Abstract
Objective:
The purpose of this study was to evaluate the performance of three severity scoring tools and procalcitonin (PCT) in severity stratification and mortality prediction among patients with community-acquired pneumonia (CAP) in Singapore.
Methods:
The method used was a retrospective observational study of all the consecutive patients with CAP admitted through the emergency department of Singapore General Hospital between 2012–2013.
Results:
Among 1902 study subjects, the overall 30-day mortality was 15.7%. The mortality rates for Pneumonia Severity Index (PSI) class I–III were 0, 0, and 3.7%, which were comparable to the original published data. CURB-65 and CRB-65 had higher mortality rates in all severity levels. In three levels of risk stratification, the low risk group of PSI (class I–III) included 42.6% of the patients with mortality rate of 1.9%, whereas the low risk group defined by CURB-65 (score 0–1) and CRB-65 (score 0) included 52.0% and 24.4% of the patients with higher mortality rates (7.3% and 4.5% respectively). PSI was the most sensitive in mortality prediction with area under receiver operating characteristic (ROC) curve of 0.82, higher than CURB-65 (0.71), CRB-65 (0.67), and PCT (0.63) (p<0.001). The initial level of PCT was higher in non-survivors and intensive care unit (ICU)-admitted patients compared to survivors (0.91 vs 0.36 ng/ml, p<0.001) and non-ICU patients (3.70 vs 0.38 ng/ml, p<0.001). Incorporating PCT did not improve the discriminatory power of the scoring tools for mortality prediction.
Conclusions:
PSI was a reliable tool for severity stratification and morality prediction among the patients with CAP in Singapore.
Introduction
Community-acquired pneumonia (CAP) is one of the most common infectious diseases worldwide. It is associated with considerable mortality and morbidity, especially in elder patients and patients with comorbidities.1,2 Pneumonia represents a significant health issue in Singapore. It is the fifth most common cause of hospitalizations and the second principle cause of death, leading to 13,000 admissions and over 3000 deaths annually, consisting of 18.5% of total deaths. 3 The estimated direct cost of a single CAP hospitalization ranges from S$2000–16,000 (US$1400–12,000).
Pneumonia is the major respiratory disease seen in the emergency department (ED). Timely and accurate severity assessment is crucial to the initial management.4–6 To assist clinicians in giving an objective severity evaluation,7–10 two major clinical scoring tools, Pneumonia Severity Index (PSI) and CURB-65, have been developed,11,12 PSI uses 20 clinical variables to compute the severity score (Table 1). 11 The patients are then categorized into five severity classes with increasing likelihood of death within 30 days. Class I–III are low risk groups with cumulative mortality rate <1%; whereas class IV and V are intermediate and high risk groups with mortality rates ranging from 9–30%. CURB-65 is a simple severity calculator with use of only five criteria (confusion, urea respiratory rate, blood pressure, age ⩾65).12–14 CRB-65 is a simplified version of CURB-65 obtained by omitting blood urea measurement.15,16 PSI, CURB65, and CRB65 have been validated extensively and proved to be powerful in severity stratification and mortality prediction.11,12,16–20 In Europe and North America PSI and CURB-65 are incorporated into clinical guidelines as the standard of care of pneumonia.5,6,21
Comparison of the components of Pneumonia Severity Index (PSI), CURB-65 and CRB-65.

BP: blood pressure.
Procalcitonin (PCT), a systemic inflammatory protein, has appeared to be a novel prognostic biomarker of pneumonia in recent years. PCT helps to differentiate bacterial from viral infections, and guides the decision on antibiotic therapy.22–25 PCT was associated with septic shock, organ failures, and occurrence of complications in patients with pneumonia.26,27 Non-survivors and patients in the high severity class had higher levels of PCT.18,27,28 Adding PCT to PSI or CURB-65 improved the prediction of adverse complications of CAP.18,27
Despite intensive investigations worldwide, the evidence for the predictive efficacy of these severity scoring tools among Asian patients is limited with various conclusions19, 29–32 (Table 2). Man et al. have reported that PSI, CURB-65, and CRB-65 perform similarly in mortality prediction among CAP patients in Hong Kong and recommended CURB-65 in daily clinical practice because of its simplicity. 19 A Korean study, however, reported that for mortality prediction CURB-65 was more valid for less severe patients, but PSI performed better among the severe cases. 30 The only validation study conducted in Singapore selectively included patients who were 55 years or older and the study setting was not the hospital ED. 32 In view of the serious burden of pneumonia in ED and in the Singapore healthcare system, a thorough validation study is indispensable. Here we explicitly evaluated the effectiveness of PSI, CURB-65, CRB-65, and PCT on severity stratification and mortality prediction in a large cohort of patients in the hospital emergency setting in Singapore.
Summary of Asian studies on pneumonia severity scoring scales.
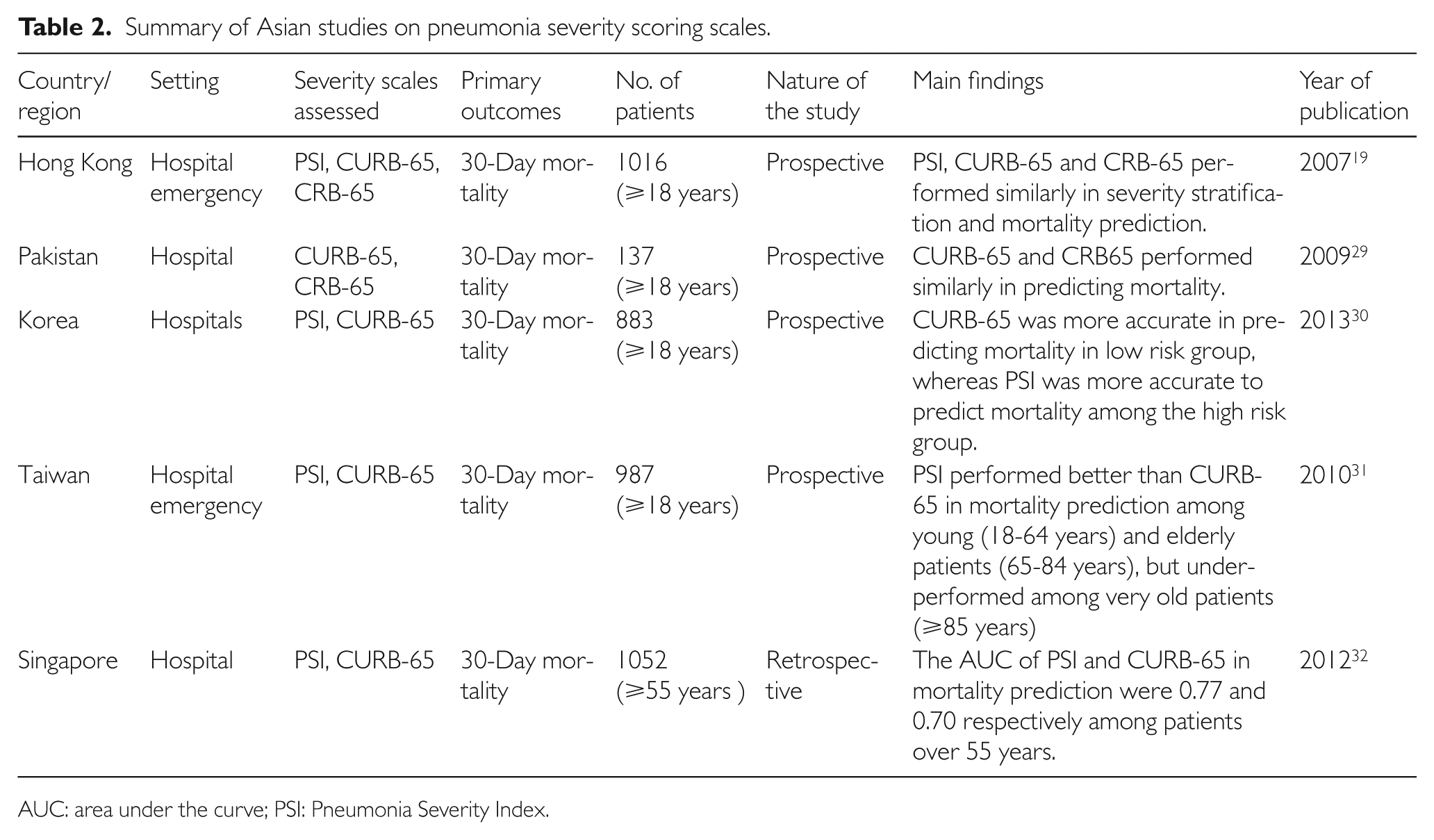
AUC: area under the curve; PSI: Pneumonia Severity Index.
Methods
Study setting and study subjects
The study was performed in Singapore General Hospital (SGH), an adult urban tertiary hospital with more than 1500 beds. The ED has approximately 130,000 non-trauma patients per year, and 10% seek medical care for respiratory symptoms.
All the consecutive patients admitted to hospital through the ED with a provisional diagnosis of pneumonia (International Classification of Diseases, 9th revision, Clinical Modification, ICD-9CM code 480.x–487.x) between 1 January 2012–31 December 2013 were included. Ethical approval and waiver of informed consent was obtained from the Centralized Institutional Review Boards of the SingHealth Authority of Singapore (2014/226/A). This study was kindly funded by SingHealth Foundation Research Grant SHF/FG590S/2013.
Data collection
The patients’ case notes were reviewed by experienced and trained research coordinators with a nursing or medical background. The 20 variables required for PSI calculation were extracted, including patients’ demographics, comorbidities, initial vital signs, laboratory test results, and chest X-ray reports. 11 All the collected data was the first reading in ED. Information on six additional chronic conditions, including ischemia heart disease, chronic obstructive pulmonary disease (COPD), diabetes mellitus, hypertension, dementia, and Parkinson’s disease were collected as well. The level of PCT measured within the first 24 h of admission was taken as the initial level of PCT.
Pneumonia definition and exclusion criteria
Pneumonia was defined as an acute infection of the lung parenchyma characterized by symptoms of acute respiratory infection and the presence of an acute pulmonary infiltrate on chest X-ray or abnormal auscultatory findings. 33 Patients with human immunodeficiency virus (HIV) infection, pulmonary tuberculosis, cystic fibrosis, or were on long term immunosuppressant or steroid treatment were excluded.
Severity score calculation and stratification
The scores of PSI, CURB-65, and CRB65 were calculated according to original studies.11,12 Patients were subsequently stratified into three levels of risk groups:11,12,19 (a) PSI: low risk (classes I-III); intermediate risk (class IV); and high risk (class V); (b) CURB-65: low risk (scores 0–1); intermediate risk (score 2); and high risk (scores 3-5); (c) CRB65: low risk (score 0); intermediate risk (score 1–2); and high risk (score 3–4).
The primary outcome, all-cause mortality at 30 days after hospital admission were compared. Length of stay (LOS) in hospital was analyzed as well.
Statistical analysis
Categorical variables were expressed as counts (percentages) and continuous variables as mean±standard deviation (SE) or median with 25–75th quartile range) if the data were not normally distributed. Frequency comparison was done by chi-square test. For non-parametric continuous variables, Mann-Whitney U test or Kruskal-Wallis test was used respectively. Receiver-operating characteristic (ROC) curve analysis was performed to evaluate the discriminatory power of the risk scores and PCT on mortality prediction. Area under the curve (AUC) and 95% confidence interval was computed. Standard sensitivity, specificity, positive, and negative predictive values were calculated at various cut-offs. Adopted from previous studies,18, 27 the initial level of PCT was stratified into the 4 ranges, which were <0.12, ⩽0.12<0.25; ⩽0.25<0.5, and ⩾0.5 ng/ml (0.12 ng/ml was the lowest detection limit of the PCT assay). To test whether incorporating PCT improved the predictive performance of the risk scores, joint logistic regression and ROC curve analysis were conducted as other studies described.18,27 All statistical tests were two-tailed. Values of p<0.05 were considered significant. All calculations were performed using SPSS, version 20 for Windows.
Results
In the two-year study period, a total of 3224 patients in ED received ICD-9-CM code 480 (pneumonia viral), 482 (bacterial pneumonia), 485 (bronchopneumonia), and 486 (pneumonia unspecified) as the primary diagnosis (Figure 1). Among them, 347 patients were discharged from ED right after the treatment. Of 2841 admitted patients, 1902 patients satisfied the study criteria and comprised the study cohort; 939 patients were excluded either because they were not pneumonia or they fulfilled the exclusion criteria. The 30-day mortality data was kindly provided by National Registry of Disease Office, Health Promotion Board Singapore.

Study design. ICD: international classification of diseases; ED: emergency department.
Patients’ demographic information and baseline clinical features were summarized in Table 3. All the cut-off values in physical examinations and laboratory tests were recommended by Fine et al. in their original paper for PSI calculation. 11 The overall 30-day mortality rate was 15.7%. Intensive care unit (ICU) admission rate was 5.8%. The median length of hospital stay was four days with 25th–75th interquartile range (IQR) of 2–8 days.
Baseline characteristics and outcomes of study subjects.

COPD: chronic obstructive pulmonary disease; ICU: intensive care unit; IQR: interquartile range; LOS: length of stay; SD: standard deviation; TB: tuberculosis.
Data are presented as n (%) unless other stated. All the cut-offs in physical examination and laboratory findings are recommended by Fine et al. for PSI calculation. 11
The 30-day mortality rates for PSI class I–III were 0, 0, and 3.7%, which were comparable to the original data, whereas PSI class IV and V had significantly higher mortality rates (Table 4). For CURB-65 and CRB-65, the mortality rates were significantly higher for all severity levels than the original study. In three-level risk stratification, the low risk group of PSI (class I–III) included 42.6% of the subjects with the mortality rate of 1.9% (Table 5); whereas CURB-65 (score 0–1) included more patients (52.0%) with significantly higher mortality rate (7.3%, p<0.001); CRB-65 (score 0) included substantially fewer patients (24.4%), whereas the mortality rate was much higher (4.5%). The median LOS increased significantly with increasing risk levels (p<0.001).
30-Day mortality rates and intensive care unit (ICU) admission rates in each severity level of Pneumonia Severity Index (PSI), CURB-65 and CRB-65.

Data are numbers and percentages of the total study subjects (n=1903).
Data are numbers and percentages of the subjects under each severity level.
30-Day mortality and length of stay (LOS) in three-level risk categories of Pneumonia Severity Index (PSI), CURB-65 and CRB-65.

The number and percentage of the total study subjects (n=1977).
The number and percentage of the subjects under each risk class, and it was tested by chi2 test.
LOS in hospital was presented as median (25th–75th interquartile range) as it was not normally distributed, and was tested by Kruskal-Wallis test.
The level of PCT within 24 h of admission was available in 1410 patients (Table 6). The median level of PCT significantly increased with increasing risk levels in all tested scoring scales (p<0.001). Non-survivors had significantly higher levels of PCT than the survivors (0.91 µg/l vs 0.36 µg/l, p<0.001); so did the patients who were admitted to ICU when compared with those who had ICU admission (3.7 ug/l vs 0.38 ug/l, p<0.001).
Procalcitonin (PCT) levels in different severity classes and major clinical outcome groups.

ICU: intensive care unit; IQR: interquartile range; PSI: Pneumonia Severity Index.
The level of initial PCT is presented as median (25th–75th IQR). The difference in PCT levels between severity levels were compared using non-parametric Kruskal-Willis test.
Sensitivity, specificity, and positive and negative predictive value (PPV and NPV) for prediction of 30-day mortality at different cut-offs for each severity score and PCT are shown in Table 7. PSI gave the most sensitive prediction of mortality at all cut-offs (100%, 100%, 100%, 95.0%, and 47.8%) with the highest NPV (NA, 100%, 100%, 98.1%, and 90.0%). Initial level of PCT appeared to be the poorest in prediction of 30-day mortality.
Sensitivity, specificity, positive predictive values (PPVs) and negative predictive values (NPVs) for 30-day mortality prediction at different cut-offs for each severity scoring tool and procalcitonin (PCT).

NA: not available; PSI: Pneumonia Severity Index.
The ROC curves for prediction of 30-day mortality for each scoring tool were shown in Figure 2. AUC of PSI was 0.82 (95% CI: 0.80–0.84), which was significantly higher than CURB-65 (AUC 0.71, 95% CI: 0.68–0.74) and CRB-65 (AUC 0.67, 95% CI: 0.63–0.70). The AUC of PCT was 0.63 (95% CI: 0.59–0.67) for mortality prediction, which was the lowest among the tested scoring tools (Figure 3). Incorporating PCT did not further improve the discriminatory power of the scoring tools on mortality prediction (p>0.05).

Receiver-operating characteristic (ROC) curves of Pneumonia Severity Index (PSI), CURB-65, and CRB-65 with respect to prediction of 30-day mortality. AUC: area under the curve; CI: confidence interval.

Receiver-operating characteristic (ROC) curves of procalcitonin (PCT) and combined PCT with Pneumonia Severity Index (PSI), CURB-65, and CRB-65 respectively with respect to prediction of 30-day mortality. AUC: area under the curve; CI: confidence interval.
Discussion
This was the first large scale validation study to evaluate the performance of the three severity scoring tools and PCT in severity stratification and mortality prediction in hospital emergency department setting in Singapore. In comparison to CURB-65 and CRB-65, PSI was more accurate in defining patients in low risk classes and more sensitive in mortality prediction. PSI classified reasonable proportion of patients into the low risk group with comparable mortality rate to the original published data and other subsequent studies.11,17,19,34 Conversely, CURB-65 and CRB-65 underestimated the severity and miscategorized some patients with high risk of death into the low risk classes. Our finding was consistent with many previous studies.17,35,36 A systematic review and meta-analysis which screened 402 articles and included the retrieved data from 23 studies also concluded that PSI was superior to CURB-65 and CRB-65 in mortality prediction and more accurate in identifying non-severe patients with low risk of death. 37
PSI makes use of 20 variables ranging from clinical presentations, laboratory test results, and radiological findings to compute the severity score. The estimation is generally more accurate and sensitive than CURB-65 and CRB-65 although the process of information collection and score computation is complicated and time-consuming. 37 However, the performance of scoring tools varies from population to population. Different clinical characteristics and racial composition of the patients could result in various ranking. Therefore, thorough validation study among a particular population is critical.
Patients in PSI class I and II can be safely treated as outpatients.11,36 In this study more than 20% of the study subjects were in these two severity classes. They were much younger with less chronic conditions (data not shown). Should some of these patients be cared for in an outpatient setting, the admission rate, and the usage of healthcare resources would be markedly decreased. We also noticed that patients in high severity classes had much higher mortality rates compared to the original studies where the severity scores were derived and validated.11,12 The factors leading to this discrepancy could be complicated. Low ICU admission rate could be one of the reasons. In this study approximately 85% of the deaths occurred before hospital discharge (data not shown). For patients in intermediate and high severity classes, the frequencies of ICU admission were significantly lower than the mortality rates (Table 4) which meant many severe patients died with no intensive care received. As is known that many factors play a crucial role in the decision on ICU admission, patient’s age, coexisting diseases, long-term prognosis etc. are often the determinant factors besides the severity of disease. Elderly patients with multiple comorbid diseases, especially the diseases with extremely poor prognosis would have less opportunity of being admitted to ICU because they may not have long-term benefit from ICU care. 38 Moreover, patients’ social and economical status and support have a big influence on patients’ clinical management and outcome.
In addition to the severity scoring tools, we evaluated the prognostic value of PCT. Here PCT showed significant association with the severity of pneumonia which was consistent with the published data, that patients with high severity score had higher initial PCT level.20,27,39,40 However, PCT was not a good predictor for mortality in our patient cohort. Huang et al. and Schuetz et al. have also reported that initial PCT had significantly lower discriminatory power in mortality prediction compared to PSI and CURB-65.18,27 Adding PCT could not improve the performance of the scoring tools in prediction of mortality.18,27
The study had limitations. Firstly, the study was not novel. PSI and CURB-65 have been developed for more than a decade. Numerous validation studies have been performed worldwide, especially among western nations. In Singapore, however, this was the first large validation study conducted in hospital emergency setting among adult patients. The clear findings may bring significant clinical impact, especially on lowering the admission rate and medical cost of pneumonia. Secondly, the study used the retrospective design. All the data were extracted from case-note review, which was not as accurate as information directly collected through face-to-face interview or questionnaire. However, a retrospective study is quick, economical, and easy to conduct, a good method for a pilot study. Thirdly, there was no stringent exclusion of healthcare associated pneumonia (HAP) because of the lack of data on patients’ hospital admission history prior to the episode we studied. Fourthly, not all study subjects had PCT value for the analysis of the mortality predictive value, and the time of blood sample taken for PCT measurement varied although all the reported levels of PCT in this study were measured within 24 h of admission. Serum PCT changes dynamically over time. Ideally all the blood samples should be taken at the same time. However, it is very difficult to achieve this in a retrospective study. Another limitation we would like to mention was the exclusion of non-hospitalized patients with compatible ICD-9 code (383 out of 3224 patients) because in the pilot study we found that majority of these patients were short of positive radiological support for the diagnosis of pneumonia or they did not have the necessary laboratory test results for computing PSI and CURB-65 score (data not shown). Unfortunately we still missed a small proportion of patients who had mild pneumonia and were treated as outpatients. This could produce a selection bias since hospitalized patients were generally more severe. However, PSI in this study was able to accurately identify the mild cases with low risk of death among the hospitalized patients. If un-hospitalized mild cases were included into the analysis, the mortality rate of the low risk group could be even lower. Therefore, the conclusion of study would not be affected. The main strength of the study lay in the size of the study cohort, which was comparable or even larger than many published data. 37 Meanwhile, we retrieved patient clinical data through case-note review, and the findings would be more accurate and informative than those data obtained merely by matching ICD code.
In conclusion, PSI was a valid and reliable scoring system for severity stratification and mortality prediction in patients with pneumonia in Singapore despite its complexity and cumbersomeness. Implementation of PSI into daily clinical practice would help to guide the management of pneumonia, reduce unnecessary admission and improve the efficiency of medical resource usage. Further prospective validation study is still required.
Footnotes
Acknowledgements
The authors wish to thank Shen Lian in the Biostatistics Unit, Yong Loo Lin of the School of Medicine, National University Health System for their assistance in biostatistical analysis. The authors are also grateful to the National Registry of Diseases Office, Singapore Health Promotion Board for providing 30-day mortality data.
Conflict of interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
