugu state University Teaching hospital, and also low disease prevalence. Though the prevalence of HBV infection was low, organising more awareness-raising activities in the facility will improve prevention and further reduce prevalence.
Introduction
Hepatitis B virus (HBV) infection, previously known as serum hepatitis, is a systemic infection that essentially attacks the liver. The parenteral route is the usual route of transmission, though it is also transmitted through sexual intercourse. 1 This infection can lead to acute illness or a chronic disease state such as hepatocellular carcinoma or cirrhosis of the liver. Health-care workers (HCWs) are significantly at risk of acquiring HBV infection, since they are usually exposed to infected patients. 2 The disease poses a worrisome health challenge globally, especially in the World Health Organization (WHO) Western Pacific and African regions where 6.2%, and 6.1%, respectively, of the adult population are infected. 2 The World Health Assembly resolution 63.18 of 2010 recognised viral hepatitis generally as a global health problem. 3 About two billion people are infected with HBV globally. 4 In 2009, about 10–15% of the Nigerian population was reported to be infected with HBV, 5 and the disease was documented to be the highest cause of chronic liver disease in Nigeria. 6 The incubation period of this virus ranges between six weeks and six months. Hence, it was also known as long-incubation period hepatitis. 7
Approximately two million HCWs globally each year are at risk of becoming infected with HBV through their routine duties in their workplaces, and very few HCWs are vaccinated. 8 It is estimated that about 5.9% of HCWs globally are exposed to HBV infection every year, 9 and this virus is very infectious, being 50–100 times more infectious than the dreaded human immunodeficiency virus. 10 It has been documented that older HCWs, those in exposure-prone professions such as laboratory scientists and those who have been employed for a long time have higher rates of HBV infection.11–14 In recognition of the immense occupational hazard posed by HBV infection to HCWs, at the World Hepatitis Summit held in Sao-Paulo, Brazil, the WHO called on governments to include vaccination of HCWs against HBV in national immunisation programmes, since it has been documented that hepatitis B vaccines could reduce the risk of infection to almost zero.15,16 In addition, there should be a policy of providing post-exposure prophylaxis to HCWs who are significantly exposed to the blood of patients infected with HBV. 17 Some countries have included immunisation of their HCWs in their immunisation programmes, while many others have not. 18 It has been shown that vaccinating HCWs and practicing standard infection control measures have contributed to the decreasing incidence of HBV infection in this group. 19
Nigeria is HBV holoendemic, with carrier rates as high as 15–37%. Hence, HCWs have a reasonable risk of becoming infected. 20 A high HBV infection prevalence rate of 25.7% among surgeons was recorded in a study in Nigeria, 21 even though a very effective and safe vaccine has been available globally since 1982 and was introduced in Nigeria in 1995.22,23 The national guidelines developed in 2016 for the prevention, care and treatment of HBV and hepatitis C virus has vaccination of HCWs as a preventive strategy, but it is doubtful if any implementation policy is in place for this. Some studies in Nigeria revealed low rates (20–50%) of hepatitis B vaccination among HCWs, with reasons for non-vaccination including a lack of opportunity, ignorance and the high cost of the vaccine.24–28
HCWs are exposed to HBV infection daily, taking a fatal course in many cases. This infection is very preventable. Hence, it is essential that the vaccination status and the prevalence of HBV infection among HCWs in all heath facilities are established. The ultimate goals are to prevent infection in uninfected HCWs and to prevent complications in infected HCWs. The objectives of this study were to assess the vaccination status of HCWs in a tertiary health facility, and also to determine the prevalence of infection among them.
Methods
Study area and period
This study was carried out in Enugu State University Teaching Hospital (ESUTH) Parklane, Enugu. ESUTH is a state-owned health institution that evolved from a nursing home in 1930 for the then colonial masters to a teaching hospital in June 2006. 29 It is located in the capital of the old Eastern region and the current Enugu state in Southeast Nigeria, with an estimated population of 722,664 people according to the 2006 national census. 30 ESUTH provides service in different departments such as community medicine, gynaecology, paediatrics, ophthalmology, psychiatry, internal medicine, surgery, pharmacy and medical laboratory, among others. Currently, there are 1720 health-care staff working in the hospital. The study was conducted between 30 July and 6 August 6 as part of the activities to mark the 2018 World Hepatitis Day.
There is an infection prevention and control committee at the hospital that developed a policy and standard operating guidelines for the screening, provision of post-exposure prophylaxis and management of highly infectious diseases, but HCWs’ awareness of this policy document and the subsequent implementation of this policy and guidelines is poor. Free screening for HBV is only available on World Hepatitis Day when pharmaceutical companies support this process. However, hepatitis B screening can be done easily but for a small fee at the hospital laboratory at other times. HBV vaccine is also readily available at the primary care unit of the hospital but is not subsidised by the hospital management. Therefore, staff have to pay the full price if they want to be vaccinated. Employee health records are available at the facility, but it is not mandatory to receive a hepatitis B vaccine as part of workplace safety in the facility.
Study design and subjects
A cross-sectional study design was employed to assess the vaccination status of HCWs against HBV infection. To mark the 2018 World Hepatitis Day, the hospital management circulated a memo to all the departments informing them about the objectives of the world hepatitis need and the urgent need to be tested and vaccinated. Two weeks prior to the event, the Department of Community Medicine in collaboration with partners developed and adapted some WHO-themed flyers and posters which were shared to all the departments during meetings and seminars. These activities culminated in a walk for life on World Hepatitis Day and a sensitisation workshop for all HCWs in the facility. Subsequently, all health-care professionals who turned up for screening during the study period were enrolled in the study. Finally, 241 HCWs were included in the study.
Data collection and management
A structured pretested interviewer-administered questionnaire was used to collect information from HCWs. Pretesting of the tool was carried out among 40 HCWs sampled from Uwani District Hospital in Enugu South Local Government Area. Questions were adjusted accordingly during pretesting in order to ensure that proper meanings were conveyed. The data-collection tool was divided into three sections: participants’ sociodemographic characteristics, questions that measured their previous screening and questions about their vaccination status. HCWs were said to have received complete vaccination if they had received three doses of the hepatitis vaccine in accordance with the vaccination schedule. The tool was written in English. Since questionnaires were administered by an interviewer, participants were able to obtain immediate clarification from data collectors. The questionnaires were administered and collected immediately by four resident doctors in the Department of Community Medicine. Written informed consent was obtained from all respondents. No names of the HCWs were collected, and participants were assured of confidentiality of all results obtained. Completed questionnaires were stored by the team lead and will be destroyed two years after the survey. HCWs were screened for the presence of hepatitis B antigen using Determine Rapid Diagnostic Kits (Abbott Laboratories, Abbott Park, IL). New lancets were used to prick each client’s thumb, and two drops of blood were added to the diagnostic kit, which was read after 15 minutes. Results were reported as either negative when no red band was seen in the test band area or positive when a red band was seen in the test band area. HCWs whose results were negative and who could afford the subsidised vaccine were given the vaccine. Those who were diagnosed as positive were referred to the gastroenterology clinic for further management. Subsequently, the respondents were classified as clinical staff and non-clinical staff. Clinical staff consist of those who have direct contact with patients, including doctors, nurses, pharmacists and laboratory scientists. The hospital departments were also grouped into clinical and non-clinical. Clinical departments included community medicine, radiology, internal medicine, obstetrics and gynaecology, paediatrics, accident and emergency, nursing and medical laboratory departments. Non-clinical departments consisted of administrative, nutrition and others.
Data analysis
Data entry and analysis was done using IBM SPSS for Windows v23 (IBM Corp., Armonk, NY). A test of association was carried out. The level of significance was set at a
Results
Table 1 highlights the sociodemographic characteristics of the respondents. Out of the 241 HCWs, the majority were female (192/241; 79.67%) and within the 25- to 44-year age group (163/241; 67.63%). Their mean age was 40.60±7.90 years, four-fifths (195/241; 80.91% had completed tertiary education and more than one third (93/241; 38.59%) worked in the administrative department of the hospital. The prevalence of hepatitis B surface antigen (HBsAg) was 2.07% (5/241), 25.31% (61/241) of the respondents had been previously screened for HBV infection and 6.67% (16/241) of the respondents had been previously fully vaccinated.
Sociodemographic characteristics of the health-care workers.

Table 2 revealed that when HBV positivity was stratified according to the sociodemographic characteristics of the HCWs, the prevalence of the disease was highest among HCWs who were male, aged 35–44 years, had completed secondary education and worked as non-clinical staff and in non-clinical departments. HCWs who had worked for less than five years were also more likely to have the disease. These findings were not statistically significant.
Factors associated with HBV positivity among Healthcare workers.
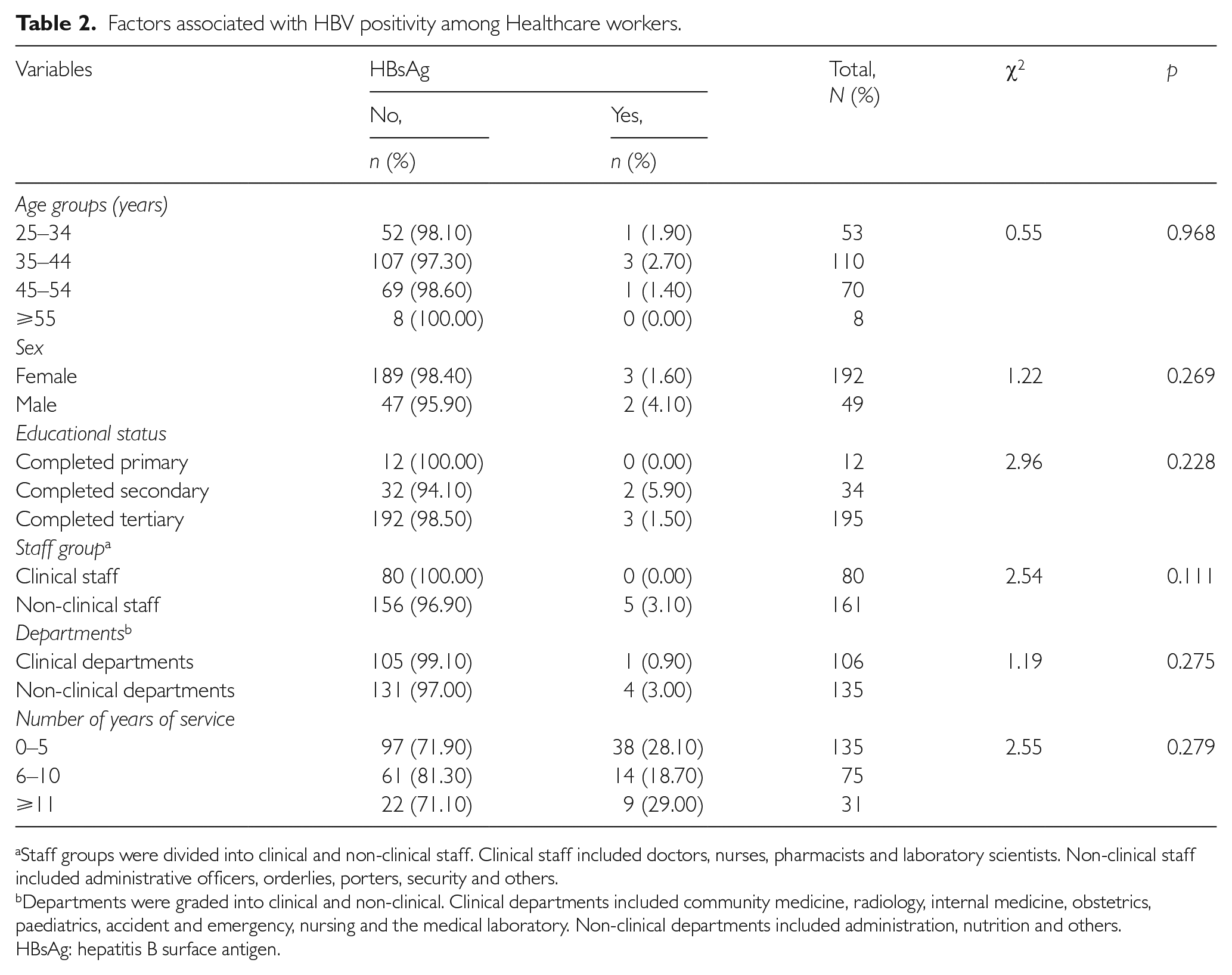
Staff groups were divided into clinical and non-clinical staff. Clinical staff included doctors, nurses, pharmacists and laboratory scientists. Non-clinical staff included administrative officers, orderlies, porters, security and others.
Departments were graded into clinical and non-clinical. Clinical departments included community medicine, radiology, internal medicine, obstetrics, paediatrics, accident and emergency, nursing and the medical laboratory. Non-clinical departments included administration, nutrition and others.
HBsAg: hepatitis B surface antigen.
Table 3 depicts the predictors of previous HBV vaccination. Respondents who had ever been screened and who worked in clinical departments were about 12 times and 5 times more likely, respectively, to have been vaccinated against hepatitis B infection than those who had never been screened or were working in non-clinical departments. These results were statistically significant.
Factors associated with previous HBV vaccination among health-care workers.

Staff groups were divided into clinical and non-clinical staff. Clinical staff included doctors, nurses, pharmacists and laboratory scientists. Non-clinical staff included administrative officers, orderlies, porters, security and others.
Departments were graded into clinical and non-clinical. Clinical departments included community medicine, radiology, internal medicine, obstetrics, paediatrics, accident and emergency, nursing and the medical laboratory. Non-clinical departments included administration, nutrition and others.
HBV: hepatitis B virus; NA: not applicable; AOR: adjusted odds ratio; CI: confidence interval.
Discussion
Prevalence of HBV among HCWs
Overall, 241 HCWs participated in this study. The mean age of the HCWs and their duration of employment were 40.60±7.90 years and 11.20±7.70 years, respectively. The HBV prevalence of 2.07% found in this study is slightly less than reported in a similar Nigerian study (13%). 31 This invariably reveals a decline in the prevalence of HBV, like other infectious diseases in the region. This effect could have resulted from enhanced uptake of interventions targeted at reducing contact with blood and body fluids. A prevalence of 2.9% was reported among HCWs in a comparable study group in Rwanda, despite high reported exposure to body and blood fluids. 32 A lower prevalence has been recorded among HCWs in Libya (1.8%), 33 Poland (1.2%) 34 and Brazil (0.8%), 35 while a higher HBsAg positivity rate of 8.1% has been reported in Uganda, 36 7.0% in Tanzania 37 and 8.7% in Saudi Arabia. 38 The prevalence of HBV infection in the general population and the high frequency of probable accidents with HBV among HCWs make it paramount that appropriate and consistent safety measures by HCWs be adopted. 39
The prevalence of the disease was found to be lower among the hospital staff who have contact with patients than those who do not have contact with the patients. Findings from this study reveal that 60% of the positive cases were from the hospital’s administrative staff. This group of HCWs can generally be classified as HCWs working in the low-risk sector. Contrary findings have been reported in a South American study where there was no significant difference in HBV serology between clinical and non-clinical staff. 40 Ciorlia Luiz et al. reported a higher prevalence in HCWs who worked in the maximum-risk sector in Brazil. 35 Likewise, the highest rates of HBsAg in HCWs were reported among nurses and nurse aides and also HCWs who work in obstetric wards, isolation rooms, dialysis units and dentist units in Eastern Libya. 33 Thus, this lower prevalence recorded among the high-risk sector in this study could be attributed to the effectiveness of the hospital protocol on infection prevention and control, ensuring that universal precautions are in place to reduce contact with blood and fluid. This has invariably reduced possible transmission from positive patients and vice versa.
Screening and vaccination status
It is disturbing that despite the high endemicity of HBV infection in Nigeria, 41 only 61/241 (25.31%) of the HCWs had previously been screened for HBsAg. Though a safe, effective and highly acceptable HBV vaccine has been available for more than three decades now, 36 a low vaccination coverage rate (completed vaccination schedule of three doses) of 6.6% was found in this study. This is an improvement from the 3.7% vaccination coverage rate recorded in 2006 within Enugu. 42 A low vaccination coverage rate (29.8%) has surprisingly been reported among theatre staff and laboratory scientists working in a Nigerian tertiary health institution, taking into consideration the fact that they work in areas classified as having the highest risk of occupational exposure to blood-borne pathogens. 39 This low vaccination coverage rate can be attributed to the absence of a national HBV vaccination programme for HCWs in the country and should be addressed, as studies have reported low vaccination uptake among HCWs in Nigeria.31,43 A completed vaccination coverage rate <50% has also been recorded among HCWs in other African countries such as Kenya (12.8%), 44 Cameroon (12.3%), 45 Rwanda (0.8%), 32 Ethiopia (5.4%) 46 and Uganda (34.8%). 36 This brings to light a public-health hazard, as HCW are at risk of contracting HBV from infected patients and, if infected, are equally at risk of transmitting the virus to other patients. 47 Hence, there is a need to prevent the occurrence of this infection primarily among the HCWs. Contrary to this finding, high vaccination coverage rates among HCWs as high as 52% have been reported in Libya and 90% in Poland. 34 This could be attributed to efficient vaccination programmes, as well as low HBV endemicity in these regions, having a HBsAg prevalence <2%, with low risk of progression to chronicity. 48
Factors affecting vaccination status
On bivariate analysis, being a clinical member of staff, working in clinical departments and having been screened for HBV previously were associated with uptake of the HBV vaccine. However, on multivariate analysis, HCWs who had previously been screened against HBV had about 12 times the odds of being vaccinated compared to those who had never been screened for the virus. The members of the staff working in clinical departments were also about five times more likely to have been vaccinated compared to their counterparts working in non-clinical departments. This explains the lower prevalence recorded among clinical staff in this study. There is a higher chance of HCWs in clinical departments being more knowledgeable on the modes of transmission and prevention against HBV than those not in clinical departments. This level of knowledge could have invariably translated to better attitude and practice. In a study by Muhammad et al., the frequency of vaccination was reported to be highest among doctors (92.4%) and lowest among nursing assistants (18.9%). 49 Similarly, vaccination uptake was significantly higher among doctors in South Africa. 50
Limitations
Although all HCWs in the facility were expected to take part in the vaccination programme, only 14% participated. This number may not be a true representative of the hospital population. Hence, study findings may not be generalisable. Due to poor funding, polymerase chain reaction could not be performed on all positive samples of HBsAg antibody to determine the level of HBV DNA viraemia and to differentiate between HCWs with acute or chronic infections. The post-vaccine (anti-HBs) serological test recommended for all who were vaccinated is yet to be carried out due to non-availability of funds.
Conclusion
Although the available data show that vaccination of HCWs has been proven to reduce HBV infection in several health facilities globally, vaccination coverage among HCWs in this study was poor. Since it could not be ascertained if these infections were occupationally acquired, pre-employment screening and vaccination is recommended. The hepatitis B awareness exercise increased uptake of vaccination of HCWs. This was encouraged by provision of the vaccine at subsidised rates to the HCWs. At the end of the vaccination campaign, a reasonable proportion of the HCWs had received full HBV vaccination. Thus, it can be concluded that a hospital vaccination awareness campaign is a viable and effective intervention that should be adopted with the aim of increasing vaccination uptake in health-care facilities. Due to the high prevalence of the disease among non-clinical staff, emphasis on awareness should be placed on other means of transmission, including unprotected sexual contact.
Footnotes
Acknowledgements
We would like to thank Emzor and Mega Life Pharmaceuticals for supporting the hospital during the 2018 World Hepatitis Day.
Authors’ contributions
E.N. and O.C. researched literature and conceived the study. C.J. was involved in the development, gaining ethical approval, patient recruitment and data analysis. O.C. wrote the first draft. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
Availability of data and materials
The data sets generated and /or analysed during the current study are available with the lead author.
Ethical approval
Ethical approval to report this case/these cases was obtained from the Ethics and Review Committee of the Enugu State University Teaching Hospital, Parklane Enugu.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
