Abstract
Background:
Children with Down syndrome have an increased burden of respiratory infections. We hypothesized that children with Down syndrome hospitalized for bronchiolitis would stay longer compared with children without Down syndrome.
Methods:
We conducted a retrospective case–control study of children with Down syndrome who were hospitalized for bronchiolitis in Singapore from 2004 to 2012.
Results:
There were 27 and 43 admissions in the Down syndrome and control groups respectively. More children with Down syndrome had congenital heart defects (14 (52%) vs. none in controls). Children with Down syndrome stayed longer in hospital compared with controls (7 (interquartile range (IQR) 5–14) vs. 3 (IQR 2–4) days, p<0.001). In a subgroup analysis of patients without or surgically corrected congenital heart defects, children with Down syndrome still had a longer stay (6 (IQR 5–8) vs. 3 (IQR 2–4) days, p<0.001).
Conclusion:
Our study suggests that children with Down syndrome hospitalized for bronchiolitis stayed longer in hospital compared with those without Down syndrome.
Introduction
Down syndrome is one of the most common genetic syndromes worldwide. 1 Children with Down syndrome have been demonstrated to have increased burden of respiratory tract infections such as bronchiolitis.2,3 Previous studies performed in temperate regions demonstrated that children with Down syndrome with lower respiratory tract infections had higher rate of hospitalization compared with children without Down syndrome.4,5 We undertook this study to examine the clinical burden of bronchiolitis among children with Down syndrome in Singapore. Our primary hypothesis is that children with Down syndrome who were admitted with bronchiolitis require more support and stay in hospital longer compared with age-matched children without Down syndrome.
We conducted a retrospective case–control study in KK Women’s and Children’s Hospital, Singapore. Cases were patients ⩽ 2 years old with Down syndrome hospitalized with primary diagnosis of bronchiolitis between 2004 and 2012.
Methods
Controls were age-matched patients without Down syndrome hospitalized with acute bronchiolitis within seven days of admission date of the index cases (patients with Down syndrome who were admitted for bronchiolitis). Baseline demographics, co-morbidities and the clinical course of hospitalization were recorded for both groups. All patients’ nasopharyngeal aspirate was tested for respiratory virus antigen by immunofluorescence technique. We defined haemodynamically significant congenital heart defects (CHDs) as all CHDs except small atrial septal defect and small patent ductus arteriosus. We described the severity of the bronchiolitis using the modified Wood’s clinical asthma score. 6 A higher score (maximum of 12) indicates worse respiratory distress.
Our primary outcome was hospital length of stay (LOS). Other outcomes were need for high dependency and intensive care unit admissions. We performed subgroup analysis by excluding those with CHD in the Down syndrome group who had not undergone corrective cardiac surgery prior to the episode of bronchiolitis. Corrective cardiac surgery is defined as any surgery that restores the heart structure and circulation to normal physiology. We also performed a subgroup analysis of all patients with respiratory syncytial virus (RSV) infection.
This study was approved by the institutional review board in our hospital and informed consent was waived.
We described categorical variables in absolute numbers and percentages. Continuous variables were summarized as medians and interquartile ranges (IQRs). Categorical variables were compared using Pearson chi square tests while continuous variables were compared using Wilcoxon rank sum tests. A value of p < 0.05 was considered significant. Statistical analysis was performed using Stata version 12.1 (College Station, TX, USA).
Results
Over the period of eight years, there were a total of 27 admissions (number of children=25) in the Down syndrome group. Two patients with Down syndrome were hospitalized twice for bronchiolitis. Random selection for age-matched controls identified 43 admissions (number of children=43) in the control group (Table 1). Median age of both groups (n=70) was eight (IQR 4–12) months. Median gestational age at birth was 37 (IQR 37–38) weeks. In all our admissions (n=70), the most common presenting symptoms were cough (97%) and coryza (84%). In the Down syndrome group, 10 (37%) were found to have RSV infection. In the control group, 18 (42%) were found to be positive for RSV.
Demographics of children in Down syndrome and control groups.

All continuous variables described in median and interquartile ranges.
CHD: congenital heart disease; DS: Down syndrome; RSV: respiratory syncytial virus.
Fourteen (52%) in the Down syndrome group had CHD compared with none in the control group (p <0.001). Most of the patients with CHD had acyanotic heart defects (n=11); the most common CHD was ventricular septal defect (n=4). Only one patient in the Down syndrome group had immunodeficiency due to chemotherapy for leukaemia. Median oxygen saturation at admission for both groups was within normal range. Median Wood’s score in all the admissions was 1 (IQR 1–1).
Patients with Down syndrome had a longer hospital LOS compared with the control group (7 (IQR 5–14) vs. 3 (IQR 2–4) days, p<0.001). In the Down syndrome group, six (22%) required high dependency care and two (7%) required intensive care. In the control group, only one (2%) required high dependency care and none needed intensive care. In the RSV subgroup analysis, patients with Down syndrome had a longer hospital LOS compared with the controls. (6.5 (IQR 5–8) vs. 3.5 (IQR 3–4) days, p<0.001).
Because of the significant difference in proportion of CHD between our groups, we further analysed the data by excluding those with CHD in the Down syndrome group who had not undergone corrective surgery prior to the episode of bronchiolitis. We assumed that children with CHD had undergone full corrective surgery to be equivalent to those without CHD. In this analysis, there were 19 admissions in the Down syndrome group and 43 admissions in the control group (Table 2). In this subgroup analysis, patients in the Down syndrome group (without CHD) still had a longer hospital LOS compared with controls (6 (IQR 5–8) vs. 3 (IQR 2–4) days, p<0.001). Within the RSV subgroup, patients in the Down syndrome group similarly had a longer hospital LOS compared with the control group. (6.5 (IQR 5.5–8) vs. 3 (IQR 2–4) days, p<0.001).
Demographics of Down syndrome group excluding those with haemodynamically significant congenital heart disease without corrective surgery and control group.
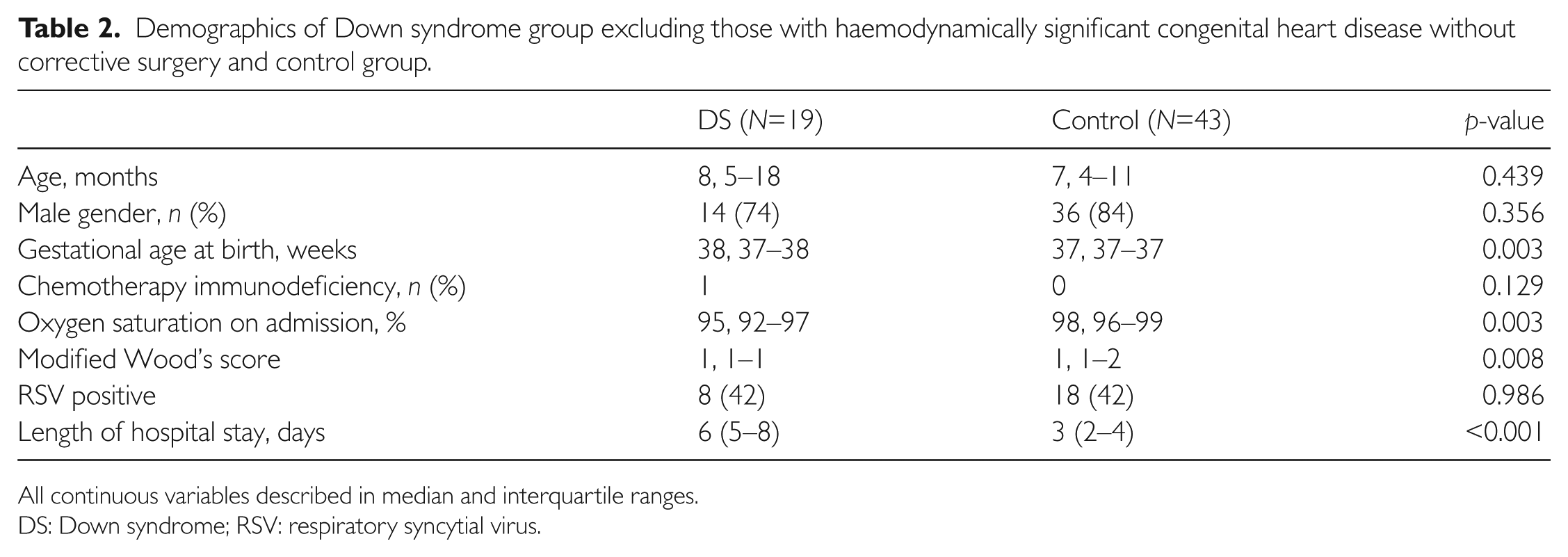
All continuous variables described in median and interquartile ranges.
DS: Down syndrome; RSV: respiratory syncytial virus.
Discussion
Our study demonstrated that children with Down syndrome who were hospitalized for bronchiolitis stayed longer than those without Down syndrome. Even after excluding those with haemodynamically significant CHD, the difference in hospital LOS remained significant.
Previous studies have demonstrated that children with Down syndrome with RSV bronchiolitis and lower respiratory tract infections had a higher risk of hospitalization.4,5,7,8 (Table 3). Our study supports the hypothesis that children with Down syndrome with lower respiratory tract infections require more clinical resources compared with those without Down syndrome.
Studies on morbidities due to respiratory infections among children with Down Syndrome.

DS: Down syndrome; RSV LRTI: respiratory syncytial virus lower respiratory tract infection; CHD: congenital heart defect; OR: odds ratio; CI: confidence interval.
Children with Down syndrome have more-severe lower respiratory tract infections due to a few possible reasons. Children with Down syndrome have been demonstrated to have persistent pulmonary hypertension even in the absence of CHD. 9 Viral respiratory infections can worsen underlying pulmonary hypertension. T-cell and B-cell lymphocytes dysfunction and immunoglobin G subclass deficiencies observed in children with Down syndrome 10 may cause more-severe respiratory infections. Children with Down syndrome have an increased baseline risk of aspiration which is exacerbated by bronchiolitis. 11
CHD is a known risk factor for severe RSV infection. 12 Because of this potential confounding factor, we performed a subgroup analysis by excluding those in the Down syndrome group with haemodynamically significant CHD without corrective surgery because we felt that surgically repaired CHD and haemodynamically insignificant CHD should pose minimal risk to severe bronchiolitis. When this group is compared with the control group without risk factors, Down syndrome is still associated with longer hospital LOS. Our study findings were consistent with two previous studies.4,5 After adjusting CHD, pulmonary hypertension, chronic lung disease and prematurity, Bloemers et al. 4 and Zachariah et al. 5 demonstrated that children with Down syndrome and RSV bronchiolitis had higher morbidities compared with children without Down syndrome. Although our study was not limited to RSV infection, RSV was the most common pathogen detected (40% of all the patients). Even within our patients who tested positive for RSV, patients with Down syndrome still had a longer hospital LOS compared with controls.
Yi et al. reported that palivizumab (immunoprophylaxis for RSV infection) was associated with a 3.6-fold reduction in incidence rate ratio for hospitalization related to RSV infection for children with Down syndrome in the temperate region. 13 However, the American Academy of Pediatrics subcommittee for clinical practice guidelines for bronchiolitis concluded that there is insufficient evidence to justify offering routine palivizumab to children with Down syndrome unless they have other established risk factors such as CHD or prematurity. 14 Bronchiolitis is a perennial medical problem in tropical region with no particular variation. 15 The decision to give palivizumab to children with Down syndrome is more challenging in Singapore because we cannot select a particular period to give the monoclonal antibody. This makes the cost–benefit ratio of palivizumab unfavourable in our setting.
In our study, there was a significant longer hospital LOS for the Down syndrome group even though there was no clinical significant difference in Wood’s score during admission. Upon further analysis, we noted that 26% (7/27) of the patients in the Down syndrome group received intravenous antibiotics for secondary bacteria pneumonia and 22% (6/27) in the same group received intravenous drip or nasogastric tube feeding for poor feeding. In the control group, only 14% (6/43) received intravenous antibiotics and 5% (2/43) received intravenous drip or nasogastric tube feeding. All the management decisions were based on physicians’ opinions. There was an apparent higher incidence of secondary bacteria pneumonia and poor feeding among the Down syndrome group and that might have delayed hospital discharge. Our study is limited by its small sample size. Subgroup analysis for different CHDs and different oxygen saturation on admission was not performed due to the small sample size. Most of our patients had mild respiratory distress (median Wood’s score ⩽ 4) at initial assessment. The number of patients requiring medical care beyond the care of a general ward was also small. The data collection is done in a retrospective manner and cases were identified based on diagnostic coding therefore there might be missing cases due to inaccurate classification and recording. On the other hand, some of the patients might have had a recurrent wheezing episode due to evolving infantile asthma that had not been diagnosed during the hospitalization.
Conclusion
Patients with Down syndrome who were hospitalized for bronchiolitis stayed longer in hospital compared with those without Down syndrome. This increase in LOS was also demonstrated in children with Down syndrome without significant CHD. Moving forward, a prospective study with a larger sample size will provide more robust evidence on this subject.
Footnotes
Conflict of interest
None declared.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
