Abstract
Background:
Evidence shows that early initiation of a continuous chain of rehabilitation is associated with better functional outcomes in traumatic brain injured patients. The Department of Rehabilitation Medicine initiated early screening and review of patients with all traumatic brain injury (TBI) severity within 72 hours of acute admission, followed by direct transfer of suitable patients to acute inpatient rehabilitation (AIR).
Objectives:
This study aim to document the demographics and clinical characteristics of all TBI patients admitted to the local acute hospital; determine the characteristics of patients with TBI who are directly transferred to AIR following early screening and review; and determine clinical predictors affecting functional outcomes of patients of all TBI severity.
Methods:
A total of 491 patients were screened and reviewed; 116 patients were directly transferred to AIR.
Results:
The median age of the screened cohort was 67.0 years (interquartile range 50.0–77.0 years). Falls were the leading mechanism of TBI. Infection (odds ratio (OR)=2.95, 95% confidence interval (CI) 1.59–5.49) and neurosurgical intervention (OR=2.18, 95% CI 1.24–3.81) increased the odds of transfer to AIR. The Functional Independence Measure (FIM) gain after receiving AIR was significant (p<0.001). Increased age, complications, high motor admission FIM (AFIM) and long rehabilitation length of stay (RLOS) were negatively associated with FIM gain and FIM efficiency.
Conclusions:
Our study demonstrated that falls were the leading mechanism of TBI, with the majority of patients being older. Infection and neurosurgical intervention increased the likelihood of transfer to AIR. There was functional improvement after AIR. Age, complications, motor AFIM and RLOS were negatively associated with FIM gain and FIM efficiency. Further local research is warranted to confirm these findings.
Introduction
Early rehabilitation medicine specialist care and consultation during the acute hospitalisation of patients with traumatic brain injury (TBI) have been shown to be associated with better functional outcomes and shorter length of stay (LOS).1,2 Earlier rehabilitation admission was associated with greater recovery, lower costs and shorter LOS in severe TBI patients.3–5 Early initiation of rehabilitation within an acute setting followed by direct transfer to a specialised rehabilitation hospital (continuous chain of early rehabilitation) has also shown a decrease in disability and increase in cost-effectiveness.6,7
With the aim of improving the standard of care for patients with TBI, the Department of Rehabilitation Medicine started a pilot service of early screening and review of patients of all TBI severity within 72 hours of acute admission in an acute tertiary hospital, followed by direct transfer of suitable patients to its acute inpatient rehabilitation (AIR) unit. The objectives of the study are: (a) to document the demographics and clinical characteristics of patients of all TBI severity admitted to the acute hospital; (b) to determine the characteristics of patients with TBI who are directly transferred to the AIR unit, following early screening and review; and (c) to determine the clinical predictors affecting functional outcomes of patients of all TBI severity.
Methods
Participants
A total of 491 patients with head trauma were screened and reviewed between 1 November 2010 and 30 October 2012 by the on-duty rehabilitation medicine specialist within 72 hours of admission to the Department of Neurosurgery (NES) ward in an acute tertiary hospital. Five rehabilitation medicine specialists were rostered to perform the screening and review at that time.
Patients received twice weekly multidisciplinary reviews and approximately half an hour to two hours of therapy per day, five days a week, depending on their medical stability and rehabilitation needs, while they were acutely admitted under NES. The multidisciplinary team consisted of a rehabilitation medicine specialist, nurse, physiotherapist, occupational therapist, speech therapist, dietician and medical social worker. Patients who fulfilled the following criteria were then recommended and transferred to AIR: (a) presence of impairments or disabilities which could benefit from a comprehensive inpatient rehabilitation programme, (b) potential to participate in a goal-oriented rehabilitation programme and (c) medical stability to participate in a rehabilitation setting. These criteria were based on our department’s general criteria for admission to AIR which were similar to other clinical practice guidelines for the rehabilitation of TBI patients. 8
A total of 116 patients were directly transferred to AIR (continuous chain of early rehabilitation).
Procedures
This was a retrospective study of the Department of Rehabilitation Medicine Traumatic Brain Injury Registry and Database. Approval and waiver of consent was obtained from the Institutional Review Board. The principal investigator and co-investigators reviewed the medical records.
The data collected included demographic variables consisting of age, sex, and race; acute clinical characteristics, including mechanism of injury, Glasgow Coma Scale (GCS) upon admission, neuroimaging findings and neurosurgical interventions; complications, including nosocomial infections, post-traumatic seizures, deep-vein thrombosis (DVT), dysautonomia and the need for tracheostomy; acute LOS (ALOS) and the discharge disposition; rehabilitation outcomes, including the Functional Independence Measure (FIM) and Rancho Los Amigos Scale-Revised (RLAS-R) scale. For patients transferred directly to AIR, rehabilitation LOS (RLOS), FIM gain (discharge FIM (DFIM)–admission FIM (AFIM)) which measures functional improvement and FIM efficiency (FIM gain/RLOS) which measures rate of functional improvement were collected. 9
Measures
The FIM is a standardised functional outcome measure commonly used in rehabilitation, and its validity in patients with TBI is well supported.10,11 It consists of 13 motor and five cognitive items. The scores range from 1 (totally dependent) to 7 (totally independent) for each item, with a maximum score of 126. The FIM was recorded during the first review within 72 hours of admission for all screened patients.
The RLAS-R is a standardised 10-level descriptive scale which describes the cognitive and behavioural patterns in brain-injured patients as they recover. 12 It facilitates communication among health-care professionals and is useful in treatment planning and cognitive recovery tracking. 12 The RLAS-R was recorded during the first review.
The injury mechanisms were classified as falls, road traffic accidents (RTA), assault, sports and other. Falls were categorised into mechanical (e.g. slipped and fell on wet surface), non-mechanical (e.g. fell as a result of muscle weakness) and unwitnessed falls. The term ‘mechanical fall’ was based on the description recorded by the admitting doctors, which was associated with a slip or trip, implying an external mechanical force or object had caused the fall. 13 Sports were further differentiated into non-contact versus contact sports (e.g. rugby, boxing, martial arts and soccer).14,15
The GCS was documented on admission and was used to classify the severity of TBI into mild (GCS 13–15), moderate (9–12) and severe (GCS 3–8) categories.16–18
The types of head injury were determined according to predominant neuroimaging findings and were categorised into isolated subdural haematoma (SDH), isolated subarachnoid haemorrhage, isolated extradural haemorrhage, isolated contusion, isolated intracerebral haemorrhage, mixed haemorrhage (combination of any of the above haemorrhages), other (face or skull fractures and/or scalp haematoma) and concussion. Concussion is usually associated with normal structural neuroimaging. 19 It is defined as ‘biomechanical injury leading to altered brain function and its sequelae include somatic, cognitive and emotional disturbances, which are usually most severe within the first week post-injury’. 19
Nosocomial infections and DVT were recorded based on investigations; post-traumatic seizures and dysautonomia were recorded based on medical records; tracheostomy and neurosurgical interventions were recorded based on surgical records.
The ALOS for all screened patients was defined as the time from acute NES admission to direct discharge from NES. For patients who were directly transferred to AIR, the RLOS was defined as the time from admission to AIR to discharge.
Statistical analysis
Descriptive statistics for continuous data are presented as percentages or as the median with interquartile (IQR) range. For normally distributed data, an independent t-test and one-way analysis of variance were used to assess differences in group means for continuous variables, while Fisher’s exact test and the chi-square test were used to examine the differences for categorical variables. For non-normally distributed data, the Mann–Whitney U-test or Kruskal–Wallis H-test was used instead.
Variables which were clinically relevant for transfer to AIR, with p<0.10 in the univariate analyses, were selected for entry into a multivariate logistic regression model to determine the variables associated with discharge outcome of the early screened patients (directly discharged from the acute NES ward or directly transferred to AIR). 20
Wilcoxon’s signed rank test was used to compare AFIM and discharge DFIM within the AIR group. Age was divided into <30 years, 30–59 years and ⩾60 years to determine whether there were differences in FIM gain and FIM efficiency among the young, middle-aged and older groups. Multiple linear regression analyses were performed to identify the independent clinical variables associated with FIM gain and FIM efficiency.
Significance was determined at p⩽0.05, and statistical analysis was done using IBM SPSS Statistics v 25 (IBM Corp., Armonk, NY).
Results
Demographics and clinical characteristics of the early screened group
The median age of the patients was 67.0 years (IQR 50.0–77.0 years). The ratio of men to women was 1.96. There was a unimodal age distribution, with a peak in those aged 70–79 years, which was also the peak incidence of falls (Figures 1 and 2). The TBI admissions were mostly mild in severity (82.5%; Table 1).
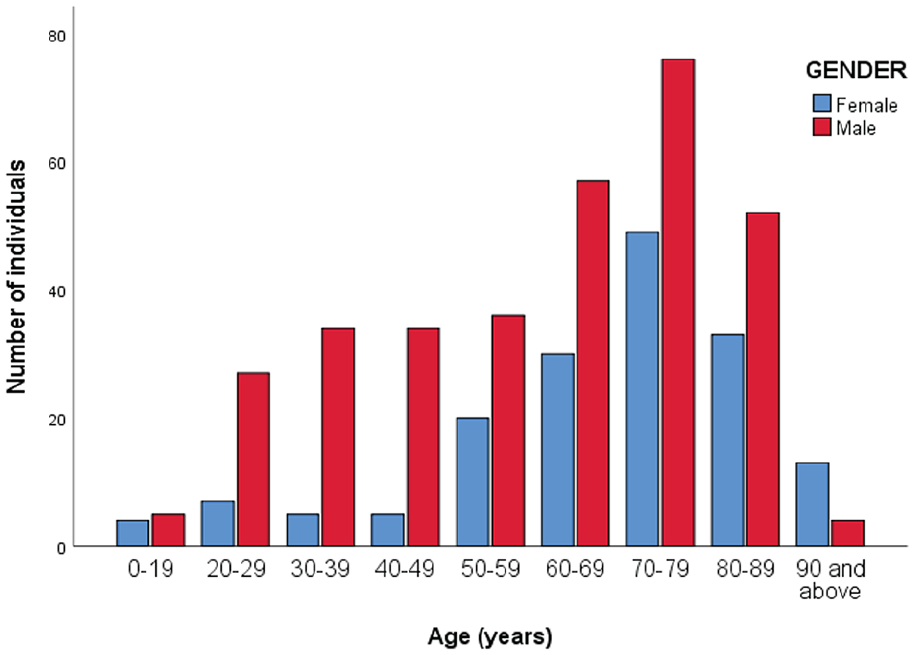
Sex distribution of individuals with traumatic brain injury (TBI) according to age groups.

Mechanism of injury according to age groups.
Baseline characteristics of patients admitted with TBI.

TBI: traumatic brain injury; IQR: interquartile range; RTA: road traffic accident; RLAS-R: Rancho Los Amigos Scale-Revised; SDH: subdural haematoma; SAH: subarachnoid haemorrhage; ICH: intracerebral haemorrhage; EDH: extradural haemorrhage; EVD: external ventricular drain; ICP: intracranial pressure; FIM: Functional Independence Measure; LOS: length of stay.
Patients with severe TBI were younger than those with moderate and mild TBI (p<0.001). The median age was 54.0 years (IQR 36.0–66.0 years) in the severe TBI group, 61.0 years (IQR 41.0–74.0 years) in the moderate TBI group and 70.0 years (IQR 54.0–78.0 years) in the mild TBI group. In the severe TBI cohort, there was a bimodal age distribution, with two peaks in those aged 30–39 and 60–69 years (Figure 3).

Age and injury mechanism distribution in severe TBI.
Falls (76.8%, n=377) were the leading mechanism of injury, followed by RTA (11.2%, n=55; Table 1). More patients <60 years old were involved in assault, RTA and sports than those aged ⩾60 years old (14.7%, n=26 vs. 1.3%, n=4; 20.3%, n=36 vs. 6.1%, n=19; and 5.1%, n=9 vs. 0.0%, n=0, respectively; p<0.001). Falls affected more patients ⩾60 years old (89.5%, n=281 vs. 54.2%, n=96; p<0.001).
Among patients who fell, 74.5% (n=281) were ⩾60 years old (p< 0.001). There were 127 mechanical falls (33.7%), 152 non-mechanical falls (40.3%) and 98 unwitnessed falls (26.0%). The median ages of patients who sustained unwitnessed, non-mechanical and mechanical falls were 70.0 years (IQR 56.0–78.0 years), 72.0 years (IQR 59.3–80.0 years) and 72.5 years (IQR 61.8–81.0 years), respectively (p=0.123).
Among the nine cases of sports-related TBI, seven involved non-contact sports (77.8%), whereas two (22.2%) involved contact sports (one boxing and one Taekwondo).
Isolated SDH constituted 39.3% (n=193) of the injuries (Table 1). In one (0.2%) individual, no signs of intracerebral injury or haemorrhage were detected on computed tomography scan. Most patients did not require neurosurgical intervention (78.2%, n=384; Table 1). Twelve (2.4%) patients required tracheostomy.
Eighty-three (16.9%) patients developed nosocomial infections, with pneumonia and urinary tract infection (UTI) being the two leading infections (90.4%). The seven cases of non-infective complications comprised one (14.3%) DVT, four (57.1%) seizures and two (28.6%) dysautonomia.
The median total AFIM was 73.0 (IQR 28.0–103.0), and the median ALOS was 7.0 days (IQR 3.0–14.0 days; Table 1).
A total of 347 (70.7%) patients were directly discharged, and 116 (23.6%) patients were transferred directly to AIR (Table 2). The median ALOS of those directly discharged were shorter than those who received continuous chain of early rehabilitation (5.00 days (IQR 3.00–11.00 days) vs. 12.50 days (IQR 7.25–21.00 days); p<0.001).
Univariate analysis of clinical variables by discharge.

DVT: deep-vein thrombosis.
Out of the 28 patients who died, 12 (42.9%) sustained a severe TBI, 10 (35.7%) sustained a mild TBI and six (21.4%) sustained a moderate TBI.
Clinical predictors associated with transfer to AIR
Univariate analysis indicated age, sex, severity of TBI, neurosurgical intervention, infection and total FIM on review were significantly associated with transfer to AIR (Table 2). Multivariate analysis showed infection (OR=2.95, 95% CI=1.59–5.49) and neurosurgical intervention (OR=2.18, 95% CI 1.24–3.81) increased the odds of transfer to AIR (Table 3). Higher AFIM was associated with reduced likelihood of transfer to AIR (OR=0.98, 95% CI 0.97–0.99).
Multivariate analysis predicting likelihood of acute patient rehabilitation.

Moderate TBI and severe TBI are compared against mild TBI.
OR: odds ratio; CI: confidence interval.
Clinical characteristics of the continuous chain of early rehabilitation group
Demographics
Out of the 463 patients who survived, 116 (25.1%) patients were transferred directly to AIR, with a median age of 72.0 years (IQR 58.3–79.8 years). Most had sustained a mild injury (75.9%, n=88). Moderate and severe injuries each constituted 12.1% (n=14) of the injuries. The majority of the elderly (aged ⩾60 years) sustained a mild injury (87.1%, n=74) compared to the young (aged <30 years; 16.7%, n=1). Half of those aged <30 years (50.0%, n=3) sustained a severe injury, 52.0% (n=13) of those aged 30–59 years sustained a mild injury and 87.1% (n=74) of those aged ⩾60 years sustained a mild injury (p<0.001). Older age groups were moderately associated with milder injuries (r=0.473, p<0.001). Falls were the predominant cause (79.3%, n=92) followed by RTA (9.5%, n=11).
Functional recovery
Using the total DFIM to define recovery, 9.5% achieved a good recovery (FIM 109–126), 56.9% with moderate disability (FIM 72–108) and 33.6% with severe disability (FIM <72). One third (33.3%) of those aged <30 years achieved a good recovery, whereas 24% of those aged 30–59 years and 3.5% of those aged ⩾60 years achieved a good recovery (p=0.002).
The median total AFIM was 58.50 (IQR 19.75–84.75); the median total DFIM was 86.00 (IQR 60.50–98.75). The total functional and motor gains after AIR were significant (p<0.001; Table 4). The median total FIM gain was 12.00 points (IQR 2.00–41.00 points). The median FIM efficiency was 0.55 (IQR 0.67–1.58) points/day.
Median (IQR) total FIM and subscale scores on admission and discharge.

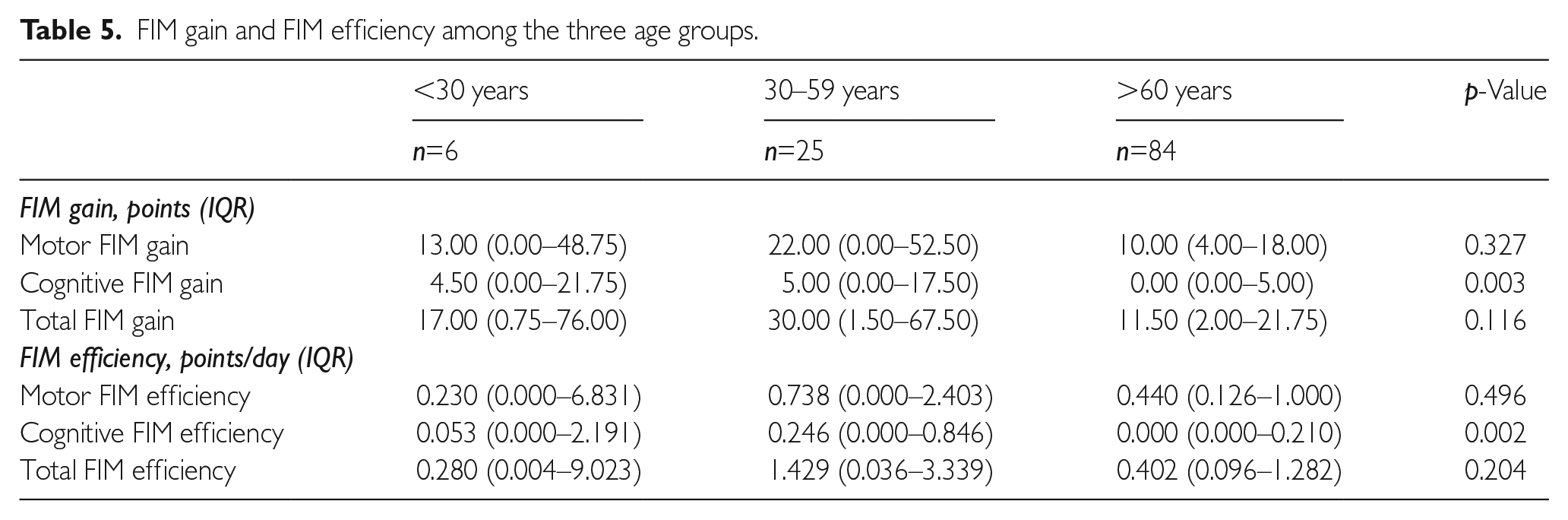
There were no differences in total FIM gain (p=0.116), total FIM efficiency (p=0.204), motor FIM gain (p=0.327) or motor FIM efficiency (p=0.496) among the three age groups. The cognitive FIM gain and cognitive FIM efficiency were different among the three age groups (Table 5).
FIM gain and FIM efficiency among the three age groups.
LOS
The median ALOS was 12.00 days (IQR 7.00–21.00 days). The ALOS of those with mild, moderate and severe TBI were 10.00 days (IQR 7.00–16.00 days), 17.5 days (IQR 9.50–30.00 days) and 27.00 days (IQR 13.50–38.75 days), respectively (p<0.001). The median RLOS was 20.50 days (IQR 12.25–30.50 days). The RLOS of those with mild, moderate and severe TBI were 20.00 days (IQR 13.00–26.75 days), 21.50 days (IQR 10.75–59.50 days) and 26.00 days (IQR 10.75–79.50 days), respectively (p=0.481). The ALOS was 31.50 days (IQR 21.50–50.0 days) in those aged <30 years, 13.00 days (IQR 10.00–20.00 days) in those aged 30–59 and 10.00 days (IQR 7.00–21.00 days) in those aged ⩾60 years (p=0.008). There was no difference in the RLOS among the age groups (p=0.891).
Linear regression analysis on FIM gain and FIM efficiency
Increased age, complications, high motor AFIM and long RLOS were associated with lower FIM gain and lower FIM efficiency (Tables 6 and 7).
Linear regression analysis on FIM gain.

Adjusted
GCS: Glasgow Coma Scale; AFIM: admission FIM; RLOS: rehabilitation length of stay.
Linear regression analysis on FIM efficiency.

Adjusted R2=0.323.
Discussion
This study provides information on the demographics of patients with TBI acutely admitted in a Singapore tertiary hospital and the functional outcomes related to a continuous chain of early rehabilitation. Most local studies focused on patients with moderate and severe TBI.21–24
Our study showed more males were admitted acutely for TBI, which was consistent with other demographic studies, as male sex has been established as a risk factor for TBI.25,26 The suggested reasons for higher TBI risk in males were related males often participating in more risk-taking behaviour, contact sports and alcohol consumption. 26 We did not analyse the sex-associated risk factors for TBI in our cohort, as this is not the focus of our study.
Our study showed a peak incidence of TBI in elderly patients, especially those aged 70–79 years, with falls being the predominant mechanism of TBI in the elderly, whereas RTA was the leading cause in younger patients. This was also the case in a recent study which reported a shift in local TBI demographics towards an older population, with an increased incidence of falls. 27 The rates of fall-related TBI could increase due to our rapidly ageing nation, which highlights the need to identify at-risk elderly populations and strengthen fall-prevention strategies.
Our study showed that the majority of patients selected for AIR were older patients with mild TBI. Functional impairment is prevalent in mild TBI, and studies have shown that mild TBI can result in cognitive and psychosocial impairment.28,29 Older patients with mild TBI have increased risk of poor cognitive performance, which could explain their need for inpatient rehabilitation, despite the mild severity. 28 Non-medical reasons for selection of mild TBI and older patients could be related to lack of caregivers (e.g. an aged spouse and/or working children), inadequate step-down facilities and limited home-care resources. We acknowledge that the demographic profile of the acute TBI admissions was skewed, with the majority of cases being mild TBI and older patients. This could have affected the profile of patients selected for AIR. Nevertheless, our study provided a snapshot of the local demographic TBI profile.
Our study showed that older age was a negative predictor of FIM gain and FIM efficiency, which is consistent with other studies. 30 This was despite older patients tending to have less severe TBI than younger patients. The possible reasons could be that older patients likely had more co-morbidities, less neurological and physical reserves and a higher tendency of poly-pharmacy which could affect recovery.31–33 This could account for there being no detectable cognitive FIM gain observed in our elderly group. Other reasons for the dismal cognitive FIM gain are discussed in a later section.
There has been a frequent selection bias in clinical and research practice towards younger patients with TBI. A systematic review showed that elderly patients were being under-represented in TBI research. 34 Cnossen et al. reported that age was an important determinant of referral decisions in 46% of the European neurotrauma centres, with younger patients often referred directly to specialised rehabilitation centres whereas patients aged ⩾65 years were often referred directly to nursing homes or local hospitals. 35 By implementing the service of early screening and review of all patients with TBI within 72 hours of acute admission, older patients have a similar opportunity as younger patients of being reviewed and accepted to AIR.
An interesting point to note from our results was that infection increased the likelihood of transfer to AIR. This could be due to sarcopenia associated with infection, which led to functional decline. Sarcopenia is defined as loss of skeletal muscle mass and muscle function and is associated with falls, functional decline and fraility.36–39 Patients with pre-existing sarcopenia on hospital admission had a higher risk of nosocomial infection. 40 Sarcopenia could also develop from the hypercortisolaemia, oxidative stress and inflammatory insults related to the infection. 41 We also found neurosurgical intervention increased the likelihood of transfer to AIR. Possible explanations were neurosurgical interventions were usually required in more severe TBI cases which could reflect the higher degree of motor and/or cognitive impairments, and the medical complexity of the patients who required neurosurgical intervention followed by specialised rehabilitation care. This illustrates the advantage of an AIR unit, which can handle highly complex cases through providing close rehabilitation medical supervision and 24-hour medical attention.
Our study showed a total FIM gain of 12.00 points (IQR 2.00–41.00 points), which was lower than the minimal clinically important difference for FIM of 22 commonly reported in the acquired brain injury literature. 42 Possible reasons for this included that some patients deteriorated functionally while they were in AIR due to medical co-morbidities and medical complications, resulting in negative FIM gain, and our study included TBI of all severity, of which mild severity constituted a large majority. FIM gains tend to be smaller among higher functioning patients, for example those with milder severity TBI or higher AFIM, due to the ceiling effect. 43 Thus, the FIM may not be sensitive enough to detect functional improvements in such patients. There is also a recognised floor effect of the FIM, for example a patient with severe TBI who required two-person maximum assistance and who progressed to one-person maximum assistance would have very little FIM gain. 43 In addition, the cognitive components of the FIM have low internal consistency and are not sensitive to change.43–45 This could possibly account for our dismal cognitive FIM gain results. To overcome this, other measurements such as Glasgow Outcome Scale–Extended could be used in conjunction with the FIM. 46 Nonetheless, FIM assesses the outcome of rehabilitation and is widely used during the regular weekly multidisciplinary meetings to discuss rehabilitation goals, rehabilitation intervention, functional improvement and discharge planning.
In terms of the efficiency of our AIR program, our FIM efficiency of 0.55 points/day seemed low in comparison with several US studies whose reported figures were 1.50–2.00,47–49 but we did not underperform in comparison with UK studies (0.14–0.25).43,50 Such variability could be related to differences in selection criteria for admission into inpatient rehabilitation, health and social services, demographic profile and case mix.
Our study showed that besides age, complications, high motor AFIM and increased RLOS were associated with reduced FIM gain and reduced FIM efficiency. Complications could lead to poorer functional outcomes as a result of treatment requiring longer RLOS and extended periods of immobility resulting in deconditioning and sarcopenia. Moreover, complications could happen more frequently in older patients and in patients with more co-morbidities and severe impairments. All these could negatively impact the outcome.
Study limitations
The principal investigator and co-investigators retrospectively reviewed the medical records for the data collection. The quality of the data collection was therefore dependent on the accuracy and reliability of the records documentation and the quality of data extraction. Although we attempted to collect data on duration of post-traumatic amnesia (PTA), which is a clinically relevant prognostic indicator in TBI, much of the data were incomplete and so we were not able to report PTA duration in the results.
We recognise the term ‘mechanical fall’ has not been well defined in academic research, and what differentiates a mechanical from a non-mechanical fall is subject to interpretation. A ‘mechanical fall’ is often associated with a slip or trip leading to a fall and implies that an external mechanical force or object caused the fall. 13 We are aware that external factors are rarely the sole cause of an elderly patient’s fall, and the use of ‘mechanical falls’ could inaccurately imply there is a benign cause for an elderly patient’s fall. 13 As our study did not focus solely on elderly patients, we have kept the use of the term ‘mechanical fall’.
Conclusion
Our study showed most of the acute TBI admissions were older patients, with the predominant mechanism related to falls. Patients who had neurosurgical intervention or infection were shown to have increased likelihood of being transferred to AIR. There was functional improvement in patients with TBI receiving a continuous chain of early rehabilitation. Increased age, presence of complications, high motor AFIM and increased RLOS were associated with lower FIM gain and lower FIM efficiency. Further local research is warranted to confirm these findings.
Footnotes
Acknowledgements
We would like to acknowledge Tan Yeow Leng and Jane Annie Nalanga who collected a proportion of the data, and Ng Yee Sien and Bok Chek Wai who supported the study.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Availability of data and materials
The data sets generated and/or analysed during the current study are available from the corresponding author.
Authors’ contributions
L.S.K. was involved in the literature research, collection and analysis of data, obtaining ethical approval from Institutional Review Board and writing of the first draft. T.Q.Q. was involved in the literature research and analysis of data. S.F.C. reviewed and assisted in the statistical analysis. All authors reviewed, edited the manuscript and approved the final version of the manuscript.
Conflict of interest
L.S.K., T.Q.Q. and S.F.C. declare there are no affiliations with or financial involvement with any commercial organisation with direct financial interest in the subject or materials discussed in this manuscript.
Ethical approval
Ethical approval for this study was obtained from the Centralised Institutional Review Board (CIRB Ref 2012/333/F: Department of Rehabilitation Medicine Traumatic Brain Injury Registry and Database).
Informed consent
Waiver of informed consent was obtained from the institution’s Centralised Institutional Review Board.
