Abstract
Objectives:
High body mass index (BMI) has been associated with increased mortality, healthcare utilization and costs. This study investigates the one-year chronic disease progression and risk of developing diabetes with varying cardiovascular disease (CVD) risks based on the Asian BMI categories.
Methods:
Patients with BMI information from 2008 to 2014 were included in the analysis (N=23,508). Patients were stratified into low, moderate, high and very high CVD risk categories. To study disease progression for patients with varying CVD risks, patients were further segmented into seven mutually exclusive disease states based on prevalence of chronic diseases and their complications. The categories were no known chronic disease, at-risk of developing chronic disease, one chronic condition, more than two chronic conditions, chronic conditions with complications, patients with cancer and death. Logistic regression was used to determine the association of CVD risk categories and risk of having diabetes.
Results:
High CVD risk patients had more chronic diseases in the following year as compared with low CVD risk patients. With reference to low CVD risk patients, patients in the moderate, high and very high risk categories had an odds ratio of 1.78 (95% confidence interval (CI): 1.60 to 1.98), 2.84 (95% CI: 2.51 to 3.21) and 3.99 (95% CI: 3.30 to 4.82) for having diabetes after adjusting for age, gender and ethnicity.
Conclusions:
Higher BMI is associated with greater chronic disease progression in the following year. Diet control and lifestyle modifications should be encouraged to prevent people from shifting to higher BMI strata as this can be detrimental in the long run.
Introduction
The Global Burden of Disease Study estimated an increase in worldwide proportions of overweight and obese individuals by 27.5% between 1980 and 2013. 1 Previously considered an epidemic of developed countries, in recent years the growing burden of obesity has affected most regions, including Southeast (SE) Asia. 2 The high prevalence of obesity is particularly concerning as it is an established risk factor for many chronic conditions such as cardiovascular diseases, type 2 diabetes mellitus, certain types of cancers and increased risk of all-cause mortality. 3
Body mass index (BMI), defined as a person’s weight in kilograms divided by the square of their height in meters, is a common clinical measure to classify overweight and obesity. The World Health Organization (WHO) has provided the following BMI categories as a measure of relative body weight: <16.0 kg/m2 (severe underweight), 16.0–16.9 kg/m2 (moderate underweight), 17.0–18.49 kg/m2 (mild underweight), 18.5–24.9 kg/m2 (normal range), ⩾25.0 (overweight), 25.0–29.9 kg/m2 (pre-obese), ⩾30.0 kg/m2 (obesity). The relationship between body fat percentage and BMI is not only age- and gender-specific but also dependent on ethnicity.4,5 Evidence from published studies found that Asian populations have higher body fat percentages at lower BMI values as compared with Western cohorts.6–8 For example, Indonesians are found to have higher body fat percentage compared with Caucasians with the same BMI values. 7 Accounting for ethnic differences, the WHO established lower BMI thresholds specific to Asian populations. These Asian BMI cut-offs correspond to risk categories for cardiovascular diseases (CVDs): <18.5–23.0 kg/m2 (low risk); 23.0–27.5 kg/m2 (moderate risk); 27.5–32.4 kg/m2 (high risk) and ⩾32.5 kg/m2 (very high risk). 6
A 2010 Singapore National Health Survey reported that one in nine residents were obese (BMI ⩾30.0 kg/m2). 9 Based on the Asian BMI risk categories, 23% of those who responded were at high risk of developing CVDs (BMI⩾ 27.5 kg/m2). The higher prevalence of obesity in Singapore seems to mirror a relatively high burden of obesity-related chronic diseases. In addition, the fact that increasing BMI levels is also associated with an elevated risk of developing CVD complications in Singapore, 10 more emphasis must be put on preventive strategies to reduce the prevalence of obesity.
Developed by Lynn and colleagues, the ‘Bridges to Health’ model is a patient segmentation framework that categorizes the population into eight distinct groups ranging from healthy to long-term frailty. 11 Segmenting the population into relatively homogenous, distinct subgroups based on their healthcare needs or clinical characteristics enables healthcare providers to better understand the profiles of various subgroups within a population, optimize healthcare services and allow for more efficient resource allocation. This study aims to (1) investigate the one-year chronic disease progression and (2) to determine the independent effects of CVD risk categories and risk of having diabetes, by stratifying patients living in central region Singapore into the CVD risk categories based on Asian BMI.
Methods
Data for this study was taken from the Regional Health Systems (RHS) database. Briefly, the RHS database is a conglomeration of four isolated databases from three RHSs in Singapore that contains National Healthcare Group polyclinic (NHGP) visit records, specialist outpatient clinic visit records, hospital discharges records, chronic disease management system records and mortality records obtained from national registries.12,13 A detailed report about the setup of this database can be found in previous publications.12,13 Briefly, data on height and weight for patients with complete information for seven consecutive years (2008–2014) was taken and BMI was computed (weight/height 2 ). Chronic disease information and patient demographics were determined from the RHS database. All patients belonged to the central region of Singapore (defined by Ministry of Health as nine Development Guide Plan areas: Ang Mo Kio, Bishan, Geylang, Hougang, Kallang, Novena, Rochor, Serangoon, Toa Payoh). Patients who were included in the analysis were Singaporean or permanent resident, living in central region Singapore, at least 18 years of age, having Chinese, Malay or Indian ethnicity, with at least one visit to Tan Tock Seng Hospital and/or one of the nine National Healthcare Group polyclinics (NHGPs) in 2008 and have BMI data recorded during 2008–2014. All patients were alive as of 31 December 2014.
Patients were stratified in two phases. Patients were first segmented into CVD risk categories based on Asian BMI cut-offs. The categories were:
(a) Low risk (BMI of 18.0 kg/m2 to 22.9 kg/m2)
(b) Moderate risk (BMI of 23.0 kg/m2 to 27.4 kg/m2)
(c) High risk (BMI of 27.5 kg/m2 to 32.4 kg/m2)
(d) Very high risk (BMI of 32.5 kg/m2 and above).
In order to study the disease progression of patients with different BMI risk categories, patients were then further segmented into mutually exclusive disease states based on prevalence of chronic disease and their complications. Figure 1 illustrates how patients were segmented into seven groups, in increasing order of disease severity for each CVD risk category. This patient segmentation model is a reflection of the spectrum of diabetes. Pre-diabetes or obese patients are categorized into the at-risk group. Patients diagnosed with diabetes are categorized into one or more than two chronic diseases, depending on the patient’s multimorbidity status. If diabetes patients are poorly managed, their conditions will deteriorate faster and complications will develop along the way. Some patients may then progress to death. To determine the proportion of patients that develop cancer, the patient segmentation model included a category ‘patient with cancer’. Based on BMI and chronic disease data collected from 2008 to 2014, a one-year transition matrix using Markov modeling was performed to quantify the probability of patients’ progression from one risk group to another. 14 The transition matrix is an upper diagonal matrix, which is consistent with the one-way progression assumption. The percentages in each cell represent the conditional probability of staying or progressing from one group (row) to another group (column) after one year.

Patient segmentation model.
Descriptive analysis was used to report baseline characteristics of patients. The independent effects of the CVD risk categories on predicting risk of having diabetes was assessed using a logistic regression model via the backward stepwise method. A p value of 0.2 was considered significant for inclusion into the multivariate model. The final model level of significance was set at 0.05. Most of the analyses were conducted using STATA (StataCorp, College Station, TX, USA) statistical software, version 12.0. The one-year transition matrix was developed using R statistical program. The study was approved by the National Healthcare Group’s Domain-specific Ethics Review Board, which is an independent committee comprising medical, scientific and non-scientific members.
Results
Patient demographics
Patients with complete information on height and weight for seven consecutive years from 2008 to 2014 were included for analysis (N=23,508). The average yearly BMI was taken for each patient during the seven years. The proportion of patients having low CVD risk remained stable during the seven-year period (29.5% in 2008 to 29.3% in 2014). There was a slight drop in the proportion of patients in the moderate CVD risk category (44.7% in 2008 to 42.9% in 2014). The proportion of patients with high CVD risk increased from 20.3% in 2008 to 21.3% in 2014 and the proportion of patients with very high CVD risk increased from 5.6% in 2008 to 6.5% in 2014. Table 1 shows the demographics of the patients in the year 2014.
Patient demographics in 2014.
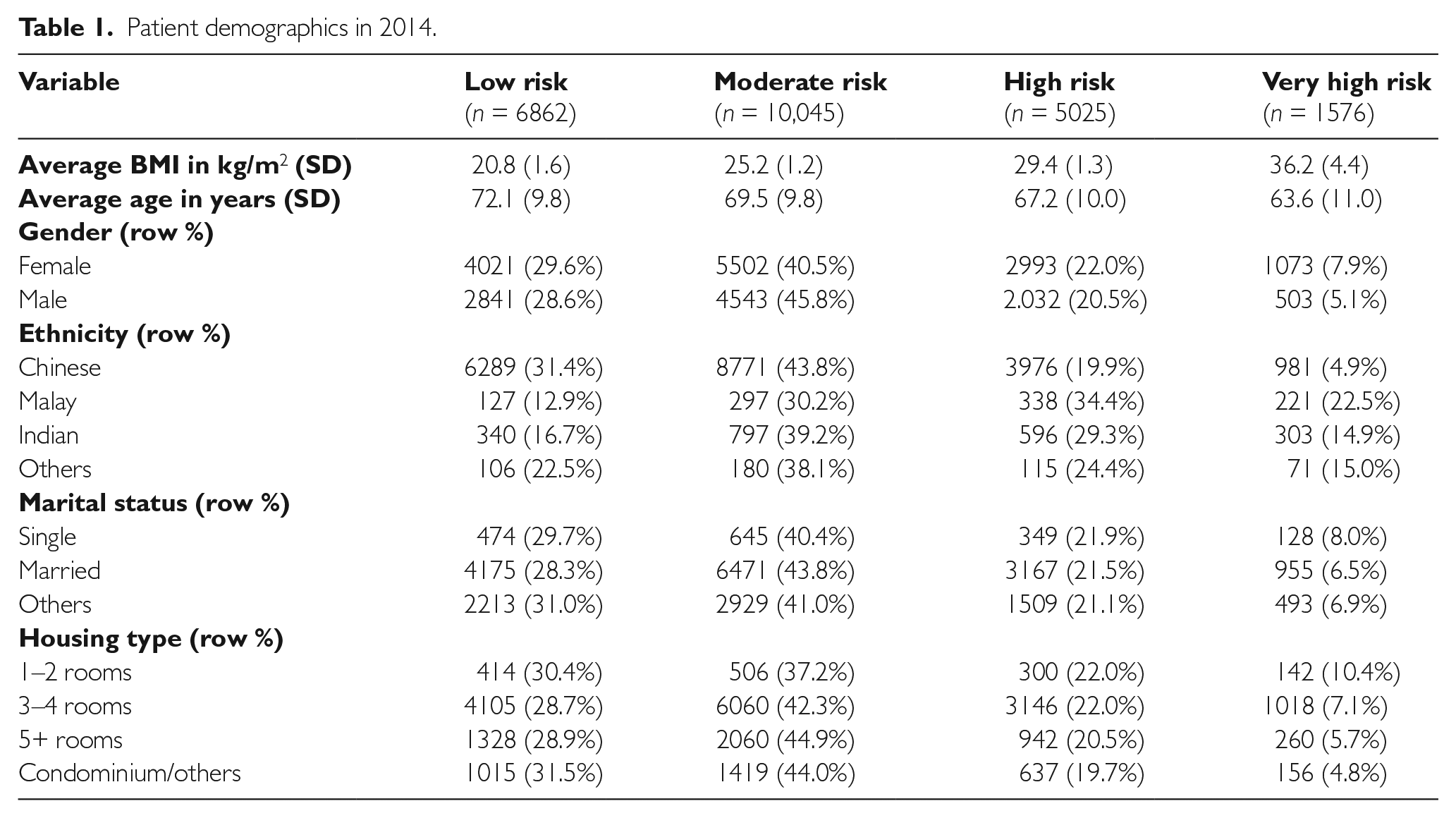
For patients categorized as moderate or high risk of CVD, the highest proportion of Indians and Malays were aged 55–64 years while the highest proportion of Chinese belonged to the 65–74 years age category. For patients with very high risk of CVD, the highest proportion of patients were seen in the 55–64 years age category for each ethnic group. Over the seven-year period, prevalence of chronic diseases increased, with nearly all patients developing hypertension and dyslipidemia in 2014 compared with 2008 irrespective of their initial CVD risk category (Figure 2).
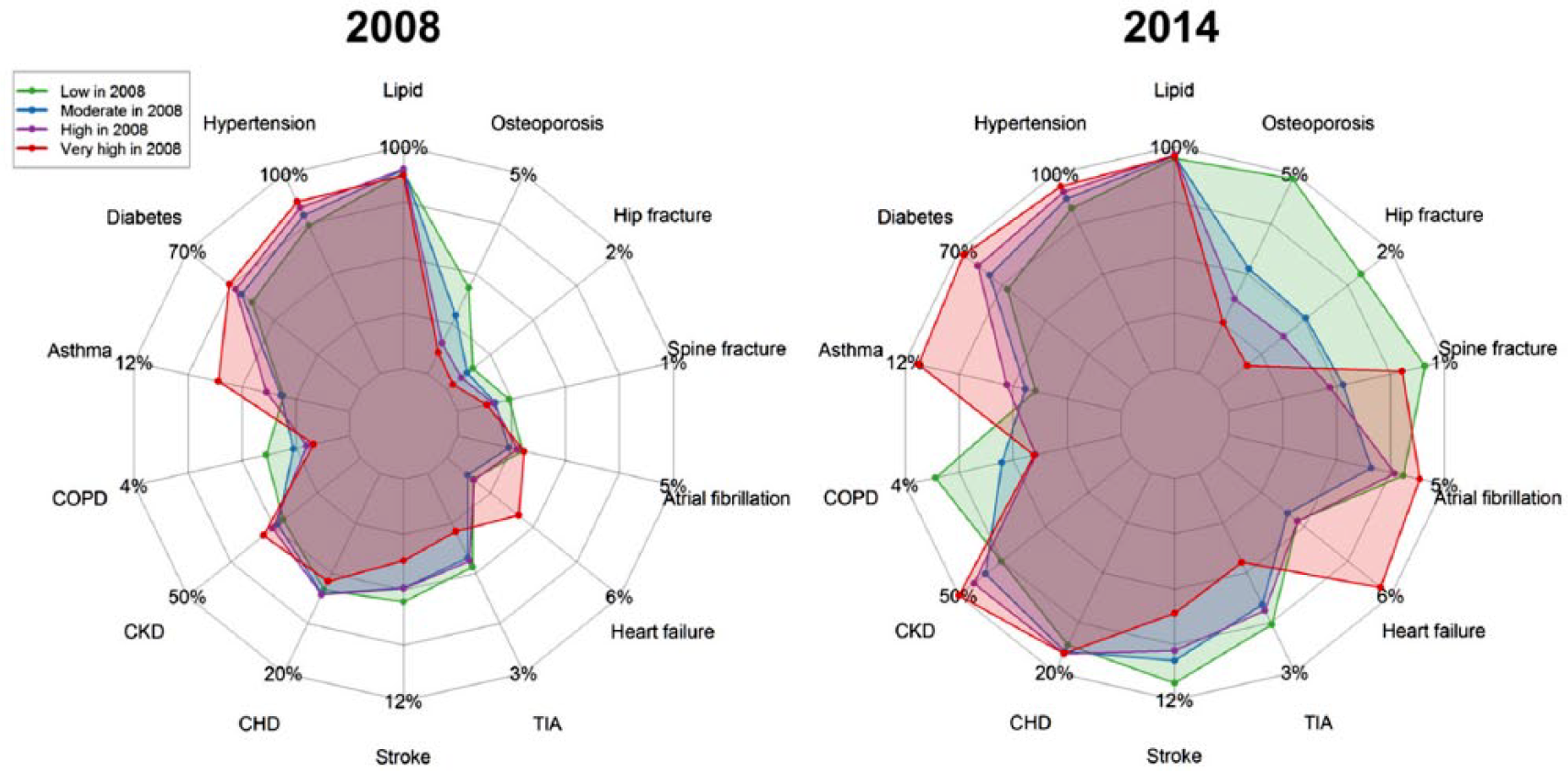
Prevalence of chronic diseases in 2008 and 2014 by initial (2008) cardiovascular disease risk categories.
Disease progression by CVD risk categories
Table 2(a)–(d) shows how patients with different initial CVD risk progress to different categories of disease states in the following year. Patients who had cancer or died were excluded from the transition matrix as there would be no further progression in the following year. It is observed that the majority of the patients stayed in the same group as the previous year. There were also patients who progressed across more than one group within a year. Among patients in the low CVD risk category, 55% of the patients remained in the ‘no known chronic’ group after one year of follow up. The remaining 45% progressed to either ‘at-risk’ (13%), developed one chronic disease (27%), developed two or more chronic diseases (1%), were diagnosed with chronic disease with complications (3%) or developed cancer (2%). With increasing BMI, the risk of disease progression increased. Comparing the ‘at-risk’ groups for the four CVD risk categories, 13%, 20%, 27% and 28% progressed to the next stage (excluding cancer). Similar trends were seen with the other disease states.
Progression of patients to different disease states by CVD risk categories.
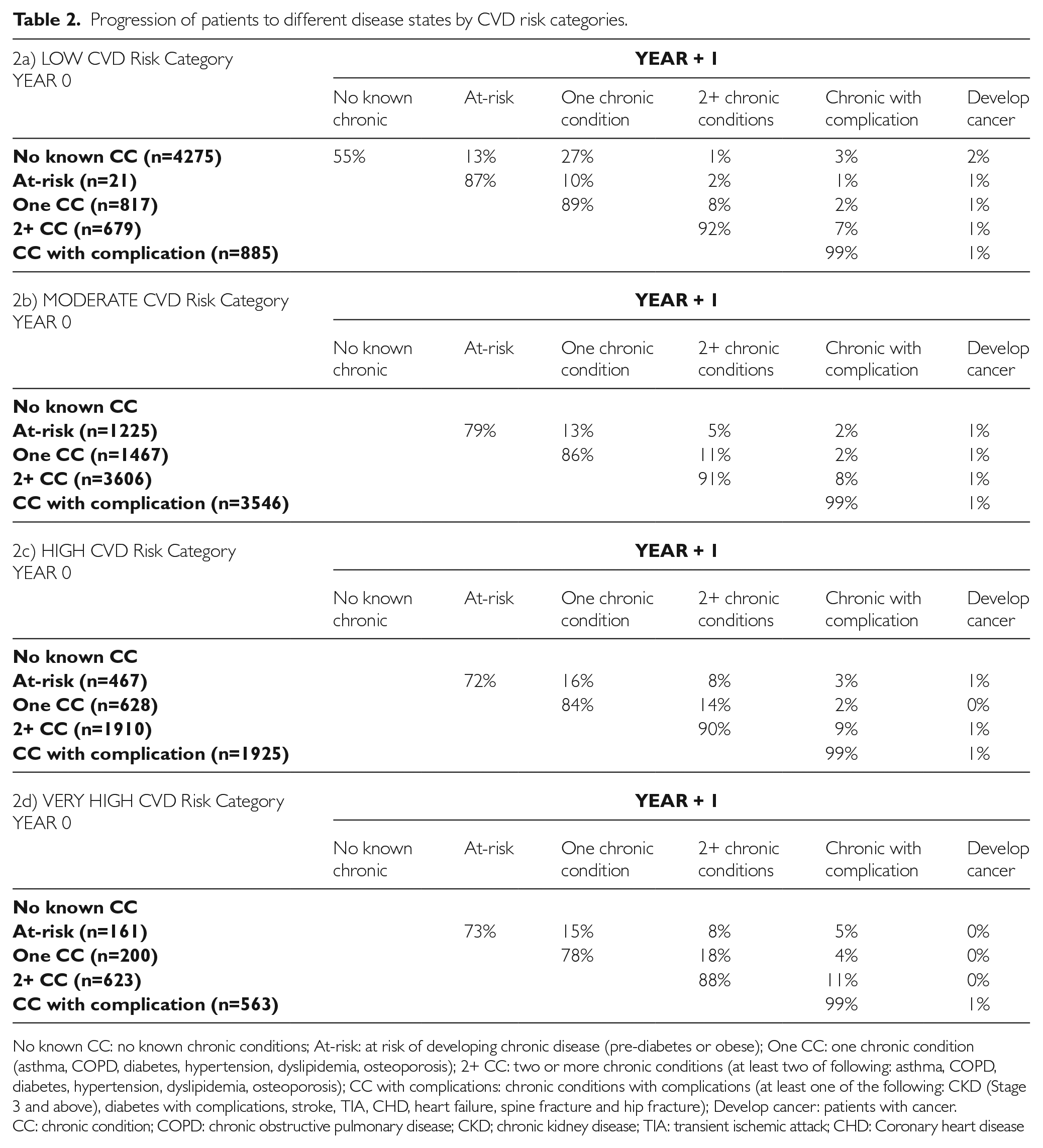
No known CC: no known chronic conditions; At-risk: at risk of developing chronic disease (pre-diabetes or obese); One CC: one chronic condition (asthma, COPD, diabetes, hypertension, dyslipidemia, osteoporosis); 2+ CC: two or more chronic conditions (at least two of following: asthma, COPD, diabetes, hypertension, dyslipidemia, osteoporosis); CC with complications: chronic conditions with complications (at least one of the following: CKD (Stage 3 and above), diabetes with complications, stroke, TIA, CHD, heart failure, spine fracture and hip fracture); Develop cancer: patients with cancer.
CC: chronic condition; COPD: chronic obstructive pulmonary disease; CKD; chronic kidney disease; TIA: transient ischemic attack; CHD: Coronary heart disease
Association of CVD risk categories and diabetes
After adjusting for age, gender and ethnicity the risk of having diabetes increased with progressively higher CVD risk categories (Table 3). With reference to the low CVD risk category, patients in the moderate, high and very high risk categories had an odds ratio of 1.78 (95% confidence interval (CI): 1.60 to 1.98), 2.84 (95% CI: 2.51 to 3.21) and 3.99 (95% CI: 3.30 to 4.82) for diabetes (Table 3).
Risk of diabetes with increasing CVD risk categories a .

Model was adjusted for age, ethnicity and gender. Only significant variables were reported.
BMI: body mass index; CVD: cardiovascular disease; ref.: reference.
Discussion
This study investigated chronic disease progression and the risk of developing diabetes among patients with varying CVD risks based on the Asian BMI. The one-year transition matrix for each CVD risk category has shown significant disease progression, with higher CVD risk patients having more chronic diseases in the following year as compared with patients in the low CVD risk category. With increasing BMI, the odds of developing diabetes increased in a dose–response relationship.
Findings from this study corroborate national and global studies on BMI and morbidity trends. Adjusting for age, gender, duration of diabetes and exercise status, Singaporean Chinese had the lowest mean BMI (24.9 kg/m2), followed by Indians (25.7 kg/m2) and Malays (27.4 kg/m2). In the current analysis, it was noted that with increasing BMI, the proportion of patients developing one or more chronic diseases or chronic diseases with complications increased in the following year with the exception of cancer. As BMI increased, the risk of developing diabetes increased. The odds of patients at very high risk of CVD (BMI ⩾32.5 kg/m2) developing diabetes were 3.99 times more as compared with low CVD risk patients, suggesting that CVD risk categories are predictors for diabetes. Excess body fat accumulation is frequently associated with metabolic abnormalities. 15 Longitudinal trend studies demonstrated that the increase in the prevalence of overweight and obesity is often accompanied with an increase in the prevalence of obesity-related chronic diseases.16–18 Based on the cross-sectional National Health and Nutrition Examination Surveys, there was an increase in the prevalence of obese adults from 30.1% in 1999 to 34.3% in 2010. 16 The prevalence of cardiovascular risk factors such as diabetes, hypertension and dyslipidemia was the highest amongst the obese adults, followed by overweight and normal adults. 16 Empirical evidence from large pooled studies has consistently shown positive associations between elevated BMI and risk of diabetes, CVD and all-cause death.19–21 A meta-analysis that evaluated the association of elevated BMI and incidence of 18 comorbidities from 89 studies reported that overweight and obesity were significantly associated with the incidence of type 2 diabetes, most cancers, all CVD (except congestive heart failure in overweight individuals), asthma, gallbladder disease, osteoarthritis and chronic back pain as compared with normal weight individuals, thus suggesting a direct association between increasing BMI and risk of developing comorbidities. 19 The strongest association was found between unhealthy BMI levels and incidence of type 2 diabetes, where, when compared with normal weight individuals, the pooled relative risk (RR) for overweight males and females and incident type 2 diabetes was RR 2.40 (95% CI: 2.12 to 2.72) and RR 3.92 (95% CI: 3.10 to 4.97) respectively, while obese male and females were RR 6.74 (95% CI: 5.55 to 8.19) and RR 12.41 (95% CI: 9.03 to 17.06) respectively. 19
In this study, Indian ethnicity had 44% higher risk of developing diabetes as compared with Chinese ethnicity, while the male gender had 15% higher risk of developing diabetes as compared with females. The 2010 Singapore National Healthy Survey reported that a higher proportion of males were diabetic as compared with females. 9 Prevalence of diabetes was highest in Indians (17.2%) compared with Malays (16.6%) and Chinese (9.7%). 9 Global studies have established ethnic differences in the risk of developing type 2 diabetes. Asian Indians have a higher prevalence of type 2 diabetes as compared with other ethnic groups.9,22,23 Empirical evidence from a multiethnic cohort reported that ethnic differences persisted in the prevalence of diabetes despite stratification by BMI. 24 Varying lifestyle factors such as nutritional intake, physical activity and genetic differences may result in differential risks in developing diabetes amongst different ethnic groups. 23 Globally, more males are diagnosed with type 2 diabetes. 25 Reasons for this phenomenon include smoking rates, fat distribution and diet.26–28 Visceral fat mass is strongly associated with diabetes.28,29 Males have higher visceral fat and hepatic fat as compared with females. 30 Females, on the other hand, tend to have higher peripheral fat distribution.26,30 Females may need to accumulate greater total adiposity in order to develop harmful fat deposits that will result in insulin resistance.26,30 Prevention strategies should be tailored to risk factors specific to each ethnicity and gender in Singapore.
This study is not one without limitations. A simple anthropometric measure of total adiposity such as the BMI is limited in its ability to discriminate elevated body weight due to lean or body fat mass, thus reducing accuracy in predicting cardiovascular mortality. 31 Methods to assess obesity can be refined to include measures of central adiposity such as waist circumference and waist–hip ratio to accurately predict cardiovascular mortality. 32 The RHS database pools patient utilization and chronic disease information from nine public primary care and three acute hospitals, capturing information for more than 50% of the Singapore population. Due to the administrative nature of the RHS database, the data pooled is limited. Detailed information of other known risk factors such as smoking status and socioeconomic factors were not captured and therefore not included in the logistic regression model as potential confounders.
Maintaining weight loss long-term may be a challenge due to obesogenic environments and biological mechanisms.33,34 Varying BMI trajectories from adolescence into adulthood may differentially associate with adult morbidity. A recent systematic review which analyzed 37 cohorts worldwide reported that elevated BMI amongst children aged 12 to 18 years was associated with an increased incidence of adult diabetes (OR 1.70; 95% CI: 1.30 to 2.22), coronary heart disease (OR 1.20; 95% CI: 1.10 to 1.31) and certain cancers. 35 Achieving and maintaining a healthy weight should be actively promoted from early childhood and throughout an individual’s lifetime. Prevention of excessive weight gain can have a significant impact in reducing the burden of obesity-related diseases and should be applied to individuals of all ages with varying BMI.
Conclusion
In Singapore, excessive weight prevention and weight maintenance must be prioritized given that with higher BMI, the risk of developing chronic diseases and disease progression increases. An ecological approach is fundamental to reversing the consequences of obesity. Targeted public health strategies and political commitment aimed at addressing root causes on a societal level will likely reduce the prevalence of overweight and obesity as well as its related diseases, resulting in a healthier and more productive population and reduced stress on the healthcare system.
Footnotes
Acknowledgements
We are thankful to the staff of the Department of Health Services and Outcomes Research, National Healthcare Group, Singapore for their contributions in providing the data and valuable inputs to this study.
Availability of data and materials
No additional data available.
Authors’ contributions
Zhu Zhecheng designed the study and conducted the data analysis. Palvinder Kaur and Nakul Saxena wrote up the manuscript with inputs from Zhu Zhecheng. All authors read and amended the manuscript and all authors vetted the final version of the manuscript.
Conflict of interest
The authors declare that there is no conflict of interest.
Informed consent
No informed consent was required as this is a database study.
Ethical approval
Ethical approval to report these cases was obtained from The National Healthcare Group Doman Specific Review Board (RHS DSRB: 2013/00505).
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
