Abstract
Epidermal inclusion cysts (epidermoid cysts) occur from penetration of epidermal cells into underlying dermal tissue. They are most commonly found on the scalp, face, neck, and back with a reported incidence of 10% on the extremities. We present the case of a 53-year-old female who presented with complaint of a painful plantar forefoot soft-tissue mass of insidious origin. After magnetic resonance imaging, she was treated with surgical excision and plastic rotational flap closure. The surgical site healed without incident, and she was able to ambulate pain free in her normal footwear with full weight bearing and no shoe modifications or orthotics. This case was novel in that the size of the lesion required the use of a uni-lobe full-thickness rotational skin flap to achieve complete tension-free closure.
Introduction
Epidermal inclusion cysts (epidermoid cysts) occur from penetration of epidermal cells into underlying dermal tissue.1–6 They are most commonly found on the scalp, face, neck, and back with a reported incidence of 10% on the extremities. 4 They generally range in size from 0.2 to 5 cm and can be solitary or multiple masses. Epidermoid cysts are typically unilateral, although bilateral inclusion cysts have been reported, and they can be of traumatic or non-traumatic etiology.2,5,6 Iatrogenic causes occur in the setting of improper wound-edge eversion upon skin closure or if epidermal cells are driven into the wound during any surgical procedure. 2
After implantation into the dermis, epidermal cells can slowly grow, producing a lipid- and keratin-filled cystic cavity. Epidermoid cysts tend to be asymptomatic unless they enlarge enough to interfere with surrounding tissue, often adhering to nerves or eroding bone.1–3 If growth continues until the cyst ruptures, the released keratin is physiologically perceived as a foreign body, triggering a giant-cell reaction with subsequent formation of a keratotic granuloma of giant cells.1,2
Epidermoid cysts with or without giant-cell reaction will present with a nonspecific increase in soft-tissue density on plain-film radiographs. 5 If evidence of osseous involvement exists on plain-film computed tomography (CT) should be ordered for further evaluation; otherwise, magnetic resonance imaging (MRI) is more specific for soft-tissue masses and will typically reveal a semi-solid mass with several interspersed fluid-filled cavities.3,5 A benign epidermal inclusion cyst cannot be differentiated from a malignant transformation on CT or MRI, the incidence of which varies from 0.01% to 9.2%.2–6 The use of ultrasound, however, has been shown to differentiate between benign and malignant lesions. 6
First described by Wernher 7 in 1855, epidermal inclusion cysts have been generally noted to occur on the plantar-lateral aspect of the foot with peak incidence between the ages of 20 and 35.8 –10 Epidermal inclusion cysts are the fifth most common pedal soft-tissue lesion and account for 3.2% of all soft-tissue masses of the foot. 11 Although typically sporadic in nature, they have been noted to occur in patients with a family history of polyposis, fibrous tissue tumors, osteomatosis, and Gardner’s syndrome. 3
Epidermal inclusion cyst treatment requires complete excision, including the wall of the cyst. 2 The importance of removing the cyst without rupturing it must be emphasized. Rupture leads to a higher recurrence rate and increases the risk of setting off a giant-cell reaction. 1 Most important, the cells must be confined because of the possibility of malignant transformation. All soft-tissue masses removed should be sent to pathology to rule out malignancy.
Case report
The patient is a 53-year-old female with past medical history significant for non-insulin-dependent diabetes mellitus, diverticulosis, hypertension, gastroesophageal reflux disease, and generalized anxiety disorder. She was referred to the attending physician’s office (RCT) for evaluation of a painful plantar foot mass. The mass was insidious in onset and had been present for several years. The patient denied traumatic onset and insisted that she noticed a recent increase in size and pain affecting her ability to perform activities of daily living. Clinically there was an appreciable protrusion in the area of the plantar left third intermetatarsal space measuring 1.8 cm by 2.4 cm by 0.5 cm that was firm with palpation and painful to direct pressure (Figure 1).

Clinical preoperative imaging.
No osseous abnormalities were present on plain-film radiographs. An MRI of the left foot with and without contrast was obtained that showed a well-circumscribed dermal space soft-tissue mass along the plantar aspect of the left third intermetatarsal space immediately adjacent to the epidermal tissue. The mass measured approximately 2.4 cm in craniocaudal dimension, 1.7 cm in the transverse dimension, and 1.9 cm in the anteroposterior dimension. The lesion was isointense to muscle on the T1-weighted images and showed mild-to-moderate hyperintensity on the fluid-sensitive sequences.
After thorough discussion with the patient she elected to pursue surgical excision. Preoperative vascular studies were obtained and were within normal limits. The patient was subsequently evaluated by her primary care physician and was felt to be an acceptable surgical candidate with her most recent hemoglobin A1c being 6.0.
A circumferential incision was performed surrounding the mass with a greater than 6 mm margin (Figures 2 and 3). The lesion was contiguous with the skin as well as the subcutaneous tissue and adherent to the plantar fascia. There was a readily identifiable feeder arterial vessel into this lesion stemming from the plantar aspect that was ligated to maintain hemostasis.
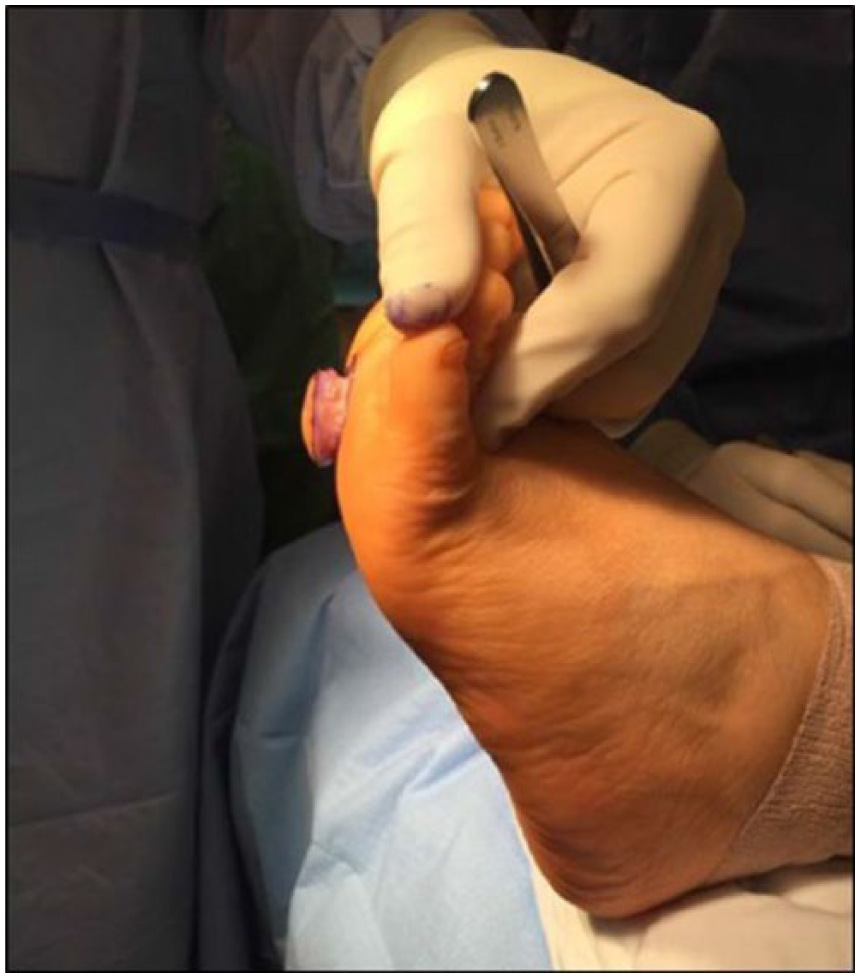
Lateral clinical intraoperative imaging.

Plantar clinical intraoperative imaging.
The distal extent of the third plantar common-digital nerve was transected as it branched into the digits distally. Proximally, the nerve was transected and the remnant was buried in the adjacent lumbricale muscle belly. The mass was meticulously dissected and excised in toto then passed to the back table. The specimen was well encapsulated with a violaceous hue and measured 2.4 cm in length, 2.1 cm in width, and 2.3 cm in depth (Figures 4 and 5). The mass was collected in formalin and sent to pathology for histopathological evaluation.

Excised mass posterior to anterior.
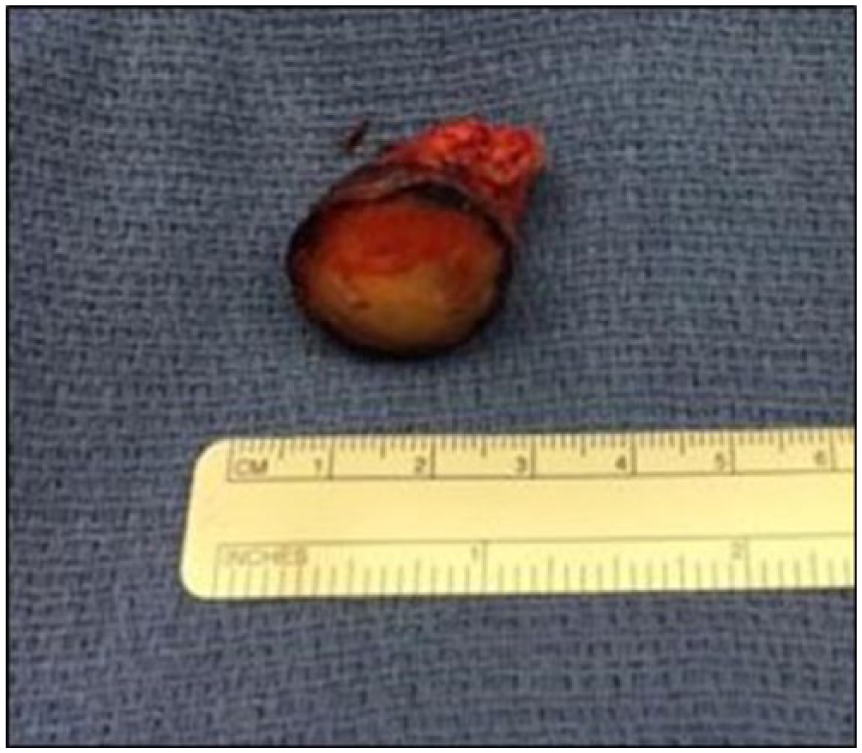
Excised mass anterior to posterior.
The decision was made to perform a local single-lobe rotational skin flap to allow for primary closure of the surgical site (Figure 3). An incision was extended from the medial aspect of the soft-tissue void and curved back an equal distance from the wound. Adjacent soft tissue was undermined and freed to the level of the subcutaneous tissue plane. Care was taken to maintain a 90-degree angle at the base of the flap to allow easier transposition and reduce dog-ear formation. The flap was then rotated into the void at the surgical excision site taking care not to overly tension the pedicle. The skin was pliable enough to allow for primary closure using a nylon suture (Figure 6). Vascular status remained intact to the flap site.

Immediate clinical postoperative imaging.
The patient was discharged to home per post-anesthesia care unit protocol. She was given prescriptions for oral antibiotics, opioids, and venous thromboembolism prophylaxis. The pathology report was obtained from the operative specimen and confirmed the diagnosis of epidermal inclusion cyst with giant-cell reaction.
She remained strictly non-weight bearing on the left foot for a total of six weeks. Sutures were removed postoperative week 2 and capillary fill time remained immediate to the full thickness rotational flap. No signs of clinical infection were appreciated, and the soft tissue healed without incident. At postoperative week 6 she progressed to full protected weight bearing in a controlled ankle motion boot. Then, at postoperative week 10, the patient was progressed to full unrestricted weight bearing in her normal footwear.
The patient was followed postoperatively at weeks 1, 2, 6, and 10 with her final postoperative appointment being greater than12 months from the procedure. The surgical site showed no signs of a recurring lesion and she was able to ambulate pain free in her normal footwear with no shoe modifications or orthotics (Figure 7). She has had no activity restrictions or signs of recurrence and remains pleased with the outcome.
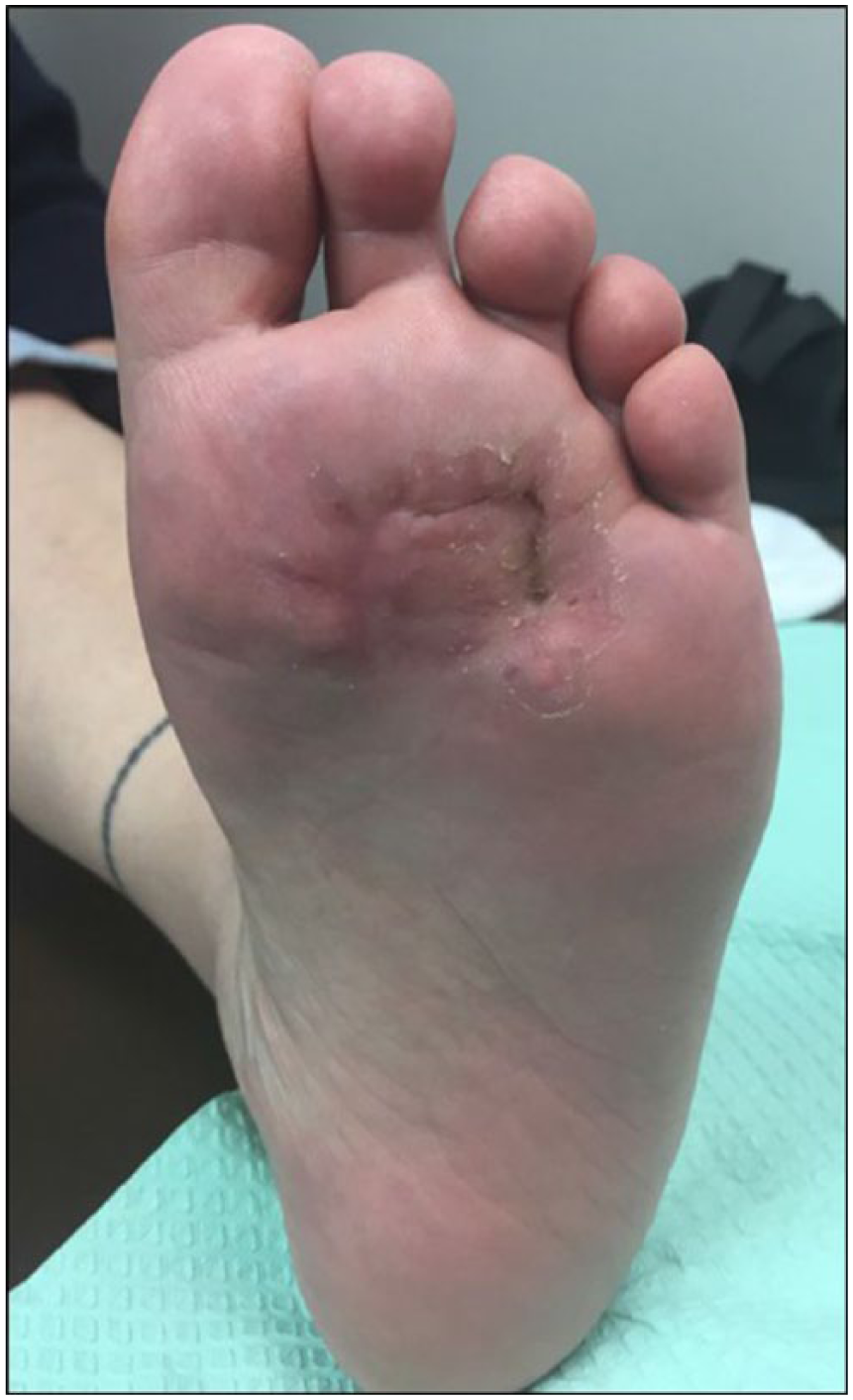
Clinical imaging at final postoperative follow-up.
Discussion
With the cyst presented above, repeated trauma from daily ambulation led to rupture into the adjacent soft tissue that elicited significant inflammation and the formation of foreign-body giant cells. In this case the lesion grew so it completely encompassed the third common digital nerve as well as its distal branches requiring complete excision of the nerve in order to remove the lesion in its entirety. This case was novel in that the size of the lesion required the use of a uni-lobe full-thickness rotational skin flap to achieve complete tension-free closure. A vacuum-assisted dressing may have been an option in treating the soft-tissue deficit in lieu of the single-stage flap closure; however, given the extent and depth of the tissue excised, this would likely have resulted in prolonged exposure of deep-tissue structures and a significant delay in returning to full weight bearing and presurgical levels of activity.
The proximity of the cyst to the superficial tissue required circumferential excision, including the overlying epidermal tissue, to avoid potential iatrogenic rupture and maintain appropriate excisional margins. The resulting tissue deficit to the plantar midfoot was felt to be too large to accommodate a direct fusiform (3–4:1) closure typically reserved for smaller superficial lesions in regions with appropriate soft-tissue mobility and elasticity. 11 A variety of techniques have been described for closure of plantar foot wounds including fusiform closure, uni-lobe or bi-lobe flaps, and rhomboid flaps. Diabetic plantar foot wounds have been shown to respond well to uni-lobe rotational flap closure in treatment of chronic wounds and ulcerations.12,13
In this case a Schrudde’s type 1 uni-lobe rotational skin flap was performed. The technique was described by Dockery and is suggested for closure of plantar foot circular defects. 14 Saipoor et al. performed a retrospective audit of the literature showing the technique to be an effective and safe single-stage procedure to achieve closure of excised plantar foot lesions. 15
Although largely benign, epidermal inclusion cysts with potential for subsequent giant-cell reaction must remain a part of an exhaustive differential diagnosis in the evaluation of plantar foot soft-tissue masses. These lesions can be successfully treated with single-stage primary excision and rotational flap closure as demonstrated in this case.
Footnotes
Declaration of conflicting interest
None declared.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
