Abstract
Objective
This study aimed to compare short-term arthroscopic and clinical outcomes between microfractures with (treatment group) and without (control group) acellular particulated costal allocartilage in patients undergoing concurrent high tibial osteotomy (HTO).
Design
This retrospective cohort study enrolled 19 and 21 patients in the treatment and control groups, respectively, and reviewed them at a minimum 2-year follow-up after HTO. Cartilage regeneration status was evaluated according to the International Cartilage Repair Society–Cartilage Repair Assessment (ICRS-CRA) grading and Koshino’s macroscopic staging systems during medial locked plate removal. Patient-reported measures, including the visual analog scale pain score, Knee Injury and Osteoarthritis Outcome Score, and International Knee Documentation Committee score, assessed clinical outcomes.
Results
The total points of the ICRS-CRA grading system were significantly higher in the treatment group than in the control group (7.7 ± 3.8 vs 4.2 ± 3.0, respectively; P = 0.007). Likewise, the cartilage status according to Koshino’s macroscopic staging system was better in the treatment group (P = 0.022). Patient-reported functional outcomes significantly improved postoperatively but were equivalent between the study groups at the final follow-up.
Conclusions
Microfractures augmented with acellular particulated costal allocartilage resulted in better repair quality than microfractures alone at a minimum 2-year follow-up after HTO, but functional outcomes improved similarly for both treatment approaches.
Keywords
Introduction
High tibial osteotomy (HTO) is a realigning surgical procedure that shifts the load-bearing axis from the diseased compartment to the other compartment (i.e., from the medial to lateral compartment or lateral to medial compartment).1-3 In patients with concurrent osteoarthritis or focal cartilage defect in the medial compartment of the knee and varus deformity, medial open-wedge HTO became an established surgical option because of its ease of performance, safety, and feasibility in achieving target alignment.4,5 HTO provides favorable clinical outcomes regarding symptomatic pain relief, functional recovery, and return to sports or work, even in intermediate- or long-term follow-ups.6-8 Furthermore, HTO can delay the need for total knee arthroplasty, with a conversion rate of 18% to 27% at 10 years.9,10
The degree of restoration of the damaged cartilage can affect patient-reported clinical outcomes and possibly the survivorship of HTO.10-12 Efforts to improve cartilage quality have been made, although biomechanical changes in the knee joint from unloading the diseased compartment by HTO alone may result in cartilage restoration.12-14 Marrow stimulation by procedures such as microfracture or microdrilling, regarded as the gold standard for cartilage repair, has been used as an adjunct to improve the quality of the repaired cartilage.15-19 However, the clinical results of the marrow stimulation procedures were conflicting, probably due to the unpredictable and insufficient restoration of cartilage quality by microfracture alone. 20
Microfracture augmentation with various scaffolding techniques was proposed to overcome the shortcomings of microfractures and lead to better clinical and magnetic resonance imaging (MRI) outcomes than microfracture alone.21,22 However, whether augmented microfracture benefits patients undergoing HTO remains unclear because of sparsity of literature on the subject. Only a few studies have reported favorable outcomes after augmented microfracture with a scaffold to enhance the quality of the repaired cartilage in addition to HTO.23,24 Recently, particulated costal allocartilage resembling native hyaline cartilage has been introduced as a potentially ideal scaffold for cartilage regeneration. 25 However, the influence of particulated costal allocartilage as an augmentation for microfracture in patients who underwent concurrent HTO remains elusive.
This study aimed to compare the arthroscopic and clinical outcomes between microfractures with particulated costal allocartilage and microfractures alone in patients undergoing concurrent HTO. We hypothesized that in patients with HTO, particulated costal allocartilage with microfracture would have (1) superior quality of the repaired cartilage at the time of second-look arthroscopy and (2) better clinical outcomes than those of microfracture alone after a minimum 2-year follow-up.
Methods
Study Design and Population
Using data from a previous randomized controlled trial (RCT), patients who underwent concurrent HTO for varus malalignment and microfracture for a cartilage defect were retrospectively reviewed. 25 The RCT, a multicenter, prospective, randomized study across 4 hospitals, compared microfracture with particulated costal allocartilage and microfracture alone for knee cartilage defects, regardless of lower extremity malalignment. This RCT included patients aged 19 to 65 years with focal cartilage defects measuring <10 cm2 in size and an International Cartilage Repair Society (ICRS) grade III or IV. The RCT excluded patients with a body mass index ≥30 kg/m2, inflammatory or autoimmune arthritis, a history of cartilage surgery (within 1 year before enrollment), systemic steroid medication (within 1 month before enrollment), or any form of intra-articular injection, such as hyaluronic acid or steroids (within 3 months before enrollment), current pregnancy or breastfeeding, and systemic or localized infection. Concurrent HTO was indicated in patients with a mechanical tibiofemoral angle of more than varus 5° on standing full-length lower extremity radiograph and a good range of motion in the knee joint (arc of motion >100°, flexion contracture <15°). The institutional review board of each 1 of the 4 hospitals approved the study and waived the requirement for obtaining informed consent from the patients. The research process was performed in accordance with the Declaration of Helsinki.
The final RCT cohort included 44 patients for each type of microfracture, including a microfracture with particulated costal allocartilage group and a microfracture alone group. In this cohort, concurrent HTO was performed in 19 patients of the microfracture with particulated costal allocartilage group (treatment group) and 21 patients of the microfracture alone group (control group;

Patient flowchart of the inclusion and exclusion process.
Surgical Procedures
The surgical procedures were performed by 4 sports medicine surgeons at 4 different hospitals. Diagnostic arthroscopy was performed in each knee compartment to confirm cartilage defects and identify additional pathologies. Unstable cartilage flaps near the defects were meticulously debrided using an arthroscopic shaver, curette, or gouge to create healthy vertical cartilage surroundings. The residual calcified layer in the cartilage defect was entirely removed while preserving the subchondral layer. Microfracture was then performed using drills to make as many holes as possible at a depth of more than 2 mm and approximately 3 to 4 mm apart.
In the treatment group, the cartilage defects were augmented with particulated costal allocartilage (MegaCarti, L&C BIO Co., Seongnam, Korea) in addition to the microfractures (
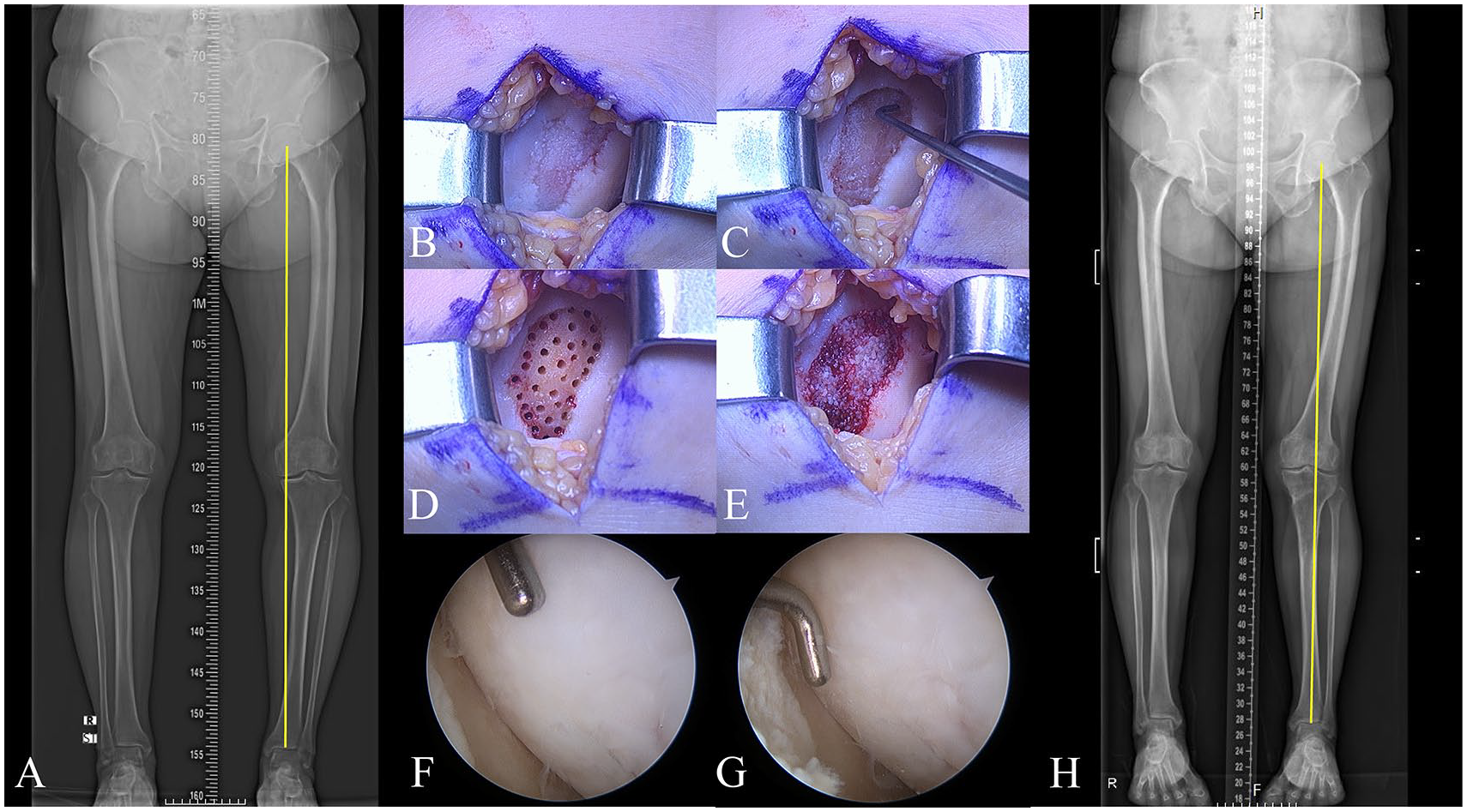
A 64-year-old female patient with varus malalignment of the lower extremity (
Concurrent biplanar open-wedge HTO was performed in all included patients to correct varus malalignment. An oblique skin incision was made on the proximal-medial tibia between the tibial tubercle and the medial border of the proximal tibia. After the complete release of the superficial medial collateral ligament, 2 parallel guidewires were obliquely inserted toward the upper fibular head. Separate vertical osteotomy was performed in the coronal plane from approximately 1 cm behind the tibial tubercle to the level of the inserted guidewires, and transverse osteotomy was performed along the guidewires following the vertical osteotomy. An adjustable bone spreader was used to maintain the opening gap at a predetermined angle. The opening angle of the osteotomy site was determined preoperatively using the Miniaci method, targeting the mechanical axis line passing through the Fujisawa point. 26 Afterward, a medial locked plate (Ohtofix; Ohtomedical, Goyang, Korea) was used to fix the osteotomy site.
Postoperative Rehabilitation
All patients underwent the same rehabilitation protocol. Exercises, including knee range of motion exercises, manual patellar mobilization, and quadriceps setting exercises, were started immediately after the index surgery. Active and passive machine-assisted range of motion was maintained for 4 to 6 weeks after surgery. Partial weight-bearing ambulation was allowed from 4 weeks after surgery, and full weight-bearing was allowed from 8 to 12 weeks after surgery.
Second-Look Arthroscopic Evaluation
Diagnostic arthroscopy was performed at the time of medial locked plate removal to evaluate the status of the repaired cartilage (
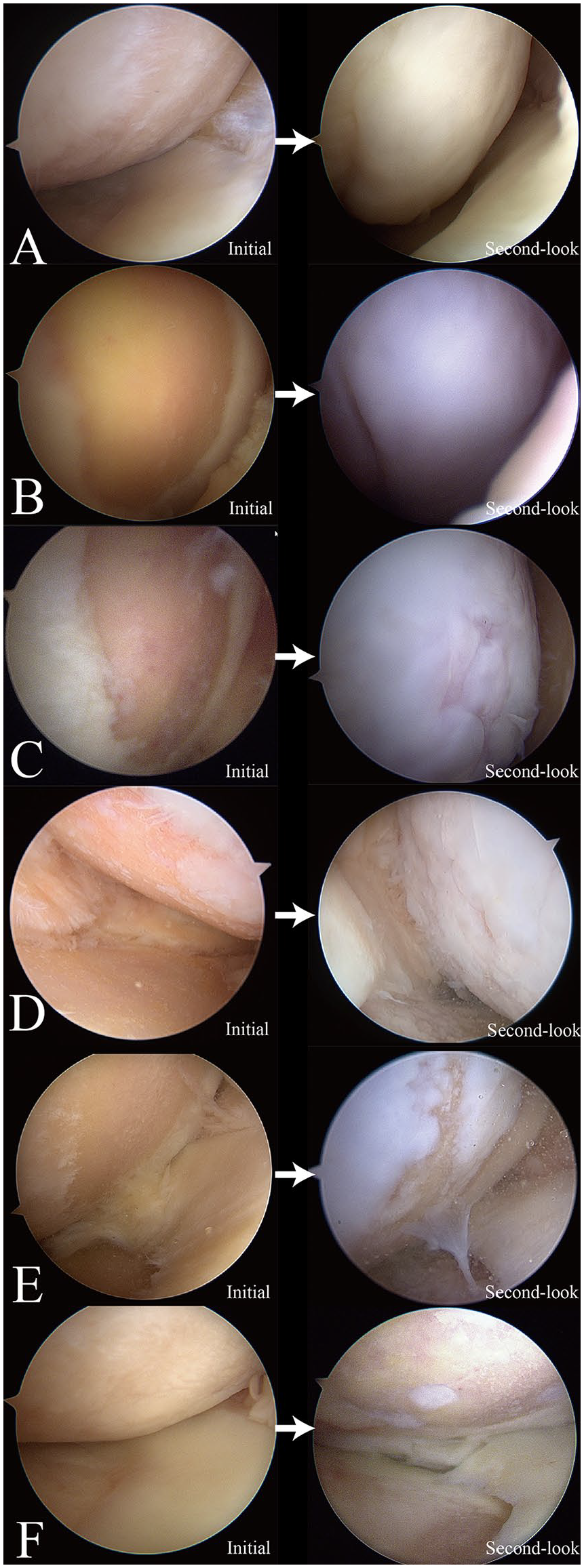
Initial arthroscopic images of the cartilage defect and second-look arthroscopic images of the repaired cartilage in the treatment group. The repaired cartilage status is shown as excellent (
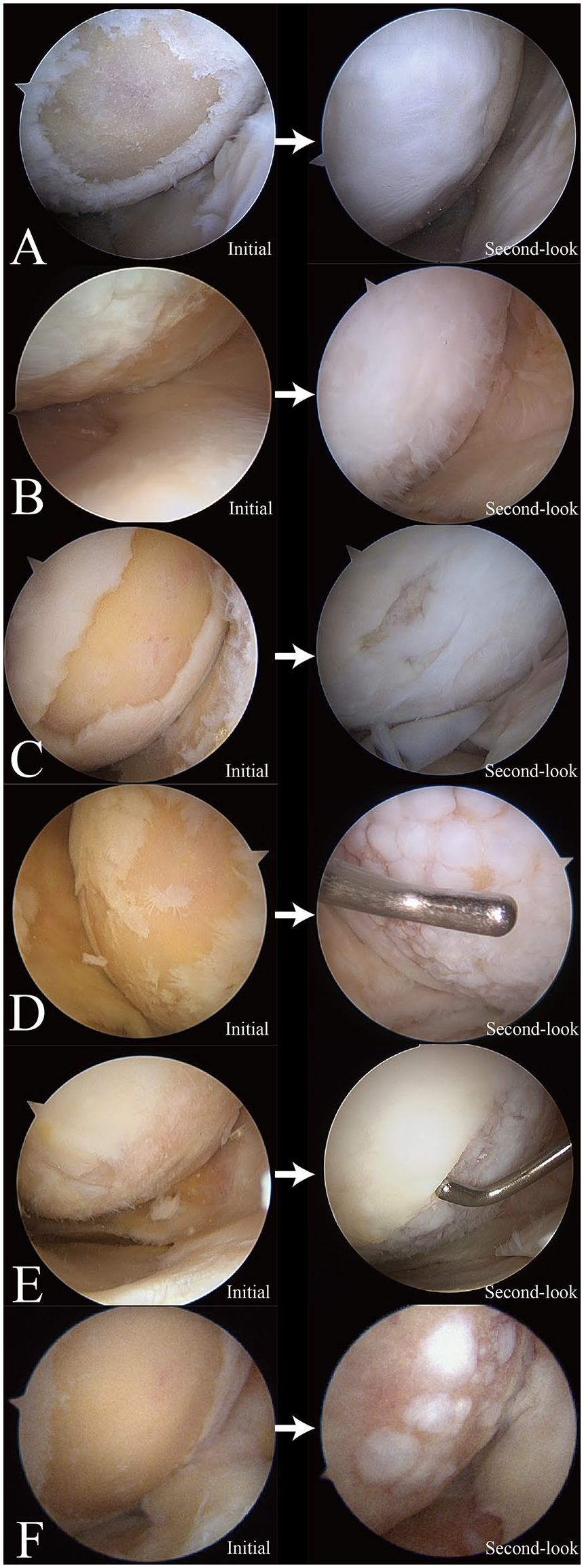
Initial arthroscopic images of the cartilage defect and second-look arthroscopic images of the repaired cartilage in the control group. The repaired cartilage status is shown as excellent (
Clinical Evaluation
Clinical outcomes were collected by blinded independent raters at 12, 24, and 48 weeks after surgery and thereafter annually or at every visit. The clinical outcomes were assessed using patient-reported outcome measures, such as the visual analog scale (VAS) pain score, 28 Knee Injury and Osteoarthritis Outcome Score (KOOS), 29 and International Knee Documentation Committee (IKDC) score.30,31
Statistical Analysis
Statistical analyses were performed using SAS software (version 9.4; SAS Institute Inc., Cary, NC, USA), with statistical significance set at P < 0.05. Depending on the results of the Shapiro–Wilk test, the independent t-test or Wilcoxon rank-sum test was used to compare continuous variables between the 2 study groups. The chi-square test or Fisher’s exact test was used to compare categorical variables between the groups. The paired t-test or Wilcoxon signed-rank test was used to compare changes in continuous variables before surgery and at every follow-up visit within each group. Power analysis was calculated using G*Power (version 3.1) with a significance level (α) of 5%, based on the mean difference of the total points according to the ICRS-CRA grading system between the groups. 32
Results
Patient Characteristics
The number of patients who underwent HTO in the RCT cohort was 19 and 21 in the treatment and control groups, respectively. Among them, 18 patients in the treatment group and 15 in the control group underwent diagnostic arthroscopy at the time of medial locked plate removal, at a mean of 1.4 years after surgery. The baseline characteristics of the patients were not significantly different between the groups (
Table 1
and
Baseline Characteristics.

Values are presented as mean ± standard deviation or number of patients (percentages).
ICRS = International Cartilage Repair Society.
Arthroscopic Outcome
At the time of the index surgery, the size or ICRS grade of the cartilage defect treated with microfracture was similar in patients with and without particulated costal allocartilage ( Table 2 ). At the time of the second-look arthroscopy, the quality of the repaired cartilage in the treatment group was superior to that in the control group. The total points based on the ICRS-CRA grading system were significantly higher in the treatment group than in the control group (7.7 ± 3.8 vs 4.2 ± 3.0, respectively; P = 0.007). However, the proportion of repaired cartilage was not significantly different between groups according to the ICRS-CRA grading system (P = 0.052). According to Koshino’s macroscopic staging system, the repaired cartilage status was better in the treatment group than in the control group (P = 0.022).
Initial and Second-Look Arthroscopic Findings of the Cartilage Lesion.

Values are presented as mean ± standard deviation or number of patients (percentages).
ICRS = International Cartilage Repair Society; CRA = cartilage repair assessment.
Bold font indicates statistically significant results (P < 0.05).
Clinical and Radiological Outcomes
Clinical outcomes evaluated based on patient-reported functional outcomes were significantly improved after the surgery at a follow-up of a minimum of 2 years and a mean of 2.2 years (treatment group 106.0 ± 6.0 weeks vs control group 108.0 ± 4.6 weeks, P = 0.109; Table 3 ). However, the clinical scores, including IKDC score, VAS pain score, and KOOS, were equivalent between the groups at the latest follow-up.
Comparison of Patient-Reported Functional Outcomes Between the Groups.

Values are presented as mean ± standard deviation.
ADL = activities of daily living; IKDC = International Knee Documentation Committee; KOOS = Knee Injury and Osteoarthritis Outcome Score; QOL = quality of life; VAS = visual analog scale.
Bold font indicates statistically significant results (P < 0.05).
In terms of radiographic parameters, the mean hip-knee-ankle angle was significantly corrected in both groups (both P < 0.001), and the mean posterior tibial slope was significantly increased in the treatment group (P = 0.032; Table 4 ). However, the radiological outcomes did not differ between the groups at the latest follow-up.
Comparison of Radiological Outcomes Between the Groups.

Values are presented as mean ± standard deviation or number of patients (percentages).
HKA = hip-knee-ankle.
Varus alignment of the lower extremity is indicated as a positive value and valgus alignment as a negative value.
Bold font indicates statistically significant results (P < 0.05).
Discussion
The principal finding of this study was that in patients who underwent concurrent HTO, microfracture augmented with particulated costal cartilage produced better cartilage quality than microfracture alone. Regardless of the postoperative cartilage status, patient-reported clinical outcomes significantly improved in both groups after a minimum of 2 years after HTO, and the short-term clinical outcomes at a minimum 2-year follow-up did not differ between the study groups.
High tibial osteotomy alone can regenerate defective cartilage by offloading the lesion and changing the biomechanical environment in the knee joint.12-14 Koshino et al. 33 reported that the cartilage was regenerated fully in 32%, partially in 59%, and not in 9% of patients who underwent HTO alone. Kim et al. 13 also showed that 52% of the cartilage lesions treated with HTO alone were improved according to the ICRS grade. Moreover, 38% of all treated patients had total regeneration for cartilage defects, and 35% had partial regeneration, according to Koshino’s macroscopic grading system. Compared to these previous studies, the treatment group in our study showed better total and partial cartilage regeneration according to Koshino’s macroscopic grading system (67% and 28%, respectively). This implies that microfractures with particulated costal allocartilage contribute to cartilage regeneration, in addition to HTO.
Whether adding microfractures without augmentation, which is regarded as the first-line treatment for cartilage defects, to HTO produces better cartilage regeneration than HTO alone remains controversial. Using the Outerbridge classification, Matsunaga et al. 34 compared second-look arthroscopic outcomes between HTO alone and HTO combined with microfracture and found no difference between these approaches. Jung et al. 16 demonstrated that HTO supplemented with subchondral drilling did not differ from HTO alone regarding cartilage regeneration at 2 years according to second-look arthroscopic results. In contrast, Lee et al. 15 showed better cartilage regeneration in terms of ICRS grading during second-look arthroscopy and modified magnetic resonance observation of cartilage repair tissue score evaluated by MRI. These inconsistent findings suggest that the quality of the regenerated cartilage after a microfracture may not be sufficient to add a regenerative effect to HTO owing to the probable low quality of the repaired cartilage.
To overcome the limitations of the microfracture technique, several types of scaffolds have been developed to augment the microfracture of cartilage defects, and these scaffolds showed promising results.23,24,35 Particulated costal allocartilage which resembles the contents and architecture of articular cartilage and induces chondrogenesis similar to articular cartilage is one of the recently developed potentially ideal scaffolds to enhance microfracture effects. 25 In the previous RCT comparing microfracture with particulated costal allocartilage and microfracture alone, particulated costal allocartilage showed superior cartilage repair quality in terms of MRI evaluation at 48-week follow-up, regardless of whether HTO was performed or not. 25 In the present study, patients who underwent second-look arthroscopy during the medial locked plate removal could be evaluated for the gross appearance of the cartilage regeneration. The cartilage repair status was significantly superior in the group with particulated costal allocartilage augmentation according to both ICRS-CRA and Koshino’s macroscopic grading systems, although the patient-reported clinical outcomes were equivalent in the short-term follow-up of a minimum of 2 years. Our study results provide further evidence that augmented microfractures during HTO can improve cartilage repair quality compared to HTO alone or HTO with microfractures.
A few studies reported favorable short-term clinical outcomes after scaffold-augmented microfracture in patients who underwent HTO, but evidence of its superiority over microfracture alone is inconclusive.17,24 Kim et al. 23 demonstrated that the 1-year clinical outcomes, including VAS pain score, KOOS, IKDC score, and Tegner activity score, were improved after microfracture with porcine-derived type I collagen augmentation in patients undergoing HTO but were equivalent to those of microfracture alone. Shon et al. 24 performed subchondral drilling with particulated costal cartilage augmentation in patients who underwent HTO and compared it with subchondral drilling alone after propensity score matching. Their results showed that based on both KOOS and Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC), the 2 treatment approaches were not different 2 years after index surgery. Our study is in accordance with these previous studies in that short-term clinical outcomes were not superior in the treatment group compared with those in the control group, even though the cartilage regeneration status was superior in the treatment group. The similar results between the groups might be due to the excellent short-term clinical outcomes observed with microfracture alone, which could be comparable to those achieved with other advanced cartilage restoration methods. 36 However, considering that a 2-year follow-up may be insufficient to fully demonstrate the superior effects of particulated costal allocartilage, we anticipate that microfracture combined with particulated costal allocartilage will result in not only improved cartilage repair but also superior clinical outcomes with longer follow-up, compared to microfracture alone. Additionally, significantly better cartilage regeneration may be necessary to impact short-term outcomes in HTO patients, as other factors beyond cartilage regeneration could also influence clinical results.
The cartilage regeneration quality after HTO is crucial because it might be related to clinical outcomes, especially intermediate outcomes and survivorship after HTO.10-12,37 Yang et al. 11 classified patients who underwent HTO into 2 groups according to the cartilage status of the medial femoral condyle in second-look arthroscopy. They found that the patient-reported clinical outcomes, including IKDC score and WOMAC, were significantly better in the group with good cartilage status (ICRS grades I and II) than in the group with poor cartilage status (ICRS grades III and IV) with a mean 5-year follow-up. Moreover, ICRS-CRA grades were significantly correlated with IKDC score and WOMAC. In this context, because the cartilage status was significantly better in the treatment group than in the control group in our study, it would be beneficial to closely monitor the intermediate- or long-term follow-up results of microfracture with particulated costal allocartilage to determine the effects of cartilage regeneration on functional outcomes.
Unlike autologous minced cartilage implantation, which uses autologous, activated, nondedifferentiated chondrocytes within the minced cartilage, particulated costal allocartilage functions as an acellular extracellular matrix scaffold, closely resembling native hyaline cartilage in mechanical, biochemical, and structural properties. 38 It has the potential to induce progenitor cells to develop in a chondrogenic direction through migration, adherence, proliferation, and differentiation. 25 As demonstrated in our current study and previous RCT, particulated costal allocartilage effectively enhances cartilage repair. 25 Furthermore, the “off-the-shelf” nature of the particulated costal allocartilage provides a practical advantage in surgical settings, allowing for immediate deployment in the operating theater, particularly when larger cartilage defects are unexpectedly encountered, ensuring efficient and timely cartilage repair.
This study has several limitations. First, it included a relatively small number of patients. This study focused on patients who underwent HTO in a previous RCT, comparing microfractures with and without particulated costal allocartilage. However, the statistical power of the total points according to the ICRS-CRA grading system between the groups, as calculated using G*Power, was sufficient (80.9%). Second, gross morphology grading systems, including the ICRS-CRA or Koshino’s macroscopic grading systems, were used to assess the repair cartilage quality. The best way to determine cartilage quality is histological evaluation by articular biopsy; however, it is invasive, destructive, and unethical. 39 Diagnostic arthroscopy at the time of medial locked plate removal after HTO is a well-established method to evaluate cartilage quality and avoid issues regarding articular biopsy. Third, the clinical outcomes were evaluated approximately 2 years after HTO, which is a relatively short-term result. More extended follow-up periods would be needed to establish a solid conclusion regarding the effect of microfracture with particulated costal allocartilage during HTO because the cartilage restoration quality after HTO might be related to intermediate-term clinical outcomes. 11 Fourth, 4 sports medicine surgeons in 4 different hospitals performed the surgery, possibly leading to performance bias. The surgeons held several meetings to reduce bias and share the same surgical concepts.
In conclusion, microfractures augmented with particulated costal allocartilage resulted in better repair quality than microfractures alone in patients who underwent HTO. The functional outcomes improved for both treatments after a minimum of 2 years after HTO but were not different between the treatments.
Supplemental Material
sj-docx-1-car-10.1177_19476035241292321 – Supplemental material for Acellular Particulated Costal Allocartilage Improves Cartilage Regeneration in High Tibial Osteotomy: Data From a Randomized Controlled Trial
Supplemental material, sj-docx-1-car-10.1177_19476035241292321 for Acellular Particulated Costal Allocartilage Improves Cartilage Regeneration in High Tibial Osteotomy: Data From a Randomized Controlled Trial by Kwangho Chung, Min Jung, Ki-Mo Jang, Sanghoon Park, Jaehong Kim and Sung-Hwan Kim in CARTILAGE
Footnotes
Abbreviations
CRA, cartilage repair assessment; HTO, high tibial osteotomy; ICRS, International Cartilage Repair Society; IKDC, International Knee Documentation Committee; KOOS, knee injury and osteoarthritis outcome score; RCT, randomized controlled trial; VAS, visual analog scale; WOMAC, Western Ontario and McMaster Universities Osteoarthritis Index.
Acknowledgments and Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
The study was approved by the Institutional Review Board of Severance Hospital, Yonsei University College of Medicine (1-2023-0057), Anam Hospital, Korea University College of Medicine (2023AN0288), National Health Insurance Service Ilsan Hospital (NHIMC 2023-06-013), and Gangnam Severance Hospital, Yonsei University College of Medicine (3-2023-0155).
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
