Abstract
Introduction:
The polymorphisms of the angiotensin-converting enzyme (ACE) and angiotensin-converting enzyme 2 (ACE2) genes have been demonstrated to be involved in some cardiovascular diseases. We hypothesised that the polymorphisms of ACE and ACE2 relate to the formation of thoracic aortic diseases and coronary heart disease.
Methods:
A total of 86 patients (four groups: thoracic aortic dissection; thoracic aortic aneurysm; coronary heart disease; and control group) were recruited. The ACE I/D polymorphism and the ACE2 (A8790G) polymorphism were measured in all patient samples.
Results:
There were no significant differences in groups with regard to either the ACE I/D polymorphism or the ACE2 (A8790G) polymorphism.
Conclusion:
The polymorphisms of the ACE and ACE2 genes are not associated with thoracic aortic dissection, thoracic aortic aneurysm and coronary heart disease.
Keywords
Introduction
Thoracic aortic aneurysm (TAA) is characterised by localised dilation of the aorta to a diameter greater than 50% of normal wall tissue. Thoracic aortic dissection (TAD) is a sudden event with high mortality involving a tear in the intimal layer of the aorta, haematoma formation and separation of the arterial wall. These diseases are characterised by infiltration of inflammatory cells, depletion of vascular smooth muscle cells and degradation of the extracellular matrix within the aortic wall. 1 Several risk factors such as smoking, hypertension, atherosclerosis and diabetes may predispose to the progression of aneurysmal dilatation and dissection.1,2 Furthermore, some TAD cases are related to inherited diseases such as bicuspid aortic valve, Marfan syndrome and Loeys–Dietz syndrome;1–3 however, the genetic propensity associated with non-syndromic TAD and TAA remains largely unknown.
The renin–angiotensin system (RAS) has been known to be intimately involved in disturbances for some cardiovascular diseases.1,4 The RAS regulates sodium balance, extracellular fluid volume, vascular resistance and arterial blood pressure. Angiotensin-converting enzyme (ACE) is a key regulator of RAS, and angiotensin-converting enzyme 2 (ACE2) acts in a counter-regulatory manner, modulating the balance between vasoconstrictors and vasodilators within the heart and kidney to regulate cardiovascular and renal function. ACE catalyses the conversion of angiotensin (Ang) I to Ang II. The latter affects the arterial wall by modulating the function of numerous adhesion molecules, cytokines and growth factors that may be responsible for inflammation, hypertrophy, extracellular matrix degradation and proliferation and apoptosis of dysregulated vascular smooth muscle cells.5–7 ACE2, a homologue of ACE, has emerged as an important player in the pathophysiology of vascular diseases due to its protective role in metabolising pro-inflammatory, pro-proliferative and pro-hypertensive Ang I and Ang II into favourable Ang (1–9) and Ang (1–7), respectively.7,8 The physiological role of ACE2 opposes that of ACE, and studies suggest that ACE2 can stabilise atherosclerotic plaques, reduce platelet adhesion, mitigate thrombosis, reduce inflammation, promote myocardial remodelling and lower blood pressure.9–11
Despite significant differences in ACE and ACE2 expressions in TAD, TAA and coronary heart disease (CHD) having previously been demonstrated, 12 the roles that ACE and ACE2 gene polymorphisms play in TAD and TAA are still unclear. The activities of ACE and ACE2 are based on the ACE I/D polymorphism and the ACE2 (A8790G) polymorphism,13–15 respectively. Studies evaluating the association between the ACE I/D polymorphism, the ACE2 (A8790G) polymorphism and thoracic aortic diseases or hypertension have produced conflicting results. The reason is that these polymorphisms may play a role in aortic diseases or hypertension for certain populations. To our knowledge, such polymorphisms in populations from southwest China have not previously been studied. Therefore, the present study examines these polymorphisms to determine if either one plays a role in vascular diseases among a population from southwest China.
Methods
Patients
All participants gave written informed consent prior to data collection, and the investigation conformed to the principles outlined in the Declaration of Helsinki. A total of 86 unique blood samples was collected between March 2011 and October 2012. Samples were divided into four groups: a TAD group (n=34, including those with Stanford classification types A and B); a TAA group (n=18); a CHD group (n=21) that suffered unstable angina in lesions of the left anterior descending coronary artery, left circumflex artery and right coronary artery; and a control group (n=13). Control subjects had no history of hypertension, diabetes, or other cardiovascular, endocrine, or renal diseases. Patients with therapeutic histories that included ACE inhibitors or angiotensin binding receptor drugs or those with Marfan syndrome were excluded.
Polymorphism of the ACE and ACE2 genes
Venous blood samples were collected in 5 ml ethylene diamine tetraacetic acid tubes from patients. Genomic DNA was extracted using the phenol–chloroform method. Assessment of the ACE I/D polymorphism was performed using polymerase chain reaction (PCR) with the primers 5′-CTGGAGACCACTCCCATCCTTTCT-3′ and 5′-GATGTGGCCATCACATTCGTCAGAT-3′. This was carried out in a final reaction volume of 25 µl mixture containing 3 µl genomic DNA, 1 µl of each primer, 12.5 µl Taq PCR MasterMix and 7.5 µl water. The thermocycling profile was one cycle at 94°C for 5 minutes, followed by 30 cycles each at 94°C for 1 minute, 58°C for 1 minute and 72°C for 2 minutes, and a final cycle at 94°C for 1 minute, 58°C for 1 minute and 72°C for 7 minutes. The PCR products were separated on 2.0% agarose gel and visualised under ultraviolet light after ethidium bromide staining. The lengths of the fragments separated were 490 bp and 190 bp, corresponding to the insertion allele (I) and the deletion allele (D), respectively. Polymorphism for ACE2 (A8790G) was likewise assessed using the primers 5′-CATGTGGTCAAAAGGATATCT-3′ and 5′-AAAGTAAGGTTGGCAGACAT-3′. Using identical reagent volumes as outlined above, the thermocycling profile in this case was 94°C for 1 minute, followed by 32 cycles of 40 seconds at 94°C, 30 seconds at 58.5°C and 30 seconds at 72°C, finally, 72°C for 7 minutes. After digestion with Alu I for 16 hours at 37°C, the digested products were separated on 2% agarose gel and visualised under ultraviolet light after ethidium bromide staining. The resultant PCR products yielded two DNA fragments of 281 and 185 bp for the AA genotype, one DNA fragment of 466 bp for the GG genotype, and three DNA fragments of 466, 281 and 185 bp for the AG genotype. Because the gene encoding ACE2 is assigned on the X chromosome, women expressed the AA, GG and AG genotypes while the men expressed only either the A or G allele.
Statistical analysis
Categorical data are presented as percentages. Differences in gender and histories of hypertension or diabetes and the differences of the ACE I/D polymorphism and the ACE2 (A8790G) polymorphism in groups were calculated using a χ2 test. The Fisher’s exact test was performed when any group had a frequency of less than five. A value of P<0.05 was considered significant.
Results
Patient characteristics are summarised in Table 1. There were no significant differences between groups (P>0.05). The genotype distributions and allele frequencies of the ACE and ACE2 genes are shown in Tables 2 and 3, respectively. The distributions of genotypes and alleles were not significantly different between groups (P>0.05), even when sex was taken into account in the latter.
Patient characteristics.

CHD: coronary heart disease; NA: not applicable; TAD: thoracic aortic dissection; TAA: thoracic aortic aneurysm.
Genotype distribution and allele frequencies of ACE I/D polymorphism.

ACE: angiotensin-converting enzyme; TAD: thoracic aortic dissection; TAA: thoracic aortic aneurysm; CHD: coronary heart disease.
Genotype frequencies χ2=2.926, P=0.843; allele frequencies χ2=1.348, P=0.725.
Genotype distribution and allele frequencies of ACE2 polymorphism.
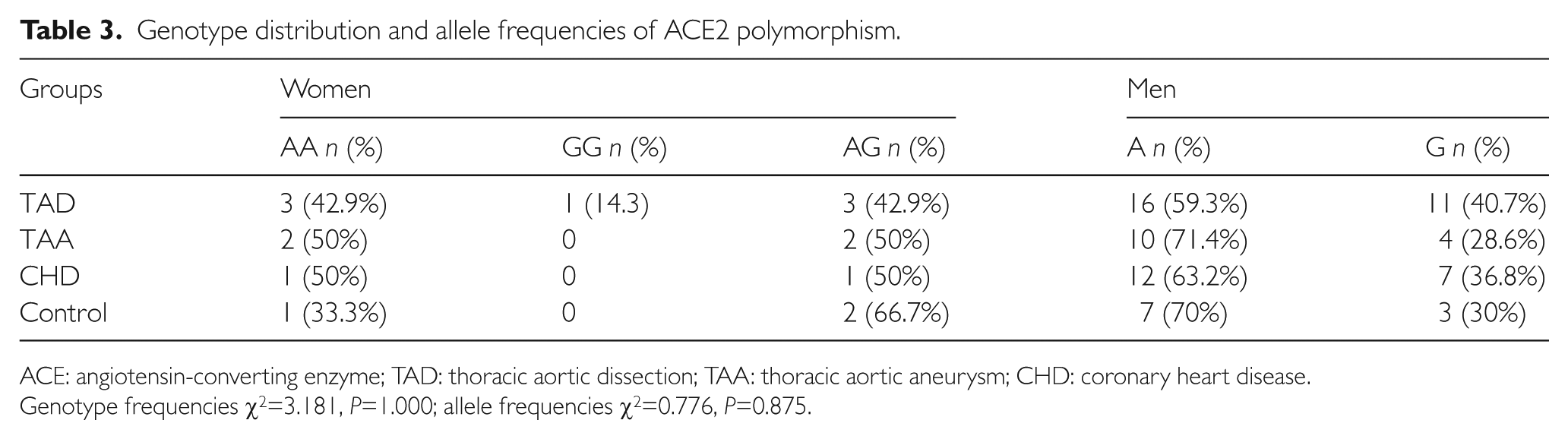
ACE: angiotensin-converting enzyme; TAD: thoracic aortic dissection; TAA: thoracic aortic aneurysm; CHD: coronary heart disease.
Genotype frequencies χ2=3.181, P=1.000; allele frequencies χ2=0.776, P=0.875.
Discussion
Previous studies have shown that ACE and ACE2 messenger RNA expressions are significantly different in people with TAD, TAA and CHD, 12 suggesting the importance of the ACE family in the pathogenesis of arterial diseases. The activities of ACE and ACE2 and their relationship to the ACE I/D and ACE2 (A8790G) polymorphisms were also assessed,13–15 and no significant differences were found.
Although ACE has been shown to play a role in heart diseases, the role of the ACE I/D polymorphism in them is still unclear. Some studies have demonstrated a relationship between the ACE I/D polymorphism and hypertension,16,17 but others have indicated otherwise. 18 Such uncertainty has also been demonstrated for the relationship between the polymorphism and coronary atherosclerosis disease.19,20
Conflicting results have also been reported for the role of the ACE I/D polymorphism in TAD and aortic aneurysms. Kalay et al. 21 and Jing et al. 22 have reported that the ACE DD genotype represents a susceptibility factor for TAD. Huang et al. 23 postulated that the ACE I/D polymorphism was associated with the risk of aortic aneurysm. On the other hand, Tangurek et al. 24 found no association between the ACE I/D polymorphism and TAD, which agrees with our results here. The difference in results might be due to the ethnicities studied, sample sizes and enrolling conditions. The study of Kalay et al. 21 involved a smaller sample size and subjects of a different ethnicity (Turks vs. Chinese) than in our study. Even when the subjects’ ethnicities were identical (e.g. Jing et al. 22 vs. this study), differences in climate and living conditions (northeast vs. southwest China, respectively) may be confounding factors. The meta-analysis of Huang et al. 23 involved subjects that were almost entirely afflicted with abdominal aortic aneurysm and the tiny proportion of subjects with TAA might have caused the opposite conclusion (compared to our study) to be reached. Finally, the conditions of the control group used in the studies may have also led to conflicting results: both Tangurek et al. 24 and Kalay et al. 21 used subjects of the same ethnicity, but different control group conditions (hypertension patients and chest pain patients, respectively). To conclude, some polymorphisms may be linked to cardiovascular disease in some populations and not others due to the ethnicity, geography and cultural factors such as diet and exercise.
The identification of the renin/prorenin receptor ACE2 as an angiotensin peptide-processing enzyme and a viral receptor, along with the identification of Mas as a receptor for Ang (1–7) has given us new insights into the RAS system. The ACE2 is an important Ang (1–7)-forming enzyme that turns Ang I to Ang (1–9), and this may offer a unique role for the local RAS in the heart and kidney. The physiological role of ACE2 opposes that of ACE, and studies suggest that ACE2 can stabilise atherosclerotic plaques, reduce platelet adhesion, mitigate thrombosis, reduce inflammation, promote myocardial remodelling and lower blood pressure.9–11
Based on the results of previous studies, 12 the question of whether the ACE2 gene polymorphism might play a role in protecting against TAD or TAA might be asked. However, the genotype distribution and allele frequency of the ACE2 polymorphism between groups were not statistically significant in the present study and, therefore, did not confirm this hypothesis.
The main limitation of our study lies in the limited number of patients examined, which is related to the rare morbidity of TAD. Furthermore, TAD and TAA are complex diseases. Just studying a single factor could lead to bias. Further studies with larger numbers should be undertaken to gain further insight. In conclusion, this study finds no association between TAD, TAA and polymorphisms in ACE and ACE2.
Footnotes
Conflict of interest
None declared.
Funding
This study was supported by the National Natural Science Foundation of China (nos 81300155, 81370413 and 81170288).
