Abstract
Aim:
Admission to an acute care geriatric unit may lead to adverse outcomes. It is therefore important to identify high-risk patients early so that appropriate management can be instituted to prevent or delay onset of adverse events. The aim of this study is to evaluate one-year mortality and its associated risk factors among hospitalized patients.
Methods:
This is a retrospective cohort study on consecutive patients admitted to an acute geriatric ward in a Singapore hospital from March to April 2013.Demographic and clinical information was collected from patient medical records. Linkage with death records from a national registry was performed.
Results:
Of the 196 patients assessed, 4.6%, 20.9% and 35.7% died during admission, within six months post-admission and within one year post-admission respectively. Pneumonia and cardiovascular diseases accounted for most of the death cases. In the multivariable logistic regression adjusted by age and gender, abbreviated mental test (AMT) score, admission for falls and depression were found to be significantly associated with death within one year post-admission. In the analysis stratified by gender, AMT score and depression were found to be significantly associated with death in males whereas AMT score and admission for falls were significantly associated with death in females.
Conclusions:
This study offers significant insight into mortality trends and risk factors for clinicians, hence guiding them in individualizing their management plan for acutely ill geriatric patients. Predicting long-term prognosis will enhance rehabilitation goal-setting and advance care-planning.
Keywords
Introduction
The population of Singapore is ageing rapidly resulting in increased consumption of healthcare resources. Among Singapore residents, the proportion of those aged 65 years and above has increased from 6.0% in 1990 to 11.8% in 2015. 1 In tandem with the ageing population, the proportion of elderly patients who were admitted to hospitals has grown from 28.1% in 2012 to 29.8% in 2014 for males and from 26.8% in 2012 to 28.7% in 2014 for females. 2 For many elderly patients, hospitalization in an acute care geriatric unit is a major episode in their clinical evolution, leading to adverse outcomes such as prolonged length of stay, functional decline, readmissions and even death. It is important for clinicians to identify high-risk patients early so that appropriate management can be instituted to prevent or delay the onset of the adverse events. Furthermore, a better understanding of the prognosis of the elderly patients would guide clinicians in providing individualized management and initiating advance care-planning for them during the course of hospitalization.
A myriad risk factors on mortality in elderly hospitalized patients have been identified. These include age, gender, functional status, cognition, polypharmacy and depression. 3 These risk factors have been studied extensively in Western countries but little is known of their actual contribution to mortality rates in Asia. The objective of this study was to evaluate one-year mortality and its associated risk factors among patients admitted to an acute geriatric ward in a Singapore hospital.
Method
Study population
Changi General Hospital (CGH) is a tertiary public hospital providing a comprehensive range of healthcare services for the community in the Eastern region of Singapore. We performed a retrospective cohort study on consecutive patients admitted to geriatric acute care wards in CGH over a six-week period from 4 March 2013 to 12 April 2013. Ethics approval was obtained from the Singapore Health Services Institutional Review Board. Informed verbal consent was obtained from 196 patients or their authorized representatives for those who lacked mental capacity to consent. Twelve patients did not participate due to refusal or because they rapidly demised within one day of admission. All patients or their authorized representatives were given an information sheet.
Data collection
We collected demographic and clinical information from the patient medical records. Premorbid 20-point Barthel index and Abbreviated Mental Test (AMT) scores were derived from a standardized comprehensive geriatric assessment performed on admission. A detailed falls history, including history of admission for falls, was also recorded. Linkage with the records from the Singapore Registry of Births and Deaths was performed to obtain outcomes on mortality. 4
Statistical analysis
We studied the differences in patient characteristics among patients who died and survived within one year post-admission using the Chi-Square test or Fisher’s exact test for categorical variables; independent samples
Results
Of the 196 patients assessed, 4.6%, 20.9% and 35.7% died during admission, within six months post-admission and within one year post-admission respectively. The baseline characteristics were as follows: mean age 86.6 ± 5.9 years; 68.4% females; 76.9% Chinese; 19.5% Malays; 2.1% Indians; mean BMI 20.5 ± 5.1 kg/m2; mean AMT score 3.4 ± 3.4; mean Barthel score 10.3 ± 7.3; 13.4% on tube feeding; 13.0% admitted from nursing home; 35.2% admitted previously for falls; 45.4% with dementia; and 20.4% with depression. Patients who died within one year post-admission tended to be older, had lower AMT and Barthel scores, on tube feeding and were admitted from nursing homes (

The causes of death at one year post-admission are shown in Table 2. Pneumonia (40.0%) and cardiovascular diseases (20.0%) accounted for most of the death cases. Most died in hospital (68.6%).

Others include cellulitis, chronic myeloproliferative disease, chronic obstructive pulmonary disease (COPD), end stage renal disease (ESRD), head injury, interstitial pulmonary disease, myelodysplastic syndrome, other and unspecified cirrhosis of liver, other gastroenteritis and colitis, unspecified diabetes mellitus: with peripheral circulatory complication.
Includes care homes, hospices.
Table 3 shows the risk factors associated with mortality at one year post-admission. In the bivariable analysis, age, tube feeding, admission from nursing home, AMT and Barthel scores were found to be significantly associated with mortality.
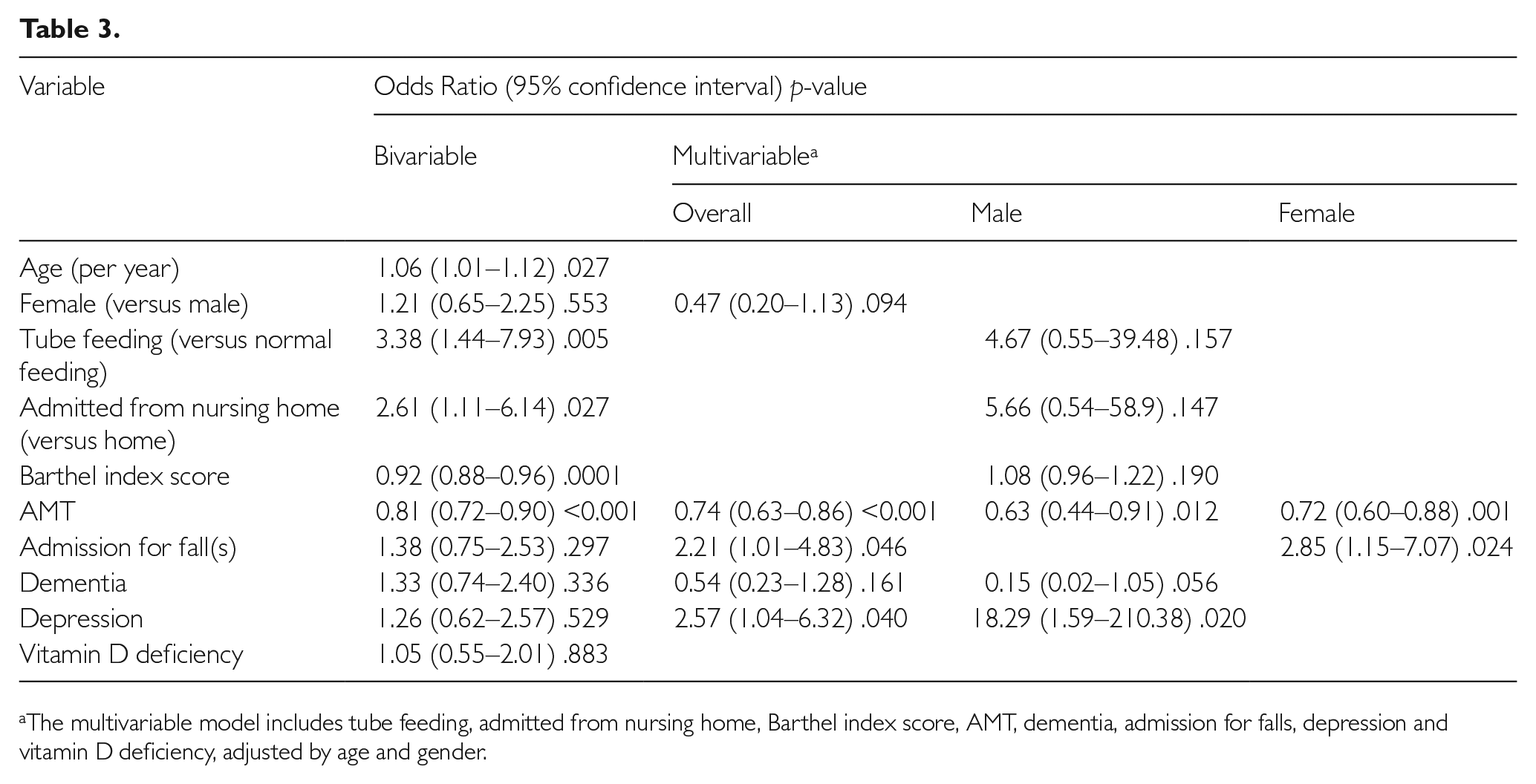
The multivariable model includes tube feeding, admitted from nursing home, Barthel index score, AMT, dementia, admission for falls, depression and vitamin D deficiency, adjusted by age and gender.
In the overall multivariable logistic regression model adjusted by age and gender, patients with higher AMT score were less likely to die within one year post-admission, with an odds ratio of 0.74 (95% CI, 0.63−0.86). Other significant risk factors in the model were admission for falls (OR, 2.21; 95% CI, 1.01−4.83) and depression (OR, 2.57; 95% CI, 1.04−6.32).
Due to interaction between gender and a number of variables in the model, a stratified analysis of the final multivariable model by gender was performed. Among males, the significant risk factors were AMT score (OR, 0.63; 95% CI, 0.44−0.91) and depression (OR, 18.29; 95% CI, 1.59−210.38). Among females, AMT score and admission for falls were significantly associated with mortality within one year post-admission (OR, 0.72; 95% CI, 0.60−0.88; and OR, 2.85; 95% CI, 1.15−7.07) respectively.
Discussion
The overall mortality rate within one year post-admission in our study was 35.7 %. This proportion ranged from 27% to 35% in earlier similar studies.5–7 The mortality rate of patients in our study was comparable to the results in these studies even though the mean age in our patient cohort (87 years) was higher than the mean age in these earlier studies (ranging from 70 to 82 years).5–8 Moreover, we also included patients who demised during their hospital stay. However, caution needs to be taken in interpretation due to possible heterogeneity of the studies, in which patients may differ in terms of baseline clinical characteristics. Nevertheless, our findings constitute a significant health concern as a high proportion of these elderly patients demised within one year of their hospital admission.
The mortality rate within one year post-admission was markedly higher than that during hospital admission in our study, suggesting worsening in clinical status over time after hospitalization. Likewise, it has been documented that progressive physical and clinical deterioration usually follows hospitalization for an acute illness, thereby leading to a high death rate during the months post-discharge. 9 Following discharge, elderly patients and their caregivers may face problems of inadequate medical, rehabilitative and socioeconomic support, which are readily addressed in the acute hospital, but less so in the community. Much more should be done to prevent the progressive health decline and recurrence of acute illnesses through appropriate and coordinated discharge planning, education and enhanced follow-up in the community. Pneumonia was the most common primary cause of death in our study. Elderly patients often have numerous chronic diseases accompanied by considerable frailty, and pneumonia may be viewed as a “stressor event” 10 that accelerates rapid decline towards adverse outcomes such as mortality. This emphasizes the critical role of dysphagia management and preventive healthcare, including vaccinations for pneumonia and influenza. In our study, the risk factors for mortality reflect the interplay of multidimensional domains affecting outcomes of the elderly beyond the confines of hospital − medical, functional and emotional and social factors. While risk factors such as worsening AMT score and admission for falls may reflect mental and functional decline as a result of physiological ageing coupled with the presence of numerous comorbidities commonly found in the elderly, these factors are modifiable with appropriate and holistic geriatric intervention in the community to prevent adverse outcomes.
Our findings confirm that cognitive impairment, as indicated by AMT score, was strongly associated with mortality. This is consistent with findings from other studies. 3 It was hypothesized that cognitive impairment may impede compliance with treatment.11,12 Secondly, it may be a proxy for overall health decline. 13 Furthermore, it may pose considerable challenges in discharge planning. 14 Recognition of the important contribution of cognitive status to the prognosis of geriatric inpatients, through simple cognitive assessment should be carried out in routine clinical practice. This seemingly subtle indicator can be incorporated in needs assessment for more intensive geriatric interventions or resources for support upon discharge, as well as in advance care-planning for patients with dementia. Low-impact falls from standing height are a leading cause of injury in the elderly. Fall risk has been studied as a geriatric syndrome8,15 and this is an important component of a comprehensive geriatric assessment performed routinely in the acute geriatric care unit. In this study, a history of admission for falls was found to be associated with mortality within one year post-admission. A few hypotheses may explain our findings. First, patients who had admission for falls might have serious underlying acute medical conditions precipitating the fall. They may also suffer a greater burden of chronic comorbidities as predisposing factors for falling. Second, there is also a negative impact on the patient following the fall as a direct result of injuries, functional loss, prolonged hospitalization, and a slippery slope to developing more complications, which herald a progressive decline towards mortality. Fragility fractures, especially hip fractures, and traumatic brain injuries from falls are well established causes of trauma-related hospitalization and poor outcomes. 16 In a study of elderly people with ground-level falls admitted to a trauma center, one-year mortality was reported to be 33.2%. 17 In our institution, these patients are often managed in the acute geriatric unit after their initial stabilization with or without surgical intervention in the orthopaedic trauma or neurosurgical units. They are also more likely to be readmitted to the acute geriatric unit subsequently, usually from various complications of functional decline and immobility, and hence captured in our study population.
Admission for falls was identified as a significant risk factor for mortality in our study. Hence, we propose utilizing it as an objective measure of fall severity. We conclude that it is useful to incorporate a history of admission for falls as part of a comprehensive geriatric assessment in view of its relevance to mortality and ease of ascertainment of such a measure. Further studies should be performed to confirm this risk factor, whilst implementation of geriatric trauma programs and a more active, holistic approach to managing geriatric trauma patients should be pursued.
The effect of admission for falls on mortality persisted in females when we stratified our analysis by gender, but not in males. Females constituted two-thirds of our study cohort. Females are generally frailer than males and frailty was related to death to a larger extent in females compared to males. 18 There may also be residual confounding unaccounted for in our finding in females; further research may be needed to elucidate the factors for the increased risk of mortality among females who had admission for falls. Vitamin D deficiency, which is associated with increased risk of falls and also linked with all-cause mortality, 19 was not found to be significantly associated with mortality in our study. This may be attributable to our small sample size.
Depression is common in elderly people. It was found to influence mortality in the overall multivariable analysis and its effect remained in males after stratification by gender. An association has been found between baseline depression scores and all-cause mortality in the elderly. 20 Depression could result in poor compliance with a treatment regimen 14 or interfere with ability to seek treatment advice. 21 It often contributes to worsening of functional and nutritional status. 14 In hospital, the emphasis clinicians place on treating acute conditions may undermine the importance of depression in contributing to outcomes for geriatric inpatients. 21 Thus it is important to educate physicians in recognizing depressive symptoms and institute prompt management, in an effort to improve the survival and functional level of geriatric inpatients.
We found an association between enteral feeding and mortality in bivariate analysis although the effect was much attenuated in the multivariable analysis. This group of patients constitutes those on pre-existing enteral feeding as well as those with newly instituted enteral feeding. The vast majority of them were on nasogastric tube feeding. Elderly patients placed on enteral feeding have compromised nutritional status or dysphagia, predisposing them to infections such as pneumonia. Hence, it is prudent for clinicians to be aware that tube-fed patients have a higher mortality rate, thus instituting proper measures to reduce the risk of aspiration.
Advance care-planning is an important component of holistic care of the hospitalized elderly. It has been established that patients and families are inadequately educated about prognosis and critical end-of-life decisions such as the extent of resuscitation, procedural interventions, broad-spectrum antibiotic therapy, tube feeding and preferred place of demise. 22 In Singapore, there is much room to implement advance care-planning programs in public hospitals. With accurate identification of patients at high risk of mortality over one year, this can greatly enhance patient-centered care and potentially reduce unnecessary intensification of care at the end of life.
There are several strengths and limitations in our study. First, information on the death status was obtained from a national registry which ensured reliability and completeness of outcome data. Our study has bridged the existing knowledge gaps on the magnitude of mortality in Singapore elderly inpatients as most of the previous studies were conducted in Western countries. It also provided us with an insight into the adverse outcomes of the patients post-admission as this may reflect the effect of multiple domains beyond the confine of direct hospital care which may be related to functional, cognitive, community and socioeconomic factors. On the other hand, the sample size in our study was relatively small for in-depth analysis, especially for the male population. In addition, we did not examine other important risk factors that were reported in other studies such as the presence of delirium, frailty, polypharmacy, nutritional status and self-rated health. We would also have liked to benchmark our data with other public hospitals in Singapore.
This study offers significant insight into mortality trends and risk factors for clinicians, hence guiding them in individualizing their management plan for acutely ill geriatric patients. Predicting long-term prognosis will enhance rehabilitation goal-setting and advance care-planning. This study may also provide impetus for larger scale studies in the study of mortality for both the hospitalized and community-dwelling elderly.
Footnotes
Declaration of conflicting interests
None declared.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
