Abstract
Introduction:
Heart failure is a progressive and often incurable condition associated with a poor quality of life. The aim of this study was to understand the experiences and preferences regarding care, communication and decision-making among patients living with heart failure in Singapore.
Methods:
Five focus groups were conducted with 27 patients that had heart failure. The focus groups were audio-recorded and transcribed verbatim. Thematic analysis was used for analyzing transcripts.
Results:
Six themes representing the experiences of patients with heart failure were identified. These were: 1) physical and psychological symptoms; 2) financial concerns; 3) uncertainty and lack of knowledge about disease; 4) difficulties in navigating the healthcare system; 5) end-of-life care concerns; and 6) fear of burdening family.
Conclusion:
The study highlights that health care services for patients with heart failure need to address the multifaceted impacts of the disease on patient’s lives. A focus on the provision of comprehensive health care services at the primary care level, training of health care providers in communication skills, involving patients and their families in decision making, and discussions about end-of-life care preferences and goals of care may help to improve care for patients with heart failure.
Introduction
Heart failure is a major public health issue and one of the leading cardiac causes of hospitalization in many countries.1–3 Median survival is less than five years, and one-year mortality among those with advanced disease may reach 50%. 4 This condition is progressive and currently incurable for a majority of patients, with a prognosis worse than that of many cancers. 5
While significant resources have been spent in efforts to increase survival for patients with heart failure, longer survival may not be the only treatment goal of patients. Heart failure often results in physical symptoms, and psychosocial and spiritual distress, which can lead to poor quality of life.6–9 Furthermore, patients have a fluctuating trajectory of illness that creates uncertainty about prognosis and makes it challenging for them to plan for end-of-life care.8,10,11 Comprehensive health care services are thus needed to address multifaceted impacts of the disease on patient’s lives. In order to plan and provide such holistic care, which may involve multi-disciplinary health care teams, it is first important to understand the experiences of patients living with heart failure.
We conducted a series of focus groups (FGs) with patients with heart failure in order to understand their experiences of living with the disease and their preferences regarding care, communication and decision-making. The study was conducted in Singapore, a rapidly aging country in Southeast Asia. With an aging population, both the incidence and prevalence of heart failure in the population is also likely to increase. However, there is a major lack of knowledge regarding the experiences of patients with heart failure in Asian countries, including Singapore, because studies on the preferences and experiences of heart failure patients have mostly been conducted in Western settings.4,12 Context-specific information derived from this study will thus enable practitioners and policy makers to tailor heart failure services to meet the specific needs of patients in these countries.
Methods
Participants
We conducted five FGs with a total of 27 patients with heart failure between April and October 2013. This method was chosen because it encourages communication, helping participants to explore and clarify their own views and preferences.13–14 We recruited patients from a single hospital in Singapore from March to September 2013. Clinical coordinators identified and screened patients with heart failure admitted to the hospital’s cardiology department from the clinical system on a daily basis. Eligible participants were at least 18 years old, had heart failure and were judged by the clinical coordinators to be physically and mentally competent to participate. The study was approved by the Institutional Review Board affiliated with the hospital.
We obtained written informed consent and demographic data from all participants before each FG. All of the patients, except one, were classified as being in New York Heart Association (NYHA) classification class I or II. All except one had a left ventricular ejection fraction of less than 55%. Three FGs were conducted in English and two in Mandarin. Each session lasted 75–110 minutes, included 5–6 participants, and was facilitated by a pair of medical social workers, who are native Singaporeans conversant in both English and Mandarin, using an FG guide developed by the study team. The medical social workers were trained to facilitate the discussion using the FG guide and to ask probing questions to uncover the participants’ values and preferences.
During the discussion, we first asked the participants to tell us about their experience of living with heart failure, the symptoms they faced, how these symptoms had affected their lives and whether they needed more help with any of their symptoms. In the second part of the discussion, we asked the participants about how much they thought they understood about their own illness and the type of health care they may need in the future. We then explored their preferences for care that they would like to receive when they are not able to care for themselves. Lastly, we explored participants’ concerns regarding their treatment and care.
We also asked follow-up questions to gain more information from patients or to clarify comments. We made sure that all participants had an equal opportunity to contribute to the discussion. An observer, also a native Singaporean, conversant in both English and Mandarin, attended each FG to audiotape the discussion and take notes. The observer then transcribed FGs verbatim and, in the case of the Mandarin FGs, translated the transcript into English. We reviewed transcriptions and translations for accuracy. We also analyzed the transcripts after each FG and, as the FGs progressed, revised the guide to probe more deeply into areas identified by earlier FGs. We ended data collection when analysis showed saturation of themes.
Analysis
Thematic analysis was used for identifying and reporting themes within the data to answer the research question. This method was used because it was not dependent on any theoretical framework and provides adequate flexibility for analysis. 15 Each FG transcript was coded independently by two members of the research team. The results were checked for consistency and revised as necessary. The coding and collation of codes were carried out manually. The initial list of themes was reviewed and then refined based on several discussions among team members. Illustrative quotes were edited for ease of reading but no substantive changes were made. Repeated words and grammatical inconsistencies were edited where necessary to clarify the meaning.
Results
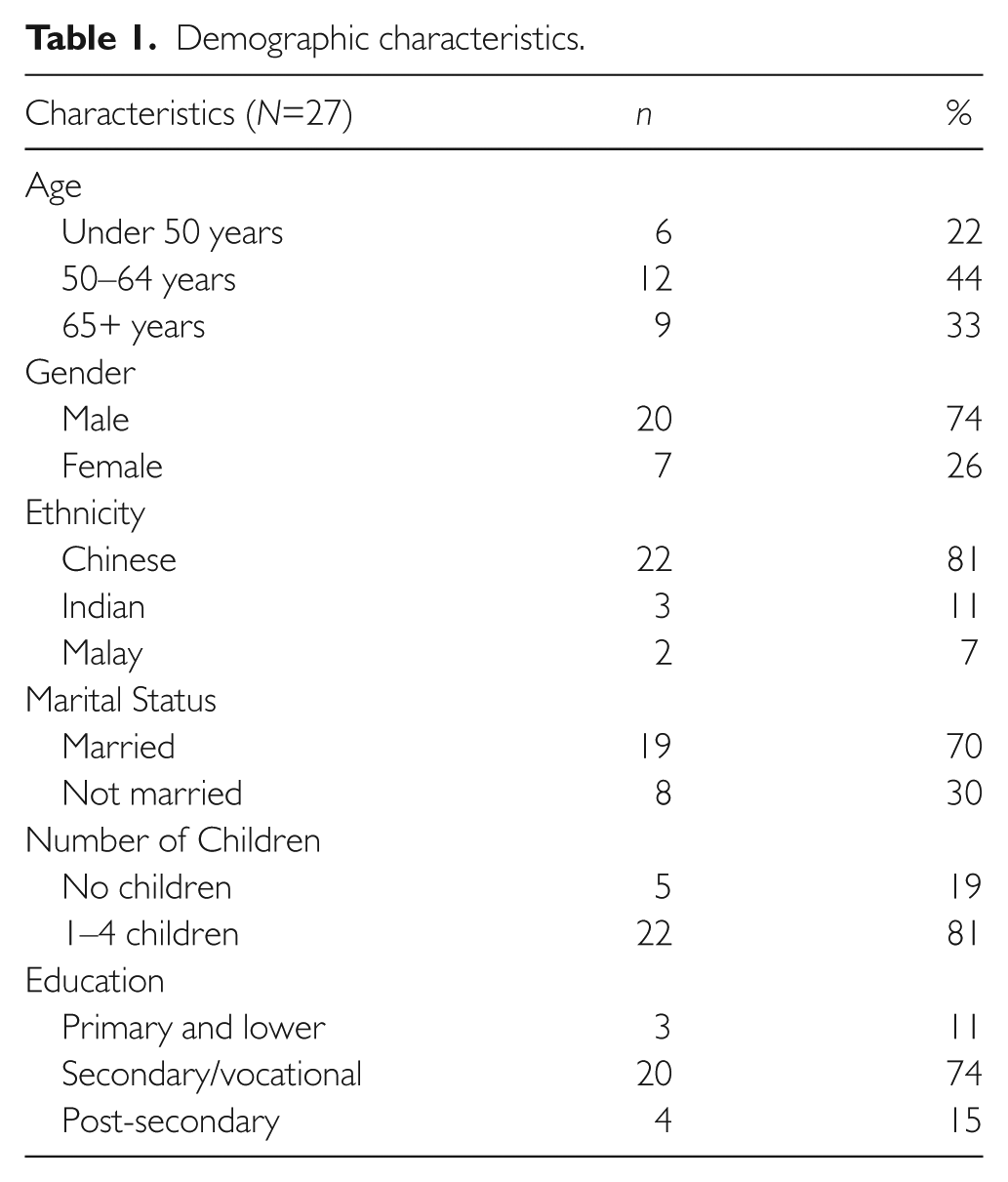
The demographic characteristics of patients are shown in Table 1. Patients ranged in age from 32 to 77 years, with a mean age of 58.6 years. Most were male (74%), Chinese (81%), married (70%), with secondary education (74%) and had one or more children (81%). All patients lived in public housing (Housing and Development Board (HDB) housing), 48% in 1–3-room HDB flats and 48% in 4–5-room or executive HDB flats. Socioeconomic status has been reported to be correlated with household income, with larger units reflecting higher income. 16 Seven patients had participated in Advance Care Planning (ACP). We identified six underlying themes that represent the experiences and concerns of patients with heart failure.
Demographic characteristics.
Physical and psychological symptoms
During the FGs, patients reported having experienced severe breathlessness, fatigue, sleep disturbances, anxiety, depression and panic attacks. Many described how they had stopped engaging in certain activities, such as climbing pedestrian bridges, swimming, shopping, meeting up with friends or taking vacations, as a result of their symptoms. Patients also explained how they had made changes to their lifestyle and restricted their liquid and food intake. Managing multiple medications and dealing with their side effects were problematic and sometimes caused patients to miss medications. Dealing with comorbidities further complicated the situation, especially among older patients.
It affected me emotionally, I became very depressed, I had bouts of depression. At one time I sort of gave up on life… one of the common emotion is frustration. I used to be able to do this thing you know, I used to be able to go out, to handle such situations; now I cannot. (57 years, male, Chinese, married, FG3) Now, I have to take about 20+ tablets a day. I have to take all sorts of medications. High blood pressure and so on. (38 years, male, Chinese, married, FG3)
Financial concerns
The financial burden of living with heart failure was discussed in each session, with many patients identifying high medical costs as a primary concern. They reported having depleted their Medisave accounts and finding that Medisave, Medishield or private insurance could be used to claim only a portion of hospitalization or surgical costs. In addition, heart failure impacted patients’ ability to participate in active employment. Sometimes, financial pressures meant that patients had to continue working, even when it was detrimental to their health. As a result of financial pressures, some patients considered not going for regular check-ups or not receiving certain treatments or surgeries. Others felt that it was important to pursue treatment so that they could be around to support their families financially. Many said that if their condition was bad, they would not want to pursue expensive life-extending treatments.
For me, I can’t follow [the doctor’s directions]. My doctor told me cannot work night shift…but…I have to work night shift to earn more. You can’t say what you want. I’ve been working in a smoking environment also, because I’m working in a casino…So I either work, or don’t work…. I will go for the operation because of my children. I am the only person earning money, the only person supporting my family. (38 years, male, Chinese, married, FG3) Uh, I talked to my family regarding my illness. If the situation is not good, just give up. This is because I know that the hospital bills are expensive, so there’s no point dragging. (55 years, male, Chinese, married, FG2)
Uncertainty and lack of knowledge about disease
Throughout the FGs, patients identified many gaps in their knowledge about a range of issues relating to their disease and treatment. Many patients felt that they accurately understood their diagnosis and previous procedures they had received; however, patients expressed the desire for more functional knowledge about symptom management, side effects and disease progression, including whether recovery is possible. Many patients expressed the concern that physicians do not discuss their illness with them in detail; rather, physicians prefer to talk about the patients’ condition with the patients’ families, who may or may not discuss these details with the patients. Patients felt that having more information would allow them to manage their disease and have a general understanding of their condition, as well as empower them to make decisions and plan for their remaining time. Some patients felt that it is better not to know about the prognosis, as heart failure is very unpredictable. Patients also felt that their families needed to have more information about their disease, so that family members would know what to expect and how to support the patient.
I feel that at times, the doctors do not really like to talk to us regarding our illnesses. They would talk to our family. (63 years, female, Chinese, married, FG2) When I had this condition, my wife was lost. In fact, it was more traumatic for her than for me. So how is the caregiver going to look after us, they do not know how to do that… teaching them how to care for people like us, how to react to people like us, these are very important. (57 years, male, Chinese, married, FG3)
Difficulties in navigating the healthcare system
FGs revealed that diagnosis of heart failure was often delayed as family physicians could not always diagnose the condition. Patients with comorbidities found it especially difficult to juggle instructions and multiple medications, and had trouble knowing which doctor to listen to and which treatment plan to prioritize. Appointments and referrals often took longer than expected. Some patients had experiences in which doctors did not treat them in a respectful manner, or were less willing to answer questions or communicate information about the patient’s condition. As a result, some patients explained that they had refused certain treatments or sought out a different doctor or hospital.
Language was also identified as a potential barrier, although patients also felt better cared for when healthcare professionals did speak to them in their preferred language. Others felt that Chinese educated patients were at a disadvantage during communication with their doctors. Still others felt that patients in subsidized wards and those who could not afford to pay were discriminated against. Long waits and short appointments, lack of coordinated care between physicians and institutions, and lack of information about treatment costs all contributed to patients feeling uninformed. This, in turn, made some patients feel disrespected, undervalued or powerless.
Now got two consultants, one is the heart, one is diabetic…the medication, the diabetics that you take, that is alright. Heart side no, is no good for your heart. Then okay, then what? I’m in the middle, what am I going to do?… So make me also confused you know, whether to take or not to take. (71 years, female, Chinese, married, FG5) There are differences between the English educated and Chinese educated people. English educated people dare to rebuke the doctors. Chinese educated people are more afraid to do so. (64 years, male, Chinese, married, FG4)
End-of-life concerns
Some patients had participated in ACP and had made decisions about where they would like to be cared for towards the end of life. Most had decided to avoid undue prolongation of their life and had discussed their preferences with their families. On the other hand, those who had not participated in ACP had little idea of what care they would like to receive or the types of treatment decisions they might have to consider in the future. Most patients agreed that quality of life is important, and that it would not be worth prolonging life if quality of life is poor. Some patients wanted to make their own decisions regarding end-of-life care; others wanted their family or doctors to decide for them. Most patients seemed to think that their families’ decision would be appropriate.
That’s a question, but I feel quite okay now…but to me I think, if that bad, don’t hold [prolong life]. Make you survive some years and months for what? Might as well take out [life support], and finish. So, so, better not, I already told my family if condition no good, don’t need [life extending treatments]. But some, you know Chinese ah, children will say: “no, no, no, I want to pay for all costs, at all costs, tell doctor to hold!” So they know already. (66 years, male, Chinese, married, FG1) Based on my current situation, it’s best if this condition doesn’t drag for too long, right? It’s better if I can pass on as soon as possible. I am not scared. (77 years, male, Chinese, married, FG4)
Fear of burdening family
Many patients were worried about being a burden on their family members by requiring extensive care, spending family resources or causing emotional distress. As a result, patients based their care decisions on what they believed would be best for their family. Most patients valued the support and care they received from family members and also recognized that family members may be upset by the idea of the patient being cared for in an institution. Others wanted to avoid burdening their family members with care responsibilities. Family was also a primary concern when participants considered whether they would want to receive life-prolonging treatments or not. Some participants preferred life-prolonging treatments, as they felt that they still had responsibility for the family, especially if they were the main source of income. The prevailing attitude in most FGs, however, was that it would be better to pass away and not be a burden on family if one’s condition were to worsen significantly.
For me, I don’t want to be a burden to my family… so I’m looking for alternative situations… substitute caregiver. (57 years, male, Chinese, married, FG3) Besides troubling yourself, you will also trouble others when you aren’t able to feed yourself and have to lie on the bed the whole day, depending on others to wait on you. In such situation, everyone will pray to God to take them away to avoid troubling everyone and the society. (74 years, male, Chinese, married, FG4)
Discussion
The six themes (physical and psychological symptoms; financial concerns; uncertainty and lack of knowledge about disease; difficulties in navigating the healthcare system; end-of-life care concerns; and fear of burdening family) elicited in our study are suggestive of the experiences and concerns of patients with heart failure in Singapore.
Many patients in our sample were elderly and had multiple comorbidities, for which they had to consult multiple physicians and take several medications. In addition to the difficulties in adhering to complex regimens, this increases the risk of medical errors and adverse drug reactions.17,18 This risk is further increased as a result of inadequate discussions between patients and physicians regarding treatment plans, expected side effects and prognosis. Better provision of primary care services, in which patient’s multiple comorbidities can be managed by one family physician, would save money for the patient, improve health care coordination and thus potentially decrease the risk of complications. These primary care physicians would be backed by specialized tertiary care heart failure services to which patients can be referred in the case of acute deterioration of the condition. The development of clinical guidelines and training of primary care physicians in the comprehensive management of heart failure will improve the quality of care provided at the primary care level. Efforts to improve the responsiveness of the health care system by reducing waiting and appointment times and improving coordination between providers will further contribute to patient satisfaction. The establishment of patient-centered medical homes for patients with heart failure, similar to those in the USA, may be another way forward. Such medical homes are service-delivery systems, which are guided by the philosophy of delivering patient-centered care that is led by the patient’s personal physician, delivered in a coordinated manner, and focused on quality and safety.19,20
Our results highlight the financial burden among patients with heart failure. The financial implications of heart failure are one of the least-discussed aspects of this illness in the literature. This is partly because, in many countries, a majority of the cost is either borne by health insurance (e.g., in the USA), or care is provided by publicly financed health care services (e.g., in the UK and Canada). By contrast, in many Asian settings, including Singapore, a majority of end-of-life treatment costs are paid out of pocket. Though the Singaporean government is now introducing Medishield Life, a catastrophic government health insurance plan that provides some coverage for large hospital bills for the very old, its impact on patient’s access to health care services remains to be seen. 21 Nevertheless, comprehensive universal health coverage of primary care services for the management of heart failure will not only reduce financial hardships, but also help to reduce inequities in the provision of health care based on the ability to pay, and thus prevent dissatisfaction among patients.
Though patients are sometimes afraid of asking questions and thus relinquish decision-making to their family or doctors, they do need more information regarding disease management and progression for both themselves and their caregivers. While support groups for patients and their caregivers may promote exchanges of information and experiences, physicians and other health care providers need to be proactive in providing patients with detailed information about their disease and its management, and in eliciting patients’ treatment preferences while still involving family members in the discussions.
There are situations when family members request that the physician withhold the diagnosis and/or prognosis from the patient. Physicians may comply with this request, for fear of upsetting the family. In such situations, physicians should make efforts to initiate the difficult conversation with patients, explore their treatment preferences and involve them in decision making as much as possible. Specific training in such communication skills for primary care physicians and specialists would not only improve patient satisfaction, but also reduce patient and caregiver anxiety, increase their trust of their physician and empower them to make their own decisions.22–25 Communication models developed in Western settings may not be directly applicable to Asian settings and need to be adapted to involve family caregivers in the conversation. A good example is how the “respecting choices model” for ACP has been adapted in Singapore to include family members in the ACP discussions. 26
While the variation in end-of-life preferences was evident from the discussions, patients who had undergone ACP reported that it enabled them to make and document decisions for their end-of-life care. However, research is needed to assess whether ACP also enables patients and their families to meet their preferences at the end of the patients’ life. Apart from ACP, rigorous assessment and evaluation of various other health care service models, as well strategies for communication among patients with heart failure with respect to patient and caregiver outcomes, will also be needed.
The qualitative approach of this study aimed to provide an in-depth understanding of the experiences of patients with heart failure in Singapore; however, a limitation of this approach is that the results are not generalizable. Other potential weaknesses of this study were that patients were recruited from a single center and that a majority of them were in NYHA functional class I or II, meaning that the views of patients with more advanced heart failure were likely underrepresented. Patients in the FGs were younger than the average age of patients with heart failure in Singapore reported in other studies.27–29 Ethnic Malays were under-represented as the discussions were not held in Malay. Despite these limitations, the results will be used to develop studies which further explore the care preferences of patients with heart failure and assess the quality of care provided.
Conclusion
The study shows six primary concerns of patients with heart failure: physical and psychological symptoms; financial concerns; uncertainty and lack of knowledge about disease; difficulties in navigating the healthcare system; end-of-life care concerns; and fear of burdening family. These suggest a need for the provision of comprehensive health care services at the primary care level, training health care providers in communication skills, involving patients and their families in decision making, and the discussion of end-of-life care preferences.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
