Abstract
Acute hepatitis is an unusual manifestation of listeriosis. Most patients with listeriosis present with fever, flu-like illness and gastroenteritis symptoms due to consumption of contaminated food. Pregnancy-associated Listeria monocytogenes infection commonly occurs during the third trimester of pregnancy compared to early trimesters. We report a case of listeriosis in the first trimester of pregnancy, which presented with the acute onset of jaundice and was successfully treated with ampicillin.
Case report
A 25-year-old Malay primigravida at 13 weeks of pregnancy presented with persistent nausea, vomiting and fever for five days. It was associated with yellowish discolouration of the eyes, acute abdominal pain and diarrhoea. She denied any history of taking traditional medication, family history of liver disease and high-risk behaviours to exclude hepatitis disease. She was recently diagnosed with transient gestational thyrotoxicosis one week before admission. Her thyroid function was taken, as she had severe nausea and vomiting in pregnancy.
Upon examination, she had a spike in temperature (39.2°C) with normal blood pressure. Her abdomen was tender on the right hypochondriac area. Her total white blood cell count was normal (8.66×109/L), but she was anaemic (haemoglobin was 10.0 g/dL) and her platelet count was at the lower limit of normal (147×109L). Her liver function test showed transaminitis, with alanine transaminase of 123 IU/L, aspartate transaminase of 69 IU/L, normal alkaline phosphatase (65 IU/L) and total bilirubin of 97 µmol/L.
Based on her symptoms and blood results, she was initially treated as acute cholecystitis in pregnancy. She was given empirical intravenous (i.v.) cefoperazone and metronidazole. An urgent abdominal ultrasound was performed and revealed normal findings. The gallbladder was not distended, and no biliary stone seen. Hepatitis screening for hepatitis A, B and C was non-reactive. In view of all these findings, hepatic disease was excluded.
Blood culture was taken prior to initiation of antibiotic therapy and was flagged positive at 18 hours and four minutes of incubation. Gram staining showed Gram-positive bacilli in diphtheroid form (Figure 1). After 24 hours of incubation, blood agar grew small grey colonies with no haemolysis (Figure 2). No growth of colonies was noted on MacConkey agar. The colonies resembled Corynebacterium species. However, upon subjecting them to matrix-assisted laser desorption/ionisation time-of-flight mass spectrometry, the colonies turned out to be Listeria monocytogenes, with a persistent score value of >2.0.

Gram staining of Listeria monocytogenes shows diphtheroid form.
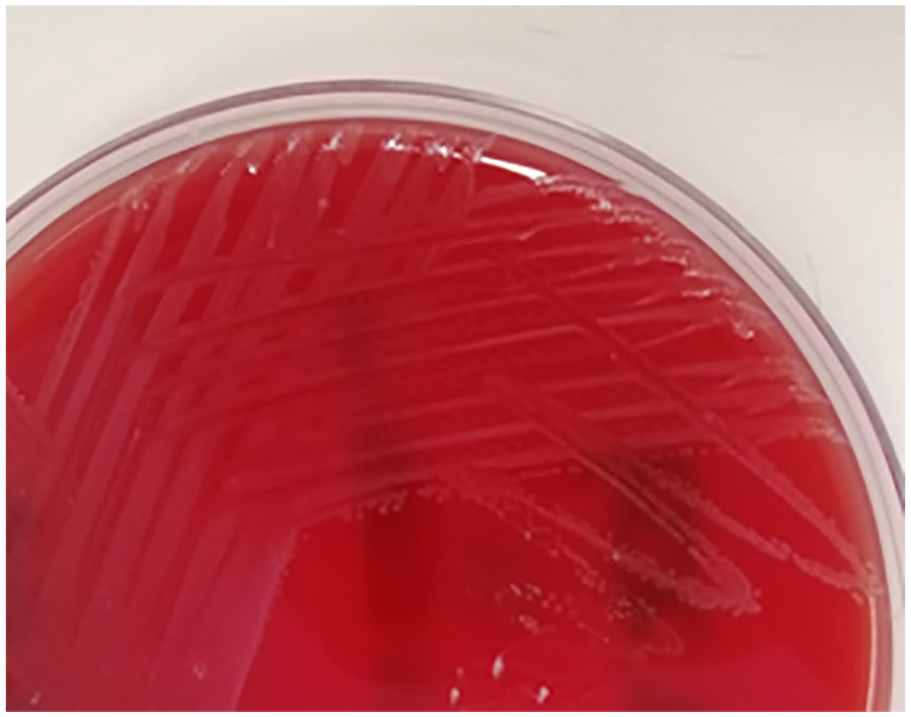
Non-haemolytic colonies L. monocytogenes on blood agar.
The antibiotic was changed to 2 g i.v. ampicillin every four hours for two weeks. On the ward, she responded well to the antibiotics given. An ultrasound scan of the foetus was normal. She was discharged with oral ampicillin for another two weeks. This patient was well after being discharged home, and her subsequent antenatal check-up was normal. She was under medical follow-up until delivery.
Discussion
L. monocytogenes is an intracellular bacterium that has the ability to survive in human cells. 1 It is known to cause food-borne illness, and outbreaks are associated with consuming contaminated food.1,2 In the environment, the organism is isolated from soil, dust, water, processed foods, raw meat and human and animal faeces.1,2 The pathogen is able to form a biofilm on the surface of many foods and can survive at 4°C in the refrigerator.1,2 Listeriosis is seen more commonly in the obstetric group compared to the general population probably due to reduce cellular immunity during pregnancy.2–4 A higher incidence during pregnancy may be associated with the eating habits of pregnant women. They consume more high-risk foods that are susceptible to L. monocytogenes contamination such as unpasteurised dairy products, preprepared food, processed food and raw-milk cheese. 4
The incidence rate of perinatal listeriosis in Singapore is 4.8 cases per 100,000 live births. The majority of the cases are Chinese (54%), as they constitute the main population in Singapore, followed by other races such as Indian, Malaysian and Indonesian. 5 The rate is higher than that in the UK (4.0 cases per 100,000 live births) and the USA (3.48 cases per 100,000 live births). 5
Listeriosis causes a mild illness in the mother but has harmful consequences for the fetus.2,6 About 30% of maternal listeriosis may cause stillbirth, miscarriage as well as preterm delivery, with those neonates surviving being infected with listeriosis.1,2,6 The most common clinical presentations for neonatal listeriosis (NL) are septicaemia (81–88%), respiratory distress (38%) and meningitis (24%). 5 Cutaneous eruptions such as papules, pustules, vesicles or ulcers, endocarditis and multiple abscesses are infrequent symptoms of NL. 5 Other presentations include granulomatosis infantiseptica – a severe form of NL manifest with widespread microabscesses, miliary granulomas, area of necrosis and liver involvement. 5
Maternal listeriosis usually presents with fever associated with flu-like illness (100%), reduced foetal movements (45%), preterm labor (36%) and diarrhoea (18%). 5 L. monocytogenes bacteraemia rarely presented with hepatic involvement. However, there are a few reports in the literature of hepatic involvement in adult listeriosis.7–9 These mainly occurred in immunocompromised patients such as those with underlying diabetes mellitus, chronic liver and renal diseases, alcoholism, malignancy, organ transplant, those on immunosuppressive drugs as well as those who were pregnant. Solitary liver abscess, multiple liver abscess and diffuse or granulomatous hepatitis are the main clinical presentations of hepatic involvement in L. monocytogenes infection.7–9
In most cases, hepatic involvement in L. monocytogenes infection is not suspected at initial presentation until a blood culture isolates this organism. 9 This was also the situation with our patient, as she was misdiagnosed with acute cholecystitis because she presented with jaundice and abdominal pain. The diagnosis was changed to listeriosis when the blood culture was positive for L. monocytogenes. Listeriosis with jaundice is a rare presentation in a pregnant woman. When a pregnant lady presents with jaundice and transaminitis, the differential diagnosis is related to pregnancy-related hepatic disease. 10 Pregnancy-related jaundice is seen in cases of severe hyperemesis gravidarum, intrahepatic cholestatic in pregnancy, eclampsia or HELLP syndrome (haemolysis, elevated liver enzyme levels and low platelet levels) and acute fatty liver. Liver disease that can induce jaundice in pregnancy includes acute viral hepatitis, drug-induced hepatitis, choledocholithiasis or exacerbation of an underlying liver disease such as chronic hepatitis, autoimmune disease, Wilson’s disease and primary biliary cirrhosis. 10 These differential diagnoses were excluded in our patient, as her blood pressure, lipid profile and ultrasound findings were normal, with no history of taking hepatotoxicity drugs, a non-reactive hepatitis screening and no haemolytic features in a peripheral blood film.
A study by Noriega et al. reported that most cases of maternal listeriosis occur in primigravidae. This situation is probably due to the lifestyle of young couples, as primigravidae live with their partner and consume a lot of prepared or processed food, keeping these foods for a longer period than expected in the fridge, eating outside most of the time and with poor refrigerator cleaning habits. 1 The source of infection for this patient was not identified. She was a primigravida and lived with her husband. Since she had hyperemesis gravidarum, her husband prepared their food, mainly processed meals. The most possible cause of listeriosis in this patient may be from the processed food that was contaminated with L. monocytogenes.
In this case, the organism was isolated from a blood culture sample. Gram staining of the colony showed diphtheroid form and non-haemolytic colonies on blood agar. L. monocytogenes can be isolated from amniotic fluid, cerebrospinal fluid and vaginal and stool samples.1,2 Women are considered as listerial carriers if the organism is isolated from a vaginal or stool culture. About 1–15% of women are faecal carrier, with the incidence of vaginal carriers being lower than that of faecal carriers. 2 L. monocytogenes appears as regular, Gram-positive bacilli or short, plump coccobacilli on Gram staining. However, there is variation in Gram staining of L. monocytogenes, as some of the isolated colonies resemble diphtheroid (Corynebacterium spp) or diplococci (Streptococcus pneumoniae). 2 The colonies of L. monocytogenes may show a narrow zone of beta haemolysis that looks like group B Streptococcus. The β-haemolysis will be more obvious with prolonged incubation. Some atypical strains of L. monocytogenes have mutations at their virulence genes that may produce weakly haemolytic or non-haemolytic colonies. 4
As listeriosis is a rare disease in pregnant women, the appropriate duration of treatment in pregnancy has not yet been standardised. 2 Optimal antibiotic treatment given to the mother will result in a favourable outcome for the neonate.3,6 It this case, the isolate was susceptible to ampicillin and trimethoprim/sulfamethoxazole (TMP/SMX). She was treated with 2 g i.v. ampicillin every four hours for two weeks. She was discharged with oral antibiotics for another two weeks. Several case reports have stated that the duration of treatment in early pregnancy was 7–14 days, and others have reported that treatments need to be continued until delivery if the foetus survives. 6 Cases of maternal listeriosis in the third trimester of pregnancy receive antibiotic treatment until delivery. 6 The pregnancy outcome in our patient is not known, as she has not yet delivered her baby. We will carry out a further follow-up of her pregnancy in the postnatal period to examine the pregnancy outcome and to make correlations regarding the early treatment advantage as well as the appropriate duration of treatment.
A few things need to be considered before starting the antimicrobial therapy. As L. monocytogenes is an intracellular organism, an antibiotic that can penetrate into the host cell, maintain a high intracellular concentration and bind to the penicillin-binding protein 3 (PBP3) of the listeria needs to be chosen. 2 Penicillin, ampicillin and amoxicillin are the recommended antibiotics for the treatment of listeriosis.1,2 A study reported that 91% of cases of maternal caseslisteriosis received ampicillin and penicillin as the treatment regime, and they fully recovered. 5 In order to obtain sufficient penetration via the umbilical cord and placenta, a high dose of antibiotic is recommended. A high dose (2 g) of ampicillin every four hours for 7–14 days is the recommended dose for pregnant women. 2 All listeriosis are susceptible to the penicillin group. So far, there are o reports on the isolate of L. monocytogenes showing resistance to penicillin. 2 Few studies recommend adding gentamicin in the treatment regimen, as this combination will give a synergistic effect. 6 Some clinicians still have doubts regarding gentamicin toxicities in this combination regimen. 2
TMP/SMX is an alternative treatment option for patients who are allergic to penicillin.1,2 It was given in high doses like penicillin, either orally or i.v. TMP/SMX can cause neural tube defects, as trimethoprim has anti-folate activity, and it should be avoided in early pregnancy. Thus, this antibiotic was not given to this patient, as the risk outweighed the benefit.1,2
Macrolide is the second line of treatment for listeriosis, and it is recommended for pregnant women who are allergic to penicillin. For effective treatment, the suggested dose is 4 g per day for 7–14 days.1,3 Unfortunately, erythromycin results in subtherapeutic concentrations in the amniotic fluid and foetal serum via transplacental passage.1,2
Summary
Acute hepatitis is rare but may occur in pregnant women with listeriosis. The clinician needs to have a high index of suspicion of listeriosis to avoid misdiagnosis at initial presentation. Prompt diagnosis and early initiation of recommended antimicrobials can save the mother and prevent neonatal complications.
Footnotes
Acknowledgements
None.
Authors’ contributions
The first, second and fifth authors performed a literature review, provided the attached images and conceived the case report. The third and fourth authors reviewed and edited the manuscript.
Availability of data and materials
Detailed patient information is available from the corresponding author.
Ethical approval
Our institution does not require ethical approval for reporting individual cases or case series.
Informed consent
Written and verbal consent were obtained from the patient for her anonymised information to be used in this article.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
