Abstract
This article reviews the current monitoring and management options for raised intracranial pressure (ICP), primarily in traumatic head injuries, in line with current literature and guidelines. The use of ICP monitoring is useful in managing, predicting outcomes, following the progression and guiding interventions of neurological disease states.
Patients with raised ICP should be monitored closely in a neurocritical care setting where appropriate interventions can be instituted based on available monitoring parameters. Various first- and second-tier methods should be considered, with the primary goal to decrease secondary insult to brain tissue for best outcomes.
Introduction
Neurocritical care has evolved with better treatment and diagnostic modalities. In addition to neurological examination, intracranial pressure (ICP) monitoring has been shown to be useful in the management of acute neurological states to follow the progress of acute intracranial disease, guide interventions and predict outcomes, especially in traumatic brain injuries (TBI). 1
ICP
ICP is defined as the pressure within the cranium which is exerted on the brain tissue by external forces such as blood and cerebrospinal fluid (CSF). Normal ICP varies according to age and ranges between 5 mmHg and 15 mmHg in adults. 2
Conditions associated with increased ICP 3
There are many ways to categorize causes of raised ICP. An intuitive approach would be to classify the various conditions under pathophysiological aetiologies as espoused by the Monro-Kellie doctrine, which will be elaborated below. There may be overlaps in these various categories (Table 1).
More common, representative conditions associated with increased ICP.

ICP: intracranial pressure; CSF: cerebrospinal fluid.
The Monro-Kellie doctrine
The Monro-Kellie doctrine describes the principle of homeostatic intracerebral volume regulation. The total volume of brain parenchyma, CSF, and blood is relatively constant. Increase in one of these three components beyond a compensated range results in intracranial compliance shifting from a near linear relationship to an exponential relationship where small changes in volume result in large changes in ICP (Figures 1 and 2).

Intracranial compliance curve.

Theoretic intracranial compliance curves.
The brain is anatomically compartmentalized by the dural reflections of the falx cerebri and tentorium cerebelli. Raised ICP frequently results in pressure gradients between compartments and possible herniation of brain structures.
Raised ICP can occur acutely or gradually. Many clinical syndromes of raised ICP are the consequence of the rapidity of change rather than the absolute level of ICP. Three types of intracranial herniation are generally recognized: transtentorial (either lateral or central), tonsillar, and subfalcine. Cerebral herniation can present with varying neurological symptoms, although somnolence and a drop in Glasgow Coma Score (GCS) are common. The patient could present with new localizing signs and symptoms such as unilateral motor or sensory findings. Herniation of the uncus of temporal lobe between the rostral brainstem and tentorial edge into the posterior fossa results in progressively impaired consciousness, dilated ipsilateral pupil, and contralateral hemiplegia. Herniation of the cerebellar through the foramen magnum into the upper spinal canal compresses the medulla and eventually results in cardiorespiratory impairment, hypertension, high pulse pressure, Cheynes-Stoke respiration, neurogenic hyperventilation, impaired consciousness, and death.
Types of ICP monitors
Both invasive and non-invasive methods of monitoring ICP are available. Invasive monitors can be classified into intraventricular and intraparenchymal devices.
Intraventricular catheters are the gold standard for monitoring ICP as they measure global ICP, while allowing in vivo calibration and therapeutic drainage of CSF. However, its insertion may be technically more challenging. The catheter may be attached to an external microstrain gauge and external transducer, allowing intermittent ICP measurement, or an in-line catheter which allows simultaneous pressure monitoring and drainage.
In comparison, ICP monitors which are inserted into brain parenchyma work through the use of fibre-optic, strain gauge or pneumatic technologies. The accuracy of the devices is dependent on their placement relative to the site of injury. 2 They can be easily placed via a cranial access device, burr hole or during a craniotomy. However, they may not be a good gauge of global ICP if pockets of raised ICP arise due to focal brain injuries. Microtransducer systems can also encounter drift when used long term, and in vivo calibration is not possible. 5
Other less-commonly used ICP monitors include subdural and epidural monitors. Adjuncts to ICP monitoring include brain tissue oxygenation monitors, microdialysis catheters, and jugular venous saturation monitors.
Two emerging non-invasive ICP monitoring methods include measuring the optic nerve sheath diameter 6 (ONSD) as seen on an ultrasound probe placed on the superolateral aspect of the orbit and the pulsatility index (PI) which is calculated from transcranial Doppler studies (TCD). Their validation and incorporation into regular ICP management is still yet to be conclusive as they are technically challenging, operator dependent and might not be useful for point-of-care use.
Indications for ICP monitoring
Invasive ICP monitoring is associated with risks and its use varies across institutions. 2
ICP monitoring is useful to calculate cerebral perfusion pressure (CPP), which is defined as the difference between the mean arterial pressure (MAP) and the ICP. CPP is an important surrogate for determining adequacy of brain perfusion, and as an endpoint for goal-directed therapy. It is a global measurement but does not provide insight into regional differences in perfusion. The presence of ischaemic or metabolic distress can occur at apparently adequate CPP.
Intracranial hypertension is directly associated with worse outcomes in TBI. Therefore, an absolute measure of ICP allows it to be an endpoint in goal-directed therapy, whereby ICP should be aimed at a value of less than 20 mmHg and values above 25 requiring treatment.
The merits and utility of ICP monitoring in improving patient outcomes have been somewhat controversial and have been recently highlighted in a study by Chesnut et al. 7 of severe head injury patients admitted to intensive care units in South America, where they were randomized to either ICP-based treatment or treatment based on clinical examination and concurrent imaging findings. There is a suggestion that management of TBI based on ICP monitoring with a goal ICP of not more than 20 mmHg was not superior to management based on imaging and clinical examination alone. The mortality, adverse events, and the primary outcome of functional and cognitive scores at six months were not significantly different between these groups. 8 This may call into question the routine use of ICP monitoring, the siting of which is not entirely risk free.
This study, however, has limitations which include a lack of details of pre-hospital and post-discharge care, and using of unvalidated scoring tool to measure a primary endpoint. There are also concerns whether these findings can be extrapolated to other countries since there is variation in pre-hospital, in-hospital and rehabilitation services, since these differences may affect outcomes.
There is, however, insufficient evidence to abandon the use of ICP monitoring. ICP monitoring can and should be used in a multi-modal approach for patients with neurological injuries for whom the use of invasive intracranial pressure monitoring and specific management based on monitored ICP is still currently recommended,9,10 especially when there is strong clinical suspicion of increased ICP and an abnormal clinical examination. 11 ICP monitoring should therefore be viewed as an additional patient management tool.
Principles of management of patients who present with raised ICP
The interpretation and treatment of raised ICP should be in conjunction with clinical neuro-examination and hemodynamic variables such as the MAP and heart rate. These could allude to any ongoing herniation (e.g. Cushing’s reflex, ischaemic sympathetic reflex). Neuroimaging should be considered when there is a new and persistent rise in ICP or clinical deterioration, even when the initial neuroimaging may be normal, as this does not preclude development of a delayed lesion, such as oedema or haemorrhage. 2
One important principle in raised ICP management is prevention of secondary injury by avoiding hypoxia, hypercarbia and hypovolemia and hypotension. Both neurologic and functional outcomes have been shown to improve by giving due attention to these variables. 12
Treatment of raised ICP should be geared towards managing different pathological processes which resulted in the raised ICP.
The management of raised ICP is focused on four main areas: (1) control and manipulation of vaso-reactivity, cerebral blood flow (CBF) and flow-metabolism coupling; (2) managing the blood/brain osmotic gradient; (3) reducing the metabolic rate of oxygen consumption of cerebral tissue; and (4) physical/surgical modalities which affect intracranial compliance.
Figures 3 and 4 illustrate how to approach management of a patient with raised ICP. Primary management should be directed at the cause of raised ICP in the first instance, e.g. resection of tumour, insertion of external ventricular drain for hydrocephalus. Medical measures to optimize first-tier measures should be instituted before considering second-tier management.
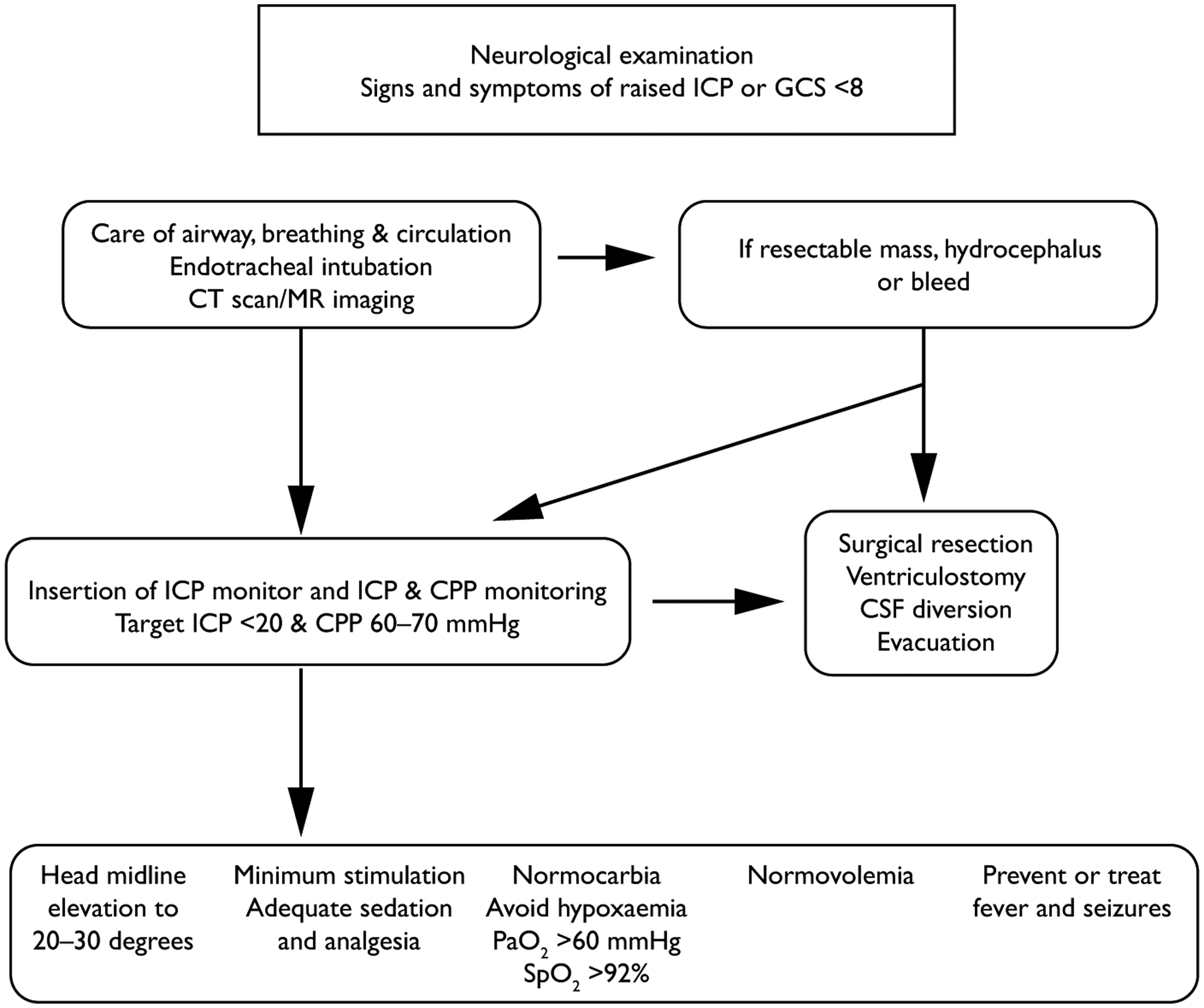
Approach to managing raised ICP.

Management of raised ICP.
The subsequent section will describe applications of the above principles in greater detail.
ICP treatment goals
The treatment goal in brain injury is to maintain a normal ICP, which is generally accepted as less than 20 cm H2O. Current guidelines by the Brain Trauma Foundation recommend that the threshold for treating ICP is 20 mmHg to 25 mmHg. Aggressive measures should be taken to prevent ICP of more than 25 mmHg or CPP less than 60 mmHg. 13
A persistent elevation in ICP is a sign of ongoing secondary injury and pathology from cerebral oedema, ischaemia, haemorrhage and hydrocephalus. There is evidence of correlation between the extent and duration of ICP elevation and poor outcomes after TBI. 14 Clinical practice guidelines recommend ICP monitoring in patients with severe TBI who are comatose (GCS score <9) after resuscitation and who either have abnormalities on computed tomography (CT) scan or meet at least two of the following three criteria: age greater than 40 years, systolic blood pressure less than 90 mmHg, or motor posturing. 15
The normal brain autoregulates CBF, which is constant at 50 ml/100 g tissue/min across a wide range of MAPs. TBI patients have abnormal cerebral autoregulation and they display pressure passive perfusion whereby the CBF varies directly with CPP. When MAP is increased, there is increased CBF and therefore increased ICP, while lower MAPs may cause hypo-perfusion and ischaemia.16,17 Conversely, raised ICP also aggravates already impaired autoregulation. 18 Therefore, with loss of protective autoregulatory mechanisms, avoidance of hypotension and hypoxia in patients with severe brain injury is paramount.
For this reason, a target CPP between 60 mmHg and 70 mmHg is aimed for. This value is chosen because it allows sufficient pressure to overcome the elevated ICP while avoiding problems associated with hypertension. To achieve this, the use of fluids or vasopressors such as norepinephrine and phenylephrine may be required. These vasopressors are preferred as they have less effect on the cerebral vasomotor tone. Overaggressive use of vasopressors and fluids to manipulate CPP to more than 70 mmHg has been associated with increased incidence of pulmonary complications and acute respiratory distress syndrome.19,20
Use of other intracranial variables
Cerebral ischaemia can occur at apparently adequate CPP and with quite normal ICP. Multimodal monitoring is therefore used to identify brain insult.
Continuous brain oxygen monitoring is accomplished by inserting a probe into the brain parenchyma. It is most often placed in perilesional brain tissue, which is most vulnerable to secondary injury. It can perform brain oxygen tension monitoring (PbtO2), which is a direct measurement of cerebral oxygen metabolism. Abnormally low brain oxygen levels are associated with poor outcome and the threshold for critical brain tissue oxygen tension is 15 mmHg, which should trigger interventions. Jugular bulb catheters are also used to measure brain oxygen by oximetry. Its use in neurotrauma patients ranges from 8 to 12% in the United States to 21% in Japan.21,22 At jugular bulb oxygen saturation of less than 50%, interventions should be performed.
Neither of these is optimal: parenchymal probe monitors discrete areas of the brain while jugular bulb measures global brain oxygenation which may not be sensitive to, or reflective of, focal areas of pathology. However, within their limits, these are able to provide some information of adequacy of perfusion. They are complementary to ICP and CPP because it has been shown that brain tissue oxygenation varies independently of cerebral haemo-dynamics and ICP.23,24 Integrating PbtO2-guided therapies into CPP/ICP-based protocols may reduce mortality and improve neurological outcome. Importantly, it allows clinicians to tolerate higher ICP and avoid problems with aggressive ICP management.
Belli et al. 25 and Stein et al. 26 have shown that microchemical changes precede the development of intracranial hypertension. Microdialysis allows individualized, close assessment of local cerebral metabolism by measurements of biochemical changes in brain tissue which produces neurochemical changes associated with secondary brain injury. It measures excessive excitatory amino acid (EAA), interstitial glucose, lactate, glycerol, glutamate and pyruvate, among others. Disadvantages of using cerebral microdialysis include wide variability over time, its invasive nature and cost. Microdialysis parameters are still unclear and critical thresholds are not well established. Like brain oxygen monitoring, brain microchemical assay is potentially promising but no randomized controlled trials have yet to provide convincing evidence that PbtO2 and microdialysis improve outcome. The Brain Tissue Oxygen Monitoring in Traumatic Brain Injury (BOOST) project may help evaluate the value of these techniques. Hence, microdialysis and routine use of brain oxygen monitoring are not recommendations in current clinical practice guidelines.
General measures in ICP management
Several commonly described measures may be effective in reducing raised ICP such as keeping the patient’s head neutral and elevated at 15 to 30° as these optimize venous drainage. Any circumferential dressing, such as tracheostomy ties, may need to be adjusted. Application of cervical collars should be performed and secured appropriately.
There is contention that routine placement of internal jugular central lines should be discouraged out of concerns of impeding venous drainage or deleterious effects from haematoma in a poorly sited line. At least one study suggests that the internal jugular vein route is well tolerated by patients with increased ICP. 27 In addition, use of the Trendelenburg position during siting of central lines should be avoided during herniation as this positioning acutely raises ICP. 28
Further elevation of ICP during intubation can be minimized with proper muscle relaxation, adequate analgesia and sedation depth. This also applies for noxious stimuli such as routine orotracheal suctioning and physiotherapy. Appropriate sedation can reduce ICP by decreasing metabolic demands, ventilator asynchrony and venous congestion. Seizures, pain, agitation, full bladder and bowel distension should be managed quickly. A quiet environment improves sleep, restores circadian rhythm and may improve outcome.
Ventilation
Many patients with traumatic head injuries have concomitant chest injuries, pulmonary aspiration or have undergone massive resuscitation, which predisposes them to acute respiratory distress syndrome and hypoxaemia and hypercarbia. It is therefore important to choose a ventilation strategy which strikes a balance between oxygenation, CO2 levels and ICP. Ill-chosen ventilator strategies have been shown to increase ICP via hypoventilation and hypercarbia. 29 End-tidal CO2 (EtCO2) monitoring is useful but should be used with an awareness that EtCO2 and arterial partial pressure of carbon dioxide (PaCO2) may be discordant (from physiological effects and aggravated by pathophysiological causes) in the setting of chest trauma, hypotension, or metabolic acidosis. 30 Hence sampling of PaCO2 should be performed whenever there is a change in ventilator settings or a change in the patient’s condition.
The use of positive end-expiratory pressure (PEEP) can increase intrathoracic pressure, thereby potentially increasing ICP by impeding venous drainage. PEEP up to 10–15 cmH2O in patients with concurrent raised ICP and chest pathologies has not been shown to have significant effects on ICP within this range.
Hyperventilation
Normocapnia should be standard of care for brain-injured patients. Hypocapnia should be limited to emergency management of life-threatening raised ICP pending definitive care. Hyperventilation to achieve hypocapnia reduces CBF by constricting cerebral blood vessels (decreases cerebral blood volume (CBV), CBF and ICP). Short durations of mild hyperventilation may be used as a temporizing measure until other methods of managing ICP are available as it can acutely and reliably lower ICP and PaCO2 within seconds. However, the PaCO2 should still be kept above 25 mmHg, especially when the jugular bulb saturation is less than 50%. The effects though, are short lived. Hyperventilating more than 12 hours will result in equilibration of bicarbonate ions across the blood–brain barrier, which negates the effectiveness.
In raised ICP, CBF may be reduced to a critical threshold of 18–20 ml/100 g brain tissue/min while metabolism is maintained. Prolonged hyperventilation exacerbates cerebral ischaemia through the constriction of cerebral blood vessels. 31 It also aggravates flow-metabolism imbalances, thereby worsening cerebral oedema.
Osmotherapeutics
Osmotic agents have complex effects on cerebral physiology, extending beyond effects on ICP. Response of ICP to these agents predicts survival after adjustment for confounders. 1 Hyperosmolar agents, such as mannitol and hypertonic saline, remove more water from the brain than other organs because the intact blood–brain barrier prevents diffusion of these osmotic agents into the brain, thereby creating an osmotic concentration gradient. The creation of increased serum osmolality relative to the brain parenchyma results in efflux of fluid from intracellular and extracellular compartments of the brain into the vasculature. This decreases the volume of the cranial compartment, thus reducing ICP and improving intracranial compliance. 28 This mechanism requires an intact blood–brain barrier. If this is damaged, low molecular weight, osmotically active particles may leak into the cerebral interstitium.
Effects from bolus administration of hyperosmotic solutions is superior to continuous infusion. 32 During continuous infusion, osmotically active molecules move into the interstitial space and exacerbate cerebral oedema, therefore raising ICP.
Mannitol
The use of mannitol in TBI has been shown to correlate with decreased ICP and improved CPP and CBF to hypoperfused areas. 33 Mannitol’s main mechanism of action is by increasing the osmolality of circulating blood, thereby drawing water from intercellular and intracellular spaces and expanding circulating volume. Blood viscosity decreases, thereby improving CBF and cerebral oxygen delivery. Its osmotic properties take effect in 15–30 minutes. The effective dose is 0.25–1 g/kg, administered intravenously over a period of 15–20 minutes. It consistently decreases ICP for one to six hours.
After prolonged administration, a rebound phenomenon of mannitol may be observed. The most widely held explanation is that some osmotically active molecules move across into the cerebral interstitial space and establishing a reverse osmotic gradient by raising brain osmolality, thereby paradoxically increasing ICP by causing cerebral oedema. 34 Regular administration of mannitol may result in intravascular depletion, increased serum osmolality, pre-renal azotaemia, hypotension, and electrolyte disturbances. 35 The osmotic diuresis should be compensated by adequate fluid replacement with isotonic saline to maintain euvolaemia. Mannitol is contraindicated in patients with renal failure 36 due to risk of osmotic nephrosis 32 and possible pulmonary oedema and heart failure.
A serum osmolality of 310–320 mOsm/l is generally accepted as a treatment endpoint, although some advocate that higher levels can be cautiously tolerated.4,37,38 Mannitol is excreted entirely in urine and there is a risk of acute tubular necrosis if serum osmolality exceeds these recommended levels. The concurrent use of frusemide with mannitol enhances mannitol’s effect on plasma osmolality, resulting in greater reduction of brain water.
Hypertonic saline (HTS) 3–23.4%
HTS is an alternative to mannitol. It produces osmotic dehydration and viscosity-related cerebral vasoconstriction. Its beneficial effects in head-injured patients include expansion of intravascular volume, reduction in ICP, and increase in cardiac contractility. HTS avoids complications such as hypotension. Unlike mannitol, it does not result in diuresis while increasing serum sodium and serum osmolality. This particular feature is especially useful in traumatic head injury with concomitant bleeding and hypovolemic shock. Prolonged administration of HTS is associated with lowered ICP with no adverse effects of supraphysiologic hyperosmolarity such as renal failure, pulmonary oedema, or central pontine demyelination.39,40
The initial treatment goal when using hypertonic saline is to achieve supranormal serum sodium levels of 155–160 mEq/l. This would be equivalent to serum osmolality of between 320 and 340 mOsmol/kg. If a continuous infusion of hypertonic saline is used, serum sodium should be monitored every four hours in order to avoiding rapid changes in serum sodium levels which could result in cerebral pontine myelinosis and cerebral oedema. 41
In a recent meta-analysis, Kamel et al. found that hypertonic saline is more effective than, and may be superior to, mannitol for the treatment of elevated ICP. 42 The use of 23% HTS administered centrally showed 50% ICP reduction with an onset in minutes but lasting for hours. 43 However, when compared to mannitol, it showed no significant difference in extent of ICP reduction or duration of action. 44
HTS has been shown to induce early and late reduction in S100B, neuron-specific enolase and myelin-basic protein markers of brain tissue injury. Elevation of these markers has been associated with poor outcome. 45
Intracranial hypertension is considered refractory when general measures, sedation, drainage of CSF, and hyperosmolar therapy fail.
Agents to reduce cerebral metabolic rate of oxygen (CMRO2)
When ICP control becomes difficult, alteration of neuronal metabolic activity via induction of pharmacological coma can be considered. 46 Drugs such as anaesthetic agents (barbiturates, propofol, midazolam) result in large reduction (approximately 50%) in CMRO2. Decreased cerebral metabolic rate and reduced tissue oxygen demand result in vasoconstriction with resulting reduction in CBF and CBV.
Barbiturates, namely pentobarbital or thiopentone, are initiated with intravenous loading followed by an infusion maintenance titrated to therapeutic goals of burst suppression on electroencephalogram (EEG) or satisfactory reduction in ICP. If ICP remains high despite achieving burst suppression, further increase in dose of barbiturates may not be effective. 47 Barbiturate therapy results in a fall in blood pressure in one in four patients. Such hypotensive episodes adversely affect CPP. 48
Although barbiturates are useful in reducing ICP, its effect on long-term outcome in patients with acute severe head injury remains unclear although severe TBI and refractory ICP treated with pentobarbital coma showed 40% survival and 68% achieved good functional outcomes. 49
Propofol is also used to reduce CMRO2 and decreasing ICP. It maintains flow-metabolism coupling even at higher doses, induces vasoconstriction and decreases CMRO2 resulting in decreased CBF, CBV and ICP. In head injury, at high doses (6–8 mg/kg/hour) it alters cerebrovascular pressure autoregulation. Long-term use and high doses are associated with propofol infusion syndrome (more than 4 mg/kg/hour, more than 48 hours). 50 Propofol may not significantly reduce ischaemic burden from TBI despite EEG burst suppression.
Hypothermia as a neuroprotectant appears intuitive because of the multiple mechanisms in protecting the brain from secondary injury, including by reduction of CMRO2.51,52 Its benefit is best evidenced by efficacy in management of transient global brain ischaemia post-cardiac arrest. However, cooling is not without side effects as it may result in coagulopathy, anti-platelet effect, shivering and susceptibility to infections. Current evidence supports avoiding hyperthermia. The Targeted Temperature Management trial 53 involving out-of-hospital cardiac arrest showed no difference in neurological outcomes or survival between the arms of hypothermia at 33°C or modest temperature control of 36°C. When only high-quality trials were analyzed, no benefit of prophylactic hypothermia on mortality or neurological morbidity could be identified. 54
Currently, use of induced hypothermia for treatment of ICP in severe head injury is a second-tier therapy of questionable value for managing refractory ICP. Future studies such as the Prophylactic Hypothermia Trial (POLAR) 55 study are awaited to determine if early cooling of patients with severe TBI is associated with better outcomes.
Avoidance of fever is paramount as fever after neurological insults is known to worsen outcomes. 56 Effecting normothermia, just like therapeutic hypothermia, can be achieved using antipyretics, ice-cold saline, airway cooling, invasive intravascular cooling, or various methods of surface cooling. 57 It is useful to note that intracranial and core temperatures are not equivalent, with the latter being higher.
Surgery
Placement of an external ventricular drain should be considered in patients with moderately sized ventricles and signs and symptoms of raised ICP. The removal of CSF via a ventriculostomy is preferred over the use of a lumbar drain due to the risk of transtentorial herniation. Drainage of 5 to 10 ml of CSF may improve compliance and the ICP.
Decompressive craniectomy (DC) is a surgical approach for the management of increased ICP especially due to TBI. Craniectomy alone lowers ICP by 15% but with dural opening, the ICP can decrease by 70%. Reported results from decompressive craniectomy are conflicting.58,59 In adults with severe diffuse TBI and brain swelling, early decompressive craniectomy decreased the ICP and length of intensive care stay but increased unfavourable outcomes.
This was evaluated in the Decompressive Craniectomy in the Patients with Severe Traumatic Brain Injury (DECRA) trial, 60 where DC did not improve functional outcomes at six months after injury when compared to a group assigned to receive best medical therapy for raised ICP. This was despite an immediate and sustained reduction of ICP by approximately 25% in the craniectomy group compared to the medical care group. A total of 70% of those who underwent decompressive craniectomy died, were in a vegetative state, or had severe disabilities six months after injury whilst only 51% of the ‘standard-care’ group had such unfavourable outcomes. This trial, however, received criticism, 61 and some neurosurgeons felt that the DECRA results should have no influence on clinical practice. They took issue with problems in randomization, with unequal severity of TBI in both arms of the study. More patients in the surgical group had unequal pupils, the ICP threshold of more than 20 mmHg for a duration of 15 minutes or more before surgery was performed did not reflect current neurosurgical practice, unusual choice of operative techniques (bifrontal procedures), and high crossover rates from standard care arm to surgical arm.
The role of DC when ICP continues to increase beyond 20 mmHg remains to be established. The results from another study, Randomized Evaluation of Surgery with Craniectomy for Uncontrollable Increase of Intracranial Pressure (RESCUEicp), may help to further define the role of DC in the management of severe TBI. 62
For completeness sake, it is appropriate to mention brain tumours as another common condition resulting in raised ICP in the neurocritical care setting. These patients usually present with compressive symptoms as a result of decompensation from raised ICP as a result of tumour growth, worsening perilesional oedema or haemorrhage into the tumour. In addition to the measures mentioned earlier in the management of raised ICP, there is an established role of steroids in the management of such vasogenic brain swelling. 63 Emergency tumour excision may also be required.
Other options to manage raised ICP which have been discussed but not formally embraced in mainstream clinical practice will be mentioned.
The use of hyperbaric oxygen therapy (HBOT) in TBI has been shown to reduce ICP, may reduce the risk of death and improve final GCS, but there is little evidence that the survivors have a good functional outcome. The routine application of HBOT to these patients cannot be justified. 64 Progesterone has been shown to have potentially protective properties in slowing development of malignant cerebral oedema and raised ICP.65,66 Two ongoing clinical trials seek to examine the potential benefit of administered progesterone therapy in traumatic head injury: Progesterone for Traumatic Brain Injury, Experimental Clinical Trial III (ProTECT III) and Study of the Neuroprotective Activity of Progesterone in Severe Traumatic Brain Injury (SyNAPSe). The anaesthetic ketamine offers yet another, if perhaps underused, option for the medical management of ICP. Ketamine, an inhibitor of the N-methyl-D-aspartate receptor, has previously been reported to cause increases in ICP. 67 Its use has been examined by several recent prospective studies and appears to be safe in increased ICP. 68 The reasons for its behaviour are not entirely known and there is variation of effects depending on its R or S or racemic states. There is growing interest in its role in management of traumatic head injury as an intubating agent, sedation or to improve CPP. 69 However, its use in the setting of raised ICP is not advocated in any of the published treatment guidelines for TBI, aneurysmal subarachnoid haemorrhage, ischaemic stroke, or intracerebral haemorrhage.
Conclusion
ICP monitoring has contributed to neurocritical care advancements and improved patient outcome. It is important to identify early those patients who would benefit from ICP monitoring and apply interventions to treat raised ICP. By considering factors such as vasoreactivity and CBF, blood/brain osmotic gradient, metabolic rate of oxygen consumption of cerebral tissue and issues of intracranial compliance, the intensivist can better instigate treatment by modifying these factors. The current evidence for instigating various first- and second-tier methods of treatment was discussed. Despite limitations of any individual method, the goal of treatment is to reduce long-term damage and prevent secondary insults to the injured brain tissues. We look forward to results from newer studies on the role of decompressive craniectomy, barbiturate coma and individualizing management based on brain tissue oxygenation levels and brain milieu to improve ICP management.
Footnotes
Conflict of interest
None declared.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
