Abstract
Objectives:
A toxicology team providing round-the-clock consultations for poisoning was established in Changi General Hospital in November 2014. This study aims to describe the epidemiology of patients referred to this service in 2015.
Methods:
A retrospective electronic and paper records review of all patients referred to the toxicology service from January to December 2015 was performed for demographics, poisoning, clinical, and outcome data. The cases were graded for poisoning severity score (PSS), likelihood of poisoning exposure and relative contribution to fatality for death cases.
Results:
A total of 306 cases were referred to this service in 2015. The median age was 34 years with majority being females (54%). The most common cause of poisoning was deliberate self-harm (62%) and the most common route of poisoning was oral (85%). Analgesics (21%) and sedatives (19%) were the most common poisoning classes. Six per cent of patients received decontamination and 17% received antidotes. The likelihood of poisoning exposure was probable to definite certainty for 85% of the cases. Mild poisoning (PSS 0–1) constituted 76% of the cohort, while 22% had moderate to severe poisoning (PSS 2–3). Out of the five fatalities, three were exposure-related fatalities contributing to a fatality rate of 1%. Fifty-four per cent of patients were admitted to the emergency department observation unit, 17% to general inpatient wards and 9% to either intensive care unit or high dependency wards.
Conclusions:
Although most poisoning cases resulted in mild clinical effects, a small but significant number of severe acuity cases occurred in this cohort.
Introduction
Poisoning, which is a worldwide problem, 1 poses a significant health problem even in a developed country like the US, where poisoning is the leading cause of injury related mortality. 2 The US poison control centres reported 2.17 million human exposures in their 2015 annual report, with 1371 exposure-related deaths. 3 A local multi-centre study from 2001 to 2003 noted that toxic exposures constituted 0.94% of total emergency department (ED) attendances, 4 with a sizable portion of them being admitted (36.1%).
Our hospital, Changi General Hospital (CGH), is a restructured tertiary hospital located in the eastern region of Singapore with approximately 150,000 ED attendances a year. A toxicology service available in the hospital since 2008 was revamped in November 2014, with the formation of a toxicology team comprising of toxicology trained consultants (in-house and visiting consultants) and toxicology fellows. The service provides round-the-clock phone consultation as well as bedside consultation where needed to health care professionals in the hospital with regards to poison information and clinical case management. The toxicology service also contributes to education in clinical toxicology by organising regular toxicology teaching case discussion rounds as well as providing a toxicology elective program for emergency medicine residents. This study describes the epidemiology of patients referred to the toxicology service in 2015.
Methods
A retrospective review of consultation records as well as clinical notes was done for all patients referred to the toxicology service from 1 January to 31 December 2015. The toxicology service consultation records are regularly uploaded into an excel sheet (kept in a secure database) for every case that is consulted. Cases that could not be traced due to inadequate identification details were excluded from the study. Most of the cases were consulted via phone consultation but some of the cases were seen in the ED by the toxicology team members who were on duty.
Patient demographics on age and gender and poisoning data which included poison type, dose, route and reason for exposure were abstracted. Clinical data on case severity and interventions received (decontamination, antidote and other specific treatment) along with the outcome data (disposition and final outcome of patients) were also abstracted.
The severity of poisoning was retrospectively graded using the poisoning severity score (PSS).5,6 The score ranges from 0 to 4 in clinical severity (0 = asymptomatic, 1 = mild, 2 = moderate, 3 = severe and 4 = fatality) (see Supplementary Table 1 online). The PSS recorded for each patient was the highest severity of poisoning that occurred during the patient’s stay in the ED and/or inpatient ward. The organ system effect that resulted in the final score was also determined.
The likelihood or certainty of poisoning exposure was further determined for each case by consensus between two independent reviewers. The likelihood of poisoning exposure is based on the clinical information available and determines how likely the exposure to poisoning could have occurred. There are four grades: definite, probable, possible and unlikely as well as an ‘unknown’ category (Supplementary Table 2). This grading system is adapted from the WHO Uppsala Monitoring Centre system on causality assessment, where the emphasis is on causation. 7
All deaths were further reviewed by two senior clinicians and the relative contributions of poisoning to the fatality were determined using the relative contribution to fatality (RCF) scale that is used in the American Association of Poison Control Centre annual reports (Supplementary Table 3). 3
All data was entered directly into a standardised Microsoft Excel (Microsoft, Redmond, WA, USA) spreadsheet. Descriptive data are presented. Categorical data are presented as percentage frequencies, while continuous data are presented as medians with interquartile ranges (IQRs). No statistical analysis is used. This study was approved by the Singapore Health Services Institutional Review Board.
Results
A total of 316 patients were referred to the toxicology service for the year 2015, wherein 10 patients were excluded due to inadequate identification details. The toxicology service received a median of 24.5 (IQR 24–26) consultations per month. The majority of consults were from the ED (83%), followed by the ED 23 h observation unit (EDOU) (13%) and the inpatient wards (4%).
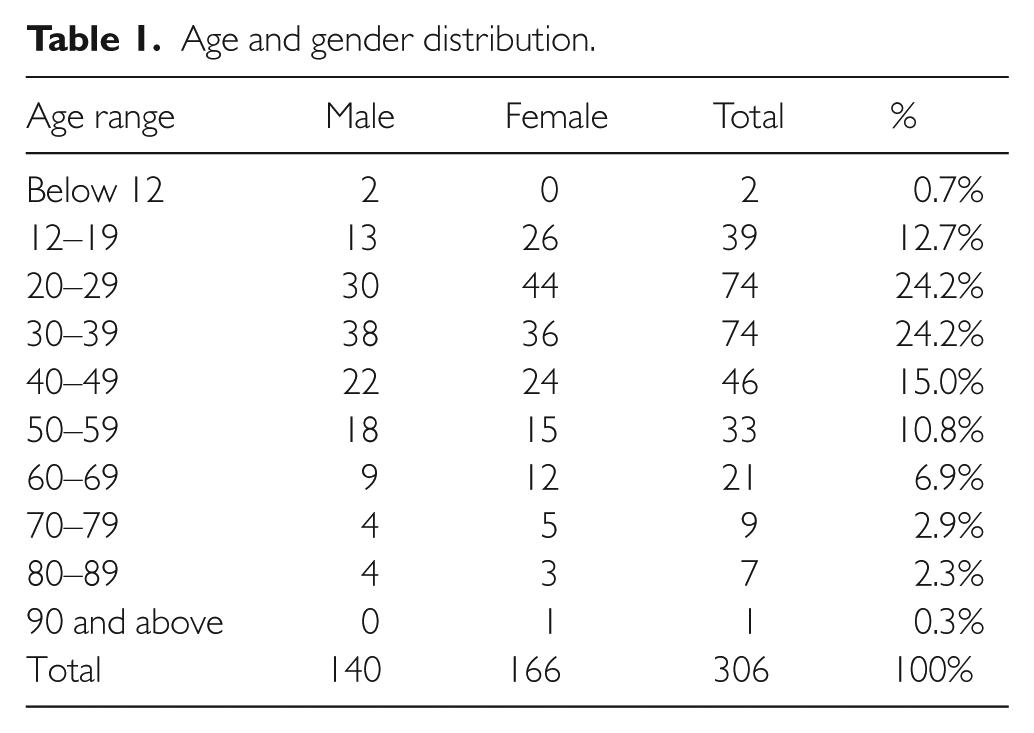
There were 166 female patients (54%) and 140 male patients (46%) referred. There was a female preponderance across all age groups except for the 30–39 and 50–59 age groups. The ‘20–39’ age range was the commonest and the median age of our cohort is 34. The age and gender distribution of the cases is shown in Table 1.
Age and gender distribution.
Three cases were assessed to be unlikely due to poisoning. This included one fatality case that was confirmed to be unrelated to poisoning after the post mortem report was reviewed. A total of 303 cases were then included in the further analysis below.
The commonest cause of poisoning was due to deliberate self-harm which accounted for 62% of the cases. The most common route of exposure is oral (85%), followed by dermal (9%) and inhalational (6%). Reasons for poisoning exposure are shown in Table 2.
Reasons for poisoning exposure.

The majority of patients (68%) took only one agent, while 20% took two agents and 12% took ≥3 agents. The three most common poison classes were analgesics (21%), sedatives (19%) and antidepressants (9%). The most common poisoning agent ingested was paracetamol, which was taken by 22% of patients. Figure 1 illustrates the distribution of the poisoning classes.

Poison class distribution.
With regards to management, the majority of patients received supportive care measures. A total of 18 patients (6%) were given decontamination treatment with activated charcoal; one of them also received gastric lavage. Fifty patients (17%) were given antidotes, wherein the three most commonly used antidotes were N-acetylcysteine (68%), naloxone (12%) and flumazenil (12%). Of the 34 patients given N-acetylcysteine, 29 of them were admitted to EDOU, while five patients were admitted to the ward. Table 3 shows the poisoning characteristics of the cohort.
Poisoning characteristics.

The disposition of cases is shown in Table 4. Of the 303 cases referred to the toxicology service, 54% were admitted to EDOU while 26% of patients were admitted to inpatient ward. Altogether 27 patients (9%) required intensive care unit (ICU) or high dependency (HD) ward management. About 12% of cases were discharged directly from the ED once they were medically cleared. Of the patients admitted to EDOU, only 15 patients (9%) subsequently required inpatient admission for poisoning related issues.
Disposition from Emergency Department (ED).

The PSS was then used to grade the severity of poisoning. The majority of patients (80%) had a PSS of 1 or 2 (mild or moderate poisoning). There were also nine cases (3%) who presented with a PSS of 3 (severe poisoning) and five cases (1.7%) who had fatal poisoning (PSS 4). The two most common organ systems affected by poisoning were the neurological system (46%) and gastrointestinal system (19%). The majority of patients had uneventful recovery during their hospital stay. The clinical severity (PSS) is shown in Tables 3 and 5.
Likelihood of poison exposure and poisoning severity score (PSS). Scores expressed as frequency of occurrences, with percentage in parentheses.

Of the five fatalities in our study, only three of them were judged to be poison related fatalities making an exposure-related fatality rate of 1% for our cohort. Details regarding the five cases are described below and summarized in Table 6.
Fatality cases.

Case 1
This patient was treated for hyperthermia with complications of rhabdomyolysis and kidney injury. Blood level of paroxetine was in the toxic range. The clinical presentation was consistent with serotonin syndrome. Work-up for other causes to account for the hyperthermia and rhabdomyolysis were negative.
Case 2
The patient had a large ingestion of clonazepam. Blood and urine toxicology level confirmed the diagnosis but also found elevated levels of olanzapine, aripiprazole and fluoxetine. Although she had initial clinical improvement, she passed away suddenly 2 days after admission. Post mortem examination did not reveal other causes of death and the cause of death was attributed to mixed drug poisoning.
Case 3
This elderly patient was intoxicated with elevated level of ethanol at more than 400 mg/dL. He was intubated and admitted to ICU. Subsequently, he developed other complications and passed away from those complications 30 days later.
Case 4
This patient had anorexia nervosa and ingested paracetamol frequently. She presented with intracerebral haemorrhage and passed away from this condition. However, she also had high anion gap metabolic acidosis and elevated paracetamol levels. Pyroglutamic acidosis was a possible cause for the persistent metabolic acidosis after other causes were excluded.
Case 5
This elderly lady presented with bradycardia and atrioventricular block with prolonged QT interval possibly due to her medication, sotalol. The bradycardia and widened QTc subsequently resolved after 2 days. However, she passed away from other unrelated causes 3 weeks later.
Discussion
CGH ED has a yearly attendance of about 150,000, which is about 15% of ED attendance at all public hospitals in Singapore. 8 For the year 2015, there were 306 consultations to the toxicology service, which is about 0.2% of ED attendances. This is much lower than the 0.94% toxic exposure that was reported from a multicentre study, 4 and the 0.4% poisoning cases reported from another local hospital. 9 However, these are retrospective reviews of all cases seen at the ED but our cases are those for which the toxicology service was consulted. From the figures, it could be estimated that the number of cases that our service was consulted is about one fifth to half the number of toxic exposure cases seen at our hospital.
The Hong Kong Poison Information Centre (HKPIC), which has been established for almost 10 years, 10 provides a consultation service to all physicians and healthcare workers in Hong Kong. They have an average annual census of about 4000 cases of poisoning. In 2015, 2142 (or half of them) were cases where consultation was made to the poison centre. The remainder 1818 cases did not consult the poison centre but were cases that were reported. Hong Kong has a population of about 7.3 million and the number of cases consulted per 1000 population is about 0.29 cases per 1000 population. Singapore has a population of 5.6 million. CGH ED sees about 15% of the share of the ED attendance which would cater for an estimated 840,000 population. The number of consults would be about 306/840 = 0.36 per 1000 population which approximates the number of consults for Hong Kong poison centre. Projecting from this number, Singapore could have about 2000 toxicology consult cases a year if there is a nation-wide physician phone consultation service for poisoning.
Poisoning and envenomation cases, though not common, can have unique diagnostic and therapeutic challenges. Various factors need to be evaluated for risk assessment when managing these patients – the nature of the chemical or drug, the dose exposed and the vulnerability of the patient involved as well as the clinical presentation. Clinical toxicologists are trained to bridge the gap between clinical medicine and the science of toxicology; to evaluate and manage patients exposed to a particular toxicant. Toxicologist involvement in the management of poisoning has been shown to improve efficacy and safety with associated cost savings. In Queen Mary Hospital in Hong Kong, 11 the development of an ED toxicology team to help in the management of poisoning showed benefit in decreased admission and hospitalization length of stay without increased complication rates. The toxicology unit established in Brisbane, Australia, 12 reported significant decreased length of stay and cost savings achieved under their management of poisoned patients. Similarly, other centres compared cases that consulted a Poison centre to those that did not and found increased savings from reduced length of hospitalization as well as efficient resource utilization.13,14 In our service, toxicology fellows do first line calls and they are backed up by toxicology consultants. The consultations are provided mainly via phone consultation but bedside reviews of patients are also provided when the clinicians are on the floor. As there are only about 1–2 toxicology consultants in each public hospital, the service is able to function round-the-clock with visiting consultant toxicologists from other hospitals.
The poisoning demographics showed that the age group most affected by poisoning are those in the 20–40s. Morbidity and mortality sustained by this younger economically viable age group would have greater socio-economic impact since they are in the prime of their lives. The poisoning agents corresponds with other local studies,4,9 as well as the AAPCC adult exposure spectrum, 3 with analgesics, sedatives and antidepressants being the most common poisoning classes. Paracetamol is the most common drug taken in overdose.
The severity of poisoning was determined using the PSS. 6 Most poisoning cases resulted in mild to moderate effects. The figures closely match that from Hong Kong where about 60% of the cohort had mild clinical effects and about 5% of the cases are graded as severe or fatal. 10 This is also consistent with other local studies.4,9 Patients with mild effects could be managed in the outpatient setting especially if the exposure is unintentional. In our cohort, 15% of cases are managed in the outpatient setting (12%) or transferred to the Institute of Mental Health (3%) for psychiatric management. Managing appropriate patients in the outpatient setting rather than being admitted to an acute hospital would help to reduce health care cost. A previous study by the poison centre in Singapore showed that there was cost savings when unnecessary admissions were prevented. 15 As for our study, the cost savings from our toxicology service in decreasing unnecessary admission cannot be assessed as data on cases not consulted is not available for comparison.
Patients with intentional exposure due to deliberate self-harm made up the majority of cases. They would require psychiatric assessment and some of these patients require inpatient psychiatric management. To ensure that the patients do not have acute poisoning issues, a period of observation and treatment in an acute hospital setting before transfer to a psychiatric facility may be required. This can be achieved by an EDOU which coordinates different services in the management of these patients. This has been shown to be efficacious and safe in a recent publication where 92% of patients were medically cleared. 16 Management of patients in the EDOU could also result in decreased length of hospital stay and resource utilisation as shown in a comparative study in patients who needed a full course of N-acetylcysteine for the treatment of paracetamol poisoning where a 47% reduction in length of stay was shown. 17
In this cohort, about 9% of the cases were admitted to the HD or ICU with an average of about 2–3 cases a month. This is much higher than the 1.7% and 3.9% in the other two local studies.4,9 This is probably because consultation to the service is more likely to occur for serious poisoning cases compared to less serious cases. A local paper on an ICU poisoning cohort reported 50 consecutive poisoning cases over a 3 year period. 18 However, our figures, and the other two local papers,4,9 did not differentiate ICU from HD care. With about 27 cases a year from our centre, we estimate that it could translate to be about 180 cases a year for all the public hospitals in Singapore since our ED sees about 15% of all ED workload. This works out to be about 1 ICU/HD admission once every 2 days amongst all public hospitals at the national level.
The poisoning related fatality rate for our cohort is about 1% which is much higher than other reported studies of 0.08% and 0%.4,9 In the ICU study, 18 however, there were four deaths over 3 years. In a local forensic report, 19 about 6.9% of unnatural death was drug related, of which 108 cases over the 2 year period were due to poisoning. The fatality rate reported in Hong Kong poison centre is also about 1%. Our study would include both deaths that occurred at the ED and those that died in the inpatient wards. In addition to the reason stated in the prior paragraph that this is a referral based study, our fatality rate is also higher compared to local ED based studies probably because cases not coded with poisoning diagnosis in the ED but was subsequently determined to be poisoning related could be missed in those studies. Some of our patients were referred from inpatient wards although they were not admitted with a poisoning diagnosis. As toxicology test results have a long turn-around time, certainty of poisoning as well as relative contribution to fatality can only be made after review of all the data. The number of fatalities associated with poisoning could be extrapolated to be about 20 deaths per year for all public health care facilities or about 1–2 fatalities per month. This figure is lower than the forensic report by Wang and Ching, 19 where about an average of 54 cases (108 cases in 2 years) of unnatural deaths a year is due to drug, alcohol and poison. Our study would not have picked up poisoning deaths that occurred outside hospital or who were brought in dead to the ED with an unknown cause of death.
Patients who are seriously poisoned need active and timely interventions and resuscitation. As serious poisoning is uncommon, clinicians may have limited experience managing these cases which could require special antidote treatment, decontamination as well as enhanced elimination measures. The availability of a round-the-clock toxicology service could help to assist clinicians in managing these challenging severe poisoning cases.
Limitations
As this is a retrospective review of cases that consulted the toxicology service, we are not able to comment on the efficacy of the service in promoting patient safety and treatment outcome. There was limited documentation on the advice given over phone consultation making it difficult to determine the extent the advice was followed through. The follow-up of patients was also limited to the hospital encounter and no data was available for post-discharge outcomes. Although the service is listed in the daily call roster in the hospital, consultation to the service is not mandatory. Comparison of this cohort with cases not consulted is not possible as the total number of toxicology related attendances is unknown. The estimation of toxicology workload for a national physician consultation service is also limited by projection from one centre which may not apply to other centres.
Conclusion
We report the 2015 epidemiology of cases that consulted the newly established 24/7 toxicology service in our hospital. Although the frequency of poisoning is low, the morbidity and mortality that resulted is quite significant for a small cohort. A toxicology service could help reduce unnecessary admissions, as well as decrease the length of stay for those admitted by improving timely care for patients. However, further studies are required to show the efficacy and safety of the toxicology service in the management of poisoning and the cost savings that could be achieved.
Footnotes
Acknowledgements
The authors would like to thank Senior Staff Nurse Lim Miao Ling from Changi General Hospital A&E department for her help in data abstraction. We would also like to thank our visiting consultants and all who contributed to the study by referrals to the toxicology service.
Declaration of conflicting interests
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
