Abstract
Background:
In Singapore, the number of hip fractures per year is projected to increase from 2500 to 9000 by 2050. Psychological factors are increasingly recognised as important predictors of healthy aging. While there are a growing number of studies examining resilience in different populations, there is a paucity of literature examining psychological resilience in individuals with hip fractures.
Objectives:
We aim to identify the association between high psychological resilience and improved functional outcomes in post-operative hip fracture patients in a Singapore Community Hospital, defined by a Conner-Davidson Resilience Scale 25 (CD-RISC 25) score of 62 and above.
Methods:
We conducted a pilot prospective cohort study in Bright Vision Community Hospital in Singapore. Post-operative elderly hip fracture patients were invited to participate in the study. Psychological resilience scores were measured on Day 1 of admission using CD-RISC 25. Functional outcomes were then tracked weekly for 21 days while participants underwent rehabilitation using the Modified Barthel Index (MBI).
Results:
High psychological resilience was found in 52.40% of the post-operative hip fracture participants in this study. Of those participants with high psychological resilience, 55% achieved functional independence (n = 11), compared with 47.47% of participants with low psychological resilience (n = 9) – although this result did not achieve statistical significance.
Conclusion:
One in two post-operative hip fracture patients had high psychological resilience, and our study suggests that patients with high psychological resilience can possibly achieve higher gains in functional scores and achieve functional independence.
Introduction
From 2000 to 2015, Singapore’s elderly population aged 65 and above doubled from 220,000 to 440,000 and is expected to increase to 900,000 by 2030. 1 Hip fracture incidence rates among men and women above 50 years old have risen 1.5-fold and 5-fold respectively since the 1960s, 2 and the number of hip fractures per year is projected to increase from 2500 at present to 9000 in 2050 because of our aging population.1,2
Poor functional outcomes have been reported after sustaining a hip fracture, with 40% unable to walk independently and 60% requiring assistance one year after sustaining a hip fracture. 3 Approximately 33% of those with poor functional outcomes became severely dependent or ended up in a nursing home one year after suffering a hip fracture . 4 Known predictors of functional outcomes in this group of patients include sociodemographic variables (age, gender, living conditions and presence of caregiver), comorbidities, characteristics of the fracture, treatment performed and destination at discharge.5–8
Psychological factors are increasingly being recognised as important predictors of healthy aging. 9 According to the World Health Organization’s Global Burden of Disease Study, these include depression, anxiety, resilience and personality traits. 10 Current rehabilitative strategies focus mainly on physical rehabilitation, but there is a growing recognition of the role that psychological factors may play in affecting the functional outcomes in patients with hip fractures.11,12
Psychological resilience is defined as the ability to effectively negotiate, adapt to, or manage significant sources of stress or trauma. 13 There is an emerging body of literature examining psychological resilience in different populations (large community samples, survivors of various trauma and adolescents), showing that higher psychological resilience levels lead to better outcomes. 13 However, there is a paucity of literature examining psychological resilience in individuals with hip fractures. Rebagliati et al. 14 looked at resilience as a possible predictor in hip fracture patients and found that low levels of resilience predicted poorer rehabilitation outcomes. Kohler et al. 15 did a similar study but did not manage to find a clear relationship between resilience and rehabilitation outcomes in this study. Therefore, we are unable to draw any conclusive deductions currently.
As Singapore is facing a silver tsunami, with the national healthcare spending almost doubling from SGD$11 billion in 2010 to SGD$21 billion in 2016, 16 it is imperative that we focus our efforts in improving our elderly’s health as this rate of growth in healthcare spending is not sustainable, and a possible addition to the solution would be to boost psychological resilience levels. Locally, no study has been conducted to determine whether there is any association between psychological resilience and functional outcomes for post-operative hip fracture patients. This association has been postulated to be an important concept to consider in the development of better individualised therapy plans and improved prognostication. 17
Therefore, our study’s objectives are to determine if there is an independent relationship between psychological resilience and change in MBI scores weekly, over a period of 21 days, and to determine if psychological resilience is independently associated with the ability to achieve functional independence (defined by an MBI status of more than 85).
Methods
Study location
This was conducted as a pilot prospective cohort study in Bright Vision Community Hospital (BVCH), a 317-bed community hospital affiliated with the Singhealth cluster, serving approximately 1500 new patients each year. 18 Patients here receive inpatient rehabilitation after their stay in a tertiary hospital. Hip fracture patients are typically bundled under a care package and the usual length of stay for these patients is approximately 21 days. 19
The standard practice in a Singapore Community Hospital is to provide 2 sessions of 45-minute inpatient rehabilitative therapy on weekdays, to improve a patient’s function so as to optimise activities of daily living (ADLs) and facilitate re-integration to a patient’s home environment or other long-term care settings. 20
Patient population
All post-operative hip fracture patients 65 years old and above, admitted from 4 June 2018 to 31 August 2019, who fulfilled inclusion criteria, were invited to participate in the study by consecutive sampling (Figure 1). The inclusion criteria included patients who were allowed full or partial weight bearing and were able to undergo rehabilitation. We excluded patients who were uncommunicative, unable to understand the questionnaires, declined to participate, or non-weight bearing. The participants could choose to answer in English, Mandarin, Tamil or Malay, and the questionnaires were interviewer-administered.
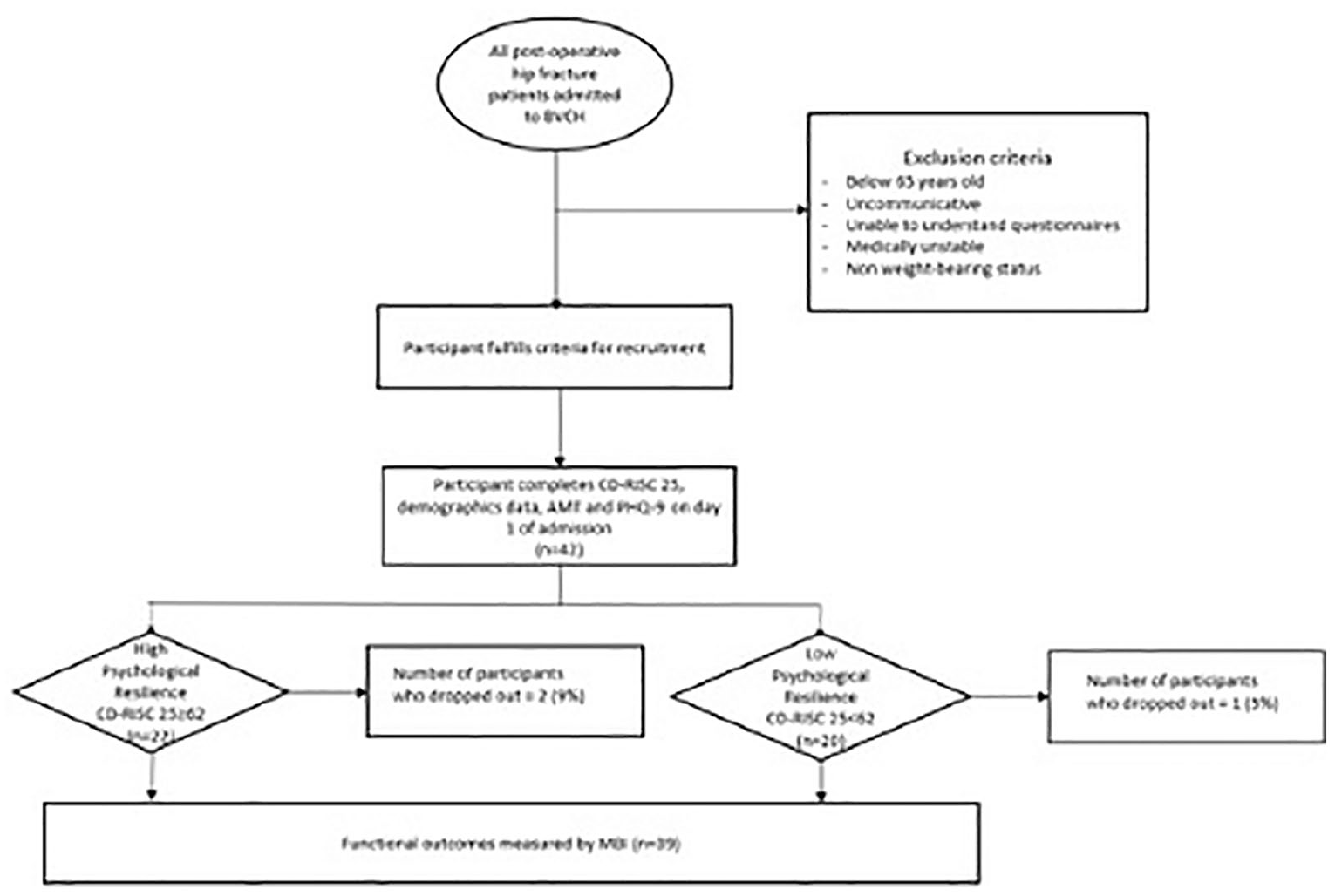
Participant recruitment and follow up.
Study design
On the first day of admission, we approached potential participants and invited them to participate in the study. If they agreed, written consent was obtained and their psychological resilience was measured using the Conner-Davidson Resilience Scale 25 (CD-RISC 25). We categorised participants into high psychological resilience if CD-RISC 25 score was ⩾62 or low psychological resilience if the score was < 62, based on the cutoff derived from a large community study of approximately 11,000 participants in Hong Kong.21,22
As part of the study, we also collected potential confounders of functional outcomes from our participant samples.23,24 These included social demographics data, presence of depression and cognitive impairment.
We then followed up these participants and measured their functional outcomes weekly for 21 days while they underwent rehabilitation.
Psychological resilience (CD-RISC 25)
We used the CD-RISC 25 to measure psychological resilience. The 25-item scale assesses psychological resilience with the following 5 factors:
Personal competence, high standards and tenacity
Trust in one’s instincts, tolerance of negative affect and strengthening effects of stress
Positive acceptance of change and secure relationships
Control
Spiritual influences
Each item is rated on a five point Likert scale ranging from 0–4: (0) not true at all, (1) rarely true, (2) sometimes true, (3) often true and (4) true nearly all of the time. These ratings result in a number between 0–100, with higher scores indicating higher psychological resilience.
There is currently no gold standard for psychological resilience scales, but a methodological review published by Windle et al. in 2011 showed that the CD-RISC 25 has one of the highest total quality assessment and psychometric ratings. 25 Although initially developed to assess resilience in post-traumatic stress disorder patients, the CD-RISC 25 has now been studied in various populations, including community dwelling populations, Asians and elderly populations. It is available in 77 languages, including English, Mandarin, Malay and Tamil, which are the 4 main languages used in Singapore. An extensive literature review revealed that most studies measuring psychological resilience use the CD-RISC 25.26–28 The CD-RISC 25 has shown good internal consistency (Cronbach α coefficient = 0.89), good test-retest reliability (r = 0.87, p < 0.01) and convergent validity with other measures of social support and hardiness. 29 Permission was obtained from the original authors of the scale prior to the start of the study.
Independent variables
We collected social demographic data such as the participant’s age, gender, race, marital status, living arrangement, type of housing, education level and presence of a caregiver.
We used the Patient Health Questionnaire-9 (PHQ-9) 30 to measure depression. The PHQ-9 is a 9-question instrument used to screen for the presence and severity of depression and is based on the diagnostic criteria of major depression from DSM-IV(31). Questions are about the level of interest in doing things, feeling down or depressed, difficulty with sleeping, energy levels, eating habits, self-perception, ability to concentrate, speed of functioning and thoughts of suicide. Responses range from 0–3: (0) not at all, (1) several days, (2) more than half of the days and (3) nearly every day. A score of 10 or more on the PHQ-9 has a sensitivity of 88% and a specificity of 88% in detecting major depressive disorder.32,33 Kroenke et al. conducted validity and reliability tests, and found a Cronbach’s alpha of 0.89 among 3000 primary care patients. The test-retest reliability was assessed by the correlation between PHQ-9 scores obtained from in-person and phone interviews with the same patients, and the correlation value obtained was 0.84. 32 In an assessment of construct validity, the correlation coefficient between the PHQ-9 and the SF-20 mental health scale was 0.73. 32
We used the Abbreviated Mental Test (AMT) 34 to measure cognition. The AMT is a 10-question instrument that is a screening tool for cognitive impairment. The questions include asking the participant about their age, date of birth, current location, current time, current year, home address, identifying two persons, the Prime Minister, counting backwards from 20 to 1 and a recall memory phase. A score of 7 or less on the AMT suggest cognitive impairment at the time of testing, with a sensitivity of 70–80% and a specificity of 71–90%.35,36
Functional outcomes
We used the Shah-Modified Barthel’s Index (MBI)37,38 to measure functional outcomes. MBI consists of 10 items describing basic activities of daily living and mobility. The values assigned to each item are based on the amount of physical assistance required to perform the task. A higher score indicates a higher level of independence in physical functioning. The total summation score ranges from 0 to 100, which corresponds to the following dependency levels: independent (100 points), minimal (91–99 points), mild (75–90 points), moderate (50–74 points), severe (25–49 points) and total dependency (0–24 points). Shah also came up with a prediction model for MBI scores: dependency in mobility and self-care (less than 40 points), moving from dependency to assisted independence (60–80 points), and functional independence (more than 85 points). The MBI has demonstrated high internal consistency (Cronbach’s alpha = 0.90) and test–retest reliability (correlation = 0.89), as well as high correlations (0.74–0.8) with other measures of physical disability, demonstrating convergent validity. 39 Most community hospitals in Singapore adopt MBI as their measurement of functional outcome, and this was a similar practice in our setting. 40
Statistical analysis
Baseline participant characteristics were presented as the number of participants (%) for categorical variables and mean (SD) for continuous variables. The change in mean MBI scores between participants with high psychological resilience and low psychological resilience were described and analysed using the independent t-test. The ability to achieve functional independence between the participants with high psychological resilience and low psychological resilience were described and analysed using Chi-square test. The p value < 0.05 was set to be statistically significant.
Data analysis was performed using SPSS version 24.0. This project was assessed and approved by the Singhealth Research Centralised Institutional Review Board (CIRB Ref: 2017/3144).
Results
Sample characteristics
Table 1 shows the baseline demographics of the participants and other variables that may influence functional outcomes. A total of 52.40% (n = 22) of the study population had high psychological resilience. The mean age of participants was 75.4 ± 6.20. The majority were female participants who were married, staying with their family in government subsided housing and had no dedicated caregiver on discharge. The participants with high psychological resilience were older (77.4 ± 5.80) compared with the participants with low psychological resilience (73.8 ± 5.70). There were more participants with low psychological resilience who stayed alone (30%, n = 6) compared with participants with high psychological resilience (13.63%, n = 3). Half of the participants with high psychological resilience received at least secondary school education (n = 11) compared with 35% (n = 7) of the participants with low psychological resilience. We did not find any statistically significant differences between the 2 groups with regards to the baseline demographics.
Characteristics of participants at baseline.

PHQ-9: Patient Health Questionnaire-9; AMT: Abbreviated Mental Test; MBI: Modified Barthel’s Index
Out of the psychometric scales, there was a statistically significant difference for PHQ-9 between participants with high psychological resilience versus those with low psychological resilience. A total of 20% (n = 4) of the participants with low psychological resilience had evidence of major depression, compared with none in those with high psychological resilience, and this difference was statistically significant (p =0.04). There were no statistically significant differences for AMT and baseline MBI scores between the two groups (p > 0.05). The length of stay in participants with high psychological resilience was shorter at 23.2 ± 7.00, as compared with 27.8 ± 15.60 in participants with low psychological resilience, but, as p = 0.23, this difference was most likely attributable to chance.
Objectives
Psychological resilience and mean MBI scores across different time points
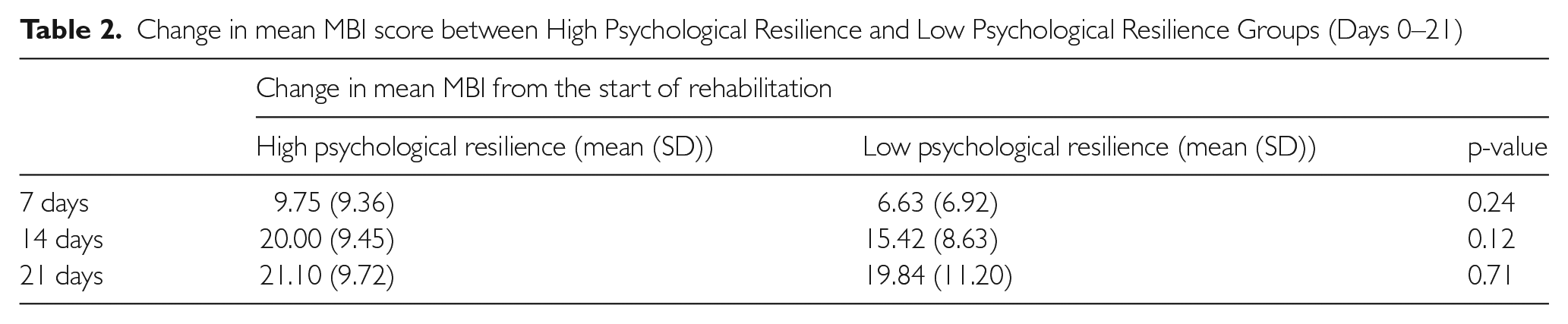
Figure 2 compares the mean MBI scores between the high psychological resilience and low psychological resilience groups. In both groups, as illustrated in Table 2, the largest gain in MBI was achieved in the first 2 weeks of stay, after which the rate of gain reduced by the third week of stay.

Mean MBI scores between high psychological resilience and low psychological resilience groups across the period of rehabilitation (days 0–21).
Change in mean MBI score between High Psychological Resilience and Low Psychological Resilience Groups (Days 0–21)
Psychological resilience and ability to achieve functional independence (MBI > 85)
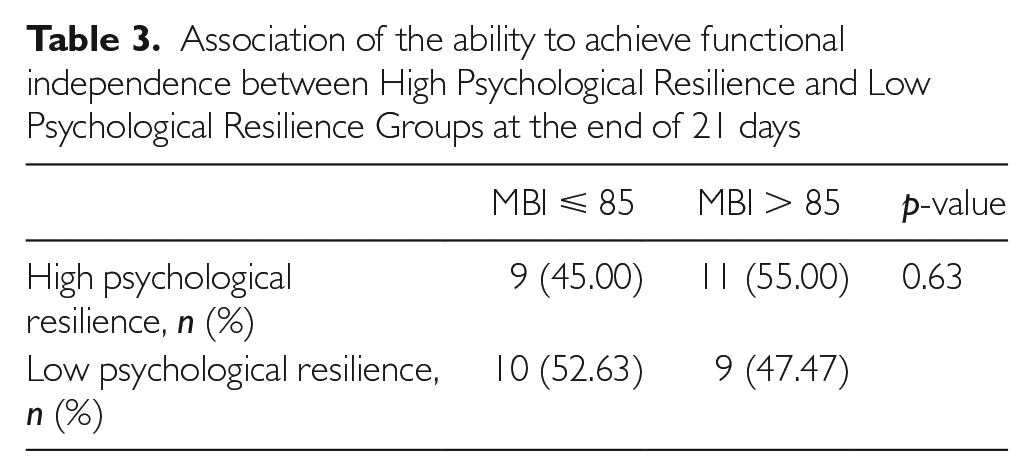
Figure 3 compares the number of participants who were able to achieve functional independence between the high psychological resilience and low psychological resilience groups. Out of the study participants, 47.62% achieved an MBI score of more than 85 in total (n = 20). From Table 3, 55% of the participants with high psychological resilience achieved functional independence (n = 11), compared with 47.47% of participants with low psychological resilience (n = 9), although this result did not achieve statistical significance.
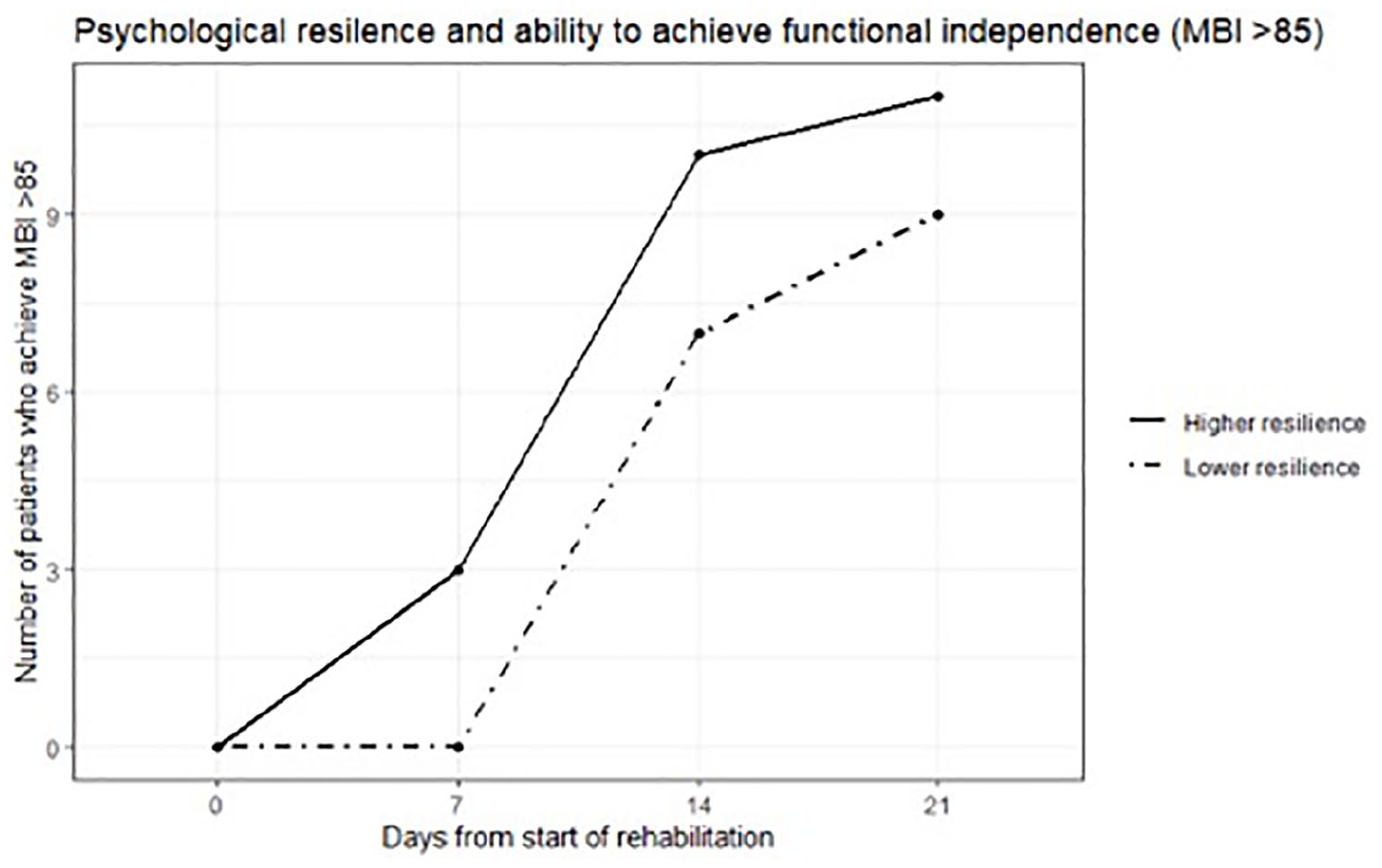
Achieving functional independence between high psychological resilience and low psychological resilience groups over 21 days (n = 20).
Association of the ability to achieve functional independence between High Psychological Resilience and Low Psychological Resilience Groups at the end of 21 days
Discussion
Using CD-RISC 25, we found that approximately one in two geriatric patients who had undergone surgery following a hip fracture in this study had high psychological resilience. This is higher compared with elderly populations from Western countries, where the prevalence ranged from 14–34%. 41 The difference in prevalence rates may be due to the differences in culture. In Asian countries like Singapore, the elderly are valued and respected for their life experiences, and this in turn may account for the higher prevalence rates of high psychological resilience as compared with the Western population, where ageism is common. 42
Resnick 43 showed that social support is positively correlated with improved functional outcomes in the elderly. In our study, there were more participants with low psychological resilience who stayed alone (30%, n = 6) compared with participants with high psychological resilience (14.3%, n = 3). We also found that there were more participants with low psychological resilience with evidence of major depression (20%, n = 4) as compared with none of the participants with high psychological resilience having evidence of major depression. This result was statistically significant (p = 0.04) and supports current literature that resilience is a protective factor against depression. 44
Participants with high psychological resilience were able to achieve a greater gain in MBI (21.10 ± 9.72) as compared with participants with low psychological resilience (19.84 ± 11.20). From Figure 2, it appears that there were more participants with high psychological resilience who were able to achieve functional independence (55%, n = 11) as compared with participants with low psychological resilience (47.4%, n = 9). These findings support this study’s hypothesis that high psychological resilience can lead to better functional outcomes in post-operative hip fracture patients as they are more likely to be motivated to participate in rehabilitation.
Aging adults may not have the capacity to improve psychological resilience on their own, hence a number of interventions have been proposed: mindfulness meditation to assist in positive coping, cognitive reframing to change negative perceptions and mastery development to enhance one’s sense of achievement.45,46 However, there is no one-size-fits-all, and strategies to boost one’s psychological resilience should be individualised. 47 In our local context, such interventions may be incorporated into programmes offered by day care centres or senior activity centres. Improved psychological resilience is associated with better health and well-being, and resilience levels do not decline with age. 48
The main limitation in our study was the challenge in recruiting participants due to the lack of health literacy among the elderly population in Singapore as the majority of the elderly in Singapore received only up to primary school education. 49 Health literacy is key in producing accurate information about a patient’s knowledge, attitudes and perceptions, but less educated patients face struggles filling out medical questionnaires. 50 This limitation was partially circumvented by using standardised interviewer administered language questionnaires in English, Mandarin, Malay or Tamil, but many were excluded due to their inability to understand the questionnaires.
Recommendations for future studies of a similar nature should consider testing for additional variables such as the presence of co-morbidities and baseline function prior to sustaining hip fractures as possible confounders of functional outcomes, and incorporating quality of life measures to understand the patient’s perspective about their health, as the MBI only accounts for physical functional outcomes.
Conclusion
We found that high psychological resilience is present in approximately half of post-operative hip fracture patients and, although the results did not achieve statistical significance, our pilot findings suggest that high psychological resilience does seem to correlate with higher gains in MBI scores and improves the ability to be functionally independent.
Footnotes
Acknowledgements
We would like to thank Lim Ka Keat for his assistance and guidance in this research.
Authors’ contributions
Low LL and Tan YFC conceptualised this study. Tan YFC performed the literature review, gained ethical approval and wrote the first draft of the manuscript. Fang HSA and Koh YLE were involved in data analysis. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
Availability of data and materials
The datasets generated and/or analysed during the current study are available from the first author Tan YFC.
Conflict of Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval
Ethical approval for this study was obtained from Singhealth Research Centralised Institutional Review Board (CIRB Ref: 2017/3144).
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article
